Abstract
Recent studies suggest that individual subunits of chromatin-remodeling complexes produce biologically specific meaning in different cell types through combinatorial assembly. Here we show that granulocyte development requires SMARCD2, a subunit of ATP-dependent SWI/SNF (BAF) chromatin-remodeling complexes. Smarcd2-deficient mice fail to generate functionally mature neutrophils and eosinophils, a phenotype reminiscent of neutrophil-specific granule deficiency (SGD) in humans, for which loss-of-function mutations in CEBPE (encoding CEBPɛ) have been reported. SMARCD2-containing SWI/SNF complexes are necessary for CEBPɛ transcription factor recruitment to the promoter of neutrophilic secondary granule genes and for granulocyte differentiation. The homologous SMARCD1 protein (63% identical at the amino acid level) cannot replace the role of SMARCD2 in granulocyte development. We find that SMARCD2 functional specificity is conferred by its divergent coiled-coil 1 and SWIB domains. Strikingly, both CEBPE and SMARCD2 loss-of-function mutations identified in patients with SGD abolish the interaction with SWI/SNF and thereby secondary granule gene expression, thus providing a molecular basis for this disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
Accession codes
Primary accessions
BioProject
Gene Expression Omnibus
Referenced accessions
NCBI Reference Sequence
References
Akashi, K., Traver, D., Miyamoto, T. & Weissman, I.L. A clonogenic common myeloid progenitor that gives rise to all myeloid lineages. Nature 404, 193–197 (2000).
Iwasaki, H. et al. The order of expression of transcription factors directs hierarchical specification of hematopoietic lineages. Genes Dev. 20, 3010–3021 (2006).
Berliner, N. Lessons from congenital neutropenia: 50 years of progress in understanding myelopoiesis. Blood 111, 5427–5432 (2008).
Cantor, A.B. & Orkin, S.H. Hematopoietic development: a balancing act. Curr. Opin. Genet. Dev. 11, 513–519 (2001).
Enver, T., Heyworth, C.M. & Dexter, T.M. Do stem cells play dice? Blood 92, 348–351, discussion 352 (1998).
Metcalf, D. Hematopoietic cytokines. Blood 111, 485–491 (2008).
Metcalf, D. Lineage commitment and maturation in hematopoietic cells: the case for extrinsic regulation. Blood 92, 345–347, discussion 352 (1998).
Yamanaka, R. et al. Impaired granulopoiesis, myelodysplasia, and early lethality in CCAAT/enhancer binding protein ɛ–deficient mice. Proc. Natl. Acad. Sci. USA 94, 13187–13192 (1997).
Lekstrom-Himes, J. & Xanthopoulos, K.G. CCAAT/enhancer binding protein ɛ is critical for effective neutrophil-mediated response to inflammatory challenge. Blood 93, 3096–3105 (1999).
Verbeek, W. et al. Myeloid transcription factor C/EBPɛ is involved in the positive regulation of lactoferrin gene expression in neutrophils. Blood 94, 3141–3150 (1999).
Strauss, R.G., Bove, K.E., Jones, J.F., Mauer, A.M. & Fulginiti, V.A. An anomaly of neutrophil morphology with impaired function. N. Engl. J. Med. 290, 478–484 (1974).
Komiyama, A., Morosawa, H., Nakahata, T., Miyagawa, Y. & Akabane, T. Abnormal neutrophil maturation in a neutrophil defect with morphologic abnormality and impaired function. J. Pediatr. 94, 19–25 (1979).
Breton-Gorius, J., Mason, D.Y., Buriot, D., Vilde, J.L. & Griscelli, C. Lactoferrin deficiency as a consequence of a lack of specific granules in neutrophils from a patient with recurrent infections. Detection by immunoperoxidase staining for lactoferrin and cytochemical electron microscopy. Am. J. Pathol. 99, 413–428 (1980).
Gallin, J.I. et al. Human neutrophil-specific granule deficiency: a model to assess the role of neutrophil-specific granules in the evolution of the inflammatory response. Blood 59, 1317–1329 (1982).
