Key Points
-
Glycosylation is a key cellular mechanism regulating several physiological and pathological functions. Alterations in glycoproteins, glycosphingolipids and proteoglycans are common features of cancer cells.
-
The most-widely occurring cancer-associated changes in protein glycosylation are increased sialylation, increased branched-glycan structures and overexpression of 'core' fucosylation.
-
The overexpression of branched-N-glycan structures interferes with epithelial cadherin-mediated cell–cell adhesion, promoting tumour cell dissociation and invasion.
-
Modifications of integrins with branched N-glycans, truncated O-glycans and/or sialylated structures modulate tumour cell–matrix interactions, fostering the process of tumour cell migration.
-
Altered expression of proteoglycans and their glycosaminoglycan chains interfere with extracellular signalling molecules and modulate the activation of tyrosine kinase protein receptors.
-
Altered glycosylation of growth factor receptors and the modified expression of gangliosides affect cancer cell signal transduction pathways, modulating tumour cell growth and proliferation.
-
Glycans and their corresponding endogenous carbohydrate-recognition lectins are key regulators of the inflammation and immune response towards the tumour cells.
-
Several serological markers currently used in the clinic are based on the detection of circulating glycoproteins or glycoconjugates with altered glycosylation.
-
Glycans have major potential applications in improving early diagnosis, determination of prognosis and risk stratification, as well as in serving as markers of specific therapeutic targets.
Abstract
Despite recent progress in understanding the cancer genome, there is still a relative delay in understanding the full aspects of the glycome and glycoproteome of cancer. Glycobiology has been instrumental in relevant discoveries in various biological and medical fields, and has contributed to the deciphering of several human diseases. Glycans are involved in fundamental molecular and cell biology processes occurring in cancer, such as cell signalling and communication, tumour cell dissociation and invasion, cell–matrix interactions, tumour angiogenesis, immune modulation and metastasis formation. The roles of glycans in cancer have been highlighted by the fact that alterations in glycosylation regulate the development and progression of cancer, serving as important biomarkers and providing a set of specific targets for therapeutic intervention. This Review discusses the role of glycans in fundamental mechanisms controlling cancer development and progression, and their applications in oncology.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Fuster, M. M. & Esko, J. D. The sweet and sour of cancer: glycans as novel therapeutic targets. Nat. Rev. Cancer 5, 526–542 (2005).
Hakomori, S. Glycosylation defining cancer malignancy: new wine in an old bottle. Proc. Natl Acad. Sci. USA 99, 10231–10233 (2002).
Reis, C. A., Osorio, H., Silva, L., Gomes, C. & David, L. Alterations in glycosylation as biomarkers for cancer detection. J. Clin. Pathol. 63, 322–329 (2010).
Taniguchi, N., Hancock, W., Lubman, D. M. & Rudd, P. M. The second golden age of glycomics: from functional glycomics to clinical applications. J. Proteome Res. 8, 425–426 (2009).
Pinho, S. S. et al. Gastric cancer: adding glycosylation to the equation. Trends Mol. Med. 19, 664–676 (2013).
Freeze, H. H. Understanding human glycosylation disorders: biochemistry leads the charge. J. Biol. Chem. 288, 6936–6945 (2013). This Review describes the genetic and biochemical advances in the diagnosis of several inherited human glycosylation disorders.
Ohtsubo, K. & Marth, J. D. Glycosylation in cellular mechanisms of health and disease. Cell 126, 855–867 (2006).
Varki, A. et al. (eds) Essentials of Glycobiology 2nd edn (Cold Spring Harbor Laboratory Press, 2009).
Cummings, R. D. The repertoire of glycan determinants in the human glycome. Mol. Biosyst. 5, 1087–1104 (2009).
Gabius, H. J., Andre, S., Jimenez-Barbero, J., Romero, A. & Solis, D. From lectin structure to functional glycomics: principles of the sugar code. Trends Biochem. Sci. 36, 298–313 (2011).
Moremen, K. W., Tiemeyer, M. & Nairn, A. V. Vertebrate protein glycosylation: diversity, synthesis and function. Nat. Rev. Mol. Cell Biol. 13, 448–462 (2012).
Bennett, E. P. et al. Control of mucin-type O-glycosylation: a classification of the polypeptide GalNAc-transferase gene family. Glycobiology 22, 736–756 (2012). This article reports on the biological function of the polypeptide GalNAc transferase gene family, the largest glycosyltransferase enzyme family.
Clausen, H. & Bennett, E. P. A family of UDP-GalNAc: polypeptide N-acetylgalactosaminyl-transferases control the initiation of mucin-type O-linked glycosylation. Glycobiology 6, 635–646 (1996).
Brockhausen, I., Yang, J., Lehotay, M., Ogata, S. & Itzkowitz, S. Pathways of mucin O-glycosylation in normal and malignant rat colonic epithelial cells reveal a mechanism for cancer-associated sialyl-Tn antigen expression. Biol. Chem. 382, 219–232 (2001). This Review describes the pathways of mucin-type O -glycosylation.
Ma, J. & Hart, G. W. O-GlcNAc profiling: from proteins to proteomes. Clin. Proteomics 11, 8 (2014).
Luther, K. B. & Haltiwanger, R. S. Role of unusual O-glycans in intercellular signaling. Int. J. Biochem. Cell Biol. 41, 1011–1024 (2009).
Julien, S., Bobowski, M., Steenackers, A., Le Bourhis, X. & Delannoy, P. How do gangliosides regulate RTKs signaling? Cells 2, 751–767 (2013).
Ladenson, R. P., Schwartz, S. O. & Ivy, A. C. Incidence of the blood groups and the secretor factor in patients with pernicious anemia and stomach carcinoma. Am. J. Med. Sci. 217, 194–197 (1949).
Hakomori, S. I. & Murakami, W. T. Glycolipids of hamster fibroblasts and derived malignant-transformed cell lines. Proc. Natl Acad. Sci. USA 59, 254–261 (1968).
Feizi, T. Carbohydrate antigens in human cancer. Cancer Surv. 4, 245–269 (1985).
Holmes, E. H., Ostrander, G. K., Clausen, H. & Graem, N. Oncofetal expression of Lex carbohydrate antigens in human colonic adenocarcinomas. Regulation through type 2 core chain synthesis rather than fucosylation. J. Biol. Chem. 262, 11331–11338 (1987).
Hakomori, S. & Kannagi, R. Glycosphingolipids as tumor-associated and differentiation markers. J. Natl Cancer Inst. 71, 231–251 (1983).
Marcos, N. T. et al. ST6GalNAc-I controls expression of sialyl-Tn antigen in gastrointestinal tissues. Front. Biosci. (Elite Ed.) 3, 1443–1455 (2011).
Julien, S. et al. ST6GalNAc I expression in MDA-MB-231 breast cancer cells greatly modifies their O-glycosylation pattern and enhances their tumourigenicity. Glycobiology 16, 54–64 (2006).
