Abstract
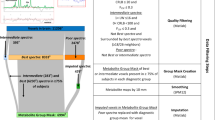
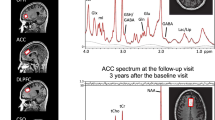
Proton magnetic resonance spectroscopy (1H MRS) neurometabolite abnormalities have been detected widely in subjects with and at risk for schizophrenia. We hypothesized that such abnormalities would be present both in patients with schizophrenia and in their unaffected twin siblings. We acquired magnetic resonance spectra (TR/TE=3000/30 ms) at voxels in the mesial prefrontal gray matter, left prefrontal white matter and left hippocampus in 14 twin pairs discordant for schizophrenia (2 monozygotic, 12 dizygotic), 13 healthy twin pairs (4 monozygotic, 9 dizygotic) and 1 additional unaffected co-twin of a schizophrenia proband. In the mesial prefrontal gray matter voxel, N-acetylaspartate (NAA), creatine+phosphocreatine (Cr), glycerophosphocholine+phosphocholine (Cho) and myo-inositol (mI) did not differ significantly between patients with schizophrenia, their unaffected co-twins or healthy controls. However, glutamate (Glu) was significantly lower in patients with schizophrenia (31%, percent difference) and unaffected co-twins (21%) than in healthy controls (collapsed across twin pairs). In the left hippocampus voxel, levels of NAA (23%), Cr (22%) and Cho (36%) were higher in schizophrenia patients compared with controls. Hippocampal NAA (25%), Cr (22%) and Cho (37%) were also significantly higher in patients than in their unaffected co-twins. Region-to-region differences in metabolite levels were also notable within all three diagnosis groups. These findings suggest that 1H MRS neurometabolite abnormalities are present not only in patients with schizophrenia, but also in their unaffected co-twins. Thus, reduced mesial prefrontal cortical Glu and elevated hippocampal NAA, Cr and Cho may represent trait markers of schizophrenia risk and, when exacerbated, state markers of schizophrenia itself.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Karlsgodt KH, Glahn DC, van Erp TG, Therman S, Huttunen M, Manninen M et al. The relationship between performance and fMRI signal during working memory in patients with schizophrenia, unaffected co-twins, and control subjects. Schizophr Res 2007; 89: 191–197.
van Erp TG, Saleh PA, Huttunen M, Lonnqvist J, Kaprio J, Salonen O et al. Hippocampal volumes in schizophrenic twins. Arch Gen Psychiatry 2004; 61: 346–353.
Cannon TD, Huttunen MO, Lonnqvist J, Tuulio-Henriksson A, Pirkola T, Glahn D et al. The inheritance of neuropsychological dysfunction in twins discordant for schizophrenia. Am J Hum Genet 2000; 67: 369–382.
Moffett JR, Namboodiri AM . Preface: a brief review of N-acetylaspartate. Adv Exp Med Biol 2006; 576: vii–xiii.
Baslow MH, Suckow RF, Gaynor K, Bhakoo KK, Marks N, Saito M et al. Brain damage results in down-regulation of N-acetylaspartate as a neuronal osmolyte. Neuromolecular Med 2003; 3: 95–104.
Bates TE, Strangward M, Keelan J, Davey GP, Munro PM, Clark JB . Inhibition of N-acetylaspartate production: implications for 1H MRS studies in vivo. Neuroreport 1996; 7: 1397–1400.
Dautry C, Vaufrey F, Brouillet E, Bizat N, Henry PG, Conde F et al. Early N-acetylaspartate depletion is a marker of neuronal dysfunction in rats and primates chronically treated with the mitochondrial toxin 3-nitropropionic acid. J Cereb Blood Flow Metab 2000; 20: 789–799.
Gasparovic C, Arfai N, Smid N, Feeney DM . Decrease and recovery of N-acetylaspartate/creatine in rat brain remote from focal injury. J Neurotrauma 2001; 18: 241–246.
Battistuta J, Bjartmar C, Trapp BD . Postmortem degradation of N-acetylaspartate and N-acetyl aspartylglutamate: an HPLC analysis of different rat CNS regions. Neurochem Res 2001; 26: 695–702.
Vrenken H, Barkhof F, Uitdehaag BM, Castelijns JA, Polman CH, Pouwels PJ . MR spectroscopic evidence for glial increase but not for neuro-axonal damage in MS normal-appearing white matter. Magn Reson Med 2005; 53: 256–266.
