Abstract
Objective:
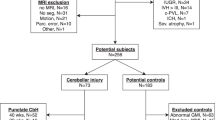
To determine the impact of cerebellar hemorrhage (CH) on mortality and adverse neurodevelopmental (ND) outcome rates in extremely preterm infants admitted to a tertiary neonatal unit.
Study Design:
A total of 1120 eligible infants (<28 weeks gestation) were born from 1998 to 2008 and had at least one cranial ultrasound. ND outcome was determined at 12 to 18 months corrected age.
Results:
Most CH (75%) occurred in infants <25 weeks gestation. CH did not affect mortality rates, however, it was associated with both mental and motor impairments, with incidence rate ratios of 3.08 (1.71 to 4.84) and 2.12 (1.12 to 3.45), respectively. Moreover, the risk of cerebral palsy (CP) was increased in infants with CH involving the medial part of the cerebellum.
Conclusion:
Our findings substantiate recent reports about the cerebellum, highlighting its role in cognitive and executive functions, and associating early cerebellar injury not only with CP but also with learning, affective and behavioral disorders.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Itabashi K, Horiuchi T, Kusuda S, Kabe K, Itani Y, Nakamura T et al. Mortality rates for extremely low birth weight infants born in Japan in 2005. Pediatrics 2009; 123: 445–450.
Limperopoulos C, Benson CB, Bassan H, Disalvo DN, Kinnamon DD, Moore M et al. Cerebellar hemorrhage in the preterm infant: ultrasonographic findings and risk factors. Pediatrics 2005; 116: 717–724.
Johnsen SD, Bodensteiner JB, Lotze TE . Frequency and nature of cerebellar injury in the extremely premature survivor with cerebral palsy. J Child Neurol 2005; 20: 60–64.
Limperopoulos C, Bassan H, Gauvreau K, Robertson RL, Sullivan NR, Benson CB et al. Does cerebellar injury in premature infants contribute to the high prevalence of long-term cognitive, learning, and behavioral disability in survivors? Pediatrics 2007; 120: 584–593.
Zayek MM, Trimm RF, Hamm CR, Peevy KJ, Benjamin JT, Eyal FG . The limit of viability. A single regional unit's experience. Arch Pediatr Adolesc Med 2011; 165 (2): 126–133.
Stoodley CJ, Schmahmann JD . Evidence for topographic organization in the cerebellum of motor control versus cognitive and affective processing. Neuroimage 2009; 44: 489–501.
Timmann D, Daum I . How consistent are cognitive impairments in patients with cerebellar disorders? Behav Neurol 2010; 23: 81–100.
Maertens PM . Imaging through the posterior fontanelle. J Child Neurol 1989; 4: S62–S67.
Cramer BC, Jequier S, O’Gorman AM . Sonography of the neonatal craniocervical junction. AJR Am J Roentgenol 1986; 147 (1): 133–139.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr 1978; 92: 529–534.
Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M . The definition and classification of cerebral palsy. Dev Med Child Neurol Suppl 2007; 49: 8–14.
Bayley N . Bayley Scales of Infant Development, 2nd edn. Psychological Corp: San Antonio, TX, 1993.
Bayley N . Bayley Scales of Infant and Toddler Development, 3rd edn. Psychological Corp: San Antonio, TX, 2006.
Martin R, Roessmann U, Fanaroff A . Massive intracerebellar hemorrhage in low-birth-weight infants. J Pediatr 1976; 89 (2): 290–293.
Grunnet ML, Shields WD . Cerebellar hemorrhage in the premature infant. J Pediatr 1976; 88 (4 Part 1): 605–608.
Perlman JM, Nelson JS, McAlister WH, Volpe JJ . Intracerebellar hemorrhage in a premature newborn: diagnosis by real-time ultrasound and correlation with autopsy findings. Pediatrics 1983; 71: 159–162.
Merrill JD, Piecuch RE, Fell SC, Barkovich AJ, Goldstein RB . A new pattern of cerebellar hemorrhages in preterm infants. Pediatrics 1998; 102: e62.
