Abstract
Objective:
To characterize pregnant patients’ knowledge, attitudes and preferences regarding antenatal HIV testing for themselves and their sexual partners.
Study Design:
Observational, mixed methods study of HIV-negative pregnant women from a university-based urban clinic. Participants completed an anonymous survey about HIV testing for themselves and their partners. Descriptive statistics, bivariable analyses, multivariable logistic regression and qualitative thematic analysis were utilized.
Results:
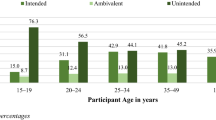
One hundred and forty-two patients (mean age 28.6±5.5 years) participated. A majority (57.7%) were married or partnered, and 92.9% reported having at least one current sexual partner. Although a majority (62.8%) reported their partner had a prior HIV test, and 93.0% of these women were aware of test results, only 20.7% reported partner testing had occurred in the past 6 months. Women who had a prior HIV test, who were older or who were non-white were more likely to be aware of their partner’s HIV status. A majority (66.9%) of women desired knowledge of their partner’s current status and 76.0% believed their partners would like to know his HIV status; in addition, 74% were interested in receiving partner testing at the site of prenatal care. Qualitative analysis demonstrated that health concerns and believing HIV knowledge is important to the relationship were motivators for desiring partner testing.
Conclusions:
In this urban community, a majority of pregnant women do not know HIV test results of their sexual partner during the current pregnancy. Women desired to know their partner’s HIV status and were receptive to partner testing at the site of prenatal care or other locations. Partner testing may be a critical step toward elimination of seroconversion during pregnancy and maternal-to-child HIV transmission.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Panel on Treatment of HIV-Infected Pregnant Women and Prevention of Perinatal Transmission. Recommendations for use of antiretroviral drugs in pregnant HIV-1-infected women for maternal health and interventions to reduce perinatal HIV transmission in the United States 2015 [December 28, 2015]. Available from http://aidsinfo.nih.gov/contentfiles/lvguidelines/PerinatalGL.pdf.
Centers for Disease Control. HIV Among Pregnant Women, Infants, and Children 2014. Available from http://www.cdc.gov/hiv/risk/gender/pregnantwomen/facts/.
Sperling RS, Shapiro DE, Coombs RW, Todd JA, Herman SA, McSherry GD et al. Maternal viral load, zidovudine treatment, and the risk of transmission of human immunodeficiency virus type 1 from mother to infant. Pediatric AIDS Clinical Trials Group Protocol 076 Study Group. N Engl J Med 1996; 335 (22): 1621–1629.
American College of Obstetrics and Gynecology Committee on Obstetric Practice. ACOG Committee Opinion No. 418: prenatal and perinatal human immunodeficiency virus testing: expanded recommendations. Obstet Gynecol 2008; 112 (3): 739–742.
Moyer VA U. S. Preventive Services Task Force. Screening for HIV: US Preventive Services Task Force Recommendation Statement. Ann Intern Med 2013; 159 (1): 51–60.
Workowski KA, Berman S, Centers for Disease Control and Prevention (CDC). Sexually transmitted diseases treatment guidelines, 2010. MMWR Recomm Rep 2010; 59 (RR-12): 1–110.
American College of Obstetricians and Gynecologists Committee on Obstetric Practice and HIV Expert Work Group. Prenatal and perinatal human immunodeficiency virus testing: expanded recommendations, Committee Opinion Number 635. Obstet Gynecol 2015; 125: 1544–1547.
Mahy M, Stover J, Kiragu K, Hayashi C, Akwara P, Luo C et al. What will it take to achieve virtual elimination of mother-to-child transmission of HIV? An assessment of current progress and future needs. Sex Transm Infect 2010; 86 (Suppl 2): ii48–ii55.
Mugo NR, Heffron R, Donnell D, Wald A, Were EO, Rees H et al. Increased risk of HIV-1 transmission in pregnancy: a prospective study among African HIV-1-serodiscordant couples. AIDS 2011; 25 (15): 1887–1895.
Duval M, Faye A, Rohrlich P, Levine M, Matheron S, Larchee R et al. Failure of pediatric AIDS prevention despite maternal HIV screening in Paris, France. J Acquir Immune Defic Syndr Hum Retrovirol 1999; 20 (1): 100–101.
