Abstract
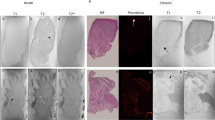
Myocardial viability is of established importance to the management of cardiac patients being considered for revascularization. Existing noninvasive imaging tests to examine myocardial viability, such as stress echocardiography and nuclear scintigraphy, are of recognized utility but are subject to intrinsic limitations. Over the past few years delayed-enhancement MRI (DE-MRI) has emerged as an alternative to traditional tests and for the first time allows direct visualization of the transmural extent of myocardial viability. In this paper we review the scientific data that underlie the use of DE-MRI in patients with ischemic heart disease. Progress in this area is largely the result of the development of a new MRI pulse sequence in the late 1990s, which improved the detection of necrotic and scarred myocardial tissue. Following this technical development, a series of detailed histologic comparisons in large animal models revealed that both acute and healed myocardial infarcts appeared as brighter (hyperenhanced) areas than viable regions, and that the effect is independent of contractile function. The resulting 'bright is dead' hypothesis has thus far proven of significant use in patients with ischemic heart disease. Data are now emerging which suggest that the DE-MRI technique also has important implications for patients with nonischemic forms of cardiomyopathy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
National Institutes for Health, National Heart, Lung, and Blood Institute (2002) Morbidity and mortality: Chart book on cardiovascular, lung, and blood diseases. Bethesda, MD: NIH/NHLBI
American Heart Association (2004) Heart Disease and Stroke Statistics—2004: update. Dallas, TX: American Heart Association
Harris PJ et al. (1979) Survival in medically treated coronary artery disease. Circulation 60: 1259–1269
Hammermeister KE et al. (1979) Variables predictive of survival in patients with coronary disease. Selection by univariate and multivariate analyses from the clinical, electrocardiographic, exercise, arteriographic, and quantitative angiographic evaluations. Circulation 59: 421–430
Mock MB et al. (1982) Survival of medically treated patients in the coronary artery surgery study (CASS) registry. Circulation 66: 562–568
Allman KC et al. (2002) Myocardial viability testing and impact of revascularization on prognosis in patients with coronary artery disease and left ventricular dysfunction: a meta-analysis. J Am Coll Cardiol 39: 1151–1158
Bonow RO (1996) Identification of viable myocardium. Circulation 94: 2674–2680
Weinmann HJ et al. (1984) Characteristics of gadolinium-DTPA complex: a potential NMR contrast agent AJR Am J Roentgenol 142: 619–624
Dendale P et al. (1998) Contrast enhanced and functional magnetic resonance imaging for the detection of viable myocardium after infarction. Am Heart J 135: 875–880
Yokota C et al. (1995) Gadolinium-enhanced magnetic resonance imaging in acute myocardial infarction. Am J Cardiol 75: 577–581
Simonetti OP et al. (2001) An Improved MR Imaging Technique for the Visualization of Myocardial Infarction. Radiology 218: 215–223
Rehr RB et al. (1986) Improved in vivo magnetic resonance imaging of acute myocardial infarction after intravenous paramagnetic contrast agent administration. Am J Cardiol 57: 864–868
McNamara MT et al. (1986) Differentiation of reversible and irreversible myocardial injury by MR imaging with and without gadolinium-DTPA. Radiology 158: 765–769
Peshock RM et al. (1986) Magnetic resonance imaging of acute myocardial infarction: gadolinium diethylenetriamine pentaacetic acid as a marker of reperfusion. Circulation 74: 1434–1440
Van Rossum AC et al. (1990) Value of gadolinium-diethylene-triamine pentaacetic acid dynamics in magnetic resonance imaging of acute myocardial infarction with occluded and reperfused coronary arteries after thrombolysis. Am J Cardiol 65: 845–851
van der Wall EE et al. (1995) Magnetic resonance imaging in coronary artery disease. Circulation 92: 2723–2739
de Roos A et al. (1989) Reperfused and nonreperfused myocardial infarction: diagnostic potential of Gd-DTPA—enhanced MR imaging. Radiology 172: 717–720
Lima JA et al. (1995) Regional heterogeneity of human myocardial infarcts demonstrated by contrast-enhanced MRI. Potential mechanisms. Circulation 92: 1117–1125
Judd RM et al. (1995) Physiological basis of myocardial contrast enhancement in fast magnetic resonance images of 2-day-old reperfused canine infarcts. Circulation 92: 1902–1910
Nishimura T et al. (1989) Determination of infarct size of acute myocardial infarction in dogs by magnetic resonance imaging and gadolinium-DTPA: comparison with indium-111 antimyosin imaging. Am J Physiol Imaging 4: 83–88
Schaeffer S et al. (1988) Gadolinium-DTPA-enhanced nuclear magnetic resonance imaging of reperfused myocardium identification of the myocardial bed at risk. J Am Coll Cardiol 12: 1064–1072
Eichstaedt HW et al. (1986) Magnetic resonance imaging (MRI) in different stages of myocardial infarction using the contrast agent gadolinium-DTPA. Clin Cardiol 9: 527–535
Matheijssen NA et al. (1991) Acute myocardial infarction: comparison of T2-weighted and T1-weighted gadolinium-DTPA enhanced MR imaging. Magn Reson Med 17: 460–409