Boxer, L.A. et al. Lactoferrin deficiency associated with altered granulocyte function. N. Engl. J. Med. 307, 404–410 (1982).
Ambruso, D.R. et al. Defective bactericidal activity and absence of specific granules in neutrophils from a patient with recurrent bacterial infections. J. Clin. Immunol. 4, 23–30 (1984).
Borregaard, N., Boxer, L.A., Smolen, J.E. & Tauber, A.I. Anomalous neutrophil granule distribution in a patient with lactoferrin deficiency: pertinence to the respiratory burst. Am. J. Hematol. 18, 255–260 (1985).
Ganz, T., Metcalf, J.A., Gallin, J.I., Boxer, L.A. & Lehrer, R.I. Microbicidal/cytotoxic proteins of neutrophils are deficient in two disorders: Chediak–Higashi syndrome and “specific” granule deficiency. J. Clin. Invest. 82, 552–556 (1988).
Lomax, K.J. et al. Selective defect in myeloid cell lactoferrin gene expression in neutrophil specific granule deficiency. J. Clin. Invest. 83, 514–519 (1989).
Raphael, G.D. et al. Glandular secretion of lactoferrin in a patient with neutrophil lactoferrin deficiency. J. Allergy Clin. Immunol. 84, 914–919 (1989).
Gombart, A.F. et al. Neutrophil-specific granule deficiency: homozygous recessive inheritance of a frameshift mutation in the gene encoding transcription factor CCAAT/enhancer binding protein-ɛ. Blood 97, 2561–2567 (2001).
Wada, T. et al. A novel in-frame deletion in the leucine zipper domain of C/EBPɛ leads to neutrophil-specific granule deficiency. J. Immunol. 195, 80–86 (2015).
Bultman, S. et al. A Brg1 null mutation in the mouse reveals functional differences among mammalian SWI/SNF complexes. Mol. Cell 6, 1287–1295 (2000).
Olave, I., Wang, W., Xue, Y., Kuo, A. & Crabtree, G.R. Identification of a polymorphic, neuron-specific chromatin remodeling complex. Genes Dev. 16, 2509–2517 (2002).
Nagl, N.G. Jr., Wang, X., Patsialou, A., Van Scoy, M. & Moran, E. Distinct mammalian SWI/SNF chromatin remodeling complexes with opposing roles in cell-cycle control. EMBO J. 26, 752–763 (2007).
Flowers, S., Nagl, N.G. Jr., Beck, G.R. Jr. & Moran, E. Antagonistic roles for BRM and BRG1 SWI/SNF complexes in differentiation. J. Biol. Chem. 284, 10067–10075 (2009).
Kadam, S. & Emerson, B.M. Transcriptional specificity of human SWI/SNF BRG1 and BRM chromatin remodeling complexes. Mol. Cell 11, 377–389 (2003).
Wu, J.I. et al. Regulation of dendritic development by neuron-specific chromatin remodeling complexes. Neuron 56, 94–108 (2007).
Lessard, J. et al. An essential switch in subunit composition of a chromatin remodeling complex during neural development. Neuron 55, 201–215 (2007).
Krasteva, V. et al. The BAF53a subunit of SWI/SNF-like BAF complexes is essential for hemopoietic stem cell function. Blood 120, 4720–4732 (2012).
Krosl, J. et al. A mutant allele of the Swi/Snf member BAF250a determines the pool size of fetal liver hemopoietic stem cell populations. Blood 116, 1678–1684 (2010).
Choi, J. et al. The SWI/SNF-like BAF complex is essential for early B cell development. J. Immunol. 188, 3791–3803 (2012).
Chi, T.H. et al. Reciprocal regulation of CD4/CD8 expression by SWI/SNF-like BAF complexes. Nature 418, 195–199 (2002).
Witzel, M. et al. Chromatin remodelling factor SMARCD2 regulates transcriptional networks controlling differentiation of neutrophil granulocytes. Nat. Genet. http://dx.doi.org/10.1038/ng.3833 (2017).
Shi, J. et al. Role of SWI/SNF in acute leukemia maintenance and enhancer-mediated Myc regulation. Genes Dev. 27, 2648–2662 (2013).