Novotny Jr EJ, Fulbright RK, Pearl PL, Gibson KM, Rothman DL . Magnetic resonance spectroscopy of neurotransmitters in human brain. Ann Neurol 2003; 54 (Suppl 6): S25–S31.
Rothman DL, Sibson NR, Hyder F, Shen J, Behar KL, Shulman RG . In vivo nuclear magnetic resonance spectroscopy studies of the relationship between the glutamate–glutamine neurotransmitter cycle and functional neuroenergetics. Philos Trans R Soc Lond B Biol Sci 1999; 354: 1165–1177.
Erecinska M, Silver IA . ATP and brain function. J Cereb Blood Flow Metab 1989; 9: 2–19.
Miller BL . A review of chemical issues in 1H NMR spectroscopy: N-acetyl-L-aspartate, creatine and choline. NMR Biomed 1991; 4: 47–52.
Irvine RF, Schell MJ . Back in the water: the return of the inositol phosphates. Nat Rev Mol Cell Biol 2001; 2: 327–338.
Abbott C, Bustillo J . What have we learned from proton magnetic resonance spectroscopy about schizophrenia? A critical update. Curr Opin Psychiatry 2006; 19: 135–139.
Wobrock T, Scherk H, Falkai P . [Magnetic resonance spectroscopy in schizophrenia. Possibilities and limitations]. Radiologe 2005; 45: 124–130, 132–126.
Keshavan MS, Stanley JA, Pettegrew JW . Magnetic resonance spectroscopy in schizophrenia: methodological issues and findings—part II. Biol Psychiatry 2000; 48: 369–380.
Sanches RF, Crippa JA, Hallak JE, Araujo D, Zuardi AW . Proton magnetic resonance spectroscopy of the frontal lobe in schizophrenics: a critical review of the methodology. Rev Hosp Clin Fac Med Sao Paulo 2004; 59: 145–152.
Steen RG, Hamer RM, Lieberman JA . Measurement of brain metabolites by 1H magnetic resonance spectroscopy in patients with schizophrenia: a systematic review and meta-analysis. Neuropsychopharmacology 2005; 30: 1949–1962.
Bertolino A, Nawroz S, Mattay VS, Barnett AS, Duyn JH, Moonen CT et al. Regionally specific pattern of neurochemical pathology in schizophrenia as assessed by multislice proton magnetic resonance spectroscopic imaging. Am J Psychiatry 1996; 153: 1554–1563.
Selemon LD, Rajkowska G, Goldman-Rakic PS . Elevated neuronal density in prefrontal area 46 in brains from schizophrenic patients: application of a three-dimensional, stereologic counting method. J Comp Neurol 1998; 392: 402–412.
Selemon LD, Rajkowska G, Goldman-Rakic PS . Abnormally high neuronal density in the schizophrenic cortex. A morphometric analysis of prefrontal area 9 and occipital area 17. Arch Gen Psychiatry 1995; 52: 805–818; discussion 819–820.
Bertolino A, Callicott JH, Elman I, Mattay VS, Tedeschi G, Frank JA et al. Regionally specific neuronal pathology in untreated patients with schizophrenia: a proton magnetic resonance spectroscopic imaging study. Biol Psychiatry 1998; 43: 641–648.
Cecil KM, Lenkinski RE, Gur RE, Gur RC . Proton magnetic resonance spectroscopy in the frontal and temporal lobes of neuroleptic naive patients with schizophrenia. Neuropsychopharmacology 1999; 20: 131–140.
Renshaw PF, Yurgelun-Todd DA, Tohen M, Gruber S, Cohen BM . Temporal lobe proton magnetic resonance spectroscopy of patients with first-episode psychosis. Am J Psychiatry 1995; 152: 444–446.
Bertolino A, Sciota D, Brudaglio F, Altamura M, Blasi G, Bellomo A et al. Working memory deficits and levels of N-acetylaspartate in patients with schizophreniform disorder. Am J Psychiatry 2003; 160: 483–489.
Block W, Bayer TA, Tepest R, Traber F, Rietschel M, Muller DJ et al. Decreased frontal lobe ratio of N-acetylaspartate to choline in familial schizophrenia: a proton magnetic resonance spectroscopy study. Neurosci Lett 2000; 289: 147–151.
Callicott JH, Egan MF, Bertolino A, Mattay VS, Langheim FJ, Frank JA et al. Hippocampal N-acetylaspartate in unaffected siblings of patients with schizophrenia: a possible intermediate neurobiological phenotype. Biol Psychiatry 1998; 44: 941–950.