Pereira RS et al. (1996) The determination of myocardial viability using Gd-DTPA in a canine model of acute myocardial ischemia and reperfusion. Magn Reson Med 36: 684–693
Rogers WJ Jr et al. (1999) Early contrast-enhanced MRI predicts late functional recovery after reperfused myocardial infarction. Circulation 99: 744–750
Wagner A et al. (2003) Contrast-enhanced MRI and routine single photon emission computed tomography (SPECT) perfusion imaging for detection of subendocardial myocardial infarcts: an imaging study. Lancet 361: 374–379
Kim RJ et al. (1999) Relationhip of MRI delayed contrast enhancement to irreversible injury infarct age and contractile function. Circulation 100: 1992–2002
Fieno DS et al. (2000) Contrast-enhanced magnetic resonance imaging of myocardium at risk: distinction between reversible and irreversible injury throughout infarct healing. J Am Coll Cardiol 36: 1985–1991
Barkhausen J et al. (2002) Imaging of myocardial infarction: comparison of magnevist and gadophrin-3 in rabbits. J Am Coll Cardiol 39: 1392–1398
Wu E et al. (2001) Visualisation of presence location and transmural extent of healed Q- wave and non-Q-wave myocardial infarction Lancet 357: 21–28
Kim RJ et al. (2000) The use of contrast-enhanced magnetic resonance imaging to identify reversible myocardial dysfunction. N Engl J Med 343: 1445–1453
Klein C et al. (2002) Assessment of Myocardial Viability With Contrast-Enhanced Magnetic Resonance Imaging: Comparison With Positron Emission Tomography. Circulation 105: 162–167
Hillenbrand HB et al. (2000) Early assessment of myocardial salvage by contrast-enhanced magnetic resonance imaging. Circulation 102: 1678–1683
Choi K et al. (2001) The transmural extent of acute myocardial infarction predicts long term improvement in contractile function. Circulation 104: 1101–1107
Gerber BL et al. (2002) Accuracy of contrast-enhanced magnetic resonance imaging in predicting improvement of regional myocardial function in patients after acute myocardial infarction. Circulation 106: 1083–1089
Rehwald WG et al. (2002) Myocardial magnetic resonance imaging contrast agent concentrations after reversible and irreversible ischemic injury. Circulation 105: 224–229
Reimer KA and Jennings RB (1992) The Heart and Cardiovascular System, 1875–1973 (Eds Fozzard HA et al.) New York, NY: Raven Press
Jennings RB et al. (1985) Effect of reperfusion late in the phase of reversible ischemic injury. Changes in cell volume electrolytes metabolites and ultrastructure. Circ Res 56: 262–278
Rochitte CE et al. (1998) Magnitude and time course of microvascular obstruction and tissue injury after acute myocardial infarction. Circulation 98: 1006–1014
Cerqueira MD et al. (2002) Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart: a statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation 105: 539–542
Mahrholdt H et al. (2004) Cardiovascular magnetic resonance assessment of human myocarditis: a comparison to histology and molecular pathology. Circulation 109: 1250–1258
Patel M et al. (2004) Improved diagnostic densitivity of contrast enhanced cardiac MRI for cardiac sarcoidosis [abstract]. Circulation 110 (suppl): 645
Choudhury L et al. (2002) Myocardial scarring in asymptomatic or mildly symptomatic patients with hypertrophic cardiomyopathy. J Am Coll Cardiol 40: 2156–2564
Moon JC et al. (2003) Toward clinical risk assessment in hypertrophic cardiomyopathy with gadolinium cardiovascular magnetic resonance. J Am Coll Cardiol 41: 1561–1567
Prasad S and Pennell DJ (2002) Magnetic resonance imaging in the assessment of patients with heart failure. J Nucl Cardiol 9: 60S–70S
Acknowledgements
We thank Joao AC Lima, Elias A Zerhouni, Francis Klocke, Robert O Bonow, Thomas Holly, Michelle Parker, Kathleen Harris, Todd Parrish, Paul Finn, Orlando Simonetti, Jeffrey Bundy and Michael Elliot for their helpful contributions to the development of the delayed enhancement technique and to the understanding of its physiologic relevance. Grants were received from NIH (National Institutes for Health) and NHLBI (National Heart, Lung, and Blood Institute).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Robert M Judd and Raymond J Kim are consultants for Tyco and Mallinckrodt, and are inventors on a related US patent owned by Northwestern University
Glossary
- DELAYED-ENHANCEMENT MRI (DE-MRI)
-
Images are acquired 5–30 min after contrast agent administration rather than during the myocardial first pass, hence 'delayed enhancement'
- CINE MRI
-
Sequential cinematic presentation of multiple images (typically 16–20) corresponding to different phases of the cardiac phases to assess contractile function
Rights and permissions
About this article
Cite this article
Judd, R., Wagner, A., Rehwald, W. et al. Technology Insight: assessment of myocardial viability by delayed-enhancement magnetic resonance imaging. Nat Rev Cardiol 2, 150–158 (2005). https://doi.org/10.1038/ncpcardio0134
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpcardio0134
This article is cited by
-
Can cardiac magnetic resonance imaging reclassify uremic cardiomyopathy in patients with end-stage renal failure?
Nature Clinical Practice Cardiovascular Medicine (2007)
-
Characterization of myocardial viability using MR and CT imaging
European Radiology (2007)
-
Rationale and design of the SMART Heart study
Netherlands Heart Journal (2007)
-
Assessment of no-reflow regions using cardiac MRI
Basic Research in Cardiology (2006)