Abstract
To enable sophisticated optogenetic manipulation of neural circuits throughout the nervous system with limited disruption of animal behavior, light-delivery systems beyond fiber optic tethering and large, head-mounted wireless receivers are desirable. We report the development of an easy-to-construct, implantable wireless optogenetic device. Our smallest version (20 mg, 10 mm3) is two orders of magnitude smaller than previously reported wireless optogenetic systems, allowing the entire device to be implanted subcutaneously. With a radio-frequency (RF) power source and controller, this implant produces sufficient light power for optogenetic stimulation with minimal tissue heating (<1 °C). We show how three adaptations of the implant allow for untethered optogenetic control throughout the nervous system (brain, spinal cord and peripheral nerve endings) of behaving mice. This technology opens the door for optogenetic experiments in which animals are able to behave naturally with optogenetic manipulation of both central and peripheral targets.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Aravanis, A.M. et al. An optical neural interface: in vivo control of rodent motor cortex with integrated fiberoptic and optogenetic technology. J. Neural Eng. 4, S143–S156 (2007).
Gradinaru, V. et al. Targeting and readout strategies for fast optical neural control in vitro and in vivo. J. Neurosci. 27, 14231–14238 (2007).
Zhang, J. et al. Integrated device for optical stimulation and spatiotemporal electrical recording of neural activity in light-sensitized brain tissue. J. Neural Eng. 6, 055007 (2009).
Anikeeva, P. et al. Optetrode: a multichannel readout for optogenetic control in freely moving mice. Nat. Neurosci. 15, 163–170 (2012).
Wang, J. et al. Integrated device for combined optical neuromodulation and electrical recording for chronic in vivo applications. J. Neural Eng. 9, 016001 (2012).
Warden, M.R., Cardin, J.A. & Deisseroth, K. Optical neural interfaces. Annu. Rev. Biomed. Eng. 16, 103–129 (2014).
Klorig, D.C. & Godwin, D.W. A magnetic rotary optical fiber connector for optogenetic experiments in freely moving animals. J. Neurosci. Methods 227, 132–139 (2014).
Wentz, C.T. et al. A wirelessly powered and controlled device for optical neural control of freely-behaving animals. J. Neural Eng. 8, 046021 (2011).
Kwon, K.Y., Lee, H.-M., Ghovanloo, M., Weber, A. & Li, W. Design, fabrication, and packaging of an integrated, wirelessly-powered optrode array for optogenetics application. Front. Syst. Neurosci. 9, 69 (2015).
Iwai, Y., Honda, S., Ozeki, H., Hashimoto, M. & Hirase, H. A simple head-mountable LED device for chronic stimulation of optogenetic molecules in freely moving mice. Neurosci. Res. 70, 124–127 (2011).
Hashimoto, M., Hata, A., Miyata, T. & Hirase, H. Programmable wireless light-emitting diode stimulator for chronic stimulation of optogenetic molecules in freely moving mice. Neurophotonics 1, 011002 (2014).
Kim, T.I. et al. Injectable, cellular-scale optoelectronics with applications for wireless optogenetics. Science 340, 211–216 (2013).
McCall, J.G. et al. Fabrication and application of flexible, multimodal light-emitting devices for wireless optogenetics. Nat. Protoc. 8, 2413–2428 (2013).
Lee, S.T. et al. A miniature, fiber-coupled, wireless, deep-brain optogenetic stimulator. IEEE Trans. Neural Syst. Rehabil. Eng. 23, 655–664 (2015).
Carr, F.B. & Zachariou, V. Nociception and pain: lessons from optogenetics. Front. Behav. Neurosci. 8, 69 (2014).
Yeh, A.J. et al. Wirelessly powering miniature implants for optogenetic stimulation. Appl. Phys. Lett. 103, 163701 (2013).
Ho, J.S. et al. Self-tracking energy transfer for neural stimulation in untethered mice. Phys. Rev. Appl. 4, 024001 (2015).
