Abstract
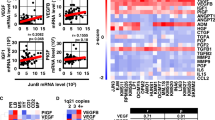
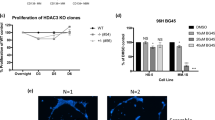
Hypoxia-inducible transcription factor-1 (HIF-1α) is overexpressed in multiple myeloma (MM) cells within the hypoxic microenvironment. Herein, we explored the effect of persistent HIF-1α inhibition by a lentivirus short hairpin RNA pool on MM cell growth either in vitro or in vivo and on the transcriptional and pro-angiogenic profiles of MM cells. HIF-1α suppression did not have a significant impact on MM cell proliferation and survival in vitro although, increased the antiproliferative effect of lenalidomide. On the other hand, we found that HIF-1α inhibition in MM cells downregulates the pro-angiogenic genes VEGF, IL8, IL10, CCL2, CCL5 and MMP9. Pro-osteoclastogenic cytokines were also inhibited, such as IL-7 and CCL3/MIP-1α. The effect of HIF-1α inhibition was assessed in vivo in nonobese diabetic/severe combined immunodeficiency mice both in a subcutaneous and an intratibial MM model. HIF-1α inhibition caused a dramatic reduction in the weight and volume of the tumor burden in both mouse models. Moreover, a significant reduction of the number of vessels and vascular endothelial growth factors (VEGFs) immunostaining was observed. Finally, in the intratibial experiments, HIF-1α inhibition significantly blocked bone destruction. Overall, our data indicate that HIF-1α suppression in MM cells significantly blocks MM-induced angiogenesis and reduces MM tumor burden and bone destruction in vivo, supporting HIF-1α as a potential therapeutic target in MM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Accession codes
References
Podar K, Richardson PG, Hideshima T, Chauhan D, Anderson KC . The malignant clone and the bone-marrow environment. Best Pract Res Clin Haematol 2007; 20: 597–612.
Vacca A, Ribatti D, Presta M, Minischetti M, Iurlaro M, Ria R et al. Bone marrow neovascularization, plasma cell angiogenic potential, and matrix metalloproteinase-2 secretion parallel progression of human multiple myeloma. Blood 1999; 93: 3064–3073.
Vacca A, Ribatti D . Bone marrow angiogenesis in multiple myeloma. Leukemia 2006; 20: 193–199.
Rajkumar SV, Leong T, Roche PC . Prognostic value of bone marrow angiogenesis in multiple myeloma. Clin Cancer Res 2000; 6: 3111–3116.
Munshi NC, Wilson C . Increased bone marrow microvessel density in newly diagnosed multiple myeloma carries a poor prognosis. Semin Oncol 2001; 28: 565–569.
Alexandrakis MG, Passam FH, Dambaki C, Pappa CA, Stathopoulos EN . The relation between bone marrow angiogenesis and the proliferation index Ki-67 in multiple myeloma. J Clin Pathol 2004; 57: 856–860.
Yaccoby S . Advances in the understanding of myeloma bone disease and tumour growth. Br J Haematol 2010; 149: 311–321.
Roodman GD . Targeting the bone microenvironment in multiple myeloma. J Bone Miner Metab 2010; 28: 244–250.
Dankbar B, Padro T, Leo R, Feldmann B, Kropff M, Mesters RM et al. Vascular endothelial growth factor and interleukin-6 in paracrine tumor-stromal cell interactions in multiple myeloma. Blood 2000; 95: 2630–2636.
Podar K, Anderson KC . The pathophisiologic role of VEGF in hematologic malignancies: therapeutic implications. Blood 2005; 105: 1383–1395.
Bisping G, Leo R, Wenning D, Dankbar B, Padró T, Kropff M et al. Paracrine interactions of basic fibroblast growth factor and interleukin-6 in multiple myeloma. Blood 2003; 101: 2775–2783.
Colla S, Morandi F, Lazzaretti M, Polistena P, Svaldi M, Coser P et al. Do human myeloma cells directly produce basic FGF? Blood 2003; 102: 3071–3072.
Shapiro VS, Mollenauer MN, Weiss A . Endogenous CD28 expressed on myeloma cells up-regulates interleukin-8 production: implications for multiple myeloma progression. Blood 2001; 98: 187–193.
Giuliani N, Colla S, Lazzaretti M, Sala R, Roti G, Mancini C et al. Pro-angiogenic properties of human myeloma cells: production of angiopoietin-1 and its potential relationship to myeloma-induced angiogenesis. Blood 2003; 102: 638–645.
Colla S, Morandi F, Lazzaretti M, Rizzato R, Lunghi P, Bonomini S et al. Human myeloma cells express the bone regulating gene Runx2/Cbfa1 and produce osteopontin that is involved in angiogenesis in multiple myeloma patients. Leukemia 2005; 19: 2166–2176.
Brahimi-Horn MC, Chiche J, Pouysségur J . Hypoxia and cancer. J Mol Med 2007; 85: 1301–1307.
