Abstract
There is growing evidence from epidemiological studies that dietary protein may beneficially influence blood pressure (BP), but findings are inconclusive. We performed a meta-analysis of 29 observational studies and randomized controlled trials (RCTs) of dietary protein and types of protein in relation to BP or incident hypertension, published until January 2012. The analysis included eight cross-sectional studies (n=48 985), four prospective studies (n=11 761) and 17 RCTs (n=1449). A modest inverse association between total protein intake and BP (−0.20 mm Hg systolic (95% CI: −0.39, −0.01) per 25 g (∼1 s.d.)) was found in cross-sectional studies, but not in prospective studies (relative risk of 0.99 (95% CI: 0.96, 1.02)). For RCTs that used carbohydrate as a control treatment, the pooled BP effect was −2.11 mm Hg systolic (95% CI: −2.86, −1.37) for a weighed mean contrast in protein intake of 41 g per day. A non-significant inverse association of −0.52 mm Hg systolic (95% CI: −1.10, +0.05) per 11 g (∼1 s.d.) was found for plant protein in cross-sectional studies, whereas animal protein was not associated with BP. In prospective studies and RCTs, however, the associations of plant protein and animal protein with BP were broadly similar. These findings suggest that increasing the intake of protein at the expense of carbohydrates may have a beneficial effect on BP. The BP effect of specific types of protein remains to be established.
Similar content being viewed by others
Introduction
Elevated blood pressure (BP) is a major risk factor for cardiovascular diseases. In 2002, the World Health Organization estimated that about 62% of cerebrovascular disease and 49% of ischemic heart disease worldwide were attributable to suboptimal BP (that is, systolic BP levels >115 mm Hg).1, 2 Prevention of high BP by healthy lifestyle and diet, therefore, can have a substantial public health impact; it has been estimated that a population-wide reduction in systolic BP of only 2 mm Hg is expected to result in a 6% reduction in fatal stroke and a 4% reduction in fatal coronary heart disease.3
Some of the well-established measures to lower BP are weight reduction in overweight and obese individuals, reduced salt intake, moderation of alcohol intake (among those who drink) and an increased potassium intake.3, 4 In addition, data from the large DASH trial among 459 (pre)hypertensive adults showed that BP can be substantially reduced by a diet rich in fruits, vegetables and low-fat dairy products compared with a typical US diet, with reductions in systolic BP being −5.5 mm Hg in the total DASH population and −11.4 mm Hg in hypertensive participants.5 More recently, interest has grown in the influence of diet composition and macronutrient intake on BP. Whether total protein content of the diet and/or types of protein are important for human BP, however, is not clear.
In a previously published systematic review, we concluded that dietary protein could have a small beneficial effect on BP.6 Observational (mainly cross-sectional) data suggested a more beneficial role for plant protein than for animal protein. More data on dietary (types of) protein and BP have recently been published.7, 8, 9, 10, 11, 12, 13 We, therefore, performed a series of meta-analyses on total protein, plant protein and animal protein in relation to BP or incident hypertension, based on observational and trial data presented in the literature until January 2012.
Materials and methods
Study selection
For the systematic literature review that has recently been published,6 a systematic MEDLINE search (1 January 1966 to 1 June 2010) was performed. Search terms on dietary protein and BP or hypertension were used to search for words in title or abstract, and Medical Subject Headings (Supplementary Table S1 in the online issue for detailed query syntax). An additional manual search was performed using reference lists of original research and review articles. For the present meta-analysis, an updated secondary search was conducted until January 2012, using the same query syntax.
We selected any observational or intervention study that examined dietary protein in relation to BP in generally healthy adults. All titles, abstracts and full papers of potentially relevant studies were assessed for eligibility based on predefined inclusion and exclusion criteria. Papers were excluded (1) if data on exposure (total protein, plant protein and animal protein) or outcome (BP, hypertension) were not sufficiently reported; (2) if no estimate for the relationship between exposure and outcome was reported; and (3) if the exclusive effect of protein could not be calculated (for example, studies that focused on dietary patterns, soy combined with isoflavones, or no isocaloric macronutrient replacement in trials). Finally, we excluded studies based on biomarkers, because the biomarkers used were too heterogeneous. Moreover, there were insufficient numbers of studies (⩽3) to perform a meta-analysis on trials investigating plant protein versus animal protein, and to perform a meta-analysis on studies examining the BP effect of protein sources (for example, dairy protein, meat protein or grain protein). A flowchart of the screening and selection process is provided in the online issue (Supplementary Figure S1).