Thomas MA, Ke Y, Levitt J, Caplan R, Curran J, Asarnow R et al. Preliminary study of frontal lobe 1H MR spectroscopy in childhood-onset schizophrenia. J Magn Reson Imaging 1998; 8: 841–846.
Jessen F, Scherk H, Traber F, Theyson S, Berning J, Tepest R et al. Proton magnetic resonance spectroscopy in subjects at risk for schizophrenia. Schizophr Res 2006; 87: 81–88.
Farber NB, Kim SH, Dikranian K, Jiang XP, Heinkel C . Receptor mechanisms and circuitry underlying NMDA antagonist neurotoxicity. Mol Psychiatry 2002; 7: 32–43.
Olney JW, Newcomer JW, Farber NB . NMDA receptor hypofunction model of schizophrenia. J Psychiatr Res 1999; 33: 523–533.
Stanley JA . In vivo magnetic resonance spectroscopy and its application to neuropsychiatric disorders. Can J Psychiatry 2002; 47: 315–326.
Fenton WS, Hibbeln J, Knable M . Essential fatty acids, lipid membrane abnormalities, and the diagnosis and treatment of schizophrenia. Biol Psychiatry 2000; 47: 8–21.
Horrobin DF, Glen AI, Vaddadi K . The membrane hypothesis of schizophrenia. Schizophr Res 1994; 13: 195–207.
Auer DP, Wilke M, Grabner A, Heidenreich JO, Bronisch T, Wetter TC . Reduced NAA in the thalamus and altered membrane and glial metabolism in schizophrenic patients detected by 1H-MRS and tissue segmentation. Schizophr Res 2001; 52: 87–99.
Theberge J, Al-Semaan Y, Drost DJ, Malla AK, Neufeld RW, Bartha R et al. Duration of untreated psychosis vs N-acetylaspartate and choline in first episode schizophrenia: a 1H magnetic resonance spectroscopy study at 4.0 Tesla. Psychiatry Res 2004; 131: 107–114.
Sharma R, Venkatasubramanian PN, Barany M, Davis JM . Proton magnetic resonance spectroscopy of the brain in schizophrenic and affective patients. Schizophr Res 1992; 8: 43–49.
Bluml S, Tan J, Harris K, Adatia N, Karme A, Sproull T et al. Quantitative proton-decoupled 31P MRS of the schizophrenic brain in vivo. J Comput Assist Tomogr 1999; 23: 272–275.
Auer DP, Putz B, Kraft E, Lipinski B, Schill J, Holsboer F . Reduced glutamate in the anterior cingulate cortex in depression: an in vivo proton magnetic resonance spectroscopy study. Biol Psychiatry 2000; 47: 305–313.
Lim KO, Adalsteinsson E, Spielman D, Sullivan EV, Rosenbloom MJ, Pfefferbaum A . Proton magnetic resonance spectroscopic imaging of cortical gray and white matter in schizophrenia. Arch Gen Psychiatry 1998; 55: 346–352.
Steel RM, Bastin ME, McConnell S, Marshall I, Cunningham-Owens DG, Lawrie SM et al. Diffusion tensor imaging (DTI) and proton magnetic resonance spectroscopy (1H MRS) in schizophrenic subjects and normal controls. Psychiatry Res 2001; 106: 161–170.
Ende G, Braus DF, Walter S, Weber-Fahr W, Soher B, Maudsley AA et al. Effects of age, medication, and illness duration on the N-acetylaspartate signal of the anterior cingulate region in schizophrenia. Schizophr Res 2000; 41: 389–395.
Yamasue H, Fukui T, Fukuda R, Yamada H, Yamasaki S, Kuroki N et al. 1H-MR spectroscopy and gray matter volume of the anterior cingulate cortex in schizophrenia. Neuroreport 2002; 13: 2133–2137.
Theberge J, Al-Semaan Y, Williamson PC, Menon RS, Neufeld RW, Rajakumar N et al. Glutamate and glutamine in the anterior cingulate and thalamus of medicated patients with chronic schizophrenia and healthy comparison subjects measured with 4.0-T proton MRS. Am J Psychiatry 2003; 160: 2231–2233.
Theberge J, Bartha R, Drost DJ, Menon RS, Malla A, Takhar J et al. Glutamate and glutamine measured with 4.0 T proton MRS in never-treated patients with schizophrenia and healthy volunteers. Am J Psychiatry 2002; 159: 1944–1946.
