Abstract
Objective:
To determine whether plasma N-terminal probrain natriuretic peptide (NT-proBNP) in premature infants could identify hemodynamically significant patent ductus arteriosus (HsPDA) and to determine the correlation between serial plasma NT-proBNP and echocardiographic assessment of ductal shunting.
Study Design:
An observational study involving 35 preterm infants who underwent echocardiographic assessment for PDA on day 2, 4 and 7 of life with simultaneous blood sampling for determination of NT-proBNP concentrations. HsPDA was diagnosed by left-to-right ductal shunt on color Doppler, measuring diameter >1.5 mm on two-dimensional echocardiography plus ⩾2 clinical features of PDA.
Result:
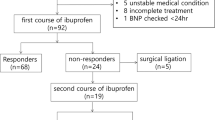
Plasma NT-proNBP levels on day 2 in the HsPDA group (n=12) were significantly higher than in non-HsPDA group (n=23) with a median of 16 353 pg ml−1 (interquartile range (IQR), 12 360–33 459; range, 10 316–104 998) vs 3914 pg ml−1 (IQR, 2601–5782; range, 1535–19 516) (P<0.001), respectively. Eight infants (67%) in the HsPDA group responded to an initial course of indomethacin or ibuprofen and their NT-proBNP levels significantly decreased within 48 h after treatment compared with non-responders (P=0.007). NT-proBNP concentrations were significantly correlated with left atrial to aortic root ratio. A cut-off NT-proBNP on day 2 of 10 180 pg ml−1 offered the best predictive values for HsPDA with a sensitivity of 100% and a specificity of 91%.
Conclusion:
Plasma NT-proBNP on day 2 was found as a sensitive marker for predicting HsPDA in preterm infants. Successful closure of PDA was also correspondent with the decline in plasma NT-proBNP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Korhonen P, Tammela O, Koivisto AM, Laippala P, Ikonen S . Frequency and risk factors in bronchopulmonary dysplasia in a cohort of very low birth weight infants. Early Hum Dev 1999; 54 (3): 245–258.
Shimada S, Kasai T, Hoshi A, Murata A, Chida S . Cardiocirculatory effects of patent ductus arteriosus in extremely low-birth-weight infants with respiratory distress syndrome. Pediatr Int 2003; 45 (3): 255–262.
Evans N, Kluckow M . Early ductal shunting and intraventricular haemorrhage in ventilated preterm infants. Arch Dis Child Fetal Neonatal Ed 1996; 75 (3): F183–F186.
Dudell GG, Gersony WM . Patent ductus arteriosus in neonates with severe respiratory disease. J Pediatr 1984; 104 (6): 915–920.
Evans N . Current controversies in the diagnosis and treatment of patent ductus arteriosus in preterm infants. Adv Neonatal Care 2003; 3 (4): 168–177.
Wyllie J . Treatment of patent ductus arteriosus. Semin Neonatol 2003; 8 (6): 425–432.
Fowlie PW, Davis PG . Prophylactic indomethacin for preterm infants: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed 2003; 88 (6): F464–F466.
Cooke L, Steer P, Woodgate P . Indomethacin for asymptomatic patent ductus arteriosus in preterm infants. Cochrane Database Syst Rev 2003; (2): CD003745.
Schmidt B, Roberts RS, Fanaroff A, Davis P, Kirpalani HM, Nwaesei C et al. Indomethacin prophylaxis, patent ductus arteriosus, and the risk of bronchopulmonary dysplasia: further analyses from the Trial of Indomethacin Prophylaxis in Preterms (TIPP). J Pediatr 2006; 148 (6): 730–734.
Gournay V, Roze JC, Kuster A, Daoud P, Cambonie G, Hascoet JM et al. Prophylactic ibuprofen versus placebo in very premature infants: a randomised, double-blind, placebo-controlled trial. Lancet 2004; 364 (9449): 1939–1944.
Van Overmeire B, Van de Broek H, Van Laer P, Weyler J, Vanhaesebrouck P . Early versus late indomethacin treatment for patent ductus arteriosus in premature infants with respiratory distress syndrome. J Pediatr 2001; 138 (2): 205–211.