Statistical methods
From each included paper, we extracted data on protein intake, source of protein and BP values or estimated risk of hypertension according to a predefined standard form. In addition, we extracted data on design, country of study, number of participants, population characteristics (including initial BP, gender and age), dietary assessment method (food frequency questionnaire, 24-h recall, food diary), adjustment for confounders and measures of variation. Data were verified by two authors (ST, WAK). To allow better comparison of results from observational studies, we expressed associations in these studies by standard units of protein intake that correspond to ∼1 s.d. of protein intake in the Dutch population, that is, 25 g per day (3.5 en%) for total protein, 11 g per day (1.4 en%) for plant protein and 23 g per day (2.9 en%) for animal protein.14 For parallel trials, we calculated the net systolic BP change by subtracting change from baseline in the intervention group from that in the control group. For crossover trials, the net systolic BP change was calculated as the final systolic BP in the intervention period minus the final systolic BP in the control period.
We used STATA version 11.0 (StataCorp, College Station, TX, USA) for meta-analysis using the METAN command. All statistical tests were two-sided with α=0.05. Forest plots were created per study type for total protein, plant protein and animal protein in relation to systolic BP difference or hypertension incidence. For observational studies, we used the results from the main multivariable model that included most confounders. Between-study heterogeneity was assessed using the I2 statistic,15 which expresses the percentage of variation attributable to between-study heterogeneity. An I2-value ⩾50% was considered to indicate substantial heterogeneity between studies.
For the meta-analysis on randomized trials with a carbohydrate control, we also conducted a meta-regression analysis on protein dose and study duration using the GLST command, with the generalized least-squares method for trend estimation of summarized dose–response data, based on the Greenland and Longnecker method.16 Furthermore, to check whether systolic BP response to dietary protein was modified by subject characteristics, we conducted a meta-regression analysis on age, gender (% males), body mass index and initial systolic BP level.
Results
Study characteristics
An overview of the eight cross-sectional studies9, 17, 18, 19, 20, 21, 22, 23 included in our meta-analysis is given in Table 1. In total, data from 48 985 individuals (from six cross-sectional studies) were available for the analysis on total dietary protein and systolic BP. The mean (±s.d.) age of the study populations was 47±6 years (range: 38–53 years), mean baseline systolic BP was 124±11 mm Hg (range: 107–135 mm Hg) and mean protein intake was 82±7 g per day (range: 74–91 g per day).
Table 2 shows the characteristics of the four prospective studies7, 8, 20, 24 on protein intake and incident hypertension. In total, data from 11 761 individuals (from three prospective cohort studies) were available for the analysis on total dietary protein and hypertension incidence. The mean age of the study populations was 48±15 years (range: 36–65 years), mean baseline systolic BP was 120±3 mm Hg, mean habitual total protein intake was 16±2 en% and follow-up lasted 2–10 years.
An overview of 17 randomized controlled trials (RCTs)10, 11, 12, 13, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36 on protein intake and BP is given in Table 3. The number of participants in these trials ranged from 17 to 273. A total of 1449 individuals were included. The mean age of the trial populations was 50±10 years (range: 31–74 years), the mean baseline systolic BP was 128±10 mm Hg (range: 112–144 mm Hg), the mean difference in protein intake between intervention groups was 48±15 g per day (range: 26–74 g per day), and the trials had a mean duration of 17±24 weeks (range: 3–104 weeks).
Total dietary protein
In the six cross-sectional studies that were available for investigating the association between total protein and BP (48 985 individuals), the combined results showed a significant, but small, inverse association with a pooled estimate of −0.20 mm Hg systolic (95% CI: −0.39, −0.01) per 25 g (∼1 s.d.) of total protein intake (Figure 1). We observed no evidence for statistical heterogeneity (I2=3.1%, P=0.40). In our meta-analysis including data from three prospective studies (11 761 participants), total protein intake was not associated with incidence of hypertension with a pooled HR of 0.99 (95% CI: 0.96, 1.02, Figure 2) and no evidence for statistical heterogeneity (I2=0.0%, P=0.53).
