Abstract
The fms-related tyrosine kinase 3 (FLT3) receptor has been extensively studied over the past two decades with regard to oncogenic alterations that do not only serve as prognostic markers but also as therapeutic targets in acute myeloid leukemia (AML). Internal tandem duplications (ITDs) became of special interest in this setting as they are associated with unfavorable prognosis. Because of sequence-dependent protein conformational changes FLT3-ITD tends to autophosphorylate and displays a constitutive intracellular localization. Here, we analyzed the effect of tyrosine kinase inhibitors (TKIs) on the localization of the FLT3 receptor and its mutants. TKI treatment increased the surface expression through upregulation of FLT3 and glycosylation of FLT3-ITD and FLT3-D835Y mutants. In T cell-mediated cytotoxicity (TCMC) assays, using a bispecific FLT3 × CD3 antibody construct, the combination with TKI treatment increased TCMC in the FLT3-ITD-positive AML cell lines MOLM-13 and MV4-11, patient-derived xenograft cells and primary patient samples. Our findings provide the basis for rational combination of TKI and FLT3-directed immunotherapy with potential benefit for FLT3-ITD-positive AML patients.
Similar content being viewed by others
Introduction
In acute myeloid leukemia (AML), approximately one-third of patients carry an activating mutation in the fms-related tyrosine kinase 3 (FLT3) gene, prevalently an internal tandem duplication (ITD) of varying length (affecting 20–30% of adult AML).1, 2 FLT3-ITD is associated with an unfavorable prognosis, characterized by shorter event-free survival (EFS) and overall survival (OS) as well as a high relapse rate.2, 3, 4, 5, 6 On a cellular level, the mutant FLT3 receptor promotes cell proliferation of hematopoietic stem and myeloid progenitor cells.2, 3, 6 FLT3-ITD mutations lead to sequence-dependent protein conformational changes in the receptor and, thus, to an endoplasmatic reticulum-retained intracellular localization, constitutive autophosphorylation and induction of growth factor signaling pathways.7, 8, 9, 10, 11 Therefore, FLT3-targeting therapies are highly warranted to impede disease progression, alternatively or in addition to convential chemotherapy. Promising agents are second-generation tyrosine kinase inhibitors (TKIs), including AC220 (quizartinib), PKC412 (midostaurin) and BAY43-9006 (sorafenib, nexavar), that block FLT3 phosphorylation.12, 13, 14, 15, 16, 17 Although complete remission rates reach a moderate level, clinical response to TKI monotherapy remains limited by the high risk of relapse that often occures within months.18, 19, 20, 21 However, the SORAML trial (NCT00893373) demonstrated sorafenib to be a benificial antileukemic additive to conventional chemotherapy with regard to increased EFS and relapse-free survival for patients aged ⩽60 years, regardless of FLT3 status.22 Furthermore, the CALGB 10603/RATIFY trial (NCT00651261) demonstrated significantly improved EFS and OS for patients, harboring a FLT3 mutation, when treated with PKC412 in addition to induction chemotherapy and 1 year of maintenance therapy.23 Nevertheless, TKIs still lack the efficiency to eradicate all FLT3-mutated AML cells because of resistance mechanisms. In FLT3-ITD-positive AML, resistance is frequently mediated by specific insertion sites of ITDs (including β1- or β2-sheet), emerging secondary FLT3 point mutations (PMs; such as D835Y, N676K), protection by the stromal microenvironment and/or altered pathway signaling.24, 25, 26, 27, 28, 29, 30, 31 The subcellular localization of FLT3 matters for activation of signaling cascades. For example, FLT3-N676K displays a mere wild-type (WT)-like membrane localization and activates mitogen-activated protein kinase signaling, whereas FLT3-D835Y localizes to the ER and activates the signal transducer and activator of transcription 5 pathway.10, 32 However, the effect of TKIs on the subcellular localization of FLT3 and its mutants has not yet been examined systematically. Therefore, we investigated the localization of FLT3 mutants under TKI treatment and observed an increase of FLT3 on the cell surface that facilitated the application of FLT3-directed immunotherapy.
Materials and methods
Cell lines and reagents
All cell lines were purchased from the German Collection of Microorganisms and Cell Culture (DSMZ, Braunschweig, Germany), except for U2OS cells that were obtained from ATCC (American Type Culture Collection, Wesel, Germany) and Phoenix eco, which were purchased from Orbigen (San Diego, CA, USA). The B-cell lymphoma cell line OCI-Ly8 was a kind gift from O Weigert (Department of Internal Medicine III, University Hospital of the LMU Munich, Munich, Germany).33, 34 All cell lines were cultivated according to supplier’s instructions or as described elsewhere.35 Stably transduced Ba/F3 cell lines were generated as described previously.36, 37 Recombinant human FLT3 ligand (FL) was obtained from Promokine (Heidelberg, Germany), recombinant murine interleukin-3 from Immunotools (Friesoythe, Germany), cycloheximide and 2-deoxy-D-glucose from Sigma-Aldrich (Taufkirchen, Germany). TKIs sorafenib (BAY43-9006, nexavar), midostaurin (PKC412) and quizartinib (AC220) were purchased from Selleck Chemicals (Houston TX, USA). Cell lines were tested for a mycoplasma contamination on a regular basis (MycoAlert Mycoplasma Detection Kit, Lonza Rockland Inc., Rockland, ME, USA).
