Abstract
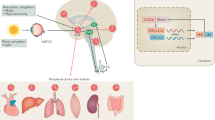
Parkinson's disease (PD) is a chronic and progressive neurodegenerative disorder. Although rare genetically linked cases of PD have been reported, most incidences are sporadic in nature. Late-onset, sporadic PD is thought to result from the combined effects of genetic and environmental risk factors exposure. Sleep and circadian rhythm disorders are recurrent among PD patients and appear early in the disease. Although some evidence supports a relationship between circadian disruption (CD) and PD, whether this is secondary to the motor symptoms or, indeed, is a factor that contributes to the pathogenesis of the disease remains to be investigated. In the present paper, we studied the direct consequence of chronic CD on the development of the phenotype in the MPTP (1-methyl-4-phenyl-1,2,3,6-tetrahydropyridinen) model of PD. Pre-exposure to CD to mice treated with MPTP resulted in an exacerbation of motor deficit and a significant reduction in the capability of acquiring motor skills. These changes were associated with a greater loss of tyrosine hydroxylase cell content and intense neuroinflammation. Taken together, our findings demonstrate that CD by triggering a robust neuroinflammatory reaction and degeneration of the nigral-dopaminergic neuronal system exacerbates motor deficit. They support the novel hypothesis that circadian rhythm disorder is an environmental risk factor for developing PD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Goedert M, Spillantini MG, Del Tredici K, Braak H . 100 years of Lewy pathology. Nat Rev Neurol 2013; 9: 13–24.
Wilson RS, Arnold SE, Schneider JA, Kelly JF, Tang Y, Bennet DA . Chronic psychological distress and risk of Alzheimer’s disease in old age. Neuroepidemiology 2006; 27: 143–153.
Comella CL . Sleep disturbances and excessive daytime sleepiness in Parkinson’s disease: an overview. J Neural Transm Suppl 2006; 70: 349–355.
Lima MMS, Andersen ML, Reksidler AB, MABF Vital, Tufik S . The role of the substantia nigra pars compacta in regulating sleep patterns in rats. PLoS ONE 2007; 2: e513.
Chen H, Schernhammer R, Schwarzschild MA, Ascherio A . A prospective study of night shift work, sleep duration, and risk of Parkinson’s disease. Am J Epidemiol 2006; 163: 726–730.
Gao J, Huang X, Park Y, Hollenbeck A, Blair A, Schatzkin et al. Daytime napping: night-time sleeping, and Parkinson’s disease. Am J Epidemiol 2011; 173: 1032–1038.
Abbot RD, Ross GW, White LR, Tanner CM, Masaki KH, Nelson JS et al. Excessive daytime sleepiness and subsequent development of Parkinson’s disease. Neurology 2005; 65: 1442–1446.
Di Meco A, Joshi YB, Praticò D . Sleep deprivation impairs memory, tau metabolism, and synaptic integrity of a mouse model of Alzheimer's disease with plaques and tangles. Neurobiol Aging 2014; 35: 1813–1820.
Coppi A, Merali S, Eichinger D . The enteric parasite Entamoeba uses an autocrine catecholamine system during differentiation into the infectious cyst stage. J Biol Chem 2002; 277: 8083–8090.
Merali S, Clarkson AB . Polyamine analysis using N-hydroxysuccinimidyl-6-aminoquinoyl carbamate for pre-column derivatization. J Chromatogr B Biomed Sci Appl 1996; 675: 321–326.
Lauretti E, Di Meco A, Chu J, Praticò D . Modulation of AD neuropathology and memory impairments by the isoprostane F2α is mediated by the thromboxane receptor. Neurobiol Aging 2014; 36: 812–820.
Joshi YB, Giannopoulos PF, Chu J, Sperow M, Kirby LG, Abood ME et al. Absence of ALOX5 gene prevents stress-induced memory deficits, synaptic dysfunction and tauopathy in a mouse model of Alzheimer's disease. Hum Mol Genet 2014; 23: 6894–6902.