Fully adjusted difference (ES, 95% CI) in systolic BP with consumption of 25 g (∼1 s.d.) higher total protein intake in six cross-sectional studies (for details of the studies see Table 1). The I2-value represents the proportion of variability in point estimates attributable to between-study heterogeneity.15 A full colour version of this figure is available at the Journal of Human Hypertension journal online.
Fully adjusted relative risk of hypertension with 25 g (∼1 s.d.) higher total protein intake in three longitudinal studies (for details of the studies see Table 2). The I2-value represents the proportion of variability in point estimates attributable to between-study heterogeneity.15 A full colour version of this figure is available at the Journal of Human Hypertension journal online.
In 14 intervention studies (1208 individuals) that used carbohydrate as a control treatment, the pooled BP effect was −2.11 mm Hg systolic (95% CI: −2.86, −1.37, Figure 3) for a weighed mean contrast in protein intake of 41 g per day and no signs of statistical heterogeneity (I2=0.0%, P=0.98). Meta-regression analyses showed no association of protein dose or study duration with BP response (Table 4). Moreover, the BP response to dietary protein was not modified by subject characteristics, such as age, gender, baseline body mass index and initial systolic BP. We identified three trials with a fat control (mainly monounsaturated fatty acids, Table 3) yielding a pooled estimate of −0.04 mm Hg (95% CI: −2.20, +2.12) and no statistical heterogeneity (I2=36.2%, P=0.21, data not shown). The type of intervention, that is, increase in protein intake by means of diet versus supplements, did not influence the BP effect (Supplementary Figure S2).
Net change (ES, 95% CI) in systolic BP with consumption of protein compared with carbohydrates in 14 randomized controlled trials (for details of the studies see Table 3). The I2-value represents the proportion of variability in point estimates attributable to between-study heterogeneity.15 In the studies of Pal et al.12 and He et al.,10 two intervention arms were included that were compared with the same control group. In the study of Meckling et al.,29 two intervention arms were included that were each compared with their own control group (intervention with and without exercise in both intervention and control group). A full colour version of this figure is available at the Journal of Human Hypertension journal online.
Plant protein versus animal protein
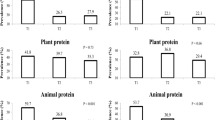
Our meta-analysis including seven cross-sectional studies (42 938 participants) showed a small, but non-significant, inverse association of −0.52 mm Hg systolic per 11 g (∼1 s.d.) for plant protein (95% CI: −1.10, +0.05, Supplementary Figure S3), whereas animal protein (five cross-sectional studies, 41 496 participants) was not associated with BP (Supplementary Figure S4). We observed substantial heterogeneity for plant protein (I2=75%, P=0.01) and animal protein (I2=55%, P=0.07). This was mainly because of the study of Umesawa et al.21 in 7585 Japanese adults, which showed an inverse association with BP for animal protein and a direct association for plant protein. After exclusion of that study, heterogeneity was strongly reduced to 17% for plant protein (P=0.31) and 0% for animal protein (P=0.61). In addition, pooled estimates changed towards a larger difference between protein types, that is, −0.73 mm Hg systolic per s.d. (95% CI: −1.08, −0.38) for plant protein and +0.24 mm Hg (95% CI: −0.09, +0.57) for animal protein.
In our meta-analysis including data from four prospective studies (12 571 participants), incident hypertension was not related to plant protein (HR: 0.96, 95% CI: 0.89, 1.03; Supplementary Figure S5) or animal protein (HR: 0.98, 95% CI: 0.95, 1.02; Supplementary Figure S6). For these analyses, we observed statistical heterogeneity for plant protein (I2=63.9%, P=0.04), but not for animal protein (I2=0.0%, P=0.99).
When analyzing trials in strata of plant protein and animal protein, there was no significant difference between the BP effects of protein from plant and animal sources. Our meta-analysis on plant protein included data from three trials (327 individuals) and provided a pooled estimate of −1.95 mm Hg systolic (95% CI: −3.21, −0.69) without evidence for statistical heterogeneity (Supplementary Figure S7). The pooled estimate for animal protein including data from four trials (574 individuals) was −2.20 mm Hg systolic (95% CI: −3.36, −1.03) without evidence for statistical heterogeneity.