Woodward LJ, Anderson PJ, Austin NC, Howard K, Inder TE . Neonatal MRI to predict neurodevelopmental outcomes in preterm infant. N Engl J Med 2006; 355: 685–694.
Hintz SR, O’Shea M . Neuroimaging and neurodevelopmental outcomes in preterm infants. Semin Perinatol 2008; 32: 11–19.
Chang CH, Chang FM, Yu CH, Ko HC, Chen HY . Assessment of fetal cerebellar volume using three-dimensional ultrasound. Ultrasound Med Biol 2000; 26 (6): 981–988.
Lemire RJ, Loeser JD, Leech RW, Alvord EC . Normal and Abnormal Development of the Nervous System. Harper and Row: Hagerstown, Maryland, 1975; 237.
Limperopoulos C, Soul JS, Gauvreau K, Huppi PS, Warfield SK, Bassan H et al. Late gestation cerebellar growth is rapid and impeded by premature birth. Pediatrics 2005; 115: 688–695.
Shah DK, Anderson PJ, Carlin JB, Pavlovic M, Howard K, Thompson DK et al. Reduction in cerebellar volumes in preterm infants: relationship to white matter injury and neurodevelopment at two years of age. Pediatr Res 2006; 60: 97–102.
Allin MPG, Salaria S, Nosarti C, Nosarti C, Wyatt J, Rifkin L et al. Vermis and lateral lobes of the cerebellum in adolescents born very preterm. Neuroreport 2005; 161: 1821–1824.
Glickstein M . Thinking about the cerebellum. Brain 2006; 129: 288–290.
Timmann D, Daum I . Cerebellar contributions to cognitive functions: a progress report after two decades of research. Cerebellum 2007; 6 (3): 159–162.
Messerschmidt A, Fuiko R, Prayer D, Brugger PC, Boltshauser E, Zoder G et al. Disrupted cerebellar development in preterm infants is associated with impaired neurodevelopmental outcome. Eur J Pediatr 2008; 167: 1141–1147.
Anderson PJ, De Luca CR, Hutchinson E, Roberts G, Doyle LW . Underestimation of developmental delay by the new Bayley-III Scale. Arch Pediatr Adolesc Med 2010; 164 (4): 352–356.
Tam EW, Rosenbluth G, Rogers EE, Ferriero DM, Glidden D, Goldstein RB et al. Cerebellar hemorrhage on magnetic resonance imaging in preterm newborns associated with abnormal neurologic outcome. J Pediatr 2011; 158 (2): 245–250.
De Vries LS, Van Haastert IC, Rademaker KJ, Koopman C, Groenendaal F . Ultrasound abnormalities preceding cerebral palsy in high-risk preterm infants. J Pediatr 2004; 144: 815–820.
Limperopoulos C, Chilingaryan G, Guizard N, Robertson RL, Du Plessis AJ . Cerebellar injury in the premature infant is associated with impaired growth of specific cerebral regions. Pediatr Res 2010; 68: 145–150.
Acknowledgements
We extend sincere appreciation to all our NICU and developmental clinic staff for their dedication to outstanding medical care.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zayek, M., Benjamin, J., Maertens, P. et al. Cerebellar hemorrhage: a major morbidity in extremely preterm infants. J Perinatol 32, 699–704 (2012). https://doi.org/10.1038/jp.2011.185
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2011.185
Keywords
This article is cited by
-
Ultrasound imaging of preterm brain injury: fundamentals and updates
Pediatric Radiology (2022)
-
Rate of head ultrasound abnormalities at one month in very premature and extremely premature infants with normal initial screening ultrasound
Pediatric Radiology (2022)
-
Preterm infants with isolated cerebellar hemorrhage show bilateral cortical alterations at term equivalent age
Scientific Reports (2020)
-
The CHOPIn Study: a Multicenter Study on Cerebellar Hemorrhage and Outcome in Preterm Infants
The Cerebellum (2019)
-
Brain imaging in preterm infants <32 weeks gestation: a clinical review and algorithm for the use of cranial ultrasound and qualitative brain MRI
Pediatric Research (2018)