Sedelis M, Hofele K, Auburger GW, Morgan S, Huston JP, Schwarting RK . MPTP susceptibility in the mouse: behavioral, neurochemical, and histological analysis of gender and strain differences. Behav Genet 2000; 30: 171–182.
Lim MM, Xu J, Holtzman DM, Mach RH . Sleep deprivation differentially affects dopamine receptor subtypes in mouse striatum. Neuroreport 2011; 22: 489–493.
Willison LD, Kudo T, Loh DH, Kuljis D, Colwell CS . Circadian dysfunction may be a key component of the non-motor symptoms of Parkinson's disease: insights from a transgenic mouse model. Exp Neurol 2013; 243: 57–66.
Campos Costa I, Nogueira Carvalho H, Fernandes L . Aging, circadian rhythms and depressive disorders: a review. Am J. Neurodegener Dis 2013; 2: 228–246.
Castanon-Cervantes O, Wu M, Ehlen JC, Paul K, Gamble KL, Johnson RL et al. Dysregulation of inflammatory responses by chronic circadian disruption. J Immunol 2010; 185: 5796–5805.
Buxton OM, Marcelli E . Short and long sleep are positively associated with obesity, diabetes, hypertension, and cardiovascular disease among adults in the United States. Soc Sci Med 2010; 71: 1027–1036.
Lima MM, Reksidler AB, Vital MA . The neurobiology of the substantia nigra pars compacta: from motor to sleep regulation. J Neural Transm Suppl 2009; 135–145.
Hood S, Cassidy P, Cossette MP, Weigl Y, Verwey M, Robinson B et al. Endogenous dopamine regulates the rhythm of expression of the clock protein PER2 in the rat dorsal striatum via daily activation of D2 dopamine receptors. J Neurosci 2010; 30: 14046–14058.
Videnovic A, Golombek D . Circadian and sleep disorders in Parkinson's disease. Exp Neurol 2013; 243: 45–56.
Parekh PK, Ozburn AR, McClung CA . Circadian clock genes: effects on dopamine, reward and addiction. Alcohol 2015; 49: 341–349.
Smeyne RJ . Vernice Jackson-Lewis. The MPTP model of Parkinson's disease. Mol Brain Res 2005; 134: 55–67.
Rappold PM, Tieu K . Astrocytes and therapeutics for Parkinson's disease. Neurotherapeutics 2010; 7: 413–423.
Acknowledgements
This study was supported in part by the Wanda Simone Endowment for Neuroscience (PD). We are grateful to Dr Anna M Gumpert for technical assistance with the Imaging Software NIS Element AR.
Author contributions
EL and DP conceived and designed the study, EL and DP wrote the manuscript, EL, ADM and SM performed the experiments. All authors reviewed and approved the final version of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Lauretti, E., Di Meco, A., Merali, S. et al. Circadian rhythm dysfunction: a novel environmental risk factor for Parkinson’s disease. Mol Psychiatry 22, 280–286 (2017). https://doi.org/10.1038/mp.2016.47
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2016.47
This article is cited by
-
Downregulation of CDK5 signaling in the dorsal striatum alters striatal microcircuits implicating the association of pathologies with circadian behavior in mice
Molecular Brain (2022)
-
The circadian clock protein Rev-erbα provides neuroprotection and attenuates neuroinflammation against Parkinson’s disease via the microglial NLRP3 inflammasome
Journal of Neuroinflammation (2022)
-
Sleep and circadian rhythms in Parkinson’s disease and preclinical models
Molecular Neurodegeneration (2022)
-
Circadian rhythms in neurodegenerative disorders
Nature Reviews Neurology (2022)
-
Altered Motor Performance, Sleep EEG, and Parkinson’s Disease Pathology Induced by Chronic Sleep Deprivation in Lrrk2G2019S Mice
Neuroscience Bulletin (2022)