Kannagi, R., Yin, J., Miyazaki, K. & Izawa, M. Current relevance of incomplete synthesis and neo-synthesis for cancer-associated alteration of carbohydrate determinants—Hakomori's concepts revisited. Biochim. Biophys. Acta 1780, 525–531 (2008). This Review describes the incomplete synthesis and neo-synthesis processes as two major concepts for cancer-associated alterations of cell-surface carbohydrate determinants.
Buckhaults, P., Chen, L., Fregien, N. & Pierce, M. Transcriptional regulation of N-acetylglucosaminyltransferase V by the src oncogene. J. Biol. Chem. 272, 19575–19581 (1997).
Hatano, K., Miyamoto, Y., Nonomura, N. & Kaneda, Y. Expression of gangliosides, GD1a, and sialyl paragloboside is regulated by NF-κB-dependent transcriptional control of α2,3-sialyltransferase I, II, and VI in human castration-resistant prostate cancer cells. Int. J. Cancer 129, 1838–1847 (2011).
Pinho, S. S. et al. Loss and recovery of Mgat3 and GnT-III Mediated E-cadherin N-glycosylation is a mechanism involved in epithelial-mesenchymal-epithelial transitions. PLoS ONE 7, e33191 (2012).
Schietinger, A. et al. A mutant chaperone converts a wild-type protein into a tumor-specific antigen. Science 314, 304–308 (2006).
Aryal, R. P., Ju, T. & Cummings, R. D. The endoplasmic reticulum chaperone Cosmc directly promotes in vitro folding of T-synthase. J. Biol. Chem. 285, 2456–2462 (2010).
Kakugawa, Y. et al. Up-regulation of plasma membrane-associated ganglioside sialidase (Neu3) in human colon cancer and its involvement in apoptosis suppression. Proc. Natl Acad. Sci. USA 99, 10718–10723 (2002).
Kumamoto, K. et al. Increased expression of UDP-galactose transporter messenger RNA in human colon cancer tissues and its implication in synthesis of Thomsen-Friedenreich antigen and sialyl Lewis A/X determinants. Cancer Res. 61, 4620–4627 (2001).
Kellokumpu, S., Sormunen, R. & Kellokumpu, I. Abnormal glycosylation and altered Golgi structure in colorectal cancer: dependence on intra-Golgi pH. FEBS Lett. 516, 217–224 (2002).
Gill, D. J., Chia, J., Senewiratne, J. & Bard, F. Regulation of O-glycosylation through Golgi-to-ER relocation of initiation enzymes. J. Cell Biol. 189, 843–858 (2010).
Brockhausen, I. Mucin-type O-glycans in human colon and breast cancer: glycodynamics and functions. EMBO Rep. 7, 599–604 (2006).
Marcos, N. T. et al. Role of the human ST6GalNAc-I and ST6GalNAc-II in the synthesis of the cancer-associated sialyl-Tn antigen. Cancer Res. 64, 7050–7057 (2004). This study demonstrates that ST6GalNAc-I is responsible for the biosynthesis of the STn antigen in gastric cancer cells.
Roth, J., Wang, Y., Eckhardt, A. E. & Hill, R. L. Subcellular localization of the UDP-N-acetyl-d-galactosamine: polypeptide N-acetylgalactosaminyltransferase-mediated O-glycosylation reaction in the submaxillary gland. Proc. Natl Acad. Sci. USA 91, 8935–8939 (1994).
Sewell, R. et al. The ST6GalNAc-I sialyltransferase localizes throughout the Golgi and is responsible for the synthesis of the tumor-associated sialyl-Tn O-glycan in human breast cancer. J. Biol. Chem. 281, 3586–3594 (2006).
Christiansen, M. N. et al. Cell surface protein glycosylation in cancer. Proteomics 14, 525–546 (2014).
Arnold, J. N., Saldova, R., Hamid, U. M. & Rudd, P. M. Evaluation of the serum N-linked glycome for the diagnosis of cancer and chronic inflammation. Proteomics 8, 3284–3293 (2008).
Kim, Y. J. & Varki, A. Perspectives on the significance of altered glycosylation of glycoproteins in cancer. Glycoconj. J. 14, 569–576 (1997).
Dall'Olio, F. & Chiricolo, M. Sialyltransferases in cancer. Glycoconj. J. 18, 841–850 (2001).
Lise, M. et al. Clinical correlations of α2,6-sialyltransferase expression in colorectal cancer patients. Hybridoma 19, 281–286 (2000).
Amado, M., Carneiro, F., Seixas, M., Clausen, H. & Sobrinho-Simoes, M. Dimeric sialyl-Lex expression in gastric carcinoma correlates with venous invasion and poor outcome. Gastroenterology 114, 462–470 (1998).
Baldus, S. E. et al. Histopathological subtypes and prognosis of gastric cancer are correlated with the expression of mucin-associated sialylated antigens: Sialosyl-Lewisa, Sialosyl-Lewisx and sialosyl-Tn. Tumour Biol. 19, 445–453 (1998).
Rosen, S. D. & Bertozzi, C. R. The selectins and their ligands. Curr. Opin. Cell Biol. 6, 663–673 (1994).
Nakamori, S. et al. Increased expression of sialyl Lewisx antigen correlates with poor survival in patients with colorectal carcinoma: clinicopathological and immunohistochemical study. Cancer Res. 53, 3632–3637 (1993).
Borsig, L. et al. Heparin and cancer revisited: mechanistic connections involving platelets, P-selectin, carcinoma mucins, and tumor metastasis. Proc. Natl Acad. Sci. USA 98, 3352–3357 (2001).
Locker, G. Y. et al. ASCO 2006 update of recommendations for the use of tumor markers in gastrointestinal cancer. J. Clin. Oncol. 24, 5313–5327 (2006).
Marrelli, D. et al. Preoperative positivity of serum tumor markers is a strong predictor of hematogenous recurrence of gastric cancer. J. Surg. Oncol. 78, 253–258 (2001).
Tanaka, F. et al. Prognostic significance of polysialic acid expression in resected non-small cell lung cancer. Cancer Res. 61, 1666–1670 (2001).
Falconer, R. A., Errington, R. J., Shnyder, S. D., Smith, P. J. & Patterson, L. H. Polysialyltransferase: a new target in metastatic cancer. Curr. Cancer Drug Targets 12, 925–939 (2012).
Todeschini, A. R., Dos Santos, J. N., Handa, K. & Hakomori, S. I. Ganglioside GM2-tetraspanin CD82 complex inhibits met and its cross-talk with integrins, providing a basis for control of cell motility through glycosynapse. J. Biol. Chem. 282, 8123–8133 (2007).