Plasmid constructs and mutagenesis
The following DNA constructs and vectors have been described before:32, 37, 38 the expression vectors pcDNA6.2-V5-HisA, pcDNA6.2-V5-HisA-FLT3-WT, pcDNA6.2-V5-HisA-FLT3-K602R(7) (described as W51) and pcDNA6.2-V5-HisA-FLT3-E611C(28) (described as NPOS); the retroviral expression vectors pMSCV-IRES-EYFP, pMSCV-IRES-EYFP-FLT3-WT, pMSCV-IRES-EYFP-FLT3-N676K, pMSCV-IRES-EYFP-FLT3-D835Y and pMSCV-IRES-EYFP-FLT3-E611C(28) (described as NPOS). The constructs pMSCV-IRES-puro-EYFP-FLT3-WT, pMSCV-IRES-puro-EYFP-FLT3-E611V(32), pMSCV-IRES-puro-EYFP-FLT3-G613E(33), pMSCV-IRES-puro-EGFP-FLT3-598/599(12), pMSCV-IRES-puro-EGFP-FLT3-598/599(22), pMSCV-IRES-puro-EGFP-FLT3-L601H(10) and pMSCV-IRES-puro-EGFP-FLT3-K602R(7) have been previously described39 and kindly provided by FH Heidel (Center of Internal Medicine, Otto-von-Guericke University Magdeburg, Magdeburg, Germany). Denotation of all FLT3-ITDs was adapted from a recent publication.39 The mutations N676K and D835Y were introduced into pcDNA6.2-V5-HisA-FLT3-WT and pMSCV-IRES-EYFP-FLT3-E611C(28), using the QuikChange II XL Site-Directed Mutagenesis Kit (Agilent, Santa Clara, CA, USA) according to the supplier’s instructions as previously described.32 Mutations were confirmed by Sanger sequencing.
Proliferation assay
Proliferation assays were performed as described before, utilizing the Vi-Cell XR (Beckman Coulter, Munich, Germany).36 AML cell lines were seeded at a density of 3 × 105/ml. Experiments were performed in biological triplicates.
Immunofluorescence staining
Transient transfection of U2OS cells and subsequent immunofluorescence staining was performed as previously described40 using the following antibodies: anti-wheat germ agglutinin-488 fluorescein conjugate (catalog number: W11261; Invitrogen–ThermoFisher Scientific, Munich, Germany), rabbit anti-FLT3 (catalog number: sc-480, clone: S-18; Santa Cruz Biotechnology, Heidelberg, Germany) and anti-rabbit IgG (H+L) F(ab’)2 fragment Alexa Fluor 594 Conjugate (catalog number: 8889S; Cell Signaling Technology, Leiden, The Netherlands). Fixation was performed for 10 min at room temperature with Dulbecco’s phosphate-buffered saline (DPBS) 2% formaldehyde (37% stock solution; Merck Schuchardt, Hohenbrunn, Germany), followed by permeabilization for 10 min with DPBS 0.5% Triton X-100 (Carl Roth, Karlsruhe, Germany). Before staining, cells were treated with 50 nM AC220 for 6 h, whereas controls were left untreated. For suspension cells, 8-well chamber slides (ibidi, Munich, Germany) were precoated with poly-L-lysine hydrobromide (Sigma-Aldrich) according to the supplier’s recommendations. Before seeding, cells were treated with 50 nM AC220, whereas controls were left untreated, washed twice with DPBS and dissolved in H2F buffer (1 × Hanks’ balanced salt solution (w/o calcium, magnesium and phenol red, ThermoFisher Scientific), 2% fetal bovine serum (Biochrom, Berlin, Germany), 1% 1 M Hepes (Sigma-Aldrich) and 1% penicillin/streptomycin (PAN Biotech, Aidenbach, Germany). After 30 min of detachment at 4 °C, glycoconjugates were stained as described previously,40 followed by cell fixation using DPBS 4% formaldehyde for 5 min. For blocking, DPBS with 0.1% Tween 20 (Carl Roth) and 10% fetal bovine serum (Biochrom) was used. Subsequent steps of the staining procedure were performed as for U2OS cells.
T cell-mediated cytotoxicity (TCMC) assay
The in vitro cytotoxicity assays against AML cells were performed as described previously.35, 41 The bispecific FLT3 × CD3 antibody construct (4G8 × UCHT1, Fabsc-format) was utilized as reported elsewhere.42 Confirmatory antibody serial dilution experiments with an effector-to-target ratio of 1:2.5 were performed using CD3-positive isolated T cells from healthy donors. For TCMC assays, AML cells and T cells were co-cultured with an effector-to-target ratio between 1:2.5 and 1:4. Then 50 nM AC220 and 1–10 μg/ml FLT3 × CD3 antibody were added at the beginning of each experiment, whereas controls were left untreated. After 72 h, cell counting and flow cytometry analysis was performed, determining the percentage of cytotoxicity as described previously.35, 41 FLT3 (CD135) surface expression was assessed simultaneously. Estimation of a potential additive effect of combined treatment was computed based on the fractional product method.43 Competitive lysis experiments were performed as described previously,35 using 1–5 μg/ml FLT3 × CD3 antibody. Untreated AML cells (HL60 or MV4-11) were mixed 1:1 with corresponding 6 h AC220-pre-treated AML cells (HL60 or MV4-11) and cultured with healthy donor T cells at an effector-to-target ratio of 1:1 for 20–24 h. Cell membrane staining of untreated AML cells (HL60 and MV4-11) was performed using the PKH26 red fluorescent cell linker kit (Sigma-Aldrich) according to the manufacturer’s protocol. Experiments were performed once, if not stated otherwise.
Additional materials and methods are provided in the Supplementary Information.