Keshavan MS, Montrose DM, Pierri JN, Dick EL, Rosenberg D, Talagala L et al. Magnetic resonance imaging and spectroscopy in offspring at risk for schizophrenia: preliminary studies. Prog Neuropsychopharmacol Biol Psychiatry 1997; 21: 1285–1295.
Tibbo P, Hanstock C, Valiakalayil A, Allen P . 3-T proton MRS investigation of glutamate and glutamine in adolescents at high genetic risk for schizophrenia. Am J Psychiatry 2004; 161: 1116–1118.
Omori M, Pearce J, Komoroski RA, Griffin WS, Mrak RE, Husain MM et al. In vitro 1H-magnetic resonance spectroscopy of postmortem brains with schizophrenia. Biol Psychiatry 1997; 42: 359–366.
Jentsch JD, Roth RH . The neuropsychopharmacology of phencyclidine: from NMDA receptor hypofunction to the dopamine hypothesis of schizophrenia. Neuropsychopharmacology 1999; 20: 201–225.
Laruelle M, Kegeles LS, Abi-Dargham A . Glutamate, dopamine, and schizophrenia: from pathophysiology to treatment. Ann NY Acad Sci 2003; 1003: 138–158.
Olney JW, Farber NB . Glutamate receptor dysfunction and schizophrenia. Arch Gen Psychiatry 1995; 52: 998–1007.
Kaprio J, Koskenvuo M . Genetic and environmental factors in complex diseases: the older Finnish Twin Cohort. Twin Res 2002; 5: 358–365.
Cannon TD, Kaprio J, Lonnqvist J, Huttunen M, Koskenvuo M . The genetic epidemiology of schizophrenia in a Finnish twin cohort. A population-based modeling study. Arch Gen Psychiatry 1998; 55: 67–74.
Spitzer RL, Williams JBW, Gibbon M, First MB . Instruction Manual for the Structured Clinical Interview for DSM-III-R (SCID). Biometrics Research: New York, NY, 1989.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th edn, American Psychiatric Association: Washington, DC, 1994.
Loranger AW, Susman VL, Oldham JM, Russakoff LM . Personality Disorder Examination: A Structured Interview for Making Diagnosis of DSM-III-R Personality Disorders. Cornell Medical College: White Plains, NY, 1985.
Cavassila S, Deval S, Huegen C, van Ormondt D, Graveron-Demilly D . Cramer-Rao bounds: an evaluation tool for quantitation. NMR Biomed 2001; 14: 278–283.
Purdon SE, Valiakalayil A, Hanstock CC, Seres P, Tibbo P . Elevated 3 T proton MRS glutamate levels associated with poor Continuous Performance Test (CPT-0X) scores and genetic risk for schizophrenia. Schizophrenia Res 2008; 99: 218–224.
Chang L, Friedman J, Ernst T, Zhong K, Tsopelas ND, Davis K . Brain metabolite abnormalities in the white matter of elderly schizophrenic subjects: implication for glial dysfunction. Biol Psychiatry 2007; 62: 1396–1404.
Wood SJ, Yücel M, Wellard RM, Harrison BJ, Clarke K, Fornito A et al. Evidence for neuronal dysfunction in the anterior cingulate of patients with schizophrenia: a proton magnetic resonance spectroscopy study at 3 T. Schizophrenia Res 2007; 94: 328–331.
Mangia S, Tkác I, Gruetter R, Van De Moortele P-F, Giove F, Maraviglia B et al. Sensitivity of single-voxel 1H-MRS in investigating the metabolism of the activated human visual cortex at 7T. Magn Reson Imaging 2006; 24: 343–348.
Venkatraman TN, Hamer RM, Perkins DO, Song AW, Lieberman JA, Steen RG . Single-voxel 1H PRESS at 4.0 T: precision and variability of measurements in anterior cingulate and hippocampus. NMR Biomed 2006; 19: 484–491.
Oz G, Terpstra M, Tkác I, Aia P, Lowary J, Tuite PJ et al. Proton MRS of the unilateral substantia nigra in the human brain at 4 tesla: detection of high GABA concentrations. Magn Reson Med 2006; 55: 296–301.
Posse S, Otazo R, Caprihan A, Bustillo J, Chen H, Henry PG et al. Proton echo-planar spectroscopic imaging of J-coupled resonances in human brain at 3 and 4 Tesla. Magn Reson Med 2007; 58: 236–244.
Provencher SW . Estimation of metabolite concentrations from localized in vivo proton NMR spectra. Magn Reson Med 1993; 30: 672–679.
