Abstract
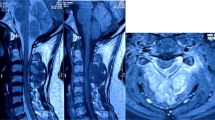
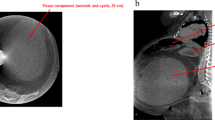
Infantile fibrosarcoma represents less than 1% of all childhood cancers, but it is the most common soft-tissue sarcoma in those under 1 year of age. We report an infant with congenital infantile fibrosarcoma diagnosed as hemangiopericytoma. He was treated with chemotherapy and extremity-sparing surgery. Amputation was avoided.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Pritchard DJ, Soule EH, Taylor WF, Ivins JC . Fibrosarcoma: a clinico pathologic study of 199 tumors of the soft tissues of extremities and trunk. Cancer 1974; 33: 888–897.
Blocker S, Koening J, Ternberg J . Congenital fibrosarcoma. J Pediatr Surg. 1987; 22: 665–670.
Ferrari A, Casanova M, Bisogno G, Mattke A, Meazza C, Gronchi A et al. Hemangiopericytoma in pediatric ages: a report from the Italian and German Soft Tissue Cooperative Group. Cancer 2001; 92: 2692–2698.
Hays DM, Mirabal VQ, Karlan MS . Fibrosarcoma in infants and children. Pediatr Surg 1970; 5: 176–183.
Cofer BR, Vesico PJ, Wiener ES . Infantile fibrosarcoma: complete excision is the apropriate treatment. Ann Surg Oncol 1996; 3: 159–161.
Kurkchubasche AG, Halvorson EG, Forman EN, Terek RM, Ferguson WS . The role of preoperative chemotherapy in the treatment of infantile fibrosarcoma. J Pediatr Surg 2000; 35: 880–883.
Rodriguez-Galindo C, Ramsey K, Jenkins JJ, Poquette CA, Kaste SC, Merchant TE et al. Hemangiopericytoma in children and in infants. Cancer 2000; 88: 198–204.
Hoey SA, Letts RM, Jimenez C . Infantile hemangiopericytoma of the musculoskeletal system: case report and literature review. J Pediatr Orthop 1998; 18: 359–362.
Blatt J, Woosley JT, Taylor L . Spontaneous remission of multifocal infantile hemangiopericytoma. Med Pediatr Oncol 2001; 36: 320–322.
Nappi O, Ritter JH, Pettinato G, Wick MR . Hemangiopericytoma: histopathological pattern or clinicopathologic entity? Semin Diagn Pathol 1995; 12: 221–232.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Akyüz, C., Sari, N., Vargel, İ. et al. A newborn with infantile fibrosarcoma of foot: treatment with chemotherapy and extremity-sparing surgery. J Perinatol 30, 63–65 (2010). https://doi.org/10.1038/jp.2009.92
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2009.92