Abstract
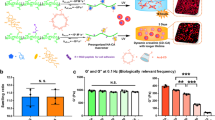
Natural extracellular matrices (ECMs) are viscoelastic and exhibit stress relaxation. However, hydrogels used as synthetic ECMs for three-dimensional (3D) culture are typically elastic. Here, we report a materials approach to tune the rate of stress relaxation of hydrogels for 3D culture, independently of the hydrogel’s initial elastic modulus, degradation, and cell-adhesion-ligand density. We find that cell spreading, proliferation, and osteogenic differentiation of mesenchymal stem cells (MSCs) are all enhanced in cells cultured in gels with faster relaxation. Strikingly, MSCs form a mineralized, collagen-1-rich matrix similar to bone in rapidly relaxing hydrogels with an initial elastic modulus of 17 kPa. We also show that the effects of stress relaxation are mediated by adhesion-ligand binding, actomyosin contractility and mechanical clustering of adhesion ligands. Our findings highlight stress relaxation as a key characteristic of cell–ECM interactions and as an important design parameter of biomaterials for cell culture.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Burdick, J. A. & Anseth, K. S. Photoencapsulation of osteoblasts in injectable RGD-modified PEG hydrogels for bone tissue engineering. Biomaterials 23, 4315–4323 (2002).
Raeber, G. P., Lutolf, M. P. & Hubbell, J. A. Molecularly engineered PEG hydrogels: A novel model system for proteolytically mediated cell migration. Biophys. J. 89, 1374–1388 (2005).
Rowley, J. A., Madlambayan, G. & Mooney, D. J. Alginate hydrogels as synthetic extracellular matrix materials. Biomaterials 20, 45–53 (1999).
Huebsch, N. et al. Harnessing traction-mediated manipulation of the cell/matrix interface to control stem-cell fate. Nature Mater. 9, 518–526 (2010).
Park, Y. D., Tirelli, N. & Hubbell, J. A. Photopolymerized hyaluronic acid-based hydrogels and interpenetrating networks. Biomaterials 24, 893–900 (2003).
Burdick, J. A., Chung, C., Jia, X., Randolph, M. A. & Langer, R. Controlled degradation and mechanical behavior of photopolymerized hyaluronic acid networks. Biomacromolecules 6, 386–391 (2005).
Lutolf, M. P. & Hubbell, J. A. Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nature Biotechnol. 23, 47–55 (2005).
Langer, R. & Tirrell, D. A. Designing materials for biology and medicine. Nature 428, 487–492 (2004).
Healy, K. E., Rezania, A. & Stile, R. A. Designing biomaterials to direct biological responses. Ann. N. Y. Acad. Sci. 875, 24–35 (1999).
Metters, A. T., Anseth, K. S. & Bowman, C. N. Fundamental studies of biodegradable hydrogels as cartilage replacement materials. Biomed. Sci. Instrum. 35, 33–38 (1999).
Nguyen, K. T. & West, J. L. Photopolymerizable hydrogels for tissue engineering applications. Biomaterials 23, 4307–4314 (2002).
Peyton, S. R., Raub, C. B., Keschrumrus, V. P. & Putnam, A. J. The use of poly(ethylene glycol) hydrogels to investigate the impact of ECM chemistry and mechanics on smooth muscle cells. Biomaterials 27, 4881–4893 (2006).
Khetan, S. et al. Degradation-mediated cellular traction directs stem cell fate in covalently crosslinked three-dimensional hydrogels. Nature Mater. 12, 5571–5580 (2013).
Wen, J. H. et al. Interplay of matrix stiffness and protein tethering in stem cell differentiation. Nature Mater. 13, 979–987 (2014).
Alsberg, E. et al. Regulating bone formation via controlled scaffold degradation. J. Dent. Res. 82, 903–908 (2003).
Levental, I., Georges, P. C. & Janmey, P. A. Soft biological materials and their impact on cell function. Soft Matter 3, 299–306 (2007).
Liu, Z. & Bilston, L. On the viscoelastic character of liver tissue: Experiments and modelling of the linear behaviour. Biorheology 37, 191–201 (2000).
Geerligs, M., Peters, G. W. M., Ackermans, P. A. J., Oomens, C. W. J. & Baaijens, F. P. T. Linear viscoelastic behavior of subcutaneous adipose tissue. Biorheology 45, 677–688 (2008).
