Abstract
Objective:
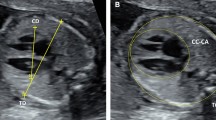
Autoimmune-mediated congenital complete heart block (CCHB) is associated with significant perinatal morbidity and mortality, and prenatal monitoring of these fetuses is a significant challenge. The cerebroplacental Doppler ratio (CPR), defined as the ratio of the middle cerebral artery pulsatility index (MCA-PI) to the umbilical artery pulsatility index (UA-PI), is predictive of perinatal outcome in growth-restricted fetuses. This study tests the hypothesis that the CPR would be useful in monitoring fetal well-being in fetuses with CCHB.
Study Design:
We reviewed data on all patients diagnosed prenatally with autoimmune-mediated CCHB at our institution over the past 2 years. The fetal echocardiograms from each patient were analyzed for: CPR, UA-PI, MCA-PI, cardiothoracic ratio, degree of tricuspid regurgitation, ventricular function and presence of effusions. We compared hemodynamic data from the fetal echocardiogram before delivery in patients who required urgent pacemaker placement postnatally to those patients that did not require an urgent pacemaker.
Result:
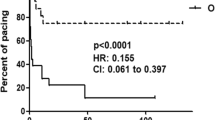
Five patients with autoimmune-mediated CCHB were identified, and two patients required urgent pacemaker placement. The CPR before delivery was significantly lower in the patients who required urgent pacemaker placement (0.97±0.06 versus 1.45±0.03; P=0.003), but there was no difference in other fetal echocardiographic markers between groups. Both patients requiring urgent pacemaker placement had a CPR less than 1.08.
Conclusion:
The CPR is predictive of postnatal outcome in fetuses with CCHB and is useful in prenatal monitoring of these patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Michaelsson M, Engle MA . Congenital complete heart block: an international study of the natural history. Cardiovasc Clin 1972; 4: 85–101.
Buyon JP, Hiebert R, Copel J, Craft J, Friedman D, Katholi M et al. Autoimmune-associated congenital heart block: demographics, mortality, morbidity and recurrence rates obtained from a national neonatal lupus registry. J Am Coll Cardiol 1998; 31: 1658–1666.
Singh GK, Shumway JB, Amon E, Marino CJ, Nouri S, Winn HN . Role of fetal echocardiography in the management of isolated fetal heart block with ventricular rate <55 bpm. Am J Perinatol 1998; 15: 661–668.
Eronen M, Siren MK, Ekblad H, Tikanoja T, Julkunen H, Paavilainen T . Short- and long-term outcome of children with congenital complete heart block diagnosed in utero or as a newborn. Pediatrics 2000; 106: 86–91.
Jaeggi ET, Hamilton RM, Silverman ED, Zamora SA, Hornberger LK . Outcome of children with fetal, neonatal or childhood diagnosis of isolated congenital atrioventricular block. A single institution's experience of 30 years. J Am Coll Cardiol 2002; 39: 130–137.
Groves AM, Allan LD, Rosenthal E . Outcome of isolated congenital complete heart block diagnosed in utero. Heart 1996; 75: 190–194.
Eronen M, Heikkila P, Teramo K . Congenital complete heart block in the fetus: hemodynamic features, antenatal treatment, and outcome in six cases. Pediatr Cardiol 2001; 22: 385–392.
Veille JC, Covitz W . Fetal cardiovascular hemodynamics in the presence of complete atrioventricular block. Am J Obstetr Gynecol 1994; 170: 1258–1262.
Bahado-Singh RO, Kovanci E, Jeffres A, Oz U, Deren O, Copel J et al. The Doppler cerebroplacental ratio and perinatal outcome in intrauterine growth restriction. Am J Obstetr Gynecol 1999; 180: 750–756.
Gosling RG, King DH . Arterial assessment by Doppler-shift ultrasound. Proc R Soc Med 1974; 67: 447–449.