Results
TKIs increase the membrane localization of FLT3-V592A, FLT3-D835Y and FLT3-ITD mutants
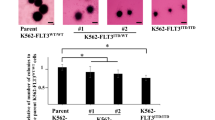
Cellular localization studies of seven ITD constructs with varying length and position, as well as two activating PMs of FLT3 (Figure 1a), revealed an altered localization of FLT3 mutants D835Y and ITDs upon TKI treatment. FLT3-ITD or FLT3-D835Y protein was retained in the perinuclear ER and after addition of AC220 a cell membrane localization similar to FLT3-WT or FLT3-N676K was observed (Figures 1b and 2a). Flow cytometry confirmed that FLT3 (CD135) surface expression differed significantly between treated and untreated FLT3-expressing Ba/F3 cells (Figure 2b and Supplementary Figure S1a) not only for ITD and D835Y but also for WT and N676K. However, the increase in surface FLT3 was significantly higher in FLT3-D835Y or FLT3-ITD compared with FLT3-WT-expressing cells (Student’s t-test: P=0.003 and P<0.001, respectively). In light of the recently reported in vitro and in vivo experiments, displaying juxtamembrane domain (JMD)-ITD to be more sensitive towards TKI-therapy than tyrosine kinase domain 1 (TKD1)-ITD,39 we evaluated four JMD-ITD and three TKD1-ITD constructs with regard to TKI-induced FLT3 surface expression and did not observe any significant differences (Figure 2b). In AML cell lines, FLT3 surface expression levels were hardly altered in cells with FLT3-WT status (THP-1, OCI-AML3) or a heterozygous FLT3-ITD (MOLM-13, PL-21), whereas the cell lines MV4-11 with FLT3-loss of heterozygosity (LOH) and MONO-MAC-6 (MM6) with an activating PM FLT3-V592A44 responded with a significant increase in FLT3 surface expression upon AC220 treatment (Table 1 and Figures 3a and b). The TKI response of MV4-11 was also obvious in immunofluorescence staining (Supplementary Figure S1b). Additional FLT3-WT AML cell lines (HL60, Kasumi-1, EOL-1, NOMO-1, MUTZ-2) confirmed this observation, except for MUTZ-2 (Student’s t-test: P<0.001; Supplementary Figures S1c and d). In the AML cell line KG-1a, the CML cell line K-562 and the B-cell lymphoma cell line OCI-Ly8, we did not detect any FLT3 surface expression, regardless of TKI treatment. In a time-course experiment over 24 h with TKI-treatment, MV4-11 cells showed a steady increase in FLT3 surface expression, whereas untreated cells remained stable in FLT3 surface expression (Supplementary Figure S2a). MOLM-13 cells started to diverge from untreated cells after 12 h of TKI treatment. Other TKIs (PKC412 and sorafenib) induced a similar response in MV4-11 cells, however, with AC220 the effect was strongest, when applying equal concentrations (Supplementary Figures S2b and c). A dose escalation experiment, applying concentrations up to 100 nM of AC220, sorafenib or PKC412, revealed that AC220 was most efficient in inducing FLT3 surface expression at concentrations from 5 to 25 nM (Supplementary Figure S2d).
FLT3 mutants and their subcellular localization with and without TKI treatment. (a) Schematic illustration of the FLT3 protein (NP_004110.2) and mutant constructs with indication of amino acid substitutions and insertion sequences (modified from Arreba-Tutusaus et al.39). (b) Immunofluorescence staining of FLT3-WT, FLT3 mutants or empty vector with or without AC220 treatment in transiently transfected U2OS cells. WGA (wheat germ agglutinin). Scale bar: 25 μm.
TKI treatment response of FLT3-expressing Ba/F3 cells. (a) Immunofluorescence staining of stably transduced Ba/F3 cells expressing FLT3-WT, FLT3-ITD or empty vector with or without AC220 treatment. WGA (wheat germ agglutinin). Scale bar: 10 μm. (b) FLT3 surface expression levels with or without AC220 treatment (mean±s.d.). (c) Viable cell counts of Ba/F3 cells expressing the indicated FLT3 mutants, normalized to the empty vector transduced control cells, after 72 h of treatment with increasing concentrations of AC220 (n=3, mean±s.d.).
TKI treatment response of AML cells. (a) Representative flow cytometry plots and (b) bar graph showing the FLT3 surface expression in AML cells, harboring different FLT3 genotypes, with or without AC220 treatment (mean±s.d.). A mean fluorescence intensity (MFI) ratio increase of ⩾0.50 is highlighted by an arrow. (c) Viable cell counts of selected AML cells, normalized to untreated control, after 72 h of treatment with increasing concentrations of AC220 (n=3, mean±s.d.).
TKI-induced increase in FLT3 surface expression in FLT3-mutated cells correlates inversely with proliferation
Treatment of Ba/F3 cells, expressing various FLT3-ITD constructs, with AC220 at nontoxic concentrations (⩽500 nM) revealed a variable inhibition of proliferation without any obvious correlation to ITD length or position (Figure 2c and Supplementary Table S1). However, the AC220-mediated reduction in proliferation of FLT3-ITD-positive cells correlated with the increase in surface FLT3 (Pearson: −0.931, P=0.002, n=7). Moreover, we confirmed that the TKI resistance-mediating PMs32, 45 reduced the TKI response with regard to FLT3 surface expression when combined with ITD (Supplementary Figures S3a–c and Supplementary Table S1). The FLT3-LOH cell line MV4-11, which showed the highest increase in FLT3 surface location upon TKI treatment, was more sensitive to AC220, compared with the heterozygous FLT3-ITD cell lines MOLM-13 and PL-21 (Figure 3c). Of note, PL-21 cells did not respond to AC220 treatment during the proliferation assay, although carrying a heterozygous FLT3-ITD and showing a slight increase in FLT3 surface expression. Targeted multiplexed amplicon sequencing revealed that the cell line PL-21 harbored a KRAS mutation (c.437C>T:p.A146V, NM_033360), constituting a potential mechanism of TKI resistance. The AML cell line MM6 with a FLT3-V592A PM displayed a prominent increase in FLT3 surface expression after AC220 treatment and responded with a moderate decrease in proliferation (Figure 3c and Supplementary Table S2). The FLT3-WT cell lines THP-1 and OCI-AML3 were resistant to AC220 treatment. When comparing the antiproliferative potential of various TKIs (PKC412, sorafenib, AC220) in the FLT3-LOH cell line MV4-11, AC220 was the most potent agent at low nanomolar levels (Supplementary Figure S2e and Supplementary Table S2). Of note, several other FLT3-WT cell lines (HL60, MUTZ-2, NOMO-1) and FLT3-expression-negative cell lines (KG-1a, K-562) also showed TKI resistance. In contrast, the FLT3-WT cell lines Kasumi-1 and EOL-1, which carry alterations of other receptor tyrosine genes (KIT c.2466T>A:pN822K, NM_000222 in Kasumi-1 and FIP1L1-PDGFRA rearrangement; del(4)(q12q12) in EOL-1), both responded, consistent with the known target profile of the tested TKIs12, 30 (Supplementary Table S2).