Discussion
The totality of evidence, especially from trials, indicates that dietary protein may have a beneficial effect on BP if consumed instead of carbohydrates, although we did not observe a dose–response relationship. There was no clear differential effect on BP for plant protein or animal protein.
Total dietary protein
In the present meta-analysis, cross-sectional studies showed a small beneficial association of total protein with BP, whereas this was not confirmed in prospective cohort studies. This discrepancy may be explained by lower BP levels in prospective population-based studies owing to the exclusion of hypertensive participants at baseline. Moreover, small associations in these studies may have been missed because of using a dichotomous outcome, that is, incident hypertension defined as BP⩾140/90 mm Hg or initiation of antihypertensive medication. This approach has the advantage that participants who started using medication during follow-up could be retained in the analysis, which reduced the risk of bias. A disadvantage, however, is that BP changes closely around the cut-off point are emphasized, whereas changes further away from the cut-off point are ignored. In addition, small BP differences may have been missed.
Trials with a carbohydrate control provided stronger evidence for a beneficial effect of dietary protein on BP than observational studies did, which may be partly attributable to the inclusion of more vulnerable individuals; for example, those with (pre)hypertension. In addition, in these trials supplements or fully controlled diets were mostly used, and attenuation of BP effects due to exposure misclassification does not occur. This is in contrast to observational studies in which protein intake is measured using memory-based methods. Finally, the contrast in protein intake was larger in trials with a weighed mean contrast in intake of 41 g per day (range: 26–74 g per day) versus a contrast of 25 g per day (∼1 s.d.) in observational studies. The relatively high doses in trials may also have masked a dose–response relationship with BP.
In isocaloric conditions, a BP effect after intake of protein will be relative to the intake of fat or carbohydrates, or both. The results of our meta-analysis indicate a stronger BP effect of protein when exchanged for carbohydrates rather than for fat (mainly monounsaturated fatty acids). A decreased carbohydrate intake, rather than an increased protein intake, may therefore also be involved in BP reduction. BP effects were more pronounced in trials using glucose or maltodextrin as a control compared with trials that were diet-based and had a mixture of carbohydrates in the control diet. The increase of protein at the expense of carbohydrates (especially ‘fast’ carbohydrates like sucrose and maltodextrin) reduces the glycemic index of diets, which may result in an attenuated insulin response. As there is some evidence for an unfavorable effect of insulin on BP, this may explain a BP-lowering effect of such diets.37 However, it cannot be excluded that the more controlled dose in the supplement-based trials, rather than the type of carbohydrates, accounted for the stronger BP effects. In observational studies it was not clear which macronutrients were exchanged, which may explain why no association was found between protein intake and BP.
Plant protein versus animal protein
Early observational studies showed an inverse association for plant protein, but not for animal protein, with BP.20, 23, 24, 38 In our meta-analysis based on cross-sectional studies, we observed a small and non-significant inverse association of −0.52 mm Hg systolic per 11 g plant protein with substantial heterogeneity (I2=75%, P=0.01). This heterogeneity was mainly because of the study of Umesawa et al.21 in 7585 Japanese adults, which showed an inverse association with BP for animal protein and a direct association for plant protein. After exclusion of that study, the pooled estimate for plant protein became larger and significant (that is, −0.73 mm Hg, 95% CI: −1.08, −0.38). No association was observed for animal protein. The deviant estimates in the study of Umesawa et al.21 may be attributable to the eating habits in Japan, where ∼24% of animal protein intake comes from fish,39 whereas in China and in western countries ∼6% of animal protein intake is derived from fish.39 Fish may be more beneficial to BP than meat,40 which may explain the inverse association between animal protein and BP in the study of Umesawa et al.21 A more beneficial influence of plant protein compared with animal protein on BP may, therefore, only be present in countries with a more westernized diet. Residual confounding from factors that are strongly correlated to intake of plant protein or animal protein cannot be excluded. Individuals in western countries who consume a diet rich in plant protein, probably have a healthier lifestyle than those who consume much animal protein. Although in most observational studies adjustments were made for nutrients that are indicators of a healthy lifestyle (for example, dietary fiber and potassium), incomplete adjustment for lifestyle factors or dietary factors, such as polyphenols that are abundant in plant food, may have resulted in residual confounding. On the other hand, in the meta-analysis based on prospective studies in western countries, plant protein was not related to incident hypertension (HR: 0.96, 95% CI: 0.89, 1.03).