Wang, N.D. et al. Impaired energy homeostasis in C/EBPα knockout mice. Science 269, 1108–1112 (1995).
Wang, W. et al. Purification and biochemical heterogeneity of the mammalian SWI–SNF complex. EMBO J. 15, 5370–5382 (1996).
Wang, W. et al. Diversity and specialization of mammalian SWI/SNF complexes. Genes Dev. 10, 2117–2130 (1996).
Gombart, A.F. et al. Regulation of neutrophil and eosinophil secondary granule gene expression by transcription factors C/EBPɛ and PU.1. Blood 101, 3265–3273 (2003).
Lupas, A., Van Dyke, M. & Stock, J. Predicting coiled coils from protein sequences. Science 252, 1162–1164 (1991).
Bennett-Lovsey, R., Hart, S.E., Shirai, H. & Mizuguchi, K. The SWIB and the MDM2 domains are homologous and share a common fold. Bioinformatics 18, 626–630 (2002).
Sandelin, A., Alkema, W., Engstrom, P., Wasserman, W.W. & Lenhard, B. JASPAR: an open-access database for eukaryotic transcription factor binding profiles. Nucleic Acids Res. 32, D91–D94 (2004).
Ho, L. et al. An embryonic stem cell chromatin remodeling complex, esBAF, is essential for embryonic stem cell self-renewal and pluripotency. Proc. Natl. Acad. Sci. USA 106, 5181–5186 (2009).
Alajem, A. et al. Differential association of chromatin proteins identifies BAF60a/SMARCD1 as a regulator of embryonic stem cell differentiation. Cell Rep. 10, 2019–2031 (2015).
Gao, Z. et al. Determination of protein interactome of transcription factor Sox2 in embryonic stem cells engineered for inducible expression of four reprogramming factors. J. Biol. Chem. 287, 11384–11397 (2012).
Chen, L. et al. Transcriptional control in cardiac progenitors: Tbx1 interacts with the BAF chromatin remodeling complex and regulates Wnt5a. PLoS Genet. 8, e1002571 (2012).
Lickert, H. et al. Baf60c is essential for function of BAF chromatin remodelling complexes in heart development. Nature 432, 107–112 (2004).
Ochi, H., Hans, S. & Westerfield, M. Smarcd3 regulates the timing of zebrafish myogenesis onset. J. Biol. Chem. 283, 3529–3536 (2008).
Mallappa, C. et al. Myogenic microRNA expression requires ATP-dependent chromatin remodeling enzyme function. Mol. Cell. Biol. 30, 3176–3186 (2010).
Goljanek-Whysall, K. et al. Regulation of multiple target genes by miR-1 and miR-206 is pivotal for C2C12 myoblast differentiation. J. Cell Sci. 125, 3590–3600 (2012).
Wu, J.I., Lessard, J. & Crabtree, G.R. Understanding the words of chromatin regulation. Cell 136, 200–206 (2009).
Armstrong, J.A., Bieker, J.J. & Emerson, B.M.A. SWI/SNF-related chromatin remodeling complex, E-RC1, is required for tissue-specific transcriptional regulation by EKLF in vitro. Cell 95, 93–104 (1998).
Takeuchi, J.K. & Bruneau, B.G. Directed transdifferentiation of mouse mesoderm to heart tissue by defined factors. Nature 459, 708–711 (2009).
Forcales, S.V. et al. Signal-dependent incorporation of MyoD–BAF60c into Brg1-based SWI/SNF chromatin-remodelling complex. EMBO J. 31, 301–316 (2012).
Thorsteinsdottir, U., Kroon, E., Jerome, L., Blasi, F. & Sauvageau, G. Defining roles for HOX and MEIS1 genes in induction of acute myeloid leukemia. Mol. Cell. Biol. 21, 224–234 (2001).
Wilhelm, B.T. et al. NRNA–seq analysis of 2 closely related leukemia clones that differ in their self-renewal capacity. Blood 117, e27–e38 (2011).
Lessard, J. & Sauvageau, G. Bmi-1 determines the proliferative capacity of normal and leukaemic stem cells. Nature 423, 255–260 (2003).
