Abstract
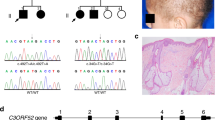
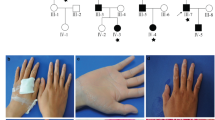
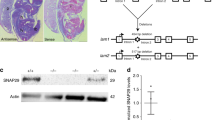
Autosomal recessive cutis laxa (ARCL) describes a group of syndromal disorders that are often associated with a progeroid appearance, lax and wrinkled skin, osteopenia and mental retardation1,2,3. Homozygosity mapping in several kindreds with ARCL identified a candidate region on chromosome 17q25. By high-throughput sequencing of the entire candidate region, we detected disease-causing mutations in the gene PYCR1. We found that the gene product, an enzyme involved in proline metabolism, localizes to mitochondria. Altered mitochondrial morphology, membrane potential and increased apoptosis rate upon oxidative stress were evident in fibroblasts from affected individuals. Knockdown of the orthologous genes in Xenopus and zebrafish led to epidermal hypoplasia and blistering that was accompanied by a massive increase of apoptosis. Our findings link mutations in PYCR1 to altered mitochondrial function and progeroid changes in connective tissues.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Accession codes
Change history
21 January 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41588-022-01013-2
References
Rajab, A. et al. Geroderma osteodysplasticum hereditaria and wrinkly skin syndrome in 22 patients from Oman. Am. J. Med. Genet. A 146A, 965–976 (2008).
Morava, E. et al. Defining the phenotype in an autosomal recessive cutis laxa syndrome with a combined congenital defect of glycosylation. Eur. J. Hum. Genet. 16, 28–35 (2008).
Guerra, D. et al. The De Barsy syndrome. J. Cutan. Pathol. 31, 616–624 (2004).
Zhang, M.C. et al. Cutis laxa arising from frameshift mutations in exon 30 of the elastin gene (ELN). J. Biol. Chem. 274, 981–986 (1999).
Al-Gazali, L.I., Sztriha, L., Skaff, F. & Haas, D. Gerodermia osteodysplastica and wrinkly skin syndrome: are they the same? Am. J. Med. Genet. 101, 213–220 (2001).
Nanda, A. et al. Gerodermia osteodysplastica/wrinkly skin syndrome: report of three patients and brief review of the literature. Pediatr. Dermatol. 25, 66–71 (2008).
Hamamy, H., Masri, A. & Ajlouni, K. Wrinkly skin syndrome. Clin. Exp. Dermatol. 30, 590–592 (2005).
Sommer, A. Photo essay–geroderma osteodysplastica. Am. J. Med. Genet. C. Semin. Med. Genet. 145C, 291–292 (2007).
Kunze, J. et al. De Barsy syndrome–an autosomal recessive, progeroid syndrome. Eur. J. Pediatr. 144, 348–354 (1985).
Phang, J.M., Pandhare, J. & Liu, Y. The metabolism of proline as microenvironmental stress substrate. J. Nutr. 138, 2008S–2015S (2008).
Hagedorn, C.H. & Phang, J.M. Transfer of reducing equivalents into mitochondria by the interconversions of proline and delta 1-pyrroline-5-carboxylate. Arch. Biochem. Biophys. 225, 95–101 (1983).
Meng, Z. et al. Crystal structure of human pyrroline-5-carboxylate reductase. J. Mol. Biol. 359, 1364–1377 (2006).
Mitsubuchi, H., Nakamura, K., Matsumoto, S. & Endo, F. Inborn errors of proline metabolism. J. Nutr. 138, 2016S–2020S (2008).
Baumgartner, M.R. et al. Delta1-pyrroline-5-carboxylate synthase deficiency: neurodegeneration, cataracts and connective tissue manifestations combined with hyperammonaemia and reduced ornithine, citrulline, arginine and proline. Eur. J. Pediatr. 164, 31–36 (2005).
Bicknell, L.S. et al. A missense mutation in ALDH18A1, encoding Delta1-pyrroline-5-carboxylate synthase (P5CS), causes an autosomal recessive neurocutaneous syndrome. Eur. J. Hum. Genet. 16, 1176–1186 (2008).
Baumgartner, M.R. et al. Hyperammonemia with reduced ornithine, citrulline, arginine and proline: a new inborn error caused by a mutation in the gene encoding delta(1)-pyrroline-5-carboxylate synthase. Hum. Mol. Genet. 9, 2853–2858 (2000).
Van Maldergem, L. et al. Cobblestone-like brain dysgenesis and altered glycosylation in congenital cutis laxa, Debre type. Neurology 71, 1602–1608 (2008).
Hennies, H.C. et al. Gerodermia osteodysplastica is caused by mutations in SCYL1BP1, a Rab-6 interacting golgin. Nat. Genet. 40, 1410–1412 (2008).
Kornak, U. et al. Impaired glycosylation and cutis laxa caused by mutations in the vesicular H+-ATPase subunit ATP6V0A2. Nat. Genet. 40, 32–34 (2008).
Hucthagowder, V. et al. Loss-of-function mutations in ATP6V0A2 impair vesicular trafficking, tropoelastin secretion, and cell survival. Hum. Mol. Genet. 18, 2149–2165 (2009).
Wallace, D.C. A mitochondrial paradigm of metabolic and degenerative diseases, aging, and cancer: a dawn for evolutionary medicine. Annu. Rev. Genet. 39, 359–407 (2005).
Balaban, R.S., Nemoto, S. & Finkel, T. Mitochondria, oxidants, and aging. Cell 120, 483–495 (2005).
D'Autreaux, B. & Toledano, M.B. ROS as signalling molecules: mechanisms that generate specificity in ROS homeostasis. Nat. Rev. Mol. Cell Biol. 8, 813–824 (2007).