To gain more insight in the BP effect of plant protein and animal protein, we conducted a meta-analysis of trials with a carbohydrate control, stratified by plant protein or animal protein in the intervention diet. We did not find a different effect between trials with protein interventions from plant sources or animal sources (data not shown). The protein source in all plant protein trials was soy, and results cannot be generalized to total plant protein. In a western diet, soy protein makes only a small contribution to total intake of plant protein (∼2.5% in the Netherlands, unpublished data). It has been estimated that grain protein contributes ∼53% to plant protein intake in the Netherlands, with other important sources being potatoes (10%), vegetables (8%) and fruits (10%). Up to date, no trial has been conducted that examined the BP effect of dietary plant protein originating from these sources compared with a balanced mix of animal protein.
In conclusion, the present meta-analysis indicates a beneficial effect of total dietary protein on BP when consumed instead of carbohydrates. In 14 trials that used carbohydrates as a control treatment, the pooled BP effect was −2.11 mm Hg systolic for a weighed mean contrast in protein intake of 41 g per day. This contrast in protein intake is larger than in observational studies (s.d. ∼25 g per day), which suggests that the BP effect in trials is likely to be higher than in the general population. However, a small BP decrease may still have a substantial public health impact. It has been estimated that a population-wide reduction in systolic BP of only 2 mm Hg is expected to result in a 6% reduction in fatal stroke, and a 4% reduction in fatal coronary heart disease.3 In the present meta-analysis, no difference in BP effect for plant protein or animal protein was observed. BP trials of protein from different sources that reflect habitual intakes in western populations are warranted. For now, a prudent diet with adequate amounts of dietary protein at the expense of carbohydrates may be recommended for the prevention of hypertension.

References
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42 (6): 1206–1252.
Reducing Risks, Promoting Healthy Life. World Health Report 2002 2002.
Whelton PK, He J, Appel LJ, Cutler JA, Havas S, Kotchen TA et al. Primary prevention of hypertension: clinical and public health advisory from the National High Blood Pressure Education Program. JAMA 2002; 288 (15): 1882–1888.
Appel LJ, Brands MW, Daniels SR, Karanja N, Elmer PJ, Sacks FM . Dietary approaches to prevent and treat hypertension: a scientific statement from the American Heart Association. Hypertension 2006; 47 (2): 296–308.
Appel LJ, Moore TJ, Obarzanek E, Vollmer WM, Svetkey LP, Sacks FM et al. A clinical trial of the effects of dietary patterns on blood pressure. N Engl J Med 1997; 336 (16): 1117–1124.
Altorf-van der Kuil W, Engberink MF, Brink EJ, van Baak MA, Bakker SJL, Navis G et al. Dietary protein and blood pressure: a systematic review. PLoS ONE 2010; 5 (8): e12102.
Altorf-van der Kuil W, Engberink MF, Geleijnse JM, Boer JMA, Verschuren WMM . Sources of dietary protein and risk of hypertension in a general Dutch population. Br J Nutr 2012; 108 (10): 1897–1903.
Altorf-van der Kuil W, Engberink MF, van Rooij FJ, Hofman A, Van’t Veer P, Witteman JC et al. Dietary protein and risk of hypertension in a Dutch older population: the Rotterdam study. J Hypertens 2010; 28 (12): 2394–2400.
Altorf-van der Kuil W, Engberink MF, Vedder MM, Boer JMA, Verschuren WMM, Geleijnse JM . Sources of dietary protein in relation to blood pressure in a general Dutch population. PLoS ONE 2012; 7 (2): e30582.
He J, Wofford MR, Reynolds K, Chen J, Chen C, Myers L et al. Effect of dietary protein supplementation on blood pressure: a randomized, controlled trial. Circulation 2011; 124: 589–595.