Rankin EB, Giaccia AJ . The role of hypoxia-inducible factors in tumorigenesis. Cell Death Differ 2008; 15: 678–685.
Liao D, Johnson RS . Hypoxia: a key regulator of angiogenesis in cancer. Cancer Metastasis Rev 2007; 26: 281–290.
Weidemann A, Johnson RS . Biology of HIF-1α. Cell Death Differ 2008; 15: 621–627.
Lisy K, Peet DJ . Turn me on: regulating HIF transcriptional activity. Cell Death Differ 2008; 15: 642–649.
Yee Koh M, Spivak-Kroizman TR, Powis G . HIF-1 regulation: not so easy come, easy go. Trends Biochem Sci 2008; 33: 526–634.
Semenza GL . Regulation of cancer cell metabolism by hypoxia-inducible factor 1. Semin Cancer Biol 2009; 19: 12–16.
Hirota K, Semenza GL . ReguIation of angiogenesis by hypoxia-inducibIe factor 1. Crit Rev OncoI Hematol 2006; 59: 15–26.
Utting JC, Flanagan AM, Brandao-Burch A, Orriss IR, Arnett TR . Hypoxia stimulates osteoclast formation from human peripheral blood. Cell Biochem Funct 2010; 28: 374–380.
Bozec A, Bakiri L, Hoebertz A, Eferl R, Schilling AF, Komnenovic V et al. Osteoclast size is controlled by Fra-2 through LIF/LIF-receptor signalling and hypoxia. Nature 2008; 454: 221–225.
Hiraga T, Kizaka-Kondoh S, Hirota K, Hiraoka M, Yoneda T . Hypoxia and hypoxia-inducible factor-1 expression enhance osteolytic bone metastases of breast cancer. Cancer Res 2007; 67: 4157–4163.
Colla S, Storti P, Donofrio G, Todoerti K, Bolzoni M, Lazzaretti M et al. Low bone marrow oxygen tension and hypoxia-inducible factor-1α overexpression characterize patients with multiple myeloma: role on the transcriptional and proangiogenic profiles of CD138(+) cells. Leukemia 2010; 24: 1967–1970.
Zhang J, Sattler M, Tonon G, Grabher C, Lababidi S, Zimmerhackl A et al. Targeting angiogenesis via a c-Myc/hypoxia-inducible factor-1alpha-dependent pathway in multiple myeloma. Cancer Res 2009; 69: 5082–5090.
Martin SK, Diamond P, Gronthos S, Peet DJ, Zannettino AC . The emerging role of hypoxia, HIF-1 and HIF-2 in multiple myeloma. Leukemia 2011; 25: 1533–1542.
Azab AK, Hu J, Quang P, Azab F, Pitsillides C, Awwad R et al. Hypoxia promotes dissemination of multiple myeloma through acquisition of epithelial to mesenchymal transition-like features. Blood 2012; 119: 5782–5794.
Hu J, Handisides DR, Van Valckenborgh E, De Raeve H, Menu E, Vande Broek I et al. Targeting the multiple myeloma hypoxic niche with TH-302, a hypoxia-activated prodrug. Blood 2010; 116: 1524–1527.
Storti P, Donofrio G, Colla S, Airoldi I, Bolzoni M, Agnelli L et al. HOXB7 expression by myeloma cells regulates their pro-angiogenic properties in multiple myeloma patients. Leukemia 2011; 25: 527–537.
Campbell RA, Berenson JR . Animal models of multiple myeloma and their utility in drug discovery. Curr Protoc Pharmacol 2008; Chapter 14, Unit 14: 9.
D'Souza S, del Prete D, Jin S, Sun Q, Huston AJ, Kostov FE et al. Gfi1 expressed in bone marrow stromal cells is a novel osteoblast suppressor in patients with multiple myeloma bone disease. Blood 2011; 118: 6871–6880.
Asosingh K, De Raeve H, de Ridder M, Storme GA, Willems A, Van Riet I et al. Role of the hypoxic bone marrow microenvironment in 5T2MM murine myeloma tumor progression. Haematologica 2005; 90: 810–817.
Hu Y, Kirito K, Yoshida K, Mitsumori T, Nakajima K, Nozaki Y et al. Inhibition of hypoxia-inducible factor-1 function enhances the sensitivity of multiple myeloma cells to melphalan. Mol Cancer Ther 2009; 8: 2329–2338.
Colla S, Zhan F, Xiong W, Wu X, Xu H, Stephens O et al. The oxidative stress response regulates DKK1 expression through the JNK signaling cascade in multiple myeloma plasma cells. Blood 2007; 109: 4470–4477.
Veschini L, Belloni D, Foglieni C, Cangi MG, Ferrarini M, Caligaris-Cappio F et al. Hypoxia-inducible transcription factor-1 alpha determines sensitivity of endothelial cells to the proteosome inhibitor bortezomib. Blood 2007; 109: 2565–2570.
