Abstract
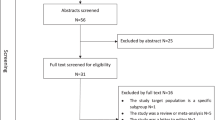
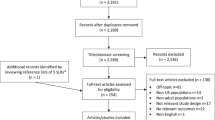
Hypertension is a rising global burden, and low- and middle-income countries account for 80% of deaths due to complications of hypertension. Hypertension can be controlled by adhering to anti-hypertensive medication. However, non-adherence is an increasing challenge. This review aims to systematically evaluate non-adherence to anti-hypertensive medication among adults in low- and middle-income countries and explore factors affecting non-adherence to anti-hypertensive medication. We performed a systematic search for studies published between 1 January 2000 and 31 August 2015. A selection process was performed for data extraction with a combination of Medical Subject Headings terms: ‘hypertension’ and ‘adherence’. Further search criteria were: language (‘english’), species (‘humans’), and low- and middle-income countries. A total of 22 studies met the inclusion criteria. The pooled percentage of non-adherence when using the eight-item Morisky Medication Adherence Scale (MMAS) was 63.35% (confidence of interval (CI): 38.78–87.91) and 25.45% (CI:17.23–33.76) when using the 80 and 90% cut-off scales. The factors were classified into the five dimensions of adherence defined by the World Health Organization, and the majority of the studies reported factors from the dimension ‘social and economic factors’. This systematic review demonstrated considerable variation of non-adherence to anti-hypertensive medication in low- and middle-income countries depending on the methods used to estimate non-adherence. The results showed a high non-adherence when the MMAS eight-item scale was used and low when the 80 and 90% cut-off scales were used. The majority of factors affecting non-adherence to anti-hypertensive medication fell within the World Health Organization defined dimension ‘social and economic factors’.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Lim SS, Vos T, Flaxman AD, Danaei G, Shibuya K, Adair-Rohani H et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 2012; 380 (9859): 2224–2260.
WHO Global Status Report on Noncommunicable Diseases 2010. World Health Organization: Geneva, 2011.
Neupane D, McLachlan CS, Sharma R, Gyawali B, Khanal V, Mishra SR et al. Prevalence of hypertension in member countries of South Asian Association for Regional Cooperation (SAARC): systematic review and meta-analysis. Medicine (Baltimore) 2014; 93 (13): e74.
Tailakh A, Evangelista LS, Mentes JC, Pike NA, Phillips LR, Morisky DE. . Hypertension prevalence, awareness, and control in Arab countries: a systematic review. Nurs Health Sci 2014; 16: 126–130.
Ataklte F, Erqou S, Kaptoge S, Taye B, Echouffo-Tcheugui JB, Kengne AP. . Burden of undiagnosed hypertension in sub-Saharan Africa: a systematic review and meta-analysis. Hypertension 2015; 65 (2): 291–298.
WHO Adherence to Long-Term Therapies: Evidence for Action. World Health Organization: Geneva, 2003.
Elliott WJ. . What factors contribute to the inadequate control of elevated blood pressure? J Clin Hypertens (Greenwich) 2008; 10: 20–26.
Tan X PI, Chang J. . Review of the four item Morisky Medication Adherence Scale (MMAS-4) and eight item Morisky Medication Adherence Scale (MMAS-8). Innov Pharm 2014; 5, (3) 165.
Ambaw AD, Alemie GA, WYohannes SM, Mengesha ZB. . Adherence to antihypertensive treatment and associated factors among patients on follow up at University of Gondar Hospital, Northwest Ethiopia. BMC Public Health 2012; 12: 282.
Kretchy IA, Owusu-Daaku FT, Danquah S. . Locus of control and anti-hypertensive medication adherence in Ghana. Pan African Med J 2014; 17 (1): 13.
Bhandari S, Sarma PS, Thankappan KR. . Adherence to antihypertensive treatment and its determinants among urban slum dwellers in Kolkata, India. Asia-Pacific J Public Health 2015; 27 (2): 74–84.
Azlin B, Hatta S, Norzila Z, Sharifa Ezat WP . Health locus of control among non-compliance hypertensive patients undergoing pharmacotherapy. Malaysian J Psychiatr 2007; 16 (1): 20–39.
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-Analysis of Observational Studies in Epidemiology (MOOSE) Group. J Am Med Assoc 2000; 283: 2008–2012.
Chalmers J, MacMahon S, Mancia G, Whitworth J, Beilin L, Hansson L et al. World Health Organization-International Society of Hypertension Guidelines for the management of hypertension. Guidelines sub-committee of the World Health Organization. Clin Exp Hypertens 1999; 21 (5–6): 1009–1060.