Larsen RN, Mann NJ, Maclean E, Shaw JE . The effect of high-protein, low-carbohydrate diets in the treatment of type 2 diabetes: a 12 month randomised controlled trial. Diabetologia 2011; 54 (4): 731–740.
Pal S, Ellis V . The chronic effects of whey proteins on blood pressure, vascular function, and inflammatory markers in overweight individuals. Obesity 2010; 18 (7): 1354–1359.
Teunissen-Beekman KFM, Dopheide J, Geleijnse JM, Bakker SJL, Brink EJ, De Leeuw PW et al. Protein supplementation lowers blood pressure in overweight adults: effect of dietary proteins on blood pressure (PROPRES), a randomized trial. Am J Clin Nutr 2012; 95 (4): 966–971.
Voedingscentrum. Zo eet Nederland, Resultaten van de voedselconsumptiepeiling 1997–1998 (Dutch food consumption survey of 1997–1998). Netherlands Nutrition Centre: The Hague, 1998.
Higgins JP, Thompson SG . Quantifying heterogeneity in a meta-analysis. Stat Med 2002; 21 (11): 1539–1558.
Greenland S, Longnecker MP . Methods for trend estimation from summarized dose-response data, with applications to meta-analysis. Am J Epidemiol 1992; 135 (11): 1301–1309.
He J, Klag MJ, Whelton PK, Chen JY, Qian MC, He GQ . Dietary macronutrients and blood pressure in southwestern China. J Hypertens 1995; 13 (11): 1267–1274.
Stamler J, Caggiula A, Grandits GA, Kjelsberg M, Cutler JA . Relationship to blood pressure of combinations of dietary macronutrients. Findings of the Multiple Risk Factor Intervention Trial (MRFIT). Circulation 1996; 94 (10): 2417–2423.
Masala G, Bendinelli B, Versari D, Saieva C, Ceroti M, Santagiuliana F et al. Anthropometric and dietary determinants of blood pressure in over 7000 Mediterranean women: the European Prospective Investigation into Cancer and Nutrition-Florence cohort. J Hypertens 2008; 26 (11): 2112–2120.
Wang YF, Yancy WY, Yu D, Champagne C, Appel LJ, Lin PH . The relationship between dietary protein intake and blood pressure: results from the PREMIER study. J Hum Hypertens 2008; 22 (11): 745–754.
Umesawa M, Sato S, Imano H, Kitamura A, Shimamoto T, Yamagishi K et al. Relations between protein intake and blood pressure in Japanese men and women: the Circulatory Risk in Communities Study (CIRCS). Am J Clin Nutr 2009; 90 (2): 377–384.
Joffres MR, Reed DM, Yano K . Relationship of magnesium intake and other dietary factors to blood pressure: the Honolulu heart study. Am J Clin Nutr 1987; 45 (2): 469–475.
Elliott P, Stamler J, Dyer AR, Appel L, Dennis B, Kesteloot H et al. Association between protein intake and blood pressure: the INTERMAP Study. Arch Intern Med 2006; 166 (1): 79–87.
Alonso A, Beunza JJ, Bes-Rastrollo M, Pajares RM, Martinez-Gonzalez MA . Vegetable protein and fiber from cereal are inversely associated with the risk of hypertension in a Spanish cohort. Arch Med Res 2006; 37 (6): 778–786.
Sacks FM, Wood PG, Kass EH . Stability of blood pressure in vegetarians receiving dietary protein supplements. Hypertension 1984; 6 (2 Part 1): 199–201.
Appel LJ, Sacks FM, Carey VJ, Obarzanek E, Swain JF, Miller ER et al. Effects of protein, monounsaturated fat, and carbohydrate intake on blood pressure and serum lipids: results of the OmniHeart randomized trial. JAMA 2005; 294 (19): 2455–2464.
Hodgson JM, Burke V, Beilin LJ, Puddey IB . Partial substitution of carbohydrate intake with protein intake from lean red meat lowers blood pressure in hypertensive persons. Am J Clin Nutr 2006; 83 (4): 780–787.
Hendler R, Bonde AA . Very-low-calorie diets with high and low protein content: impact on triiodothyronine, energy expenditure, and nitrogen balance. Am J Clin Nutr 1988; 48 (5): 1239–1247.