McDonald, S. J. et al. Early fracture callus displays smooth muscle-like viscoelastic properties ex vivo: Implications for fracture healing. J. Orthop. Res. 27, 1508–1513 (2009).
Discher, D. E., Janmey, P. & Wang, Y.-L. Tissue cells feel and respond to the stiffness of their substrate. Science 310, 1139–1143 (2005).
Legant, W. R. et al. Measurement of mechanical tractions exerted by cells in three-dimensional matrices. Nature Methods 7, 969–971 (2010).
Legant, W. R. et al. Microfabricated tissue gauges to measure and manipulate forces from 3D microtissues. Proc. Natl Acad. Sci. USA 106, 10097–10102 (2009).
Pelham, R. J. Jr & Wang, Y. l. Cell locomotion and focal adhesions are regulated by substrate flexibility. Proc. Natl Acad. Sci. USA 94, 13661–13665 (1997).
Flanagan, L. A., Ju, Y.-E., Marg, B., Osterfield, M. & Janmey, P. A. Neurite branching on deformable substrates. Neuroreport 13, 2411–2415 (2002).
Engler, A. et al. Substrate compliance versus ligand density in cell on gel responses. Biophys. J. 86, 617–628 (2004).
Kong, H. J. et al. Non-viral gene delivery regulated by stiffness of cell adhesion substrates. Nature Mater. 4, 460–464 (2005).
Paszek, M. J. et al. Tensional homeostasis and the malignant phenotype. Cancer Cell 8, 241–254 (2005).
Engler, A., Sen, S., Sweeney, H. & Discher, D. Matrix elasticity directs stem cell lineage specification. Cell 126, 677–689 (2006).
Chaudhuri, O. et al. Extracellular matrix stiffness and composition jointly regulate the induction of malignant phenotypes in mammary epithelium. Nature Mater. 13, 970–978 (2014).
Cameron, A. R., Frith, J. E. & Cooper-White, J. J. The influence of substrate creep on mesenchymal stem cell behaviour and phenotype. Biomaterials 32, 5979–5993 (2011).
Cameron, A. R., Frith, J. E., Gomez, G. A., Yap, A. S. & Cooper-White, J. J. The effect of time-dependent deformation of viscoelastic hydrogels on myogenic induction and Rac1 activity in mesenchymal stem cells. Biomaterials 35, 1857–1868 (2014).
McKinnon, D. D., Domaille, D. W., Cha, J. N. & Anseth, K. S. Biophysically defined and cytocompatible covalently adaptable networks as viscoelastic 3D cell culture systems. Adv. Mater. 26, 865–872 (2013).
Chaudhuri, O. et al. Substrate stress relaxation regulates cell spreading. Nature Commun. 6, 6364 (2015).
Lee, K. Y. & Mooney, D. J. Hydrogels for tissue engineering. Chem. Rev. 101, 1869–1879 (2001).
Zhao, X., Huebsch, N., Mooney, D. J. & Suo, Z. Stress-relaxation behavior in gels with ionic and covalent crosslinks. J. Appl. Phys. 107, 63509 (2010).
Graessley, W. W. Synthesis and Degradation Rheology and Extrusion Vol. 47, 67–117 (Springer, 1982).
Vogel, V. & Sheetz, M. Local force and geometry sensing regulate cell functions. Nature Rev. Mol. Cell Biol. 7, 265–275 (2006).
Mooney, D. J., Langer, R. & Ingber, D. E. Cytoskeletal filament assembly and the control of cell spreading and function by extracellular matrix. J. Cell Sci. 108, 2311–2320 (1995).
Parekh, S. H. et al. Modulus-driven differentiation of marrow stromal cells in 3D scaffolds that is independent of myosin-based cytoskeletal tension. Biomaterials 32, 2256–2264 (2011).
Pek, Y. S., Wan, A. C. A. & Ying, J. Y. The effect of matrix stiffness on mesenchymal stem cell differentiation in a 3D thixotropic gel. Biomaterials 31, 385–391 (2010).
Humphries, J. D., Byron, A. & Humphries, M. J. Integrin ligands at a glance. J. Cell Sci. 119, 3901–3903 (2006).
Kanchanawong, P. et al. Nanoscale architecture of integrin-based cell adhesions. Nature 468, 580–584 (2010).