Carvalho, A. S. et al. Differential expression of α-2,3-sialyltransferases and α-1,3/4-fucosyltransferases regulates the levels of sialyl Lewis a and sialyl Lewis x in gastrointestinal carcinoma cells. Int. J. Biochem. Cell Biol. 42, 80–89 (2010).
de Vries, T., Knegtel, R. M., Holmes, E. H. & Macher, B. A. Fucosyltransferases: structure/function studies. Glycobiology 11, 119R–128R (2001).
Hiraiwa, N. et al. Transactivation of the fucosyltransferase VII gene by human T-cell leukemia virus type 1 Tax through a variant cAMP-responsive element. Blood 101, 3615–3621 (2003).
Matsuura, N. et al. Gene expression of fucosyl- and sialyl-transferases which synthesize sialyl Lewisx, the carbohydrate ligands for E-selectin, in human breast cancer. Int. J. Oncol. 12, 1157–1164 (1998).
Holmes, E. H., Hakomori, S. & Ostrander, G. K. Synthesis of type 1 and 2 lacto series glycolipid antigens in human colonic adenocarcinoma and derived cell lines is due to activation of a normally unexpressed β1→3N-acetylglucosaminyltransferase. J. Biol. Chem. 262, 15649–15658 (1987).
Marcos, N. T. et al. Helicobacter pylori induces β3GnT5 in human gastric cell lines, modulating expression of the SabA ligand sialyl-Lewis x. J. Clin. Invest. 118, 2325–2336 (2008).
Magalhaes, A. et al. Helicobacter pylori chronic infection and mucosal inflammation switches the human gastric glycosylation pathways. Biochim. Biophys. Acta 1852, 1928–1939 (2015).
Trinchera, M. et al. The biosynthesis of the selectin-ligand sialyl Lewis x in colorectal cancer tissues is regulated by fucosyltransferase VI and can be inhibited by an RNA interference-based approach. Int. J. Biochem. Cell Biol. 43, 130–139 (2011).
Liu, Y. C. et al. Sialylation and fucosylation of epidermal growth factor receptor suppress its dimerization and activation in lung cancer cells. Proc. Natl Acad. Sci. USA 108, 11332–11337 (2011).
Potapenko, I. O. et al. Glycan gene expression signatures in normal and malignant breast tissue; possible role in diagnosis and progression. Mol. Oncol. 4, 98–118 (2010).
Hutchinson, W. L., Du, M. Q., Johnson, P. J. & Williams, R. Fucosyltransferases: differential plasma and tissue alterations in hepatocellular carcinoma and cirrhosis. Hepatology 13, 683–688 (1991).
Sato, Y. et al. Early recognition of hepatocellular carcinoma based on altered profiles of alpha-fetoprotein. N. Engl. J. Med. 328, 1802–1806 (1993). This study revealed the capacity of α-fetoprotein L3 and α-fetoprotein P4+P5 in serum to act as predictive markers to differentiate HCC from cirrhosis.
Takahashi, M., Kuroki, Y., Ohtsubo, K. & Taniguchi, N. Core fucose and bisecting GlcNAc, the direct modifiers of the N-glycan core: their functions and target proteins. Carbohydr. Res. 344, 1387–1390 (2009).
Dennis, J. W., Laferte, S., Waghorne, C., Breitman, M. L. & Kerbel, R. S. Beta 1–6 branching of Asn-linked oligosaccharides is directly associated with metastasis. Science 236, 582–585 (1987). This study reported that increased expression of β1–6-linked branching oligosaccharide structures is directly related to the metastatic potential of the cells.
Di Lella, S. et al. When galectins recognize glycans: from biochemistry to physiology and back again. Biochemistry 50, 7842–7857 (2011).
Croci, D. O. et al. Glycosylation-dependent lectin-receptor interactions preserve angiogenesis in anti-VEGF refractory tumors. Cell 156, 744–758 (2014). This article describes a glycosylation-dependent pathway that preserves angiogenesis in anti-VEGF refractory tumours.
Demetriou, M., Nabi, I. R., Coppolino, M., Dedhar, S. & Dennis, J. W. Reduced contact-inhibition and substratum adhesion in epithelial cells expressing GlcNAc-transferase V. J. Cell Biol. 130, 383–392 (1995).
Seberger, P. J. & Chaney, W. G. Control of metastasis by Asn-linked, β1–6 branched oligosaccharides in mouse mammary cancer cells. Glycobiology 9, 235–241 (1999).
Guo, H. B. et al. Specific posttranslational modification regulates early events in mammary carcinoma formation. Proc. Natl Acad. Sci. USA 107, 21116–21121 (2010).
Granovsky, M. et al. Suppression of tumor growth and metastasis in Mgat5-deficient mice. Nat. Med. 6, 306–312 (2000). This study reports the establishment of mice deficient in Mgat5 by targeted gene mutation. Mammary tumour growth and metastases induced by the polyomavirus middle T oncogene were considerably suppressed in Mgat5−/− mice compared with in transgenic littermates expressing Mgat5.
Guo, H., Nagy, T. & Pierce, M. Post-translational glycoprotein modifications regulate colon cancer stem cells and colon adenoma progression in Apcmin/+ mice through altered Wnt receptor signaling. J. Biol. Chem. 289, 31534–31549 (2014).
Yoshimura, M., Nishikawa, A., Ihara, Y., Taniguchi, S. & Taniguchi, N. Suppression of lung metastasis of B16 mouse melanoma by N-acetylglucosaminyltransferase III gene transfection. Proc. Natl Acad. Sci. USA 92, 8754–8758 (1995). This article provides the first demonstration of the tumour-suppressive role of GnT-III.
Zhao, Y. et al. Branched N-glycans regulate the biological functions of integrins and cadherins. FEBS J. 275, 1939–1948 (2008).
Kudelka, M. R., Ju, T., Heimburg-Molinaro, J. & Cummings, R. D. Simple sugars to complex disease—mucin-type O-glycans in cancer. Adv. Cancer Res. 126, 53–135 (2015).
Berois, N. et al. GALNT9 gene expression is a prognostic marker in neuroblastoma patients. Clin. Chem. 59, 225–233 (2013).
Gomes, J. et al. Expression of UDP-N-acetyl-d-galactosamine: polypeptide N-acetylgalactosaminyltransferase-6 in gastric mucosa, intestinal metaplasia, and gastric carcinoma. J. Histochem. Cytochem. 57, 79–86 (2009).
Gill, D. J. et al. Initiation of GalNAc-type O-glycosylation in the endoplasmic reticulum promotes cancer cell invasiveness. Proc. Natl Acad. Sci. USA 110, E3152–E3161 (2013).
Dalziel, M. et al. The relative activities of the C2GnT1 and ST3Gal-I glycosyltransferases determine O-glycan structure and expression of a tumor-associated epitope on MUC1. J. Biol. Chem. 276, 11007–11015 (2001).