Yizhar, O., Fenno, L.E., Davidson, T.J., Mogri, M. & Deisseroth, K. Optogenetics in neural systems. Neuron 71, 9–34 (2011).
Gordon, C.J. Temperature Regulation in Laboratory Rodents (Cambridge Univ., New York, 1993).
Towne, C., Montgomery, K.L., Iyer, S.M., Deisseroth, K. & Delp, S.L. Optogenetic control of targeted peripheral axons in freely moving animals. PLoS ONE 8, e72691 (2013).
Caggiano, V., Sur, M. & Bizzi, E. Rostro-caudal inhibition of hindlimb movements in the spinal cord of mice. PLoS ONE 9, e100865 (2014).
Lu, C. et al. Polymer fiber probes enable optical control of spinal cord and muscle function in vivo. Adv. Funct. Mater. 24, 6594–6600 (2014).
Iyer, S.M. et al. Virally mediated optogenetic excitation and inhibition of pain in freely moving nontransgenic mice. Nat. Biotechnol. 32, 274–278 (2014).
Nguyen, T.K. et al. Closed-loop optical neural stimulation based on a 32-channel low-noise recording system with online spike sorting. J. Neural Eng. 11, 046005 (2014).
Mattis, J. et al. Principles for applying optogenetic tools derived from direct comparative analysis of microbial opsins. Nat. Methods 9, 159–172 (2012).
Lin, J.Y., Knutsen, P.M., Muller, A., Kleinfeld, D. & Tsien, R.Y. ReaChR: a red-shifted variant of channelrhodopsin enables deep transcranial optogenetic excitation. Nat. Neurosci. 16, 1499–1508 (2013).
Chuong, A.S. et al. Noninvasive optical inhibition with a red-shifted microbial rhodopsin. Nat. Neurosci. 17, 1123–1129 (2014).
Birmingham, K. et al. Bioelectronic medicines: a research roadmap. Nat. Rev. Drug Discov. 13, 399–400 (2014).
Williams, J.C. & Denison, T. From optogenetic technologies to neuromodulation therapies. Sci. Transl. Med. 5, 177ps6 (2013).
Yizhar, O. Optogenetic insights into social behavior function. Biol. Psychiatry 71, 1075–1080 (2012).
Franklin, K.B.J. & Paxinos, G. The Mouse Brain in Stereotaxic Coordinates (Academic Press, San Diego, 1997).
Schindelin, J. et al. Fiji: an open-source platform for biological-image analysis. Nat. Methods 9, 676–682 (2012).
Acknowledgements
We acknowledge support from grants from the US National Institutes of Health (National Institute of Neurological Disorders and Stroke grant R01-NS080954), the US National Science Foundation (ECCS-1351687), the Stanford Bio-X NeuroVentures program and the Stanford Bio-X Interdisciplinary Initiatives Program. K.L.M. was supported by a Stanford Interdisciplinary Graduate Fellowship through the Bio-X program. We thank E. Tanabe for his advice about constructing the resonant cavity; A. Yee for assistance with photographing experimental setups; the Stanford Behavioral and Functional Neuroscience Laboratory for assistance with Rotarod experiments; and the members of the Deisseroth, Delp and Poon labs for useful discussions and assistance with experiments.
Author information
Authors and Affiliations
Contributions
K.L.M., A.J.Y., L.G., S.M.I., K.D., S.L.D. and A.S.Y.P. conceived the project. A.J.Y., J.S.H., Y.T. and A.S.Y.P. designed, built and characterized the wireless power source and designed the receiving coil circuitry. A.J.Y., K.L.M., V.T. and A.S.Y.P. developed the wireless implants for use in the nervous system. L.G., E.A.F., K.L.M., A.J.Y. and V.T. performed brain device experiments. S.M.I. performed and analyzed c-Fos experiments. K.L.M., A.J.Y. and V.T. completed all other experiments and analysis. Experimental work was supervised by K.D., S.L.D. and A.S.Y.P. The manuscript was written by K.L.M. and A.J.Y. with contributions from all authors.