Zhang Y, Brady M, Smith S . Segmentation of brain MR images through a hidden Markov random field model and the expectation-maximization algorithm. IEEE Trans Med Imaging 2001; 20: 45–57.
Smith SM, Jenkinson M, Woolrich MW, Beckmann CF, Behrens TE, Johansen-Berg H et al. Advances in functional and structural MR image analysis and implementation as FSL. Neuroimage 2004; 23 (Suppl 1): S208–S219.
Schuff N, Amend D, Ezekiel F, Steinman SK, Tanabe J, Norman D et al. Changes of hippocampal N-acetylaspartate and volume in Alzheimer's disease. A proton MR spectroscopic imaging and MRI study. Neurology 1997; 49: 1513–1521.
Lynch J, Peeling J, Auty A, Sutherland GR . Nuclear magnetic resonance study of cerebrospinal fluid from patients with multiple sclerosis. Can J Neurol Sci 1993; 20: 194–198.
McLean MA, Woermann FG, Barker GJ, Duncan JS . Quantitative analysis of short echo time 1H-MRSI of cerebral gray and white matter. Magn Reson Med 2000; 44: 401–411.
Kalra S, Arnold DL . Magnetic resonance spectroscopy for monitoring neuronal integrity in amyotrophic lateral sclerosis. Adv Exp Med Biol 2006; 576: 275–282; discussion 361–273.
Olbrich HM, Valerius G, Rüsch N, Buchert M, Thiel T, Hennig J et al. Frontolimbic glutamate alterations in first episode schizophrenia: evidence from a magnetic resonance spectroscopy study. World J Biol Psychiatry 2008; 9: 59–63.
van Elst LT, Valerius G, Büchert M, Thiel T, Rüsch N, Bubl E et al. Increased prefrontal and hippocampal glutamate concentration in schizophrenia: evidence from a magnetic resonance spectroscopy study. Biol Psychiatry 2005; 58: 724–730.
Rowland LM, Bustillo JR, Mullins PG, Jung RE, Lenroot R, Landgraf E et al. Effects of ketamine on anterior cingulate glutamate metabolism in healthy humans: a 4-T proton MRS study. Am J Psychiatry 2005; 162: 394–396.
Carlsson A, Waters N, Carlsson ML . Neurotransmitter interactions in schizophrenia—therapeutic implications. Biol Psychiatry 1999; 46: 1388–1395.
Goff DC, Coyle JT . The emerging role of glutamate in the pathophysiology and treatment of schizophrenia. Am J Psychiatry 2001; 158: 1367–1377.
Javitt DC, Zukin SR . Recent advances in the phencyclidine model of schizophrenia. Am J Psychiatry 1991; 148: 1301–1308.
Tamminga CA, Holcomb HH, Gao XM, Lahti AC . Glutamate pharmacology and the treatment of schizophrenia: current status and future directions. Int Clin Psychopharmacol 1995; 10 (Suppl 3): 29–37.
Barker PB, Bonekamp D, Riedy G, Smith M . Quantitation of NAA in the brain by magnetic resonance spectroscopy. Adv Exp Med Biol 2006; 576: 183–197; discussion 361–183.
Soher BJ, van Zijl PC, Duyn JH, Barker PB . Quantitative proton MR spectroscopic imaging of the human brain. Magn Reson Med 1996; 35: 356–363.
Hetherington HP, Mason GF, Pan JW, Ponder SL, Vaughan JT, Twieg DB et al. Evaluation of cerebral gray and white matter metabolite differences by spectroscopic imaging at 4.1 T. Magn Reson Med 1994; 32: 565–571.
Stockler S, Holzbach U, Hanefeld F, Marquardt I, Helms G, Requart M et al. Creatine deficiency in the brain: a new, treatable inborn error of metabolism. Pediatr Res 1994; 36: 409–413.
Buckley PF, Moore C, Long H, Larkin C, Thompson P, Mulvany F et al. 1H-magnetic resonance spectroscopy of the left temporal and frontal lobes in schizophrenia: clinical, neurodevelopmental, and cognitive correlates. Biol Psychiatry 1994; 36: 792–800.
Bustillo JR, Lauriello J, Rowland LM, Jung RE, Petropoulos H, Hart BL et al. Effects of chronic haloperidol and clozapine treatments on frontal and caudate neurochemistry in schizophrenia. Psychiatry Res 2001; 107: 135–149.