Reis, C. A., David, L., Seixas, M., Burchell, J. & Sobrinho-Simoes, M. Expression of fully and under-glycosylated forms of MUC1 mucin in gastric carcinoma. Int. J. Cancer 79, 402–410 (1998).
Itzkowitz, S. et al. Expression of Tn, sialosyl Tn, and T antigens in human pancreas. Gastroenterology 100, 1691–1700 (1991).
Radhakrishnan, P. et al. Immature truncated O-glycophenotype of cancer directly induces oncogenic features. Proc. Natl Acad. Sci. USA 111, E4066–E4075 (2014).
Pinho, S. et al. Biological significance of cancer-associated sialyl-Tn antigen: modulation of malignant phenotype in gastric carcinoma cells. Cancer Lett. 249, 157–170 (2007).
David, L., Nesland, J. M., Clausen, H., Carneiro, F. & Sobrinho-Simoes, M. Simple mucin-type carbohydrate antigens (Tn, sialosyl-Tn and T) in gastric mucosa, carcinomas and metastases. APMIS Suppl. 27, 162–172 (1992).
Dall'Olio, F., Malagolini, N., Trinchera, M. & Chiricolo, M. Mechanisms of cancer-associated glycosylation changes. Front. Biosci. (Landmark Ed.) 17, 670–699 (2012).
Ferreira, J. A. et al. Overexpression of tumour-associated carbohydrate antigen sialyl-Tn in advanced bladder tumours. Mol. Oncol. 7, 719–731 (2013).
Ricardo, S. et al. Detection of glyco-mucin profiles improves specificity of MUC16 and MUC1 biomarkers in ovarian serous tumours. Mol. Oncol. 9, 503–512 (2015).
Ju, T. & Cummings, R. D. A unique molecular chaperone Cosmc required for activity of the mammalian core 1 β3-galactosyltransferase. Proc. Natl Acad. Sci. USA 99, 16613–16618 (2002). This study describes the role of the molecular chaperone C1GALT1C1 for activity of the core 1 β3-GalT.
Ju, T. et al. Human tumor antigens Tn and sialyl Tn arise from mutations in Cosmc. Cancer Res. 68, 1636–1646 (2008).
Julien, S. et al. Sialyl-Tn vaccine induces antibody-mediated tumour protection in a relevant murine model. Br. J. Cancer 100, 1746–1754 (2009).
Sandmaier, B. M. et al. Evidence of a cellular immune response against sialyl-Tn in breast and ovarian cancer patients after high-dose chemotherapy, stem cell rescue, and immunization with Theratope STn-KLH cancer vaccine. J. Immunother. 22, 54–66 (1999).
Pinho, S. S. et al. E-cadherin and adherens-junctions stability in gastric carcinoma: functional implications of glycosyltransferases involving N-glycan branching biosynthesis, N-acetylglucosaminyltransferases III and V. Biochim. Biophys. Acta 1830, 2690–2700 (2013). This article reports the biological significance of GnT-III and GnT-V in the modulation of E-cadherin-mediated cell–cell adhesion in cancer.
Pinho, S. S. et al. The role of N-acetylglucosaminyltransferase III and V in the post-transcriptional modifications of E-cadherin. Hum. Mol. Genet. 18, 2599–2608 (2009).
Takeuchi, H. & Haltiwanger, R. S. Significance of glycosylation in Notch signaling. Biochem. Biophys. Res. Commun. 453, 235–242 (2014).
Boscher, C., Dennis, J. W. & Nabi, I. R. Glycosylation, galectins and cellular signaling. Curr. Opin. Cell Biol. 23, 383–392 (2011).
de-Freitas-Junior, J. C. et al. Insulin/IGF-I signaling pathways enhances tumor cell invasion through bisecting GlcNAc N-glycans modulation. an interplay with E-cadherin. PLoS ONE 8, e81579 (2013).
Gomes, C. et al. Expression of ST3GAL4 leads to SLex expression and induces c-Met activation and an invasive phenotype in gastric carcinoma cells. PLoS ONE 8, e66737 (2013).
Dennis, J. W., Nabi, I. R. & Demetriou, M. Metabolism, cell surface organization, and disease. Cell 139, 1229–1241 (2009).
Bassaganas, S. et al. Pancreatic cancer cell glycosylation regulates cell adhesion and invasion through the modulation of α2β1 integrin and E-cadherin function. PLoS ONE 9, e98595 (2014).
Helenius, A. & Aebi, M. Intracellular functions of N-linked glycans. Science 291, 2364–2369 (2001).
Pinho, S. S. et al. Modulation of E-cadherin function and dysfunction by N-glycosylation. Cell. Mol. Life Sci. 68, 1011–1020 (2011).
Paredes, J. et al. Epithelial E- and P-cadherins: role and clinical significance in cancer. Biochim. Biophys. Acta 1826, 297–311 (2012).
Liwosz, A., Lei, T. & Kukuruzinska, M. A. N-glycosylation affects the molecular organization and stability of E-cadherin junctions. J. Biol. Chem. 281, 23138–23149 (2006).
Guo, H. B., Lee, I., Kamar, M. & Pierce, M. N-acetylglucosaminyltransferase V expression levels regulate cadherin-associated homotypic cell–cell adhesion and intracellular signaling pathways. J. Biol. Chem. 278, 52412–52424 (2003).
Ihara, S. et al. Prometastatic effect of N-acetylglucosaminyltransferase V is due to modification and stabilization of active matriptase by adding β1–6 GlcNAc branching. J. Biol. Chem. 277, 16960–16967 (2002).
Carvalho, S. et al. Preventing E-cadherin aberrant N-glycosylation at Asn-554 improves its critical function in gastric cancer. Oncogene http://dx.doi.org/10.1038/onc.2015.225 (2015).
Yoshimura, M., Ihara, Y., Matsuzawa, Y. & Taniguchi, N. Aberrant glycosylation of E-cadherin enhances cell-cell binding to suppress metastasis. J. Biol. Chem. 271, 13811–13815 (1996).
Kitada, T. et al. The addition of bisecting N-acetylglucosamine residues to E-cadherin down-regulates the tyrosine phosphorylation of beta-catenin. J. Biol. Chem. 276, 475–480 (2001).
Xu, Q. et al. Roles of N-acetylglucosaminyltransferase III in epithelial-to-mesenchymal transition induced by transforming growth factor β1 (TGF-β1) in epithelial cell lines. J. Biol. Chem. 287, 16563–16574 (2012).
Gu, J. et al. A mutual regulation between cell-cell adhesion and N-glycosylation: implication of the bisecting GlcNAc for biological functions. J. Proteome Res. 8, 431–435 (2009).
Dennis, J. W., Granovsky, M. & Warren, C. E. Glycoprotein glycosylation and cancer progression. Biochim. Biophys. Acta 1473, 21–34 (1999).