Corresponding author
Ethics declarations
Competing interests
K.L.M., A.J.Y., J.S.H., V.T., S.M.I., L.G., E.A.F., Y.T., K.D., S.L.D. and A.S.Y.P. have disclosed this technology to the Stanford Office of Technology Licensing for potential therapy applications.
Integrated supplementary information
Supplementary Figure 1 Resonant cavity and power source.
(a) Resonant cavity powers a wireless device in a mouse on the surface of the cavity. (b) Total setup: the mouse enclosure above the resonant cavity, resonant cavity, phase shifter, signal generator, amplifier, and fan. (c) Drawing for use with assembling the components (Supplementary Data) of the cavity.
Supplementary Figure 2 Size comparison of fully internal wireless implants.
Devices reported here have the same approximate mass of a black peppercorn and are much smaller than previously reported wireless optogenetic systems (A–E); reported ranges of mass represented by rectangles. A: Wentz, C.T., et al. A wirelessly powered and controlled device for optical neural control of freely-behaving animals. J Neural Eng 8, 046021 (2011). B: Iwai, Y., Honda, S., Ozeki, H., Hashimoto, M. & Hirase, H. A simple head-mountable LED device for chronic stimulation of optogenetic molecules in freely moving mice. Neurosci Res 70, 124–127 (2011). C: Hashimoto, M., Hata, A., Miyata, T. & Hirase, H. Programmable wireless light-emitting diode stimulator for chronic stimulation of optogenetic molecules in freely moving mice. Neurophotonics 1, 011002 (2014). D: Kim, T.I., et al. Injectable, cellular-scale optoelectronics with applications for wireless optogenetics. Science 340, 211–216 (2013). E: Lee, S., et al. A miniature, fiber-coupled, wireless, deep-brain optogenetic stimulator. IEEE Trans Neural Syst Rehabil Eng (2015).
Supplementary Figure 3 Wireless implants for the brain, spinal cord and peripheral nerve endings.
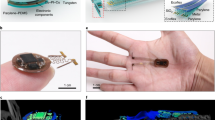
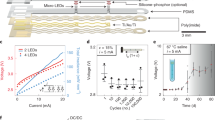
Similar construction is used for all implants, but small design variations are used to customize the implants to different nervous system targets. In brain and peripheral implants, current is delivered to a 250-μm diameter extension made of a pair of magnet wires with a micro-LED attached at the tip. The extension can be inserted in the brain or routed to peripheral nerves. The micro-LED of the brain implant points parallel to the extension axis, whereas that of the peripheral nerve ending implant points perpendicular to the extension axis. Such an extension was not included in the spinal implant to avoid damage to the cord; instead, the LED was mounted directly onto the PCB. A “spinal cord” device could equivalently be used for superficial brain targets. Peripheral implants change spatial orientation relative to the cavity more than central implants during the course of locomotion. Due to this variability in orientation of the peripheral implant, the individual turns of the coil were set to be non-parallel, thus minimizing orientation-related power fluctuations.
Supplementary Figure 4 Step-by-step construction of implants.
(a) Circuit diagram of the rectifier. This circuit converts RF energy received from the implant coil to direct current for the LED. It is a two-stage voltage doubling circuit using Schottky diodes. (b) The printed circuit board (PCB) was cut to size, and solder paste was applied to the metal traces on the PCB. (c) The surface-mount devices (SMD) were bonded with reflow soldering. (d) The power receiving coil was soldered to the PCB. (e) The coil and SMD components were stabilized with acrylic. (f) The extension was formed from a pair of twisted 36 G wires. (g) The ends of the twisted wires were separated by 70 μm. (h) Solder paste was applied to the tips of the bared wires. (i) The LED was placed on the ends of the wires. (j) The extension was positioned for reflow with a butane torch (post-reflow not shown). (k) The extension was cut to desired length and tested for polarity. (l) The extension was soldered to the bottom of the PCB. (m) The extension was bent to the desired angle and a final coat of acrylic was applied. Scale bars: black, 1 mm; white, 0.5 mm.