Updated Income Classifications. The World Bank 2014 Available at www.worldbank.org.
Lee GKY, Wang HHX, Liu KQL, Cheung Y, Morisky DE, Wong MCS . Determinants of medication adherence to antihypertensive medications among a Chinese Population Using Morisky Medication Adherence Scale. PLoS ONE 2013; 8 (4): e62775.
Zhao YMS, Wang B, Qi-Weilin MD, Yang AMS . Effect of medication adherence on blood pressure control and risk factors for antihypertensive medication adherence. J Eval Clin Pract 2015; 21: 166–172.
Yassine M, Awada S, Rachidi S, Zein S, Bawab W, El-Hajj Z et al. Evaluation of medication adherence in Lebanese hypertensive patients. J Epidemiol Glob Health, (e-pub ahead of print 29 July 2015; doi:10.1016/j.jegh.2015.07.002.
Okwuonu CG, Ojimadu NE, Okaka EI, Akemokwe FM. . Patient-related barriers to hypertension control in a Nigerian population. Int J Gen Med 2014; 7: 345–353.
Zyoud SH, Al-Jabi SW, Sweileh WM, Wildali AH, Saleem HM, Aysa HA et al. Health-related quality of life associated with treatment adherence in patients with hypertension: a cross-sectional study. Int J Cardiol 2013; 168 (3): 2981–2983.
Hashmi SK, Afridi MB, Abbas K, Sajwani RA, Saleheen D, Frossard PM et al. Factors associated with adherence to anti-hypertensive treatment in Pakistan. PLoS ONE 2007; 2 (3): e280.
Youssef RM, Moubarak II . Patterns and determinants of treatment compliance among hypertensive patients. Eastern Mediterr Health J 2002; 8: 576–592.
Wong MCS, Jiang JY, Griffiths SM. . Factors associated with antihypertensive drug compliance in 83 884 Chinese patients: a cohort study. J Epidemiol Commun Health 2010; 64: 895–901.
Morisky DE, Green LW, Levine DM. . Concurrent and predictive-validity of a self-reported measure of medication adherence. Med Care 1986; 24 (1): 67–74.
Morisky DE, Ang A, Krousel-Wood M, Ward HJ. . Predictive validity of a medication adherence measure in an outpatient setting. J Clin Hypertens (Greenwich) 2008; 10 (5): 348–354.
Kim MT, Hill MN, Bone LR, Levine DM. . Development and testing of the hill-bone compliance to high blood pressure therapy scale. Prog Cardiovasc Nurs 2000; 15 (3): 90–96.
Hu W-Y, Tseng C-T, Chiu T-Y, Yu Chao Y-M . The effectiveness of a comprehensive intervention to improve drug compliant behaviors and blood pressure control for hypertensive patients in community. Chin J Fam Med 1996; 6: 169–179.
Chen SL, Tsai JC, Lee WL. . The impact of illness perception on adherence to therapeutic regimens of patients with hypertension in Taiwan. J Clin Nurs 2009; 18 (15): 2234–2244.
Khanam MA, Lindeboom W, Koehlmoos TL, Alam DS, Niessen L, Milton AH. . Hypertension: adherence to treatment in rural Bangladesh findings from a population-based study. Glob Health Action 2014; 7: 25028.
Bharucha NE, Kuruvilla T. . Hypertension in the Parsi community of Bombay: a study on prevalence, awareness and compliance to treatment. BMC Public Health 2003; 3 (1): Available at http://www.biomedcentral.com/1471-2458/3/1.
Mungati M, Manangazira P, Takundwa L, Gombe NT, Rusakaniko S, Tshimanga M. . Factors affecting diagnosis and management of hypertension in Mazowe District of Mashonaland Central Province in Zimbabwe: 2012. BMC Cardiovasc Disorders 2014; 14 (102): Available at http://www.biomedcentral.com/1471-2261/14/102.
Ramli A, Ahmad NS, Paraidathathu T. . Medication adherence among hypertensive patients of primary health clinics in Malaysia. Patient Prefer Adherence 2012; 6: 613–622.
Turki AK, Sulaiman SAS . Elevated blood pressure among patients with hypertension in general hospital of Penang, Malaysia: does poor adherence matter? Int J Pharm Pharm Sci 2010; 2 (1): 24–32.
Osamor PE, Owumi BE. . Factors associated with treatment compliance in hypertension in Southwest Nigeria. J Health Popul Nutr 2011; 29 (6): 619–628.