Krishnan, N., Dickman, M.B. & Becker, D.F. Proline modulates the intracellular redox environment and protects mammalian cells against oxidative stress. Free Radic. Biol. Med. 44, 671–681 (2008).
Knott, A.B., Perkins, G., Schwarzenbacher, R. & Bossy-Wetzel, E. Mitochondrial fragmentation in neurodegeneration. Nat. Rev. Neurosci. 9, 505–518 (2008).
Lee, S. et al. Mitochondrial fission and fusion mediators, hFis1 and OPA1, modulate cellular senescence. J. Biol. Chem. 282, 22977–22983 (2007).
O'Connell, J.R. & Weeks, D.E. PedCheck: a program for identification of genotype incompatibilities in linkage analysis. Am. J. Hum. Genet. 63, 259–266 (1998).
Abecasis, G.R., Cherny, S.S., Cookson, W.O. & Cardon, L.R. Merlin—rapid analysis of dense genetic maps using sparse gene flow trees. Nat. Genet. 30, 97–101 (2002).
Thiele, H. & Nurnberg, P. HaploPainter: a tool for drawing pedigrees with complex haplotypes. Bioinformatics 21, 1730–1732 (2005).
Kruglyak, L., Daly, M.J., Reeve-Daly, M.P. & Lander, E.S. Parametric and nonparametric linkage analysis: a unified multipoint approach. Am. J. Hum. Genet. 58, 1347–1363 (1996).
Duvezin-Caubet, S. et al. Proteolytic processing of OPA1 links mitochondrial dysfunction to alterations in mitochondrial morphology. J. Biol. Chem. 281, 37972–37979 (2006).
Teramoto, S. et al. Hydrogen peroxide-induced apoptosis and necrosis in human lung fibroblasts: protective roles of glutathione. Jpn. J. Pharmacol. 79, 33–40 (1999).
Hofhaus, G., Shakeley, R.M. & Attardi, G. Use of polarography to detect respiration defects in cell cultures. Methods Enzymol. 264, 476–483 (1996).
Hensey, C. & Gautier, J. Programmed cell death during Xenopus development: a spatio-temporal analysis. Dev. Biol. 203, 36–48 (1998).
Sive, H., Grainger, R.M. & Harland, R.M. Early Development of Xenopus Laevis: A Laboratory Manual (Cold Spring Harbor Press, New York, 2000).
Acknowledgements
J. Common and B. Lane for advice and help with primary cultures. J. Gautier for TUNEL protocol. K. Rogers and S. Rogers for their help and advice on histology. This study was supported by the German Federal Ministry of Education and Research (BMBF) by grant 01GM0623 (SKELNET) to U.K. and S.M. and grants 01GM0880 and 01GM0801 to B.W., a grant from the Deutsche Forschungsgemeinschaft (Collaborative Research Centre 577) to U.K. and P.N., and by A*STAR and the Branco Weiss Foundation to B.R.
Author information
Authors and Affiliations
Contributions
B.R., N.E.-B., S.M. and U.K. designed the study. H.K., L.A.-G., M. Shahwan, B.R., F.B., S.F.N., A.M., F.A., D.G., P.F., A.N., A.R., D.M., M.G., J.N., A.G., A.S., R.S., A.R.J., E.S., D.S., B.D., S.R., H.H., B.W. and L.v.M. made clinical diagnoses and collected clinical data and samples. B.R., B.M., A.D., G.N., B.F., Y.L., B.B., P.N. and B.W. conducted genotyping and linkage analysis. H.L., B.O., B.M. and S.N. performed genomic loci capture. B.R., N.E.-B., A.D., B.F., D.K., S.C., M.S., P.-Y.T. performed immunoblotting, immunostaining, TUNEL, and proline level and FACS analysis. B.R., N.E.-B. and S.C. performed Xenopus work, ISH and Pycr1 constructs. U.K., B.F., M.S.-v.K. and P.S. performed zebrafish work. B.F., U.K. and M. Schuelke performed respiratory chain measurements. I.H. and G.Z. were responsible for ultrastructural and histological analysis of skin biopsies. B.R., N.E.-B., S.M. and U.K. wrote the manuscript.
Corresponding authors
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–6 and Supplementary Tables 1–2 (PDF 3105 kb)
Supplementary Video 1
Movie of circulating red blood cells and beating heart in control tadpole at stage 30. (AVI 6648 kb)
Supplementary Video 2
Movie of beating heart in Pycr1 morphant tadpole at stage 30 despite absence of circulating red blood cells. (AVI 6648 kb)
Supplementary Video 3
Movie of shared blood circulation between Pycr1 morphant (top) and control tadpole (bottom) in parabiotic embryos at stage 45. (AVI 3715 kb)
Rights and permissions
About this article
Cite this article
Reversade, B., Escande-Beillard, N., Dimopoulou, A. et al. Mutations in PYCR1 cause cutis laxa with progeroid features. Nat Genet 41, 1016–1021 (2009). https://doi.org/10.1038/ng.413
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ng.413
This article is cited by
-
Better prediction of clinical outcome in clear cell renal cell carcinoma based on a 6 metabolism-related gene signature
Scientific Reports (2023)
-
Lipodystrophy-associated progeroid syndromes
Hormones (2022)
-
Homozygous deletion of MYADML2 in cranial asymmetry, reduced bone maturation, multiple dislocations, lumbar lordosis, and prominent clavicles
Journal of Human Genetics (2021)
-
Proline metabolism and redox; maintaining a balance in health and disease
Amino Acids (2021)
-
PYCR1 promotes bladder cancer by affecting the Akt/Wnt/β-catenin signaling
Journal of Bioenergetics and Biomembranes (2021)