Abstract
Objective:
To determine whether consanguinity adversely influences pregnancy outcome in South India, where consanguinity is a common means of family property retention.
Study Design:
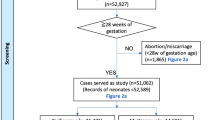
Data were collected from a prospective cohort of 647 consenting women, consecutively registered for antenatal care between 14 and 18 weeks gestation, in Belgaum district, Karnataka in 2005. Three-generation pedigree charts were drawn for consanguineous participants. χ2-Test and Student's t-test were used to assess categorical and continuous data, respectively, using SPSS version 14. Multivariate logistic regression adjusted for confounding variables.
Result:
Overall, 24.1% of 601 women with singleton births and outcome data were consanguineous. Demographic characteristics between study groups were similar. Non-consanguineous couples had fewer stillbirths (2.6 vs 6.9% P=0.017; adjusted P=0.050), miscarriages (1.8 vs 4.1%, P=0.097; adjusted P=0.052) and lower incidence of birth weight <2500 g (21.8 vs 29.5%, P=0.071, adjusted P=0.044). Gestation <37 weeks was 6.2% in both the groups. Adjusted for consanguinity and other potential confounders, age <20 years was protective of stillbirth (P=0.01), pregnancy loss (P=0.023) and preterm birth (P=0.013), whereas smoking (P=0.015) and poverty (P=0.003) were associated with higher rates of low birth weight.
Conclusion:
Consanguinity significantly increases pregnancy loss and birth weight <2500 g.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Lawn JE, Cousens S, Zupan J . 4 million neonatal deaths: when? where? why? Lancet 2005; 365 (9462): 891–900.
NNPD Network. Report Of The National Neonatal-Perinatal Database. Nodal Center: AIIMS, New Delhi, 2002–03.
World Health Organization. Promoting Optimal Fetal Development: Report of Technical Consultation. WHO: Geneva, 2006.
Jehan I, Zaidi S, Rizvi S, Mobeen N, McClure EM, Munoz B et al. Dating gestational age by last menstrual period, symphysis-fundal height, and ultrasound in urban Pakistan. Int J Gynecol Obstet 2010; 110: 231–234.
United Nations Children's Fund. State of the World's Children 2009. UNICEF: New York, 2010, pp 119–125.
Bittles AH . The role and significance of consanguinity as a demographic variable. Pop Dev Rev 1994; 20 (3): 561–584.
Bittles AH, Mason WM, Greene J, Rao NA . Reproductive behavior and health in consanguineous marriages. Science 1991; 252 (5007): 789–794.
Teebi AS, El-Shanti HI . Consanguinity: implications for practice, research and policy. Lancet 2006; 367 (9515): 970–971.
Kulkarni ML, Kurien M . Consanguinity and its effect on fetal growth and development: a South Indian study. J Med Genet 1990; 27: 348–352.
Paddaiah G, Reddy CG . Effect of consanguinity on anthropometric measurements in the newborn. Indian J Pediatr 1980; 47: 133–136.
Sibert JR, Jadhav M, Inbaraj SG . Fetal growth and parental consanguinity. Arch Dis Child 1979; 54: 317–319.
Rao PSS, Inbaraj SG . Inbreeding effects on fetal growth and development. J Med Genet 1980; 17: 27–33.
Sanghvi ID . Inbreeding in India. Eugen Quart 1966; 13: 291–301.
Bittles AH . Consanguinity and its relevance to medical genetics. Clin Genet 2001; 60: 89–98.
Harlap S, Kleinhaus K, Perrin MC, Calderon-Margalit R, Paltiel O, Deutsch L et al. Consanguinity and birth defects in the Jerusalem Perinatal Study Cohort. Hum Hered 2008; 66: 180–189.
Nath A, Patil C, Naik VA . Prevalence of consanguineous marriages in a rural community and its effect on pregnancy outcome. Indian J Community Med 2004; 29 (1): 41–43.
Liascovich R, Rittler M, Castilla EE . Consanguinity in South America: demographic aspects. Hum Hered 2001; 5: 27–34.
International Institute for Population Sciences (IIPS) and Macro International. National Family Health Survey (NFHS-3) 2005–06 India: Volume I. StatCompiler. IIPS: Mumbai, 2007.
Asha-Bai PV, John TJ, Subramanium WR . Reproductive wastage and developmental disorders in relation to consanguinity in South India. Trop Geogr Med 1981; 33 (3): 279–290.
Badaruddoza MA, Manzir A . Inbreeding effects on the incidence of congenital disorders and fetal growth and development at birth in North India. Indian Pediatr 1998; 35: 1110–1113.
Verma IC, Prema A, Puri RK . Health effects of consanguinity in Pondicherry. Indian Pediatr 1992; 29: 685–691.
Basaran N, Hassa H, Basaran A, Artan S, Stevenson JD, Sayli BS . The effect of consanguinity on the reproductive wastage in the Turkish population. Clin Genet 1989; 36: 168–173.