Pinho, S. S., Reis, C. A., Gartner, F. & Alpaugh, M. L. Molecular plasticity of E-cadherin and sialyl lewis x expression, in two comparative models of mammary tumorigenesis. PLoS ONE 4, e6636 (2009).
Seidenfaden, R., Krauter, A., Schertzinger, F., Gerardy-Schahn, R. & Hildebrandt, H. Polysialic acid directs tumor cell growth by controlling heterophilic neural cell adhesion molecule interactions. Mol. Cell. Biol. 23, 5908–5918 (2003). This study demonstrates the role of polysialic acid on neural cell adhesion molecule in cancer cells.
Lin, S., Kemmner, W., Grigull, S. & Schlag, P. M. Cell surface α2,6 sialylation affects adhesion of breast carcinoma cells. Exp. Cell Res. 276, 101–110 (2002).
Tamura, F. et al. RNAi-mediated gene silencing of ST6GalNAc I suppresses the metastatic potential in gastric cancer cells. Gastric Cancer http://dx.doi.org/10.1007/s10120-014-0454-z (2014).
Kim, S. H., Turnbull, J. & Guimond, S. Extracellular matrix and cell signalling: the dynamic cooperation of integrin, proteoglycan and growth factor receptor. J. Endocrinol. 209, 139–151 (2011).
Sarrazin, S., Lamanna, W. C. & Esko, J. D. Heparan sulfate proteoglycans. Cold Spring Harb. Perspect. Biol. 3, a004952 (2011).
Wade, A. et al. Proteoglycans and their roles in brain cancer. FEBS J. 280, 2399–2417 (2013).
Cecchi, F. et al. Targeted disruption of heparan sulfate interaction with hepatocyte and vascular endothelial growth factors blocks normal and oncogenic signaling. Cancer Cell 22, 250–262 (2012).
Tan, K. W. et al. Neutrophils contribute to inflammatory lymphangiogenesis by increasing VEGF-A bioavailability and secreting VEGF-D. Blood 122, 3666–3677 (2013).
Gunthert, U. et al. A new variant of glycoprotein CD44 confers metastatic potential to rat carcinoma cells. Cell 65, 13–24 (1991).
da Cunha, C. B. et al. De novo expression of CD44 variants in sporadic and hereditary gastric cancer. Lab. Invest. 90, 1604–1614 (2010).
English, N. M., Lesley, J. F. & Hyman, R. Site-specific de-N-glycosylation of CD44 can activate hyaluronan binding, and CD44 activation states show distinct threshold densities for hyaluronan binding. Cancer Res. 58, 3736–3742 (1998).
Katoh, S., Zheng, Z., Oritani, K., Shimozato, T. & Kincade, P. W. Glycosylation of CD44 negatively regulates its recognition of hyaluronan. J. Exp. Med. 182, 419–429 (1995).
Goupille, C., Hallouin, F., Meflah, K. & Le Pendu, J. Increase of rat colon carcinoma cells tumorigenicity by α(1–2) fucosyltransferase gene transfection. Glycobiology 7, 221–229 (1997).
Wolff, E. A. et al. Generation of artificial proteoglycans containing glycosaminoglycan-modified CD44. Demonstration of the interaction between rantes and chondroitin sulfate. J. Biol. Chem. 274, 2518–2524 (1999).
Roucourt, B., Meeussen, S., Bao, J., Zimmermann, P. & David, G. Heparanase activates the syndecan-syntenin-ALIX exosome pathway. Cell Res. 25, 412–428 (2015).
Bharadwaj, A. G. et al. Spontaneous metastasis of prostate cancer is promoted by excess hyaluronan synthesis and processing. Am. J. Pathol. 174, 1027–1036 (2009).
Paszek, M. J. et al. The cancer glycocalyx mechanically primes integrin-mediated growth and survival. Nature 511, 319–325 (2014).
Liotta, L. A. Tumor invasion and metastases—role of the extracellular matrix: Rhoads Memorial Award lecture. Cancer Res. 46, 1–7 (1986).
Jin, H. & Varner, J. Integrins: roles in cancer development and as treatment targets. Br. J. Cancer 90, 561–565 (2004).
Asada, M., Furukawa, K., Segawa, K., Endo, T. & Kobata, A. Increased expression of highly branched N-glycans at cell surface is correlated with the malignant phenotypes of mouse tumor cells. Cancer Res. 57, 1073–1080 (1997).
Guo, H. B., Lee, I., Kamar, M., Akiyama, S. K. & Pierce, M. Aberrant N-glycosylation of β1 integrin causes reduced α5β1 integrin clustering and stimulates cell migration. Cancer Res. 62, 6837–6845 (2002).
Pochec, E. et al. Expression of integrins α3β1 and α5β1 and GlcNAc β1,6 glycan branching influences metastatic melanoma cell migration on fibronectin. Eur. J. Cell Biol. 92, 355–362 (2013).
Isaji, T. et al. Introduction of bisecting GlcNAc into integrin α5β1 reduces ligand binding and down-regulates cell adhesion and cell migration. J. Biol. Chem. 279, 19747–19754 (2004).
Zhao, Y. et al. N-acetylglucosaminyltransferase III antagonizes the effect of N-acetylglucosaminyltransferase V on α3β1 integrin-mediated cell migration. J. Biol. Chem. 281, 32122–32130 (2006).
Gu, J. & Taniguchi, N. Regulation of integrin functions by N-glycans. Glycoconj. J. 21, 9–15 (2004).
Dennis, J., Waller, C., Timpl, R. & Schirrmacher, V. Surface sialic acid reduces attachment of metastatic tumour cells to collagen type IV and fibronectin. Nature 300, 274–276 (1982).
Seales, E. C. et al. Hypersialylation of β1 integrins, observed in colon adenocarcinoma, may contribute to cancer progression by up-regulating cell motility. Cancer Res. 65, 4645–4652 (2005).
Kariya, Y., Kawamura, C., Tabei, T. & Gu, J. Bisecting GlcNAc residues on laminin-332 down-regulate galectin-3-dependent keratinocyte motility. J. Biol. Chem. 285, 3330–3340 (2010).
Ranjan, A., Bane, S. M. & Kalraiya, R. D. Glycosylation of the laminin receptor (α3β1) regulates its association with tetraspanin CD151: impact on cell spreading, motility, degradation and invasion of basement membrane by tumor cells. Exp. Cell Res. 322, 249–264 (2014).
Vlodavsky, I. & Friedmann, Y. Molecular properties and involvement of heparanase in cancer metastasis and angiogenesis. J. Clin. Invest. 108, 341–347 (2001).
Lendorf, M. E., Manon-Jensen, T., Kronqvist, P., Multhaupt, H. A. & Couchman, J. R. Syndecan-1 and syndecan-4 are independent indicators in breast carcinoma. J. Histochem. Cytochem. 59, 615–629 (2011).