Meckling KA, Sherfey R . A randomized trial of a hypocaloric high-protein diet, with and without exercise, on weight loss, fitness, and markers of the Metabolic Syndrome in overweight and obese women. Appl Physiol Nutr Metab 2007; 32 (4): 743–752.
Burke V, Hodgson JM, Beilin LJ, Giangiulioi N, Rogers P, Puddey IB . Dietary protein and soluble fiber reduce ambulatory blood pressure in treated hypertensives. Hypertension 2001; 38 (4): 821–826.
Leidy HJ, Carnell NS, Mattes RD, Campbell WW . Higher protein intake preserves lean mass and satiety with weight loss in pre-obese and obese women. Obesity (Silver Spring) 2007; 15 (2): 421–429.
Brinkworth GD, Noakes M, Parker B, Foster P, Clifton PM . Long-term effects of advice to consume a high-protein, low-fat diet, rather than a conventional weight-loss diet, in obese adults with type 2 diabetes: one-year follow-up of a randomised trial. Diabetologia 2004; 47 (10): 1677–1686.
Delbridge EA, Prendergast LA, Pritchard JE, Proietto J . One-year weight maintenance after significant weight loss in healthy overweight and obese subjects: does diet composition matter? Am J Clin Nutr 2009; 90 (5): 1203–1214.
Hodgson JM, Zhu K, Lewis JR, Kerr D, Meng X, Solah V et al. Long-term effects of a protein-enriched diet on blood pressure in older women. Br J Nutr 2011; 13: 1–9.
Papakonstantinou E, Triantafillidou D, Panagiotakos DB, Koutsovasilis A, Saliaris M, Manolis A et al. A high-protein low-fat diet is more effective in improving blood pressure and triglycerides in calorie-restricted obese individuals with newly diagnosed type 2 diabetes. Eur J Clin Nutr 2010; 64 (6): 595–602.
Hochstenbach-Waelen A, Westerterp KR, Soenen S, Westerterp-Plantenga MS . No long-term weight maintenance effects of gelatin in a supra-sustained protein diet. Physiol Behav 2010; 101 (2): 237–244.
Tiwari S, Riazi S, Ecelbarger CA . Insulin’s impact on renal sodium transport and blood pressure in health, obesity, and diabetes. Am J Physiol Renal Physiol 2007; 293 (4): F974–F984.
Stamler J, Liu K, Ruth KJ, Pryer J, Greenland P . Eight-year blood pressure change in middle-aged men: relationship to multiple nutrients. Hypertension 2002; 39 (5): 1000–1006.
FAO Statistics Division. Available from http://faostat.fao.org/.
Panagiotakos DB, Zeimbekis A, Boutziouka V, Economou M, Kourlaba G, Toutouzas P et al. Long-term fish intake is associated with better lipid profile, arterial blood pressure, and blood glucose levels in elderly people from Mediterranean islands (MEDIS Epidemiological Study). Med Sci Monit 2007; 13 (7): CR307–CR312.
Acknowledgements
This study was supported by the Top Institute Food and Nutrition, Wageningen, The Netherlands, a public private partnership of science, industry and government (www.tifn.nl).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Journal of Human Hypertension website
Supplementary information
Rights and permissions
About this article
Cite this article
Tielemans, S., Altorf-van der Kuil, W., Engberink, M. et al. Intake of total protein, plant protein and animal protein in relation to blood pressure: a meta-analysis of observational and intervention studies. J Hum Hypertens 27, 564–571 (2013). https://doi.org/10.1038/jhh.2013.16
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2013.16
Keywords
This article is cited by
-
Renal and dietary factors associated with hypertension in a setting of disadvantage in rural India
Journal of Human Hypertension (2021)
-
The long-term association of different dietary protein sources with metabolic syndrome
Scientific Reports (2021)
-
Impact of a high-protein diet during lactation on milk composition and offspring in a pig model
European Journal of Nutrition (2019)
-
Fruit and vegetables consumption and incident hypertension: dose–response meta-analysis of prospective cohort studies
Journal of Human Hypertension (2016)
-
Dietary Approaches to Prevent Hypertension
Current Hypertension Reports (2013)