Carson, F.L. Histotechnology: A Self Instructional Text (ASCP Press, 2015).
Acknowledgements
The authors thank B. Turgeon, S. Harton and V. Paradis for generating the Smarcd2-deficient mice; J. Gervais for veterinary services, C. Klein (Ludwig Maximilians University) for the SMARCD2 SGD mutants and critical discussions, J. Féthière for the antibodies to SMARCD1, SMARCD2 and SMARCD3, G.R. Crabtree (Stanford University) for J1 antibody; J. Krosl and T. Hoang for hemopoietic cytokines; P. Gendron and V. Lavallée for bioinformatics analyses; D. Gagné and G. Dulude for flow cytometry; C. Charbonneau for microscopy; J. Hébert and the Quebec Leukemia Cell Bank (BCLQ) for human samples; and J. Chagraoui for scientific discussions. P.P. is supported by a scholarship from the Cole Foundation. These studies were also supported in part by grants from the Canadian Institutes for Health Research (MOP_133546 to J.L.) and a Canada Research Chair Tier 2 to J.A.L.
Author information
Authors and Affiliations
Contributions
J.A.L. contributed to study design and supervision. P.P., V.K., P.R., G.D., G.S. and L.G. contributed to data acquisition and analysis. P.P. and J.L. contributed to writing and revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Smarcd2-knockout mice die perinatally with impaired energy homeostasis.
(a) Generation of the Smarcd2 conditional knockout allele. Deletion of exons 3–5 generates a null allele (frameshift and premature stop codon). (b) The Mendelian distribution of animals resulting from Smarcd2-heterozygous parents is shown for the different developmental stages. (c) Histological analysis of a 10-h-old Smarcd2-knockout neonate. Enlarged areas shown in d–f are identified as 1, 2 and 3, respectively. Representative images of three independent animals are shown. a, thymus; b, heart; c, lung; d, liver. (d) Hypoplasic white adipose tissue (unfilled arrowhead) and brown adipose tissue (filled arrowhead) in the interscapular area. (e,f) Hypoplasic brown (e) and white (f) adipose tissue in the interscapular region. (g) Periodic acid–Schiff (PAS) staining (magenta) showing reduced glycogen storage in the liver. (h) Western blotting showing nearly complete depletion of Smarcd2 protein in the bone marrow, spleen and thymus of pI:pC-treated Smarcd2fl/fl; Mx1-Cre+ animals on day 28 after treatment. Histone H3 is used as a loading control. (i) The Smarcd2 subunit is biochemically dedicated to Brg1/Brm-containing SWI/SNF complexes in hemopoietic cells. Co-fractionation studies on 10–30% glycerol gradients using nuclear extracts from FLA2 leukemic cells. (j) Smarcd2-knockout neonates are smaller than controls. Means ± s.e.m. are shown; P = 0.043, t-test with unequal variance; n = 16 control and n = 8 Smarcd2-deficient mice. (k) Kaplan–Meier survival curve of Smarcd2-knockout neonates indicating that they die within 26 h of birth. (l) Giemsa staining of a lung section from a 10-h-old Smarcd2-knockout neonate showing no gross developmental abnormalities. Representative images from three independent animals are shown.
Supplementary Figure 2 Validation of the Smarcd2 conditional allele and Smarcd1, Smarcd2 and Smarcd3 antibodies.