Induction of FLT3 surface expression depends on the pretreatment FLT3-ITD mRNA levels
The AC220-induced FLT3 increase on the cell surface (CD135 mean fluorescence intensity ratio change, Supplementary Table S2) tended to correlate with the pretreatment FLT3-ITD mRNA levels (Supplementary Figure S4a) in tested AML cell lines (Pearson: 0.864, P=0.059, n=5). Patient-derived xenograft (PDX) cells with either FLT3-WT, heterozygous FLT3-ITD mutation or FLT3-LOH status (Table 1) revealed a stable FLT3 surface expression in FLT3-WT PDX cells (AML-372, AML-491), whereas the heterozygous FLT3-ITD PDX cells (AML-573, AML-640) showed a minimal response to AC220 treatment (Figures 4a and b). However, both PDX cells with FLT3-LOH (AML-415, AML-579) showed a significant FLT3 surface expression increase upon AC220 treatment (Student’s t-test: both P<0.001). Thus, a difference between FLT3-WT and FLT3-ITD samples was observed (Student’s t-test: P<0.001). In addition, there was a positive correlation of the FLT3 expression increase at the cell surface upon AC220 treatment with the pretreatment FLT3-ITD mRNA level (Spearman: 0.971, P=0.001, n=6; in case of AML-640, the pretreatment FLT3-ITD mRNA level of the dominant clone was used for statistics). The correlation remained significant when combining the data generated from AML cell lines and PDX cells (Figure 4c; Spearman: 0.840, P=0.001, n=11). Characteristics of PDX cells have been recently published46 and are summarized in Supplementary Table S3. The pretreatment FLT3-ITD mRNA levels of the PDX cells are shown in Supplementary Figure S4b.
TKI treatment response of PDX cells and correlation with FLT3-ITD mRNA level. (a) Representative flow cytometry plots and (b) bar graph showing the FLT3 surface expression in PDX cells, with and without AC220 treatment (mean±s.d.). A mean fluorescence intensity (MFI) ratio increase of ⩾0.50 is highlighted by an arrow. (c) Scatter plot showing the correlation of the pretreatment FLT3-ITD mRNA level and the AC220 treatment-induced MFI ratio change representing the increase in FLT3 surface expression.
FLT3 surface expression is glycosylation dependent
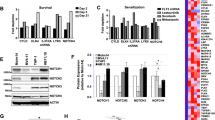
Western blot analysis showed an increase of the fully glycosylated mature (160 kDa) form of all FLT3 constructs expressed in Ba/F3 cells after 6 h of TKI treatment (Figure 5a). This effect was also obvious in the FLT3-LOH AML cell line MV4-11 and apparent in the AML cell line MM6 that carries a FLT3-V592A PM. In contrast, FLT3-WT and FLT3-expression-negative cell lines (KG-1a, K-562, OCI-Ly8) remained mostly unaffected (Figure 5b and Supplementary Figures S5a and b). The increase of mature FLT3 after TKI treatment was smaller or absent, when combining ITD with a resistance-mediating PM (Supplementary Figure S5c). Thus, the altered glycosylation pattern of FLT3, represented by relative changes of the two differentially glycosylated forms, was consistent with the increase in surface FLT3 upon TKI treatment. Consistently, the FLT3-WT PDX cells did not show any obvious difference in glycosylation pattern after AC220 treatment, in contrast to PDX cells harboring a FLT3-ITD, especially those with FLT3-LOH (Figure 5c). Treatment of MV4-11 cells with 2-deoxy-D-glucose, a compound inhibiting N-linked glycosylation,47 alone or in combination with AC220, demonstrated that TKI not only affects phosphorylation but also N-linked glycosylation (Figure 5d). After a 24 h TKI treatment period, the glycosylated form of FLT3 was increased 1.5- and four-fold for the FLT3-ITD-positive cell lines MOLM-13 and MV4-11, whereas the immature form decreased to 0.8-fold (Supplementary Figures S5d and e). Moreover, the TKI-treated MV4-11 cells showed an increase in total amount of FLT3 protein levels likely because of upregulation of FLT3 mRNA expression (Supplementary Figure S5f). Whereas in MOLM-13 cells the overall FLT3 mRNA level was not altered by AC220 treatment, the ratio of FLT3-WT to FLT3-ITD changed significantly (Student’s t-test: P<0.001) pointing toward allelic expression in favour of the WT allele (Supplementary Figures S5g and h). In addition, cycloheximide treatment indicated that TKI-mediated differential expression of mature and immature FLT3 depends on biosynthesis. Furthermore, we confirmed that PKC412 and sorafenib also have the potential to increase the glycosylation of FLT3 in MV4-11 cells (Supplementary Figure S5i).
TKI increases the glycosylation of FLT3-ITD. Western blot analysis of FLT3 or phospho-FLT3 (130 and 160 kDa) and α-tubulin (50 kDa) in whole-cell lysates with or without AC220 and/or 2-DG (2-deoxy-D-glucose) of (a) Ba/F3 cells transduced with empty vector, FLT3-WT or indicated FLT3 mutant construct, (b) AML cell lines, (c) PDX cells and (d) MV4-11 cells.
FLT3 upregulation by TKI in vivo
In vivo, cells of two AML patients with mutated FLT3 who received sorafenib treatment (TKI-PT#1 and TKI-PT#2), after conventional therapy had failed, showed a prominent increase in FLT3 surface expression when comparing FLT3 expression at diagnosis of relapse and after sorafenib treatment (Figure 6a). Sorafenib treatment schemes are shown in Figure 6b and corresponding patient characteristics are detailed in Supplementary Table S5 and Supplementary Figure S6. For TKI-PT#1, sorafenib maintenance monotherapy resulted in a reduction of leukemia burden (blast count: 40% at diagnosis of relapse and 15% after 21 days of treatment), whereas in TKI-PT#2, leukemic burden showed a persistent increase over time (blast count: 48% at diagnosis of relapse and 90% after 53 days of treatment).
TKI effect on FLT3 surface expression in patients. (a) Flow cytometry plots showing the FLT3 surface expression before (day 0) and after (indicated day) TKI treatment. A mean fluorescence intensity (MFI) ratio increase of ⩾0.50 is highlighted by an arrow. (b) Sorafenib treatment scheme with indication of the time point of relapse (R), sampling of bone marrow (BM) and peripheral blood (PB) for the assessment of treatment response. Arrows indicate dosage adjustments.