Colla S, Tagliaferri S, Morandi F, Lunghi P, Donofrio G, Martorana D et al. The new tumor-suppressor gene inhibitor of growth family member 4 (ING4) regulates the production of proangiogenic molecules by myeloma cells and suppresses hypoxia-inducible factor-1 alpha (HIF-1alpha) activity: involvement in myeloma-induced angiogenesis. Blood 2007; 110: 4464–4475.
Negaard HF, Iversen N, Bowitz-Lothe IM, Sandset PM, Steinsvik B, Ostenstad B et al. Increased bone marrow microvascular density in haematological malignancies is associated with differential regulation of angiogenic factors. Leukemia 2009; 23: 162–169.
Arendt BK, Velazquez-Dones A, Tschumper RC, Howell KG, Ansell SM, Witzig TE et al. Interleukin 6 induces monocyte chemoattractant protein-1 expression in myeloma cells. Leukemia 2002; 16: 2142–2147.
Van Valckenborgh E, Bakkus M, Munaut C, Noël A, Pierre Y, Asosingh K et al. Upregulation of matrix metalloproteinase-9 in murine 5T33 multiple myeloma cells by interaction with bone marrow endothelial cells. Int J Cancer 2002; 101: 512–518.
Purushothaman A, Chen L, Yang Y, Sanderson RD . Heparanase stimulation of protease expression implicates it as a master regulator of the aggressive tumor phenotype in myeloma. J Biol Chem 2008; 283: 32628–32636.
Choi SJ, Cruz JC, Craig F, Chung H, Devlin RD, Roodman GD et al. Macrophage inflammatory protein 1-alpha is a potential osteoclast stimulatory factor in multiple myeloma. Blood 2000; 96: 671–675.
Giuliani N, Colla S, Sala R, Moroni M, Lazzaretti M, La Monica S et al. Human myeloma cells stimulate the receptor activator of nuclear factor-kappa B ligand (RANKL) in T lymphocytes: a potential role in multiple myeloma bone disease. Blood 2002; 100: 4615–4621.
Hatfield KJ, Bedringsaas SL, Ryningen A, Gjertsen BT, Bruserud O . Hypoxia increases HIF-1α expression and constitutive cytokine release by primary human acute myeloid leukaemia cells. Eur Cytokine Netw 2010; 21: 154–164.
Nishida C, Kusubata K, Tashiro Y, Gritli I, Sato A, Ohki-Koizumi M et al. MT1-MMP plays a critical role in hematopoiesis by regulating HIF-mediated chemokine/cytokine gene transcription within niche cells. Blood 2012; 119: 5405–5416.
Krishnamachary B, Berg-Dixon S, Kelly B, Agani F, Feldser D, Ferreira G et al. Regulation of colon carcinoma cell invasion by hypoxia-inducible factor 1. Cancer Res 2003; 63: 1138–1143.
Li L, Lin X, Staver M, Shoemaker A, Semizarov D, Fesik SW et al. Evaluating hypoxia-inducible factor-1alpha as a cancer therapeutic target via inducible RNA interference in vivo. Cancer Res 2005; 65: 7249–7258.
Greenberger LM, Horak ID, Filpula D, Sapra P, Westergaard M, Frydenlund HF et al. A RNA antagonist of hypoxia-inducible factor-1alpha, EZN-2968, inhibits tumor cell growth. Mol Cancer Ther 2008; 7: 3598–3608.
Acknowledgements
This study was supported by grants from the ‘International Myeloma Foundation’; and ‘Associazione Italiana per la Ricerca sul Cancro’ A.I.R.C, IG2009 no. 8530 (N.G.), no. IG4569 (A.N.) and no. 13018 (I.A.); Special Program Molecular Clinical Oncology 5 per mille no. 9965 (N.G.) and no. 9980 (A.N.), the Multiple Myeloma Research Foundation and grant support R01 AR059679, R21 CA141426, R01AR057308, and Merit Review funds from the Veterans Administration. (G.D.R.). We thanks Ministero Italiano dell’ Istruzione, Università e Ricerca (MIUR) and Italian Association against Leukemia, Lymphoma and Myeloma (AIL). We thanks Carla Palumbo and Marzia Ferretti for their support in the histological analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Leukemia website
Supplementary information
Rights and permissions
About this article
Cite this article
Storti, P., Bolzoni, M., Donofrio, G. et al. Hypoxia-inducible factor (HIF)-1α suppression in myeloma cells blocks tumoral growth in vivo inhibiting angiogenesis and bone destruction. Leukemia 27, 1697–1706 (2013). https://doi.org/10.1038/leu.2013.24
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2013.24
Keywords
This article is cited by
-
JunB is a key regulator of multiple myeloma bone marrow angiogenesis
Leukemia (2021)
-
Hypoxia-induced CREB cooperates MMSET to modify chromatin and promote DKK1 expression in multiple myeloma
Oncogene (2021)
-
Influence of metformin on HIF-1 pathway in multiple myeloma
Pharmacological Reports (2020)
-
Established Models and New Paradigms for Hypoxia-Driven Cancer-Associated Bone Disease
Calcified Tissue International (2018)
-
Integration of hypoxic HIF-α signaling in blood cancers
Oncogene (2017)