(a) Southern blot analysis of the Smarcd2 locus configuration in the bone marrow of Smarcd2fl/fl and Smarcd2WT/WT (control) × Mx1-Cre+ hemopoietic chimeras following pI:pC-induced deletion. Genomic DNA was digested with KpnI enzyme, and an external genomic probe was used. Note the complete genomic recombination of the floxed allele as early as 7 d after pI:pC treatment. The molecular weight of the different Smarcd2 alleles is shown. (b) Southern blot analysis of genomic DNA isolated from the bone marrow of Smarcd2flox-neo/WT, Smarcd2flox/WT and Smarcd2WT/WT (control) animals using the same experimental approach described in a. (c) Validation of the specificity of the affinity-purified Smarcd1, Smarcd2 and Smarcd3 polyclonal rabbit antibodies. Top, experimental design for generating Smarcd1, Smarcd2 and Smarcd3 antibodies. Bottom, nuclear extracts of 293 cells expressing Smarcd1, Smarcd2 or Smarcd3 were used in western blotting with the indicated antibodies. (d) Expression of SWI/SNF subunits is not affected upon Smarcd2 depletion. Antibodies raised against the different SWI/SNF subunits were used in western blotting on nuclear extracts isolated from Smarcd2-knockout E14.5 fetal liver cells. See Supplementary Table 1 for antibody description. WT, wild type; Flox, floxed; KO, knockout; neo, neomycin.
Supplementary Figure 3 Analysis of Smarcd2-deficient bone marrow atypical myeloid colony-forming units.
(a) FACS analyses of pooled early-disease (ED) Smarcd2-deficient bone marrow atypical myeloid colony-forming units (CFU-M (aty); n = 20 colonies) showing a high percentage of CD34+ cells but nearly complete absence of Gr1+ and F4/80+ cells (CD34: Ctrl = 8%, KO = 57%; Gr1: Ctrl = 56%, KO = 6%; F4/80: Ctrl = 11%, KO = 0.05%). (b) Wright staining of cytospin preparations of the early-disease (ED) Smarcd2-deficient bone marrow CFU-M (aty) analyzed in a showing a significant reduction in macrophages and an increase in early granulocyte precursors (mainly myeloblasts, promyelocytes and myelocytes).
Supplementary Figure 4 Flow cytometry analyses of early-disease Smarcd2-deficient hemopoietic populations.
(a) Smarcd2-deficient bone marrow cells and splenocytes were analyzed 28 d after pI:pC-treatment. Results are expressed as means ± s.e.m Total bone marrow cells: CD34+ progenitors, n = 5 control and Smarcd2-deficient mice; lymphoid cells, n = 5 control and Smarcd2-deficient mice; myeloid lineages, n = 7 control and Smarcd2-deficient mice; erythroid lineages, n = 4 control and Smarcd2-deficient mice; bone marrow progenitors and spleen: n = 5 control and Smarcd2-deficient mice per condition. (b) Smarcd2-deficient bone marrow hemopoietic stem cell (HSC) populations were analyzed 28 d after pI:pC treatment. Results are expressed as means ± s.e.m.; n = 3 control and 3 Smarcd2-deficient mice. (c) Representative FACS profiles of the results shown in b. (d) Smarcd2-deficient bone marrow, spleen and lung monocytic populations were analyzed 28 d after pI:pC treatment. Results are expressed as means ± s.e.m.; P values are from two-tailed t-tests with unequal variance; n = 3 control and 3 Smarcd2-deficient mice, except for lung where n = 2. Ery-I, proerythroblasts (Ter119lowCD71hi); Ery-II, basophilic erythroblasts (Ter119hiCD71hi); Ery-III, late erythroblasts (Ter119hiCD71med); Ery-IV, late erythroblasts (Ter119hiCD71low).
Supplementary Figure 5 In vivo administration of G-CSF or FLT3 fails to rescue the granulocyte differentiation defect of Smarcd2-deficient mice.
(a) Experimental design for in vivo rescue experiments of the Smarcd2 neutropenic phenotype using human recombinant G-CSF or FLT3 hemopoietic cytokines. (b) Absence of hematological response of Smarcd2-deficient granulocytic progenitors to the major cytokines for neutrophil granulocytes, G-CSF or FLT3, following daily intraperitoneal injections for 10 d. Representative FACS profiles of Smarcd2-deficient CD11b+Ly6G+ bone marrow cells analyzed 2 d after the last cytokine injection are shown; n = 3 independent experiments.
Supplementary Figure 6 Smarcd2-deficient end-stage (late-disease) animals display a block at the myelocyte/metamyelocyte stage of maturation with dysplastic features.