Magnus P, Berg K, Bjerkedal T . Association of parental consanguinity with decreased birth weight and increased rate of early death and congenital malformation. Clin Genet 1985; 2: 335–342.
Hussain R . The impact of consanguinity and inbreeding on perinatal mortality in Karachi, Pakistan. Paediatr Perinat Epidemiol 1998; 12 (4): 370–382.
Khoury SA, Massad DF . Consanguinity fertility, reproductive wastage, infant mortality and congenital malformations in Jordan. Saudi Med J 2000; 21 (2): 150–158.
Stanton C, Lawn JE, Rahman H, Wilczynska-Ketende K, Hill K . Stillbirth rates: delivering estimates in 190 countries. Lancet 2006; 367 (9521): 1487–1494.
Jain VK, Nalini P, Chandra R . Congenital malformations, reproductive wastage and consanguineous mating. Aust N Z J Obstet Gynaecol 1993; 33 (1): 33–36.
Bromiker R, Glam Barch M, Hammerman C, Amitai Y . Association of parental consanguinity with congenital malformations among Arab Newborns in Jerusalem. Clin Genet 2004; 66: 63–66.
Jaber L, Merlob P, Gabriel R, Shohat M . Effects of consanguineous marriages on reproductive outcome in an Arab Community in Israel. J Med Genet 1997; 34: 1000–1002.
Mumtaz G, Nassar AH, Mahfoud Z, El-Khamra A, Al-Choueiri N, Adra A et al. Consanguinity: a risk factor for preterm birth at less than 33 weeks’ gestation. 2010. Am J Epidemiol 2010; 172: 1424–1430.
Sandridge Al, Takeddin J, Al-Kaabi E, Frances Y . Consanguinity in Qatar: knowledge, attitude and practice in a population born between 1946 and 1991. J Biosoc Sci 2010; 42: 59–82.
Darmstadt GL, Yakoob MY, Haws RA, Menezes EV, Soomro T, Bhutta ZA . Reducing stillbirths: interventions during labour. BMC Pregnancy Childbirth 2009; 9 (Suppl 1): S6.
Barros FC, Bhutta ZA, Batra M, Hansen TN, Victora CG, Rubens CE . Global report on preterm birth and stillbirth (3 of 7): evidence for effectiveness of interventions. BMC Pregnancy and Childbirth 2010; 10 (Suppl 1): S3 http://www.biomedcentral.com/1471-2393/10/S1/S3.
Bhutta ZA, Darmstadt GL, Haws RA, Yakoob MY, Lawn JE . Delivering interventions to reduce the global burden of stillbirths: improving service supply and community demand. BMC Pregnancy and Childbirth 2009; 9 (Suppl 1): S7 http://www.biomedcentral.com/1471-2393-9-S1-S7.
Lawn JE, Kinney M, Lee ACC, Chopra M, Donnay F, Paul VK et al. Reducing intrapartum-related deaths and disability: can the health system deliver? Int J Gynecol Obstet 2009; 107: S123–S142.
Acknowledgements
This study was conducted as part of the Junior Scholar Programme of the Global Network for Women's and Children's Health Research, National Institute for Child Health and Human Development, Bethesda, MD, USA and JN Medical College, Belgaum, India and the University of Missouri at Kansas City, USA. We thank all participating auxiliary nurse midwives, field research officers and Global Network Site 8 research unit staff for their efforts. We thank Dr Nancy L Sloan for editing the manuscript. Support was provided by the Department of Obstetrics and Gynecology, JN Medical College, Belgaum, India. The Eunice Kennedy Shriver National Institutes of Child Health and Human Development and the Fogarty International Center provided funding through the UMKC-JNMC Global Network for Women's and Children Health Research Unit (grant number 5U01HD042372-08) and by the Bill and Melinda Gates Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This work emanated from a collaboration to improve the research infrastructure and capacity of Jawaharlal Nehru Medical College, in Belgaum District, India. The collaboration provided NIH and RTI support for partnership with, and mentoring of, local faculty. This work was collaboratively conceptualized, implemented and analyzed by all authors.
Rights and permissions
About this article
Cite this article
Bellad, M., Goudar, S., Edlavitch, S. et al. Consanguinity, prematurity, birth weight and pregnancy loss: a prospective cohort study at four primary health center areas of Karnataka, India. J Perinatol 32, 431–437 (2012). https://doi.org/10.1038/jp.2011.115
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2011.115
Keywords
This article is cited by
-
The spectrum of chromosomal translocations in the Arab world: ethnic-specific chromosomal translocations and their relevance to diseases
Chromosoma (2022)
-
Association between adverse pregnancy outcomes and preceding risk factors: a cross-sectional study from Nashik District, India
BMC Pregnancy and Childbirth (2021)
-
Stillbirth 2010–2018: a prospective, population-based, multi-country study from the Global Network
Reproductive Health (2020)
-
Fetale Obduktionen
Der Pathologe (2017)
-
Structural and genomic variation in preterm birth
Pediatric Research (2016)