Jaeggi ET, Fouron JC, Silverman ED, Ryan G, Smallhorn J, Hornberger LK . Transplacental fetal treatment improves the outcome of prenatally diagnosed complete atrioventricular block without structural heart disease. Circulation 2004; 110: 1542–1548.
Nield LE, Silverman ED, Taylor GP, Smallhorn JF, Mullen JB, Silverman NH et al. Maternal anti-Ro and anti-La antibody-associated endocardial fibroelastosis. Circulation 2002; 105: 843–848.
Eronen M . Outcome of fetuses with heart disease diagnosed in utero. Arch Dis Child 1997; 77: F41–F46.
Donofrio MT, Gullquist SD, Mehta ID, Moskowitz WB . Congenital complete heart block: fetal management protocol, review of the literature, and report of the smallest successful pacemaker implantation. J Perinatol 2004; 24: 112–117.
Huhta J . Guidelines for the evaluation of heart failure in the fetus with or without hydrops. Pediatr Cardiol 2004; 25: 274–286.
Friedman DM, Zervoudakis I, Buyon JP . Perinatal monitoring of fetal well-being in the presence of congenital heart block. Am J Perinatol 1998; 15: 669–673.
Hecher K, Campbell S, Doyle P, Harrington K, Nicolaides K . Assessment of fetal compromise by Doppler ultrasound investigation of the fetal circulation. Arterial, intracardiac, and venous blood flow velocity studies. Circulation 1995; 91: 129–138.
Ebrashy A, Azmy O, Ibrahim M, Waly M, Edris A . Middle cerebral/umbilical artery resistance index ratio as sensitive parameter for fetal well-being and neonatal outcome in patients with preeclampsia: case-control study. Croat Med J 2005; 46: 821–825.
Al-Gazali W, Chapman MG, Chita SK, Crawford DC, Allan LD . Doppler assessment of umbilical artery blood flow for the prediction of outcome in fetal cardiac abnormality. Br J Obstetri Gynaecol 1987; 94: 742–745.
Baschat AA, Gembruch U . The cerebroplacental Doppler ratio revisited. Ultrasound Obstet Gynecol 2003; 21: 124–127.
Odibo AO, Riddick C, Pare E, Stamilio DM, Macones GA . Cerebroplacental doppler ratio and adverse perinatal outcomes in intrauterine growth restriction. J Ultrasound Med 2005; 24: 1223–1228.
Gramellini D, Folli MC, Raboni S, Vadora E, Merialdi A . Cerebral-umbilical Doppler ratio as a predictor of adverse perinatal outcome. Obstetri Gynecol 1992; 79: 416–420.
Devine PA, Bracero LA, Lysikiewicz A, Evans R, Womack S, Byrne DW . Middle cerebral to umbilical artery Doppler ratio in post-date pregnancies. Obstetr Gynecol 1994; 84: 856–860.
Akalin-Sel T, Nicolaides KH, Peacock J, Campbell S . Doppler dynamics and their complex interrelation with fetal oxygen pressure, carbon dioxide pressure, and pH in growth-retarded fetuses. Obstetr Gynecol 1994; 84: 439–444.
Sepulveda W, Shennan AH, Peek MJ . Reverse end-diastolic flow in the middle cerebral artery: an agonal pattern in the human fetus. Am J Obstetr Gynecol 1996; 174: 1645–1647.
Acknowledgements
We thank Angela J Liske, MD, for her editorial assistance. No grants or other financial support were received for this publication.
Author information
Authors and Affiliations
Corresponding author
Additional information
Conflicts of interest/Disclosure
None of the authors has a conflict of interest.
Rights and permissions
About this article
Cite this article
Fleming, G., Bircher, A., Kavanaugh-McHugh, A. et al. The cerebroplacental Doppler ratio predicts postnatal outcome in fetuses with congenital heart block. J Perinatol 28, 791–796 (2008). https://doi.org/10.1038/jp.2008.105
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.105