Dinh T, Delaney K, Goga A, Jackson D, Lombard C, Woldesenbet S et al. Impact of maternal HIV seroconversion during pregnancy on early maternal to child transmission of HIV (MTCT) measured at 4-8 weeks postpartum in South Africa 2011-2012: a national population-based evaluation. PLoS One 2015; 10 (5): e0125525.
Huang Y, Lasry A, Hutchinson A, Sansom S . A systematic review on cost effectiveness of HIV prevention interventions in the United States. Appl Health Econ Health Policy 2015; 13 (2): 149–156.
Postma MJ, Beck EJ, Mandalia S, Sherr L, Walters MD, Houweling H et al. Universal HIV screening of pregnant women in England: cost effectiveness analysis. BMJ 1999; 318 (7199): 1656–1660.
Musheke M, Bond V, Merten S . Couple experiences of provider-initiated couple HIV testing in an antenatal clinic in Lusaka, Zambia: lessons for policy and practice. BMC Health Serv Res 2013; 13: 97.
Crepaz N, Tungol-Ashmon M, Vosburgh H, Baack B, Mullins M . Are couple-based interventions more effective than interventions delivered to individuals in promoting HIV protective behaviours? A meta-analysis. AIDS Care 2015; 27 (11): 1361–1366.
Chicago Department of Public Health HIV/STI Surveillance Report, 2014. City of Chicago: Chicago, IL, USA, 2014.
Ulin P, Robinson E, Tolley E . Qualitative Methods in Public Health: A Field Guide for Applied Research. Jossey-Bass: San Francisco, CA, USA, 2005.
Sansom S, Jamieson D, Farnham P, BUlterys M, Fowler M . Human immunodeficiency virus retesting during pregnancy: costs and effectiveness in preventing perinatal transmission. Obstet Gynecol 2003; 102 (4): 782–790.
Hall H, An Q, Tang T, Song R, Chen M, Green T et al. Prevalence of diagnosed and undiagnosed HIV infection - United States, 2008-2012. MMWR Morb Mortal Wkly Rep 2015; 64 (24): 657–662.
Becker S, Mlay R, Schwandt HM, Lyamuya E . Comparing couples' and individual voluntary counseling and testing for HIV at antenatal clinics in Tanzania: a randomized trial. AIDS Behav 2010; 14 (3): 558–566.
Farquhar C, Kiarie JN, Richardson BA, Kabura MN, John FN, Nduati RW et al. Antenatal couple counseling increases uptake of interventions to prevent HIV-1 transmission. J Acquir Immune Defic Syndr 2004; 37 (5): 1620–1626.
Conkling M, Shutes E, Karita E, Chomba E, Tichacek A, Sinkala M et al. Couples' voluntary counselling and testing and nevirapine use in antenatal clinics in two AFrican capitals: a prospective cohort study. J Int AIDS Soc 2010; 13: 1–10.
Rosenberg N, Mtande T, Saidi F, Stanley C, Jere E, Paile L et al. Recruiting male partners for couple HIV testing and counselling in Malawi's option B+ programme: an unblinded randomised controlled trial. Lancet HIV 2015; 2 (11): e483–e491.
Lolekha R, Kullerk N, Wolfe M, Klumthanom K, Singhagowin T, Pattansin S et al. Assessment of a couples HIV counseling and testing program for pregnant women and their partners in antenatal care (ANC) in 7 provinces, Thailand. BMC Int Health Hum Rights 2014; 14 (39): 1–10.
Mohlala B, Boily M, Gregson S . The forgotten half of the equation: randomized controlled trial of a male invitation to attend couple voluntary counselling and testing. AIDS 2011; 25 (12): 1534–1541.
Koo K, Makin J, Forsyth B . Where are the men? Targeting male partners in preventing mother-to-child transmission. AIDS Care 2013; 25 (1): 43–48.
Acknowledgements
LMY and ESM are supported by NICHD K12 HD050121-11 and K12 HD050121-09, respectively.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This abstract was presented as a poster presentation at the 2015 National HIV Prevention Conference, 6–9 December 2015, in Atlanta, GA, USA.
Rights and permissions
About this article
Cite this article
Yee, L., Goldberger, A., Garcia, P. et al. Sexual partner testing for HIV to eliminate mother-to-child HIV transmission: a needs assessment in an urban hospital community clinic. J Perinatol 37, 21–26 (2017). https://doi.org/10.1038/jp.2016.160
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.160
This article is cited by
-
The End Is in Sight: Current Strategies for the Elimination of HIV Vertical Transmission
Current HIV/AIDS Reports (2023)