Saoncella, S. et al. Syndecan-4 signals cooperatively with integrins in a Rho-dependent manner in the assembly of focal adhesions and actin stress fibers. Proc. Natl Acad. Sci. USA 96, 2805–2810 (1999). This article describes how a proteoglycan cooperates with integrins interfering with focal adhesions and actin stress fibres.
Beauvais, D. M., Burbach, B. J. & Rapraeger, A. C. The syndecan-1 ectodomain regulates αvβ3 integrin activity in human mammary carcinoma cells. J. Cell Biol. 167, 171–181 (2004).
Warburg, O. On the origin of cancer cells. Science 123, 309–314 (1956).
Marshall, S., Bacote, V. & Traxinger, R. R. Discovery of a metabolic pathway mediating glucose-induced desensitization of the glucose transport system. Role of hexosamine biosynthesis in the induction of insulin resistance. J. Biol. Chem. 266, 4706–4712 (1991).
Wells, L., Vosseller, K. & Hart, G. W. Glycosylation of nucleocytoplasmic proteins: signal transduction and O-GlcNAc. Science 291, 2376–2378 (2001).
Slawson, C., Copeland, R. J. & Hart, G. W. O-GlcNAc signaling: a metabolic link between diabetes and cancer? Trends Biochem. Sci. 35, 547–555 (2010).
Ferrer, C. M. et al. O-GlcNAcylation regulates cancer metabolism and survival stress signaling via regulation of the HIF-1 pathway. Mol. Cell 54, 820–831 (2014).
Ma, Z. & Vosseller, K. Cancer metabolism and elevated O-GlcNAc in oncogenic signaling. J. Biol. Chem. 289, 34457–34465 (2014).
Caldwell, S. A. et al. Nutrient sensor O-GlcNAc transferase regulates breast cancer tumorigenesis through targeting of the oncogenic transcription factor FoxM1. Oncogene 29, 2831–2842 (2010).
Zachara, N. E. & Hart, G. W. Cell signaling, the essential role of O-GlcNAc! Biochim. Biophys. Acta 1761, 599–617 (2006).
Lynch, T. P. et al. Critical role of O-linked β-N-acetylglucosamine transferase in prostate cancer invasion, angiogenesis, and metastasis. J. Biol. Chem. 287, 11070–11081 (2012).
Zhu, W., Leber, B. & Andrews, D. W. Cytoplasmic O-glycosylation prevents cell surface transport of E-cadherin during apoptosis. EMBO J. 20, 5999–6007 (2001).
Hart, G. W., Slawson, C., Ramirez-Correa, G. & Lagerlof, O. Cross talk between O-GlcNAcylation and phosphorylation: roles in signaling, transcription, and chronic disease. Annu. Rev. Biochem. 80, 825–858 (2011).
Itkonen, H. M. et al. O-GlcNAc transferase integrates metabolic pathways to regulate the stability of c-MYC in human prostate cancer cells. Cancer Res. 73, 5277–5287 (2013).
Yang, W. H. et al. Modification of p53 with O-linked N-acetylglucosamine regulates p53 activity and stability. Nat. Cell Biol. 8, 1074–1083 (2006).
Lau, K. S. et al. Complex N-glycan number and degree of branching cooperate to regulate cell proliferation and differentiation. Cell 129, 123–134 (2007).
Stanley, P. A method to the madness of N-glycan complexity? Cell 129, 27–29 (2007).
Taniguchi, N. A sugar-coated switch for cellular growth and arrest. Nat. Chem. Biol. 3, 307–309 (2007).
Partridge, E. A. et al. Regulation of cytokine receptors by Golgi N-glycan processing and endocytosis. Science 306, 120–124 (2004).
Guo, H. B., Johnson, H., Randolph, M., Lee, I. & Pierce, M. Knockdown of GnT-Va expression inhibits ligand-induced downregulation of the epidermal growth factor receptor and intracellular signaling by inhibiting receptor endocytosis. Glycobiology 19, 547–559 (2009).
Song, Y., Aglipay, J. A., Bernstein, J. D., Goswami, S. & Stanley, P. The bisecting GlcNAc on N-glycans inhibits growth factor signaling and retards mammary tumor progression. Cancer Res. 70, 3361–3371 (2010).
Sato, Y. et al. Overexpression of N-acetylglucosaminyltransferase III enhances the epidermal growth factor-induced phosphorylation of ERK in HeLaS3 cells by up-regulation of the internalization rate of the receptors. J. Biol. Chem. 276, 11956–11962 (2001).
Bremer, E. G. & Hakomori, S. Gangliosides as receptor modulators. Adv. Exp. Med. Biol. 174, 381–394 (1984).
Park, S. Y., Yoon, S. J., Freire- de-Lima, L., Kim, J. H. & Hakomori, S. I. Control of cell motility by interaction of gangliosides, tetraspanins, and epidermal growth factor receptor in A431 versus KB epidermoid tumor cells. Carbohydr. Res. 344, 1479–1486 (2009).
Birks, S. M. et al. Targeting the GD3 acetylation pathway selectively induces apoptosis in glioblastoma. Neuro Oncol. 13, 950–960 (2011).
Rabinovich, G. A. & Toscano, M. A. Turning 'sweet' on immunity: galectin–glycan interactions in immune tolerance and inflammation. Nat. Rev. Immunol. 9, 338–352 (2009).
Macauley, M. S., Crocker, P. R. & Paulson, J. C. Siglec-mediated regulation of immune cell function in disease. Nat. Rev. Immunol. 14, 653–666 (2014).
Ragupathi, G. et al. Antibodies against tumor cell glycolipids and proteins, but not mucins, mediate complement-dependent cytotoxicity. J. Immunol. 174, 5706–5712 (2005).
Lavrsen, K. et al. Aberrantly glycosylated MUC1 is expressed on the surface of breast cancer cells and a target for antibody-dependent cell-mediated cytotoxicity. Glycoconj. J. 30, 227–236 (2013).
Samsen, A. et al. DC-SIGN and SRCL bind glycans of carcinoembryonic antigen (CEA) and CEA-related cell adhesion molecule 1 (CEACAM1): recombinant human glycan-binding receptors as analytical tools. Eur. J. Cell Biol. 89, 87–94 (2010).
Saeland, E. et al. The C-type lectin MGL expressed by dendritic cells detects glycan changes on MUC1 in colon carcinoma. Cancer Immunol. Immunother. 56, 1225–1236 (2007).
Laubli, H. et al. Lectin galactoside-binding soluble 3 binding protein (LGALS3BP) is a tumor-associated immunomodulatory ligand for CD33-related Siglecs. J. Biol. Chem. 289, 33481–33491 (2014).
Liu, F. T. & Rabinovich, G. A. Galectins as modulators of tumour progression. Nat. Rev. Cancer 5, 29–41 (2005).