AC220 treatment boosts FLT3 × CD3 antibody-mediated cytotoxicity against FLT3-ITD-positive AML cells
Besides TKIs, an alternative strategy to target FLT3 is immunotherapy using a FLT3-directed antibody construct.42, 48 However, FLT3-directed immunotherapy might be limited by insufficient antigen expression levels. In light of our findings, we hypothesized that TKIs will increase anti-FLT3-directed antibody-mediated cytotoxicity through upregulation of the FLT3 target antigen (Figure 7a). Therefore, we performed T-cell-mediated cytotoxicity (TCMC) assays using a bispecific FLT3 × CD3 antibody construct42 in combination with AC220. FLT3-expression-specific cell lysis by the FLT3 × CD3 antibody was demonstrated by an antibody serial dilution (Supplementary Figure S7a). Assessment of expression kinetics of FLT3-ITD-positive AML cells over 72 h showed a steady increase of FLT3 surface expression in MV4-11 cells upon addition of AC220, whereas MOLM-13 cells showed a maximum at 24 h (Supplementary Figure S7b). The FLT3 surface expression level in the FLT3-WT AML HL60 cells was not significantly changed by addition of AC220. In TCMC experiments, the combination of TKI and FLT3 × CD3 in HL60 cells showed no significant change in cytotoxicity (Figure 7b and Supplementary Table S4). In contrast, FLT3-ITD-positive MV4-11 cells were almost completely eradicated by combined treatment with a mean CD33+ cell count lower than the computed additive effect (Figure 7b and Supplementary Table S4), pointing toward a synergism of TKI and FLT3-directed immunotherapy. The difference between single-agent and combined treatment was significant (Student’s t-test: P<0.001 AC220 only and P=0.028 FLT3 × CD3 only). For the heterozygous FLT3-ITD cell line MOLM-13, the FLT3 × CD3 antibody treatment alone was very efficient in eradicating nearly all CD33+ cells (Figure 7b and Supplementary Table S4), and therefore no conclusion about synergistic or additive effects could be drawn regarding the increased lysis by combined treatment. Representative flow cytometry plots of the TCMC assays are shown in Supplementary Figure S7c. Competitive lysis experiments of untreated and AC220-pretreated AML cells confirmed a preferential killing of AC220-pretreated MV4-11 cells with higher FLT3 surface expression levels (Supplementary Figure S7d). For PDX cells a considerable increase in cytotoxicity was observed when applying the combined treatment, especially in PDX cells with FLT3-LOH (AML-415, AML-579; Figure 7c). For the heterozygous FLT3-ITD PDX cells AML-573 the single FLT3 × CD3 antibody treatment already resulted in almost complete eradication of CD33+ cells, similar to the heterozygous FLT3-ITD cell line MOLM-13 (Figures 7b and c). Moreover, two primary AML samples (PT#1, PT#2) showed a decrease in CD33+ cells by combined treatment below the computed additive effect (Figure 7c and Supplementary Table S4). Patient characteristics are shown in Supplementary Table S5; corresponding fragment analyses representing the pretreatment FLT3-ITD mRNA level of the primary samples are depicted in Supplementary Figure S6. Representative flow cytometry plots of the TCMC assays are shown in Supplementary Figure S7e.
TKI- and FLT3-directed antibody combination mediates cytotoxicity against AML cells. (a) Mechanistic mode of action when combining TKI treatment with FLT3-directed immunotherapy. Response to FLT3 × CD3 or AC220 alone or in combination with regard to FLT3 surface expression (representative flow cytometry plots) and specific T cell-mediated lysis of (b) AML cell lines (effector-to-target (E/T) 1:2.5–4, FLT3 × CD3 10 μg/ml) (mean±s.d.), (c) PDX cells and primary AML cells (E/T 1:3, FLT3 × CD3 1 μg/ml). The computed additive effect is shown as dotted line.
Discussion
FLT3-ITD is a common mutation in AML, associated with increased relapse rates and poor prognosis.4, 16 Novel treatment approaches are therefore highly warranted for patients who are not eligible for intensive treatment as well as for patients with failure of conventional therapy or allogeneic stem cell transplantation. Moreover, targeting FLT3 seems to be attractive for minimal residual disease eradication during consolidation or maintenance therapy to minimize relapse rates and to prolong EFS and OS. So far, TKI is a promising approach to target FLT3, for instance as a bridging therapy before stem cell transplantation and as treatment of medically unfit patients. However, clinical trials using TKI as a single agent indicate the need for combinatorial therapies in order to prevent resistance toward TKI and to achieve prolonged remission.18, 20, 21, 49, 50 The application of PKC412 in combination with induction chemotherapy in the CALGB 10603/RATIFY trial (NCT00651261) prolonged EFS and OS in FLT3-ITD- or FLT3-TKD-positive patients.23 In our study, we demonstrated that FLT3 surface expression could be significantly increased by TKI treatment, particularly in FLT3-ITD- and FLT3-D835Y-mutant cells. Of note, cells harboring FLT3-ITD in combination with a resistance mediating point mutation showed a reduced FLT3 surface increase upon TKI treatment consistent with TKI resistance.27, 29 In contrast to CEP701 (Lestaurtinib), which was reported to increase FLT3 surface expression in certain AML patients upon treatment51 irrespective of FLT3 genotype, we showed that AML cell lines and PDX cells responded to AC220 depending on the FLT3 genotype and pretreatment FLT3-ITD mRNA level. An exception was the AML cell line PL-21—although carrying a heterozygous ITD, the TKI was not effective in reducing proliferation, likely because of the presence of a KRAS mutation that is known to be associated with TKI resistance.52, 53 In line with previous reports,12 comparison of several TKIs confirmed that the second-generation TKI AC220 was more potent than multikinase inhibitors, such as PKC412 and sorafenib. In this context, FLT3-ITD-positive patients may benefit from the combination of TKI and therapeutic FLT3-directed antibodies. This strategy may not only overcome the limitation of FLT3 antigen availability in FLT3-ITD-positive AML cells but could also prevent adaptive TKI-resistance—a frequent problem in single-agent TKI-treatment. Although the overall impact of TKI on immune response remains controversial,54, 55, 56, 57 we provide evidence that the combination of TKI and FLT3 × CD3 antibodies enhance the T cell-mediated lysis of FLT3-ITD-positive AML cell lines, PDX cells and primary AML patient samples. Beyond increased FLT3 surface expression in FLT3-mutated cells as potential mechanism, TKI treatment may also modulate immune response through post-translational modifications as glycosylation matters in major histocompatibility complex peptide presentation and antigen recognition of T cells.58 This may be linked to the demonstrated increase in the mature, fully glycosylated form of FLT3 in FLT3-ITD-positive cells after TKI treatment, in accordance with other publications.47, 59, 60 This result suggests that autophosphorylation of the FLT3-ITD receptor may prevent physiological processing that is required for maturation and surface expression and possibly also for antigen processing and recognition. Of note, altered FLT3 mRNA expression also seems to contribute to the TKI-mediated increase in surface FLT3 that has been demonstrated in FLT3-TKI-resistant cells,21, 61 pointing toward a feedback response mechanism to compensate the lack of mature FLT3 receptor in the FLT3-mutated cellular setting.