Supplementary Figure 5 Power transferred to the wireless implant at different positions and input power levels.
(a) Measurement probe consisting of an LED and the same coil and rectifier circuitry as the brain and spinal cord implants. Light from the LED is directed to a photodiode through a silica optical fiber. (b) Power transferred to the implant at the output of the rectifier circuitry as a function of input power and position on the resonant cavity. Typical operating region on the cavity surface is shaded. The implant is operated at a 20% duty cycle; instantaneous transferred power and time-averaged input power are shown (n = 4 technical trials at each location).
Supplementary Figure 6 Closed-loop reflection monitoring reduces variability in received power.
(a) Experimental setup describing system for closed-loop adjustment of delivered power based on measurements on reflected power (Supplementary Note 1). Solid lines: power flow; dashed lines: control signals. (b) Real-time tracking with linear motion: output power increases when reflected power decreases. c) Real-time tracking with angular motion: output power increases when reflected power decreases. (d-e) Closed loop monitoring reduces variability in delivered power with changes in mouse position (d), and mouse angle (e) to within ± 10%. Center values: means, error bars: S.E.M. (n = 3 technical replicates). (f) Measurements of 'normal' stochastic variation in laser output. Variation magnitude in commonly used laser systems is similar to that achieved with closed-loop wireless system.
Supplementary Figure 7 Simulated power density as a function of the height, h, of the mouse above the surface of the cavity.
Thickness of the floor of the behavior chamber or bedding could alter height and therefore decrease delivered power, and should be accounted for (Supplementary Note 2).
Supplementary Figure 8 Local heating due to LED compared to heating due to light from a fiber-coupled laser (20 mW/mm2).
Local temperature of brain tissue of mice was measured with inserted probe (Supplementary Note 3). Center values: means, error bars: S.E.M. (n = 3 trials).
Supplementary Figure 9 Surface mouse temperature due to radio-frequency heating (4-W average input power).
(a) Temperatures of mice were measured with thermal imaging with either the cavity power off or on without an implant over 8 minutes (n = 3 mice). (b) Final reading values for both cavity power off and cavity power on. The mice exhibited a temperature rise of 0.76 °C with the power off, perhaps due to increased behavior in the enclosure tube. The temperature rise attributed to the radio-frequency energy alone is 0.52 °C.
Supplementary Figure 10 Implantation of brain device to stimulate premotor cortex.
(a) Craniotomy is drilled in the skull and the implant is positioned at the specified x-y-z coordinates of the target brain structure, in this case just superior to M2 (AP: +1.0, ML: 0.5, DV: –0.5; see reference below) using the disposable glass implantation tool attached to the stereotactic positioner. (b) The implant is bonded in place using blue light curable composite (Pentron, N11WA). (c) The stereotactic positioner is unscrewed from the implantation tool and moved out of the way. (d) The implantation tool is gently twisted off, and the skin is then sutured over the implant. Reference: Franklin, K.B.J. & Paxinos, G. The mouse brain in stereotaxic coordinates, (Academic Press, San Diego, 1997).
Supplementary Figure 11 Representative traces of mouse movement during on-off cycles (1 continuous session, 1 mouse).
Motor stimulation of the right motor cortex with 5 ms pulses at 20 Hz elicited circling behavior. Stimulation was wirelessly controlled in 20-s on-off cycles. Traces here representative of three out of five mice; the remaining two mice moved very little or not at all when cavity power was off.
Supplementary Figure 12 Implantation of spinal cord device to stimulate superficial laminae of the dorsal spinal cord.