Ohrmann P, Siegmund A, Suslow T, Pedersen A, Spitzberg K, Kersting A et al. Cognitive impairment and in vivo metabolites in first-episode neuroleptic-naive and chronic medicated schizophrenic patients: a proton magnetic resonance spectroscopy study. J Psychiatr Res 2006; Aug: 30.
Deicken RF, Zhou L, Corwin F, Vinogradov S, Weiner MW . Decreased left frontal lobe N-acetylaspartate in schizophrenia. Am J Psychiatry 1997; 154: 688–690.
Wood SJ, Berger G, Velakoulis D, Phillips LJ, McGorry PD, Yung AR et al. Proton magnetic resonance spectroscopy in first episode psychosis and ultra high-risk individuals. Schizophr Bull 2003; 29: 831–843.
Kim H, McGrath BM, Silverstone PH . A review of the possible relevance of inositol and the phosphatidylinositol second messenger system (PI-cycle) to psychiatric disorders—focus on magnetic resonance spectroscopy (MRS) studies. Hum Psychopharmacol 2005; 20: 309–326.
Delamillieure P, Constans JM, Fernandez J, Brazo P, Benali K, Courtheoux P et al. Proton magnetic resonance spectroscopy (1H MRS) in schizophrenia: investigation of the right and left hippocampus, thalamus, and prefrontal cortex. Schizophr Bull 2002; 28: 329–339.
Delamillieure P, Constans J, Fernandez J, Brazo P, Dollfus S . Proton magnetic resonance spectroscopy (1H-MRS) of the thalamus in schizophrenia. Eur Psychiatry 2000; 15: 489–491.
Harris RE, Sundgren PC, Pang Y, Hsu M, Petrou M, Kim SH et al. Dynamic levels of glutamate within the insula are associated with improvements in multiple pain domains in fibromyalgia. Arthritis Rheum 2008; 58: 903–907.
Shibuya-Tayoshi S, Tayoshi S, Sumitani S, Ueno S, Harada M, Ohmori T . Lithium effects on brain glutamatergic and GABAergic systems of healthy volunteers as measured by proton magnetic resonance spectroscopy. Prog Neuropsychopharmacol Biol Psychiatry 2008; 32: 249–256.
Shulman Y, Grant S, Seres P, Hanstock C, Baker G, Tibbo P . The relation between peripheral and central glutamate and glutamine in healthy male volunteers. J Psychiatry Neuroscience 2006; 31: 406–410.
Gallinat J, Kunz D, Lang UE, Neu P, Kassim N, Kienast T et al. Association between cerebral glutamate and human behaviour: the sensation seeking personality trait. Neuroimage 2007; 34: 671–678.
Schubert F, Gallinat J, Seifert F, Rinneberg H . Glutamate concentrations in human brain using single voxel proton magnetic resonance spectroscopy at 3 Tesla. Neuroimage 2004; 21: 1762–1771.
Acknowledgements
This work was supported by a research grant from the National Institute of Mental Health (to TDC). From the Department of Mental Health and Alcohol Research, National Public Health Institute, Helsinki, Finland, we thank Ulla Mustonen, Tiia Pirkola, Pirjo Käki, Eila Voipio and Annamari Tuulio-Henriksson for their contributions to subject recruitment and assessment; Antti Tanksanen for his contributions to the register searches; Kauko Heikkilä for his contributions to data management of the Finnish Twin Cohort Study and Sami Heikkinen for his work in setting up the protocol. We also thank Dr Provencher for providing the LCModel basis set. Finally, we thank the subjects, whose participation made this project possible.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lutkenhoff, E., van Erp, T., Thomas, M. et al. Proton MRS in twin pairs discordant for schizophrenia. Mol Psychiatry 15, 308–318 (2010). https://doi.org/10.1038/mp.2008.87
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/mp.2008.87
Keywords
This article is cited by
-
Role of cryptic rearrangements of human chromosomes in the aetiology of schizophrenia
Journal of Genetics (2023)
-
Glutamatergic and GABAergic metabolite levels in schizophrenia-spectrum disorders: a meta-analysis of 1H-magnetic resonance spectroscopy studies
Molecular Psychiatry (2022)
-
Increased PLA2 activity in individuals at ultra-high risk for psychosis
European Archives of Psychiatry and Clinical Neuroscience (2021)
-
In vivo glucose metabolism and glutamate levels in mGluR5 knockout mice: a multimodal neuroimaging study using [18F]FDG microPET and MRS
EJNMMI Research (2020)
-
Plasma amino acids profile in first-episode psychosis, unaffected siblings and community-based controls
Scientific Reports (2020)