Davis P, Turner-Gomes S, Cunningham K, Way C, Roberts R, Schmidt B . Precision and accuracy of clinical and radiological signs in premature infants at risk of patent ductus arteriosus. Arch Pediatr Adolesc Med 1995; 149 (10): 1136–1141.
Kupferschmid C, Lang D, Pohlandt F . Sensitivity, specificity and predictive value of clinical findings, m-mode echocardiography and continuous-wave Doppler sonography in the diagnosis of symptomatic patent ductus arteriosus in preterm infants. Eur J Pediatr 1988; 147 (3): 279–282.
Urquhart DS, Nicholl RM . How good is clinical examination at detecting a significant patent ductus arteriosus in the preterm neonate? Arch Dis Child 2003; 88 (1): 85–86.
Skelton R, Evans N, Smythe J . A blinded comparison of clinical and echocardiographic evaluation of the preterm infant for patent ductus arteriosus. J Paediatr Child Health 1994; 30 (5): 406–411.
Stoupakis G, Klapholz M . Natriuretic peptides: biochemistry, physiology, and therapeutic role in heart failure. Heart Dis 2003; 5 (3): 215–223.
Pfister R, Schneider CA . Natriuretic peptides BNP and NT-pro-BNP: established laboratory markers in clinical practice or just perspectives? Clin Chim Acta 2004; 349 (1–2): 25–38.
Goetze J . Biochemistry of Pro-B-Type natriuretic peptide-derived peptides: the endocrine heart revisited. Clin Chem 2004; 50: 1503–1510.
Hall C . Essential biochemistry and physiology of (NT-pro)BNP. Eur J Heart Fail 2004; 6: 257–260.
Kunii Y, Kamada M, Ohtsuki S, Araki T, Kataoka K, Kageyama M et al. Plasma brain natriuretic peptide and the evaluation of volume overload in infants and children with congenital heart disease. Acta Med Okayama 2003; 57 (4): 191–197.
Mir TS, Marohn S, Laer S, Eiselt M, Grollmus O, Weil J . Plasma concentrations of N-terminal pro-brain natriuretic peptide in control children from the neonatal to adolescent period and in children with congestive heart failure. Pediatrics 2002; 110 (6): e76.
Nir A, Nasser N . Clinical value of NT-ProBNP and BNP in pediatric cardiology. J Card Fail 2005; 11 (5 Suppl): S76–S80.
Norozi K, Buchhorn R, Kaiser C, Hess G, Grunewald RW, Binder L et al. Plasma N-terminal pro-brain natriuretic peptide as a marker of right ventricular dysfunction in patients with tetralogy of Fallot after surgical repair. Chest 2005; 128 (4): 2563–2570.
Pfister R, Scholz M, Wielckens K, Erdmann E, Schneider CA . Use of NT-proBNP in routine testing and comparison to BNP. Eur J Heart Fail 2004; 6 (3): 289–293.
Costello-Boerrigter LC, Boerrigter G, Redfield MM, Rodeheffer RJ, Urban LH, Mahoney DW et al. Amino-terminal pro-B-type natriuretic peptide and B-type natriuretic peptide in the general community: determinants and detection of left ventricular dysfunction. J Am Coll Cardiol 2006; 47 (2): 345–353.
Mir TS, Laux R, Hellwege HH, Liedke B, Heinze C, von Buelow H et al. Plasma concentrations of aminoterminal pro atrial natriuretic peptide and aminoterminal pro brain natriuretic peptide in healthy neonates: marked and rapid increase after birth. Pediatrics 2003; 112 (4): 896–899.
Koch A, Singer H . Normal values of B type natriuretic peptide in infants, children, and adolescents. Heart 2003; 89 (8): 875–878.
Yoshibayashi M, Kamiya T, Saito Y, Nakao K, Nishioka K, Temma S et al. Plasma brain natriuretic peptide concentrations in healthy children from birth to adolescence: marked and rapid increase after birth. Eur J Endocrinol 1995; 133 (2): 207–209.