Taken together, we do not only provide insights into the cellular effects of TKIs but also open up avenues to eradicate FLT3-mutated AML by combination of FLT3-targeting strategies. Further preclinical models and ultimately clinical trials are needed to translate our findings into novel therapeutic approaches.
References
Schnittger S, Schoch C, Dugas M, Kern W, Staib P, Wuchter C et al. Analysis of FLT3 length mutations in 1003 patients with acute myeloid leukemia: correlation to cytogenetics, FAB subtype, and prognosis in the AMLCG study and usefulness as a marker for the detection of minimal residual disease. Blood 2002; 100: 59–66.
Levis M, Small D . FLT3: ITDoes matter in leukemia. Leukemia 2003; 17: 1738–1752.
Mrozek K, Marcucci G, Paschka P, Whitman SP, Bloomfield CD . Clinical relevance of mutations and gene-expression changes in adult acute myeloid leukemia with normal cytogenetics: are we ready for a prognostically prioritized molecular classification? Blood 2007; 109: 431–448.
Santos FP, Jones D, Qiao W, Cortes JE, Ravandi F, Estey EE et al. Prognostic value of FLT3 mutations among different cytogenetic subgroups in acute myeloid leukemia. Cancer 2011; 117: 2145–2155.
Frohling S, Schlenk RF, Breitruck J, Benner A, Kreitmeier S, Tobis K et al. Prognostic significance of activating FLT3 mutations in younger adults (16 to 60 years) with acute myeloid leukemia and normal cytogenetics: a study of the AML Study Group Ulm. Blood 2002; 100: 4372–4380.
Steffen B, Muller-Tidow C, Schwable J, Berdel WE, Serve H . The molecular pathogenesis of acute myeloid leukemia. Crit Rev Oncol Hematol 2005; 56: 195–221.
Koch S, Jacobi A, Ryser M, Ehninger G, Thiede C . Abnormal localization and accumulation of FLT3-ITD, a mutant receptor tyrosine kinase involved in leukemogenesis. Cells Tissues Organs 2008; 188: 225–235.
Chan PM . Differential signaling of Flt3 activating mutations in acute myeloid leukemia: a working model. Protein Cell 2011; 2: 108–115.
Choudhary C, Olsen JV, Brandts C, Cox J, Reddy PN, Bohmer FD et al. Mislocalized activation of oncogenic RTKs switches downstream signaling outcomes. Mol Cell 2009; 36: 326–339.
Choudhary C, Schwable J, Brandts C, Tickenbrock L, Sargin B, Kindler T et al. AML-associated Flt3 kinase domain mutations show signal transduction differences compared with Flt3 ITD mutations. Blood 2005; 106: 265–273.
Schmidt-Arras D, Bohmer SA, Koch S, Muller JP, Blei L, Cornils H et al. Anchoring of FLT3 in the endoplasmic reticulum alters signaling quality. Blood 2009; 113: 3568–3576.
Zarrinkar PP, Gunawardane RN, Cramer MD, Gardner MF, Brigham D, Belli B et al. AC220 is a uniquely potent and selective inhibitor of FLT3 for the treatment of acute myeloid leukemia (AML). Blood 2009; 114: 2984–2992.
Levis M . Quizartinib in acute myeloid leukemia. Clin Adv Hematol Oncol 2013; 11: 586–588.
Knapper S . FLT3 inhibition in acute myeloid leukaemia. Br J Haematol 2007; 138: 687–699.
Grunwald MR, Levis MJ . FLT3 inhibitors for acute myeloid leukemia: a review of their efficacy and mechanisms of resistance. Int J Hematol 2013; 97: 683–694.
Levis M . FLT3 mutations in acute myeloid leukemia: what is the best approach in 2013? Hematology Am Soc Hematol Educ Program 2013; 2013: 220–226.
Cortes JE, Kantarjian H, Foran JM, Ghirdaladze D, Zodelava M, Borthakur G et al. Phase I study of quizartinib administered daily to patients with relapsed or refractory acute myeloid leukemia irrespective of FMS-like tyrosine kinase 3-internal tandem duplication status. J Clin Oncol 2013; 31: 3681–3687.
Wiernik PH . FLT3 inhibitors for the treatment of acute myeloid leukemia. Clin Adv Hematol Oncol 2010; 8: 429–436, 444.
Fischer T, Stone RM, Deangelo DJ, Galinsky I, Estey E, Lanza C et al. Phase IIB trial of oral Midostaurin (PKC412), the FMS-like tyrosine kinase 3 receptor (FLT3) and multi-targeted kinase inhibitor, in patients with acute myeloid leukemia and high-risk myelodysplastic syndrome with either wild-type or mutated FLT3. J Clin Oncol 2010; 28: 4339–4345.
Pawar R, Bali OP, Malhotra BK, Lamba G . Recent advances and novel agents for FLT3 mutated acute myeloid leukemia. Stem Cell Investig 2014; 1: 7.
Kindler T, Lipka DB, Fischer T . FLT3 as a therapeutic target in AML: still challenging after all these years. Blood 2010; 116: 5089–5102.