Kong, H. J., Polte, T. R., Alsberg, E. & Mooney, D. J. FRET measurements of cell-traction forces and nano-scale clustering of adhesion ligands varied by substrate stiffness. Proc. Natl Acad. Sci. USA 102, 4300–4305 (2005).
Arnold, M. et al. Activation of integrin function by nanopatterned adhesive interfaces. ChemPhysChem 5, 383–388 (2004).
Maheshwari, G., Brown, G., Lauffenburger, D. A., Wells, A. & Griffith, L. G. Cell adhesion and motility depend on nanoscale RGD clustering. J. Cell Sci. 113, 1677–1686 (2000).
Wozniak, M. A. & Chen, C. S. Mechanotransduction in development: A growing role for contractility. Nature Rev. Mol. Cell Biol. 10, 34–43 (2009).
Dupont, S. et al. Role of YAP/TAZ in mechanotransduction. Nature 474, 179–183 (2011).
Swift, J. et al. Nuclear lamin-A scales with tissue stiffness and enhances matrix-directed differentiation. Science 341, 1240104 (2013).
Hynes, R. O. The extracellular matrix: Not just pretty fibrils. Science 326, 1216–1219 (2009).
Schultz, K. M., Kyburz, K. A. & Anseth, K. S. Measuring dynamic cell-material interactions and remodeling during 3D human mesenchymal stem cell migration in hydrogels. Proc. Natl Acad. Sci. USA 112, E3757–E3764 (2015).
Diduch, D. R., Coe, M. R., Joyner, C., Owen, M. E. & Balian, G. Two cell lines from bone marrow that differ in terms of collagen synthesis, osteogenic characteristics, and matrix mineralization. J. Bone Joint Surg. Am. 75, 92–105 (1993).
Acknowledgements
The authors acknowledge the help of S. Koshy, M. Mehta, C. Verbeke, X. Zhao (now at MIT), and other members of the Mooney lab. The authors also thank the Weitz lab for use of a rheometer, O. Uzun for help with GPC, S. Reinke (Berlin-Brandenburg Center for Regenerative Therapies) for providing the human bone haematoma samples, and D. Wulsten and S. Reinke for the support in bone fracture haematoma testing. This work was supported by an NIH Grant to D.J.M. (R01 DE013033), an NIH F32 grant to O.C. (CA153802), an Einstein Visiting Fellowship for D.J.M., funding of the Einstein Foundation Berlin through the Charité—Universitätsmedizin Berlin, Berlin-Brandenburg School for Regenerative Therapies GSC 203, ZonMW-VICI grant 918.11.635 (The Netherlands) for D.K., and Harvard MRSEC for D.J.M. (DMR-1420570). This work was performed in part at the Center for Nanoscale Systems (CNS), a member of the National Nanotechnology Infrastructure Network (NNIN).
Author information
Authors and Affiliations
Contributions
O.C., L.G., D.K., M.D., N.H. and D.J.M. designed the experiments. O.C. and L.G. conducted most of the experiments. D.K. helped with experiments involving the MSCs. S.A.B. helped with alginate characterization. J.C.W. helped with EDS experiments and analysis. H.-p.L. assisted with mechanical characterization. E.L. and G.N.D. carried out fracture haematoma measurement. O.C. and L.G. analysed the data. O.C., L.G., D.K. and D.J.M. wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 3690 kb)
Rights and permissions
About this article
Cite this article
Chaudhuri, O., Gu, L., Klumpers, D. et al. Hydrogels with tunable stress relaxation regulate stem cell fate and activity. Nature Mater 15, 326–334 (2016). https://doi.org/10.1038/nmat4489
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat4489
This article is cited by
-
Self-compliant ionic skin by leveraging hierarchical hydrogen bond association
Nature Communications (2024)
-
Nano-frictional mechano-reinforcing porous nanowires scaffolds
Friction (2024)
-
Matrix viscoelasticity promotes liver cancer progression in the pre-cirrhotic liver
Nature (2024)
-
Biomimetic natural biomaterials for tissue engineering and regenerative medicine: new biosynthesis methods, recent advances, and emerging applications
Military Medical Research (2023)
-
Cell unit-inspired natural nano-based biomaterials as versatile building blocks for bone/cartilage regeneration
Journal of Nanobiotechnology (2023)