(a) Differential blood cell counts in Smarcd2-deficient LD and control animals performed by identifying 300 cells per peripheral blood smear based on morphology. Granulocytic precursors include myeloblasts to metamyelocytes. Numbers are given as means ±s.e.m. (b) Dysplastic cells in peripheral blood smears of Smarcd2-deficient LD animals. 1, myeloblast; 2, myelocyte; 3, promyelocyte; 4, myelocyte; 5, myeloblast; 6, promyelocyte; 7–9, myeloblasts; 10–12, WBCs with pseudo-Pelger–Huët anomaly and abnormal nuclei. (c) Representative images of Wright–Giemsa-stained cytospin preparations of LD Smarcd2-deficient total bone marrow cells. Note the relative increase in myelocytes and metamyelocytes and concomitant decrease in band and segmented neutrophils. (d) Differential cell counts performed by identifying 500 cells per bone marrow smear based on cell morphology. Dysplastic granulocytic cells include hyposegmented/atypical neutrophils, hypersegmented neutrophils and pseudo-Pelger–Huët. Numbers are given as means ± s.e.m.; n = 3 controls and n = 3 Smarcd2-deficient LD mice. (e) Magnification of the indicated area in c. P values are from one-tailed t-tests with unequal variance. PBL, peripheral blood cells; BM, bone marrow; lympho, lymphocytes; granu. prec., granulocytic precursors; seg. neutro, segmented neutrophils; dysplastic gran. cells; dysplastic granulocytic cells; LD, late disease (end stage).
Supplementary Figure 7 Hematological parameters of Smarcd2-deficient primary and secondary transplanted mice.
(a) Spleen weight and cellularity of Smarcd2-deficient early- and late-disease animals analyzed either 28 d after pI:pC treatment or when moribund. Results are expressed as means ± s.d.; n = 7 control and Smarcd2-deficient early-disease (ED) mice; n = 5 control and Smarcd2-deficient end-stage (LD) mice, except for the spleen cellularity of Smarcd2-deficient mice, where n = 3 mice. (b) Summary of the hematological parameters of mice transplanted with Smarcd2-deficient primary bone marrow cells (isolated when moribund) showing that the disease is not transplantable. n = 4 primary Smarcd2-deficient and 3 control bone marrows were used for transplantation. P values are from two-tailed t-tests with unequal variance.
Supplementary Figure 8 Severe impairment of lung function in Smarcd2-deficient end-stage (late-disease) animals.
(a) Pulmonary abnormalities in Smarcd2-deficient LD animals. Representative images of six independent animals are shown. See also Figure 2b. (b) Increased cellularity of LD Smarcd2-deficient lungs. Results are shown as means ± s.e.m. from five independent mice. (c) Increased frequency of CD34+CD11b+ (dysplastic) and CD11b+F4/80+ populations in LD Smarcd2-deficient lungs. Results are shown as means ± s.e.m. from four independent mice, except for CD11b+F4/80+ cells (n = 3 mice). (d) Anti-CD68 staining of a lung section of a Smarcd2-deficient end-stage animal showing nearly complete tissue consolidation by CD68+ macrophages. (e) Gram staining of a Smarcd2-deficient end-stage lung section showing no reactivity. P values are from two-tailed t-tests with unequal variance.
Supplementary Figure 9 No compensation by homologous family members in Smarcd1- and Smarcd2-deficient cells.
(a) The Smarcd1 conditional allele is a null allele (P.P., unpublished data). Western blot analysis of total bone marrow nuclear extracts from pI:pC-treated Smarcd1fl/fl × Mx1-Cre+ mice showing complete depletion of Smarcd1 on day 28 after and no compensation by the homologous Smarcd2 protein. An asterisk indicates a non-specific band. (b) mRNA levels of Smarcd1, Smarcd2, Smarcd3, CEBPA, CEBPB, CEBPE, Smarca2/Brm and Smarca4/Brg1 in Smarcd2-deficient and control granulocyte–macrophage progenitors (GMPs). Results are presented as mean TPM values ± s.e.m. from three independent experiments. P values are from two-tailed t-tests with unequal variance.
Supplementary Figure 10 Correlation coefficients of Smarcd2-deficient RNA–seq data sets in granulocyte–macrophage progenitors.