Iloh GUP, Ofoedu JN, Njoku PU, Amadi AN, Godswill-Uko EU. . Medication adherence and blood pressure control amongst adults with primary hypertension attending a tertiary hospital primary care clinic in Eastern Nigeria. Afr J Prm Health Care Fam Med 2013; 5 (1): Available at http://dx.doi.org/10.4102/phcfm.v5i1.446.
Karaeren H, Yokuşoğlu M, Uzun S, Baysan O, Köz C, Kara B et al. The effect of the content of the knowledge on adherence to medication in hypertensive patients. Ana do lu Kar di yol Derg 2009; 9: 183–188.
Ungari AQ, Dal-Fabbro AL. . Adherence to drug treatment in hypertensive patients on the Family Health Program. Braz J Pharm Sci 2010; 46: 811–818.
Von-Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. . The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 2008; 61 (4): 344–349.
Lemstra M, Alsabbagh MW. . Proportion and risk indicators of nonadherence to antihypertensive therapy: a meta-analysis. Patient Prefer Adherence 2014; 8: 211–218.
Tavakol M, Dennick R. . Making sense of Cronbach's alpha. Int J Med Educ 2011; 2: 53–55.
Lars Ostberg TB. . Adherence to medication. N Engl J Med 2005; 356 (5): 487–497.
Liu J, Liu S, Yan J, Yi Q, Huang H. . Adherence to immunosuppressive medication in renal transplant recipients from follow-up outpatient in China: association of 2 different measurement methods. Clin Ther 2015; 37 (11): 2572–2580.
Brier MJ, Chambless D, Gross R, Su HI, DeMichele A, Mao JJ. . Association between self-report adherence measures and oestrogen suppression among breast cancer survivors on aromatase inhibitors. Eur J Cancer 2015; 51 (14): 1890–1896.
Haynes RB, Taylor DW, Sackett DL, Gibson ES, Bernholz CD, Mukherjee J. . Can simple clinical measurements detect patient noncompliance? Hypertension 1980; 2 (6): 757–764.
Assawasuwannakit P, Braund R, Duffull SB. . A model-based meta-analysis of the influence of factors that impact adherence to medications. J Clin Pharm Ther 2014; 40 (1): 24–31.
AlGhurair SA, Hughes CA, Simpson SH, Guirguis LM. . A systematic review of patient self-reported barriers of adherence to antihypertensive medications using the world health organization multidimensional adherence model. J Clin Hypertens (Greenwich) 2012; 14 (12): 877–886.
Albaz RS . Factors affecting patient compliance in Saudi Arabia. J Soc Sci 1997; 25: 5–8.
AlGhurair SA, Hughes CA, Simpson SH, Guirguis LM. . A systematic review of patient self-reported barriers of adherence to antihypertensive medications using the World Health Organization Multidimensional Adherence Model. J Clin Hyperten 2012; 14 (12): 877–886.
Morrison A, Polisena J, Hosereau D, Moulton K, Clark M, Fiander M et al. The effect of english-language restriction on systematic review-based meta-analyses: a systematic review of empirical studies. Int J Technol Assess Health Care 2012; 28: 138–144.
Acknowledgements
We would like to thank Aarhus University Library for assisting on database searches. Moreover, we would like to thank Mia Enggaard Thomassen for support in the final phase of writing the article.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Nielsen, J., Shrestha, A., Neupane, D. et al. Non-adherence to anti-hypertensive medication in low- and middle-income countries: a systematic review and meta-analysis of 92443 subjects. J Hum Hypertens 31, 14–21 (2017). https://doi.org/10.1038/jhh.2016.31
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2016.31
This article is cited by
-
Management of Hypertension in the Asia-Pacific Region: A Structured Review
American Journal of Cardiovascular Drugs (2024)
-
Family support and medication adherence among residents with hypertension in informal settlements of Nairobi, Kenya: a mixed-method study
Journal of Human Hypertension (2023)
-
Blood Pressure Association with the 8-Item Morisky Medication Adherence Scale in Hypertensive Adults from Low-Resource Primary Care Settings: Results from a Prospective Cohort Nested within a Randomised Controlled Trial
High Blood Pressure & Cardiovascular Prevention (2023)
-
Adherence to antihypertensive treatment during the COVID-19 pandemic: findings from a cross-sectional study
Clinical Hypertension (2022)
-
Perception of risk of hypertension related complications and adherence to antihypertensive drugs: a primary healthcare based cross-sectional study
BMC Primary Care (2022)