Thijssen, V. L., Heusschen, R., Caers, J. & Griffioen, A. W. Galectin expression in cancer diagnosis and prognosis: a systematic review. Biochim. Biophys. Acta 1855, 235–247 (2015).
Dalziel, M., Crispin, M., Scanlan, C. N., Zitzmann, N. & Dwek, R. A. Emerging principles for the therapeutic exploitation of glycosylation. Science 343, 1235681 (2014). Addresses the potential of glycans to be an important source for the development of novel targeted therapeutic strategies.
Slovin, S. F. et al. Carbohydrate vaccines in cancer: immunogenicity of a fully synthetic globo H hexasaccharide conjugate in man. Proc. Natl Acad. Sci. USA 96, 5710–5715 (1999).
Buskas, T., Thompson, P. & Boons, G. J. Immunotherapy for cancer: synthetic carbohydrate-based vaccines. Chem Commun. 2009, 5335–5349 (2009).
Li, M., Song, L. & Qin, X. Glycan changes: cancer metastasis and anti-cancer vaccines. J. Biosci. 35, 665–673 (2010).
Beatson, R. E., Taylor-Papadimitriou, J. & Burchell, J. M. MUC1 immunotherapy. Immunotherapy 2, 305–327 (2010).
Mackall, C. L., Merchant, M. S. & Fry, T. J. Immune-based therapies for childhood cancer. Nat. Rev. Clin. Oncol. 11, 693–703 (2014).
Liu, S. D. et al. Afucosylated antibodies increase activation of FcγRIIIa-dependent signaling components to intensify processes promoting ADCC. Cancer Immunol. Res. 3, 173–183 (2015).
Gilgunn, S., Conroy, P. J., Saldova, R., Rudd, P. M. & O'Kennedy, R. J. Aberrant PSA glycosylation — a sweet predictor of prostate cancer. Nat. Rev. Urol. 10, 99–107 (2013). Describes the potential of altered PSA-glycosylation patterns to be used as a reliable diagnostic tool in discriminating between significant and insignificant prostate cancers.
Zurawski, V. R. Jr, Orjaseter, H., Andersen, A. & Jellum, E. Elevated serum CA 125 levels prior to diagnosis of ovarian neoplasia: relevance for early detection of ovarian cancer. Int. J. Cancer 42, 677–680 (1988).
Goldstein, M. J. & Mitchell, E. P. Carcinoembryonic antigen in the staging and follow-up of patients with colorectal cancer. Cancer Invest. 23, 338–351 (2005).
Ebeling, F. G. et al. Serum CEA and CA 15–13 as prognostic factors in primary breast cancer. Br. J. Cancer 86, 1217–1222 (2002).
Kumpulainen, E. J., Keskikuru, R. J. & Johansson, R. T. Serum tumor marker CA 15.3 and stage are the two most powerful predictors of survival in primary breast cancer. Breast Cancer Res. Treat. 76, 95–102 (2002).
Safi, F., Schlosser, W., Kolb, G. & Beger, H. G. Diagnostic value of CA 19–19 in patients with pancreatic cancer and nonspecific gastrointestinal symptoms. J. Gastrointest. Surg. 1, 106–112 (1997).
Fukushima, K., Satoh, T., Baba, S. & Yamashita, K. α1,2-fucosylated and β-N-acetylgalactosaminylated prostate-specific antigen as an efficient marker of prostatic cancer. Glycobiology 20, 452–460 (2010).
Jankovic, M. M. & Milutinovic, B. S. Glycoforms of CA125 antigen as a possible cancer marker. Cancer Biomark. 4, 35–42 (2008).
Saeland, E. et al. Differential glycosylation of MUC1 and CEACAM5 between normal mucosa and tumour tissue of colon cancer patients. Int. J. Cancer 131, 117–128 (2012).
Noda, K. et al. Gene expression of α1-6 fucosyltransferase in human hepatoma tissues: a possible implication for increased fucosylation of α-fetoprotein. Hepatology 28, 944–952 (1998).
Wang, M. et al. Novel fucosylated biomarkers for the early detection of hepatocellular carcinoma. Cancer Epidemiol. Biomarkers Prev. 18, 1914–1921 (2009).
Adamczyk, B., Tharmalingam, T. & Rudd, P. M. Glycans as cancer biomarkers. Biochim. Biophys. Acta 1820, 1347–1353 (2012).
Steentoft, C. et al. Mining the O-glycoproteome using zinc-finger nuclease-glycoengineered SimpleCell lines. Nat. Methods 8, 977–982 (2011). Describes the development of the SimpleCell strategy using zinc-finger nucleases for the characterization of the O -glycoproteome of cancer cells.
Campos, D. et al. Probing the O-glycoproteome of gastric cancer cell lines for biomarker discovery. Mol. Cell. Proteomics 14, 1616–1629 (2015). Details the characterization of the O -glycoproteome of gastric cancer cells and serum from patients with gastric cancer.
Lauc, G. et al. Genomics meets glycomics — the first GWAS study of human N-glycome identifies HNF1α as a master regulator of plasma protein fucosylation. PLoS Genet. 6, e1001256 (2010).
Miyoshi, E. & Nakano, M. Fucosylated haptoglobin is a novel marker for pancreatic cancer: detailed analyses of oligosaccharide structures. Proteomics 8, 3257–3262 (2008).
Gomes, C. et al. Glycoproteomic analysis of serum from patients with gastric precancerous lesions. J. Proteome Res. 12, 1454–1466 (2013).
Saldova, R., Fan, Y., Fitzpatrick, J. M., Watson, R. W. & Rudd, P. M. Core fucosylation and α2-3 sialylation in serum N-glycome is significantly increased in prostate cancer comparing to benign prostate hyperplasia. Glycobiology 21, 195–205 (2011).
Melo, S. A. et al. Glypican-1 identifies cancer exosomes and detects early pancreatic cancer. Nature 523, 177–182 (2015).
Blixt, O. et al. Autoantibodies to aberrantly glycosylated MUC1 in early stage breast cancer are associated with a better prognosis. Breast Cancer Res. 13, R25 (2011).
Pedersen, J. W. et al. Cancer-associated autoantibodies to MUC1 and MUC4 — a blinded case-control study of colorectal cancer in UK collaborative trial of ovarian cancer screening. Int. J. Cancer 134, 2180–2188 (2014).
Moloney, D. J. et al. Mammalian Notch1 is modified with two unusual forms of O-linked glycosylation found on epidermal growth factor-like modules. J. Biol. Chem. 275, 9604–9611 (2000).
Panin, V. M., Papayannopoulos, V., Wilson, R. & Irvine, K. D. Fringe modulates Notch-ligand interactions. Nature 387, 908–912 (1997).
Cohen, B. et al. Fringe boundaries coincide with Notch-dependent patterning centres in mammals and alter Notch-dependent development in Drosophila. Nat. Genet. 16, 283–288 (1997).