Replicate plots for each of the three independent samples per condition are shown. Pearson’s R values, Spearman and slopes (linear fitting model) indicate high correlation. Ctrl, control; KO, knockout; TPM, transcripts per million.
Supplementary Figure 11 Expression patterns of selected genes in purified human hemopoietic cell populations (RNA–seq data sets from n = 66 specimens).
(a) Expression patterns of human SMARCD2, CEBPE and CEBPA in purified human hemopoietic stem cells, myeloid, erythroid and lymphoid populations. RPKM values are shown. RNA–seq gene sets are from the Leucegene project (IRIC). (b,c) Expression patterns of the LTF, LCN2 and CAMP secondary granule genes (b) and the MPO, CTSG and ELANE primary granule genes (c) in the human hemopoietic cell populations shown in a. Cells derived from cord blood, bone marrow and peripheral blood are indicated in gray, red and blue, respectively. Sorting of populations was performed as described (Blood 27, 3054–3061, 2016). Cord blood CD34+, n = 5; CD34+CD45RA−, n = 12; nBM, n = 3; Ery-I and Ery-II, n = 2; Ery-III, n = 1; Ery-IV, n = 2; pre-B, n = 4; Gran-I, n = 3; Gran-II to Gran-V, n = 2; granulocytes, n = 5; monocytes, n = 5; B and T cells, n = 5; WBCs, n = 3; peripheral blood CD34+, n = 1 from a pool of 5 donors. Ery-I, most immature proerythroblasts (CD34+CD71+GlyA−); Ery-II, early erythroblasts (CD34−CD71+GlyA−); Ery-III, erythroblasts (CD34−CD71+GlyA+); Ery-IV, most mature erythroblasts (CD34−CD71−GlyA+); nBM, normal bone marrow; pre-B, B cell progenitors and precursors; Gran-I, myeloblasts and myelomonocytic progenitors and precursors; Gran-II, promyelocytes; Gran-III, myelocytes; Gran-IV, metamyelocytes; Gran-V, band and segmented neutrophils; WBCs, white blood cells; RPKM, reads per kilobase per million mapped reads.
Supplementary Figure 12 Genes most correlated with LTF, MPO and CEBPE.
(a–c) Genes co-regulated with LTF (secondary granule) (a), MPO (primary granule) (b) and CEBPE (c) in the human hemopoietic stem cells and myeloid, erythroid and lymphoid populations shown in Supplementary Figure 11 (n = 66 specimens). Pearson correlations were performed using log10 RPKM values from the normal cell populations detailed in Supplementary Figure 11. Correlations are shown for the 5,000 most correlated genes. See Supplementary Table 3 for full lists of genes with a correlation score ≥0.5. RPKM, reads per kilobase per million mapped reads.
Supplementary Figure 13 Smarcd2 structure–function analysis in Smarcd2-deficient Lin− bone marrow cells using an in vitro OP9 granulocyte differentiation model.
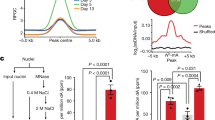
(a) Although all Smarcd2 mutants were expressed at levels similar to (or higher than) that of the exogenously expressed wild-type protein, Smarcd2 mutants lacking either the C1 or SWIB domain failed to rescue the granulocyte differentiation defect of Smarcd2-deficient Lin− bone marrow cells. Results are expressed as means ± s.e.m. Biological replicates per condition: Ctrl cells: GFP, n = 9; KO cells: GFP and ΔN(l), n = 8; WT, n = 10; ΔN(s), n = 7; ΔC1 and ΔS, n = 6; ΔINT, n = 3; ΔC2 and ΔC3, n = 2. (b) ChIP on the Onecut (negative control; no predicted CEBPɛ-binding sites) and Ltf promoters in Smarcd2-deficient and control Lin− bone marrow cells using anti-Brg1/Brm (J1) (Onecut; left) and anti-p53 (Ltf; right) antibodies. Chromatin extracts were prepared on day 14 of culture on OP9 stromal cells. Purified rabbit or mouse IgG was used as a control. Primers are within 500 bp of the TSSs. For Ltf, the amplicon was the same as in Figure 6c encompassing the CEBPɛ-binding site. Results are presented as means ± s.e.m. from three independent samples. (c) qPCR analyses of Camp and S100a8 secondary granule gene expression in NIH/3T3 cells stably expressing CEBPE or an empty vector. Results are presented as means ± s.e.m. of three independent samples; P values are from two-tailed t-tests with unequal variance. nd, non-detectable.