Puddy VF, Amirmansour C, Williams AF, Singer DR . Plasma brain natriuretic peptide as a predictor of haemodynamically significant patent ductus arteriosus in preterm infants. Clin Sci (Lond) 2002; 103 (1): 75–77.
Choi BM, Lee KH, Eun BL, Yoo KH, Hong YS, Son CS et al. Utility of rapid B-type natriuretic peptide assay for diagnosis of symptomatic patent ductus arteriosus in preterm infants. Pediatrics 2005; 115 (3): e255–e261.
Flynn PA, da Graca RL, Auld PA, Nesin M, Kleinman CS . The use of a bedside assay for plasma B-type natriuretic peptide as a biomarker in the management of patent ductus arteriosus in premature neonates. J Pediatr 2005; 147 (1): 38–42.
Sanjeev S, Pettersen M, Lua J, Thomas R, Shankaran S, L'Ecuyer T . Role of plasma B-type natriuretic peptide in screening for hemodynamically significant patent ductus arteriosus in preterm neonates. J Perinatol 2005; 25 (11): 709–713.
Oh J . Assessment of systolic function and quantification of cardiac chambers. In: Oh J, Seward J, Talik A (eds). The Echo Manual. Lippincott Williams & Wilkins: Philadelphia, 2007, p 117.
El Hajjar M, Vaksmann G, Rakza T, Kongolo G, Storme L . Severity of the ductal shunt: a comparison of different markers. Arch Dis Child Fetal Neonatal Ed 2005; 90 (5): F419–F422.
El-Khuffash AF, Amoruso M, Culliton M, Molloy EJ . N-terminal pro-B-type natriuretic peptide as a marker of ductal haemodynamic significance in preterm infants: a prospective observational study. Arch Dis Child Fetal Neonatal Ed 2007; 92 (5): F421–F422.
Farombi-Oghuvbu IO, Matthews T, Mayne PD, Guerin H, Corcoran D . N-terminal Pro-B-type natriuretic peptide: a measure of significant patent ductus arteriosus. Arch Dis Child Fetal Neonatal Ed 2008; 93 (4): F257–F260.
El-Khuffash A, Davis PG, Walsh K, Molloy EJ . Cardiac troponin T and N-terminal-pro-B type natriuretic peptide reflect myocardial function in preterm infants. J Perinatol 2008; 28 (7): 482–486.
El-Khuffash AF, Barry D, Walsh K, Davis PG, Molloy EJ . Biochemical markers may identify preterm infants with a patent ductus arteriosus at high risk of death of severe intraventricular haemorrhage. Arch Dis Child Fetal Neonatal Ed 2008; 93 (6): F407–F412.
Acknowledgements
The study is supported by the Ramathibodi Research Fund (grant no. 48055). The authors express their sincere thanks and gratitude to Professor Amnuay Thithapandha and Mahippathorn Chinnapha for their valuable comments and suggestions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nuntnarumit, P., Khositseth, A. & Thanomsingh, P. N-terminal probrain natriuretic peptide and patent ductus arteriosus in preterm infants. J Perinatol 29, 137–142 (2009). https://doi.org/10.1038/jp.2008.185
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.185
Keywords
This article is cited by
-
Early prediction of spontaneous Patent Ductus Arteriosus (PDA) closure and PDA-associated outcomes: a prospective cohort investigation
BMC Pediatrics (2019)
-
Urinary NT-proBNP levels and echocardiographic parameters for patent ductus arteriosus
Journal of Perinatology (2017)
-
The relationship between BNP, NTproBNP and echocardiographic measurements of systemic blood flow in very preterm infants
Journal of Perinatology (2014)
-
Serial N-terminal pro-brain natriuretic peptide measurement as a predictor of significant patent ductus arteriosus in preterm infants beyond the first week of life
European Journal of Pediatrics (2014)
-
Urinary NT-proBNP and ductal closure in preterm infants
Journal of Perinatology (2013)