(a) The spinal column is exposed and secured in stereotactic adaptors for the spinal cord. (b) Superficial soft tissue is removed from the vertebrae. The dorsal process of the vertebra is broken off and then drilled flat. A hole is drilled into the now flat surface of the vertebra directly dorsal to the region to be stimulated. (c) LED is positioned over the hole in the vertebra, either by hand or with a stereotax, using the glass implantation tool. The implant is cemented in place, and the implantation tool is broken off. (d) A second coat of cement is applied before the muscle is sutured in place around the implant. (e) The implant is checked for functionality using an alternate antenna. (f) Skin is sutured over the implant.
Supplementary Figure 13 Implantation of peripheral device to stimulate peripheral nerve endings in the heel of the mouse hind paw.
(a) Incision is made superficial to triceps surae muscles. (b) Size of implant compared to the incision. (c) LED at the tip of the extension is routed to the heel, and the power receiving coil is then placed under the skin, adjacent to the incision (not directly under it). (d) Incision is sutured.
Supplementary Figure 14 Effect of implant alone on mobility and pain thresholds post-implantation.
LED was not powered on at any time. (a) Mice were evaluated for Rotarod performance before and after implantation of wireless device in lower hindlimb. Control mice did not undergo surgery. Rotarod latency was not significantly different between implanted and not implanted mice at any time point (n = 9 implanted mice, 10 not implanted mice, P [effect size (Hedge’s g)] - Pre: 0.49 [0.31], Day two: 0.18 [0.62], Day fourteen: 0.86 [0.078]). (b) Mechanical (von Frey) threshold of mice before and after implantation of the wireless device in lower hind limb. Thresholds are not significantly different between the implanted limb and the contralateral limb at any time point (n = 9 mice, P [effect size (Hedge’s g)] - Pre: 0.36 [0.30], Day one: 0.58 [0.23], Day two: 0.91 [0.0.085]).
Supplementary Figure 15 Stimulation of peripheral nociceptors with a wireless device.
(a) Withdrawal latency test (cohort means): ChR2+ mice withdrew their paws within a 20 s stimulation window significantly more often than EYFP+ control mice (n = 4 ChR2+ mice, 4 EYFP+ mice, unpaired t-test, P = 0.03, effect size (Hedge’s g) = 1.71). (b) Place aversion test (individual mice): All ChR2+ mice implanted with the peripheral device spent less time in the resonant cavity chamber when the cavity was powered on (n = 5 ChR2+ mice).
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–15 and Supplementary Notes 1–6 (PDF 2268 kb)
Computer aided design file of resonant cavity.
Computer aided design file of resonant cavity. Precise specifications for machining the custom resonant cavity. (ZIP 524 kb)
Closed-loop reflection monitoring LabView program.
Closed-loop reflection monitoring LabView program. Program to control and limit fluctuations of light power density by monitoring reflected power at the cavity ports. (ZIP 524 kb)
Wireless light delivery to premotor cortex.
Representative video of circling behavior of a mouse during wireless optogenetic stimulation of premotor cortex (20 Hz frequency, 5 ms pulse width, 10 mW/mm2 light power density). (MP4 15947 kb)
Wireless light delivery in various behavioral setups.
Demonstration of wireless light delivery in mice while wheel running, walking through tube, and engaging in social behavior. (MP4 12452 kb)
Rights and permissions
About this article
Cite this article
Montgomery, K., Yeh, A., Ho, J. et al. Wirelessly powered, fully internal optogenetics for brain, spinal and peripheral circuits in mice. Nat Methods 12, 969–974 (2015). https://doi.org/10.1038/nmeth.3536
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmeth.3536
This article is cited by
-
Body-conformable light-emitting materials and devices
Nature Photonics (2024)
-
Bioinspired nanotransducers for neuromodulation
Nano Research (2024)
-
Wearable and Implantable Light-Emitting Diodes and Their Biomedical Applications
Korean Journal of Chemical Engineering (2024)
-
Activation of mechanoluminescent nanotransducers by focused ultrasound enables light delivery to deep-seated tissue in vivo
Nature Protocols (2023)
-
Customizable, wireless and implantable neural probe design and fabrication via 3D printing
Nature Protocols (2023)