Rollig C, Serve H, Huttmann A, Noppeney R, Muller-Tidow C, Krug U et al. Addition of sorafenib versus placebo to standard therapy in patients aged 60 years or younger with newly diagnosed acute myeloid leukaemia (SORAML): a multicentre, phase 2, randomised controlled trial. Lancet Oncol 2015; 16: 1691–1699.
Stone RM, Mandrekar S, Sanford BL, Geyer S, Bloomfield CD, Dohner K et al The Multi-Kinase Inhibitor Midostaurin (M) Prolongs Survival Compared with Placebo(P) in Combination with Daunorubicin(D)/Cytarabine(C) Induction (ind), High-Dose C Consolidation (consol), and As Maintenance (maint) Therapy in Newly Diagnosed Acute Myeloid Leukemia (AML) Patients (pts) Age 18-60 with FLT3 Mutations (muts): An International Prospective Randomized (rand) P-Controlled Double-Blind Trial (CALGB 10603/RATIFY [Alliance]). 57th ASH Annual Meeting. Orlando, FL, Blood, 2015, p 6.
Breitenbuecher F, Markova B, Kasper S, Carius B, Stauder T, Bohmer FD et al. A novel molecular mechanism of primary resistance to FLT3-kinase inhibitors in AML. Blood 2009; 113: 4063–4073.
Smith CC, Lin K, Stecula A, Sali A, Shah NP . FLT3 D835 mutations confer differential resistance to type II FLT3 inhibitors. Leukemia 2015; 29: 2390–2392.
Weisberg E, Sattler M, Ray A, Griffin JD . Drug resistance in mutant FLT3-positive AML. Oncogene 2010; 29: 5120–5134.
von Bubnoff N, Engh RA, Aberg E, Sanger J, Peschel C, Duyster J . FMS-like tyrosine kinase 3-internal tandem duplication tyrosine kinase inhibitors display a nonoverlapping profile of resistance mutations in vitro. Cancer Res 2009; 69: 3032–3041.
Man CH, Fung TK, Ho C, Han HH, Chow HC, Ma AC et al. Sorafenib treatment of FLT3-ITD(+) acute myeloid leukemia: favorable initial outcome and mechanisms of subsequent nonresponsiveness associated with the emergence of a D835 mutation. Blood 2012; 119: 5133–5143.
Heidel F, Solem FK, Breitenbuecher F, Lipka DB, Kasper S, Thiede MH et al. Clinical resistance to the kinase inhibitor PKC412 in acute myeloid leukemia by mutation of Asn-676 in the FLT3 tyrosine kinase domain. Blood 2006; 107: 293–300.
Kampa-Schittenhelm KM, Heinrich MC, Akmut F, Dohner H, Dohner K, Schittenhelm MM . Quizartinib (AC220) is a potent second generation class III tyrosine kinase inhibitor that displays a distinct inhibition profile against mutant-FLT3, -PDGFRA and -KIT isoforms. Mol Cancer 2013; 12: 19.
Cools J, Mentens N, Furet P, Fabbro D, Clark JJ, Griffin JD et al. Prediction of resistance to small molecule FLT3 inhibitors: implications for molecularly targeted therapy of acute leukemia. Cancer Res 2004; 64: 6385–6389.
Opatz S, Polzer H, Herold T, Konstandin NP, Ksienzyk B, Zellmeier E et al. Exome sequencing identifies recurring FLT3 N676K mutations in core-binding factor leukemia. Blood 2013; 122: 1761–1769.
Tweeddale ME, Lim B, Jamal N, Robinson J, Zalcberg J, Lockwood G et al. The presence of clonogenic cells in high-grade malignant lymphoma: a prognostic factor. Blood 1987; 69: 1307–1314.
Mehra S, Messner H, Minden M, Chaganti RS . Molecular cytogenetic characterization of non-Hodgkin lymphoma cell lines. Genes Chromosomes Cancer 2002; 33: 225–234.
Krupka C, Kufer P, Kischel R, Zugmaier G, Bogeholz J, Kohnke T et al. CD33 target validation and sustained depletion of AML blasts in long-term cultures by the bispecific T-cell-engaging antibody AMG 330. Blood 2014; 123: 356–365.
Polzer H, Janke H, Schmid D, Hiddemann W, Spiekermann K . Casitas B-lineage lymphoma mutants activate AKT to induce transformation in cooperation with class III receptor tyrosine kinases. Exp Hematol 2013; 41: 271–280 e274.
Reindl C, Bagrintseva K, Vempati S, Schnittger S, Ellwart JW, Wenig K et al. Point mutations in the juxtamembrane domain of FLT3 define a new class of activating mutations in AML. Blood 2006; 107: 3700–3707.
Kelly LM, Liu Q, Kutok JL, Williams IR, Boulton CL, Gilliland DG . FLT3 internal tandem duplication mutations associated with human acute myeloid leukemias induce myeloproliferative disease in a murine bone marrow transplant model. Blood 2002; 99: 310–318.
Arreba-Tutusaus P, Mack TS, Bullinger L, Schnoder TM, Polanetzki A, Weinert S et al. Impact of FLT3-ITD location on sensitivity to TKI-therapy in vitro and in vivo. Leukemia 2016; 30: 1220–1225.
Sandhofer N, Bauer J, Reiter K, Dufour A, Rothenberg M, Konstandin NP et al. The new and recurrent FLT3 juxtamembrane deletion mutation shows a dominant negative effect on the wild-type FLT3 receptor. Sci Rep 2016; 6: 28032.
Krupka C, Kufer P, Kischel R, Zugmaier G, Lichtenegger FS, Kohnke T et al. Blockade of the PD-1/PD-L1 axis augments lysis of AML cells by the CD33/CD3 BiTE antibody construct AMG 330: reversing a T-cell-induced immune escape mechanism. Leukemia 2016; 30: 484–491.
Durben M, Schmiedel D, Hofmann M, Vogt F, Nubling T, Pyz E et al. Characterization of a bispecific FLT3 X CD3 antibody in an improved, recombinant format for the treatment of leukemia. Mol Ther 2015; 23: 648–655.