Tanaka, H. et al. Acute myelogenous leukemia with PIG-A gene mutation evolved from aplastic anemia-paroxysmal nocturnal hemoglobinuria syndrome. Int. J. Hematol. 73, 206–212 (2001).
Ilver, D. et al. Helicobacter pylori adhesin binding fucosylated histo-blood group antigens revealed by retagging. Science 279, 373–377 (1998).
Mahdavi, J. et al. Helicobacter pylori SabA adhesin in persistent infection and chronic inflammation. Science 297, 573–578 (2002).
Magalhaes, A., Ismail, M. N. & Reis, C. A. Sweet receptors mediate the adhesion of the gastric pathogen Helicobacter pylori: glycoproteomic strategies. Expert Rev. Proteomics 7, 307–310 (2010).
Sarrats, A. et al. Glycosylation of liver acute-phase proteins in pancreatic cancer and chronic pancreatitis. Proteomics Clin. Appl. 4, 432–448 (2010).
Dias, A. M. et al. Dysregulation of T cell receptor N-glycosylation: a molecular mechanism involved in ulcerative colitis. Hum. Mol. Genet. 23, 2416–2427 (2014).
Samraj, A. N. et al. A red meat-derived glycan promotes inflammation and cancer progression. Proc. Natl Acad. Sci. USA 112, 542–547 (2015).
Chou, H. H. et al. A mutation in human CMP-sialic acid hydroxylase occurred after the Homo-Pan divergence. Proc. Natl Acad. Sci. USA 95, 11751–11756 (1998).
Ychou, M., Duffour, J., Kramar, A., Gourgou, S. & Grenier, J. Clinical significance and prognostic value of CA72-4 compared with CEA and CA19-9 in patients with gastric cancer. Dis. Markers 16, 105–110 (2000).
Valmu, L., Alfthan, H., Hotakainen, K., Birken, S. & Stenman, U. H. Site-specific glycan analysis of human chorionic gonadotropin β-subunit from malignancies and pregnancy by liquid chromatography — electrospray mass spectrometry. Glycobiology 16, 1207–1218 (2006).
Acknowledgements
The Institute of Molecular Pathology and Immunology of the University of Porto integrates the Institute for Research and Innovation in Health, which is partially supported by the Portuguese Foundation for Science and Technology (FCT). This work is funded by the European Regional Development Fund (FEDER) through the Operational Programme for Competitiveness Factors (COMPETE) and by national funds through the FCT, under the projects PEst-C/SAU/LA0003/2013, PTDC/BBB-EBI/0786/2012 and EXPL/BIM-MEC/0149/2012. S.S.P. acknowledges a grant from the FCT (number SFRH/BPD/63094/2009). C.A.R. acknowledges support from the European Union Seventh Framework Programme GastricGlycoExplorer (grant number 316929). The authors apologize that they cannot include all the relevant studies on glycosylation in cancer in this article owing to limitation of space. The authors thank Tiago Fontes-Oliveira for support in figures preparations.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Glycome
-
The entire complement of glycan structures in an organism.
- Anomeric state
-
The configuration (α or β) of the hydroxy group originating from the aldehyde or ketone group after monosaccharide ring closure.
- Sialic acid-binding immunoglobulin-type lectins
-
(Siglecs). Proteins that bind sialic acid.
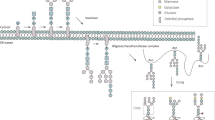
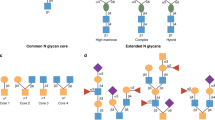
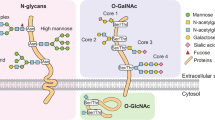
- N-glycans
-
Oligosaccharides covalently linked to an Asp residue of a protein (at the consensus sequence Asn-X-Ser/Thr, in which X is any amino acid) via a nitrogen atom. N-glycans are classified into high-mannose, complex and hybrid types.
- O-glycans
-
Oligosaccharides that are linked to a polypeptide via an oxygen atom. O-glycans are classified according to the initiating monosaccharide linked to a Ser or Thr residue.
- Glycosaminoglycan
-
(GAG). A linear co-polymer containing acidic disaccharide repeating units attached to proteoglycans via xylose linked to the hydroxyl group of a Ser residue8.
- Chondroitin sulfate
-
A GAG chain containing acidic disaccharide repeating units of N-acetylgalactosamine β1-4 glucuronic acid (GlcNAcβ1-4GlcA). The GAG is called dermatan sulfate when the repeating units is N-acetylgalactosamine β1-4 iduronic acid (GlcNAcβ1-4IdoA).
- Heparan sulfate
-
A GAG chain containing acidic disaccharide repeating units of N-acetylgalactosamine α1-4 glucuronic acid or iduronic acid (GlcNAcα1-4GlcA or GlcNAcα1-4IdoA).
- Keratan sulfate
-
A GAG chain containing acidic disaccharide repeating units of galactose 1-β4-N-acetylglucosamine (Galβ1-4GlcNAc).
- Glycosyltransferases
-
Enzymes that catalyse the transfer of saccharides (sugars) from activated donors to acceptor molecules (proteins, lipids or carbohydrates), forming covalent bonds.
- Microdomain
-
A plasma membrane domain containing glycosphingolipids and proteins receptors influencing membrane fluidity, protein assembly and signalling.
- O-GlcNAcylation
-
A covalent addition of N-acetylglucosamine (GlcNAc) to Ser or Thr hydroxyl moieties by O-GlcNAc transferase on nuclear and cytoplasmic proteins.
- Tumour editing
-
Changes in tumour immunogenicity due to the antitumour response of the immune system, leading to emergence of immune-resistant cancer cell variants.
Rights and permissions
About this article
Cite this article
Pinho, S., Reis, C. Glycosylation in cancer: mechanisms and clinical implications. Nat Rev Cancer 15, 540–555 (2015). https://doi.org/10.1038/nrc3982
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrc3982
This article is cited by
-
Glycosylation-related genes mediated prognostic signature contribute to prognostic prediction and treatment options in ovarian cancer: based on bulk and single‑cell RNA sequencing data
BMC Cancer (2024)
-
An N-glycome tissue atlas of 15 human normal and cancer tissue types determined by MALDI-imaging mass spectrometry
Scientific Reports (2024)
-
Inhibition of the galactosyltransferase C1GALT1 reduces osteosarcoma cell proliferation by interfering with ERK signaling and cell cycle progression
Cancer Gene Therapy (2024)
-
Construction of an abnormal glycosylation risk model and its application in predicting the prognosis of patients with head and neck cancer
Scientific Reports (2024)
-
Determination of L-selectin in blood plasma using DNA aptamer–based surface-enhanced Raman spectroscopy assay
Analytical and Bioanalytical Chemistry (2024)