Supplementary Figure 14 Bioinformatics analyses of Smarcd1, Smarcd2, Smarcd3 and CEBP family proteins.
(a) Bioinformatics studies revealed that the SWIB domain of SMARCD2 (of unknown function) is closely related to hydrophobic regions of MDM2 that allow interaction with the p53 α-helix (from Bennett-Lovsey, R., Hart, S.E., Shirai, H. & Mizuguchi, K. The SWIB and the MDM2 domains are homologous and share a common fold. Bioinformatics 18, 626–630, 2002, by permission of Oxford University Press). (b) Bioinformatics analysis predicts that the C1 domain of human SMARCD2 (amino acids 166–186) is not conserved in the SMARCD1 and SMARCD3 proteins. Coiled-coil prediction software was from https://npsa-prabi.ibcp.fr/cgi-bin/npsa_automat.pl?page=/NPSA/npsa_lupas.html. Blue, green and red lines represent domain predictions based on scanning windows of 28, 21 and 14 residues, respectively. (c) Several residues in the human SMARCD2 SWIB domain expected to be involved in α-helix interactions (asterisks) are not conserved in the homologous SMARCD1 and SMARCD3 proteins. The position of predicted α-helices is indicated (black lines). The SMARCD2 C1 domain (amino acids 166–186) is not conserved in the homologous SMARCD1 and SMARCD3 subunits, potentially because of substitutions of residues involved in protein folding. An arginine serine motif in the basic leucine zipper domain of CEBPɛ (asterisks) expected to be required for its transcriptional activity is not conserved in the homologous CEBPα, CEBPβ, CEPBγ and CEBPδ proteins. (d) Coimmunoprecipitation experiments in nuclear extracts from 293 cells expressing the different FLAG-tagged Smarcd2 deletion mutants performed using anti-Brg1/Brm (J1) antibody. The Smarcd2 C2 and C3 domains are essential for its integration within the SWI/SNF complex. FLAG-tagged BMI1 protein was used as a negative control.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–14 (PDF 3638 kb)
Supplementary Table 1
List of antibodies used in these studies. (XLSX 9 kb)
Supplementary Table 2
TPM values of RNA–seq data sets of BAF60b-knockout and control granulocyte–macrophage progenitors (n = 3 independent experiments). (XLSX 7847 kb)
Supplementary Table 3
Prediction of CEBPɛ-binding sites in the promoter of neutrophilic granule genes expressed at a mean TPM value above 0.3 in control granulocyte–macrophage progenitors (n = 3 independent experiments). (XLSX 127 kb)
Supplementary Table 4
List of oligonucleotides used in these studies. (XLSX 9 kb)
Rights and permissions
About this article
Cite this article
Priam, P., Krasteva, V., Rousseau, P. et al. SMARCD2 subunit of SWI/SNF chromatin-remodeling complexes mediates granulopoiesis through a CEBPɛ dependent mechanism. Nat Genet 49, 753–764 (2017). https://doi.org/10.1038/ng.3812
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ng.3812
This article is cited by
-
SWI/SNF complexes in hematological malignancies: biological implications and therapeutic opportunities
Molecular Cancer (2023)
-
BRD9 determines the cell fate of hematopoietic stem cells by regulating chromatin state
Nature Communications (2023)
-
In vivo screening characterizes chromatin factor functions during normal and malignant hematopoiesis
Nature Genetics (2023)
-
BAF53A drives colorectal cancer development by regulating DUSP5-mediated ERK phosphorylation
Cell Death & Disease (2022)
-
A Novel CEBPE Variant Causes Severe Infections and Profound Neutropenia
Journal of Clinical Immunology (2022)