Chou TC . Theoretical basis, experimental design, and computerized simulation of synergism and antagonism in drug combination studies. Pharmacol Rev 2006; 58: 621–681.
Spiekermann K, Dirschinger RJ, Schwab R, Bagrintseva K, Faber F, Buske C et al. The protein tyrosine kinase inhibitor SU5614 inhibits FLT3 and induces growth arrest and apoptosis in AML-derived cell lines expressing a constitutively activated FLT3. Blood 2003; 101: 1494–1504.
Polzer H, Janke H, Schneider S, Hiddemann W, Subklewe M, Spiekermann K . Individualized treatment strategy with small-molecular inhibitors in acute myeloid leukemia with concurrent FLT3-ITD and FLT3-TKD mutation. J Clin Case Rep 2015; 5: 622.
Vick B, Rothenberg M, Sandhofer N, Carlet M, Finkenzeller C, Krupka C et al. An advanced preclinical mouse model for acute myeloid leukemia using patients' cells of various genetic subgroups and in vivo bioluminescence imaging. PLoS ONE 2015; 10: e0120925.
Larrue C, Saland E, Vergez F, Serhan N, Delabesse E, Mansat-De Mas V et al. Antileukemic activity of 2-deoxy-D-glucose through inhibition of N-linked glycosylation in acute myeloid leukemia with FLT3-ITD or c-KIT mutations. Mol Cancer Ther 2015; 14: 2364–2373.
Hofmann M, Grosse-Hovest L, Nubling T, Pyz E, Bamberg ML, Aulwurm S et al. Generation, selection and preclinical characterization of an Fc-optimized FLT3 antibody for the treatment of myeloid leukemia. Leukemia 2012; 26: 1228–1237.
Metzelder S, Wang Y, Wollmer E, Wanzel M, Teichler S, Chaturvedi A et al. Compassionate use of sorafenib in FLT3-ITD-positive acute myeloid leukemia: sustained regression before and after allogeneic stem cell transplantation. Blood 2009; 113: 6567–6571.
Small D . Targeting FLT3 for the treatment of leukemia. Semin Hematol 2008; 45 (3 Suppl 2): S17–S21.
Knapper S, Burnett AK, Littlewood T, Kell WJ, Agrawal S, Chopra R et al. A phase 2 trial of the FLT3 inhibitor lestaurtinib (CEP701) as first-line treatment for older patients with acute myeloid leukemia not considered fit for intensive chemotherapy. Blood 2006; 108: 3262–3270.
Smith CC, Viny AD, Massi ES, Kandoth C, Socci ND, Hsu H et al. Recurrent mutations in CCND3 confer clinical resistance to FLT3 inhibitors. Blood 2015; 126: 677.
Zhang H, Watanabe-Smith KM, Bottomly D, Wilmot B, McWeeney SK, Kantarjian HM et al. Exome sequencing informs mechanisms of clinical resistance to the FLT3-D835 inhibitor crenolanib. Blood 2015; 126: 2468.
Wolleschak D, Mack TS, Perner F, Frey S, Schnoder TM, Wagner MC et al. Clinically relevant doses of FLT3-kinase inhibitors quizartinib and midostaurin do not impair T-cell reactivity and function. Haematologica 2014; 99: e90–e93.
Zhao W, Gu YH, Song R, Qu BQ, Xu Q . Sorafenib inhibits activation of human peripheral blood T cells by targeting LCK phosphorylation. Leukemia 2008; 22: 1226–1233.
Whartenby KA, Small D, Calabresi PA . FLT3 inhibitors for the treatment of autoimmune disease. Expert Opin Investig Drugs 2008; 17: 1685–1692.
Kreutzman A, Porkka K, Mustjoki S . Immunomodulatory effects of tyrosine kinase inhibitors. Int Trends Immun 2013; 1: 17–28.
Wolfert MA, Boons GJ . Adaptive immune activation: glycosylation does matter. Nat Chem Biol 2013; 9: 776–784.
Natarajan K, Xie Y, Burcu M, Linn DE, Qiu Y, Baer MR . Pim-1 kinase phosphorylates and stabilizes 130 kDa FLT3 and promotes aberrant STAT5 signaling in acute myeloid leukemia with FLT3 internal tandem duplication. PLoS One 2013; 8: e74653.
Weisberg E, Boulton C, Kelly LM, Manley P, Fabbro D, Meyer T et al. Inhibition of mutant FLT3 receptors in leukemia cells by the small molecule tyrosine kinase inhibitor PKC412. Cancer Cell 2002; 1: 433–443.
Chu SH, Small D . Mechanisms of resistance to FLT3 inhibitors. Drug Resist Updat 2009; 12: 8–16.
Acknowledgements
This study was supported by the German Research Council (DFG) within the Collaborative Research Centre (SFB) 1243 ‘Cancer Evolution’ (projects A01, A05, A06, A07, A08 and A10). We thank Bianka Ksienzyk, Gudrun Mellert, Jutta Sturm, Belay Tizazu, Maike Fritschle and Miriam Krekel for technical support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Reiter, K., Polzer, H., Krupka, C. et al. Tyrosine kinase inhibition increases the cell surface localization of FLT3-ITD and enhances FLT3-directed immunotherapy of acute myeloid leukemia. Leukemia 32, 313–322 (2018). https://doi.org/10.1038/leu.2017.257
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2017.257
This article is cited by
-
Glycosylation: mechanisms, biological functions and clinical implications
Signal Transduction and Targeted Therapy (2024)
-
Tomatidine, a Steroidal Alkaloid, Synergizes with Cisplatin to Inhibit Cell Viability and Induce Cell Death Selectively on FLT3-ITD+ Acute Myeloid Leukemia Cells
Cell Biochemistry and Biophysics (2024)
-
Blockade of de novo pyrimidine biosynthesis triggers autophagic degradation of oncoprotein FLT3-ITD in acute myeloid leukemia
Oncogene (2023)
-
FLT3-ITD transduces autonomous growth signals during its biosynthetic trafficking in acute myelogenous leukemia cells
Scientific Reports (2021)
-
MAEA is an E3 ubiquitin ligase promoting autophagy and maintenance of haematopoietic stem cells
Nature Communications (2021)