Abstract
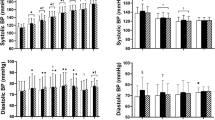
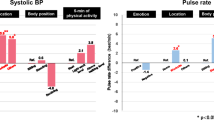
It is accepted that accuracy of auscultatory blood pressure (BP) measurement is influenced by measurement conditions. However, there is little comparative quantitative clinical data. The aim of this study was to provide these data. Auscultatory systolic and diastolic BPs (SBPs and DBPs) were measured in 111 healthy subjects under five different conditions (resting, deeper breathing, talking, head and arm movement). The measurement sequence was randomized, and repeated three times. BPs and their within-subject variabilities were compared with resting values. SBP and DBP changed significantly in comparison with the resting condition: decreasing by 4.4 and 4.8 mm Hg, respectively, with deeper breathing (both P<0.001), increasing by 3.7 and 5.0 mm Hg with opposite arm movement, and increasing by 5.3 and 6.2 mm Hg with talking (all P<0.001). The mean differences between deeper breathing and talking were 9.7 and 11.0 mm Hg for SBP and DBP. The within-subject variability for repeat measurement of SBP and DBP under resting condition were 3.7 and 3.2 mm Hg and increased for non-resting conditions (all P<0.05, except for DBP while talking). We have shown that measurement conditions significantly influence manual auscultatory BPs and their measurement variabilities, and we provide quantitative data to allow comparison of the effects.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Jones DW, Appel LJ, Sheps SG, Roccella EJ, Lenfant C . Measuring blood pressure accurately: new and persistent challenges. JAMA 2003; 289: 1027–1030.
Daly J, Speedy S, Jackson D . Contexts of Nursing. Elsevier: Australia, 2009, pp 227.
Beevers G, Lip GYH, O’Brien E . ABC of hypertension: blood pressure measurement: part I-sphygmomanometry: artefacts common to all techniques. BMJ 2001; 322: 981–985.
Netea RT, Lenders JWM, Smits P, Thien T . Influence of body and arm position on blood pressure recordings: an overview. J Hypertens 2003; 21: 237–241.
O’Brien E, Asmar R, Beilin L, Imai Y, Mallion JM, Mancia G et al. European Society of Hypertension recommendations for conventional, ambulatory and home blood pressure measurement. J Hypertens 2003; 21: 821–848.
Le Pailleur C, Helft G, Landais P, Montgermont P, Feder JM, Metzger JP et al. The effects of talking, reading, and silence on the ‘white coat’ phenomenon in hypertensive patients. Am J Hypertens 1998; 11: 203–207.
Le Pailleur C, Montgermont P, Feder JM, Metzger JP, Vacheron A . Talking effect and ‘white coat’ effect in hypertensive patients: physical effort or emotional content? Behav Med 2001; 26: 149–157.
Smith FE, Haigh A, Wild J, Bowers EJ, King S, Allen J et al. Study of the causes of blood pressure variability during manual sphygmomanometer measurement. IFMBE Proc 2005; 9: 95–96.
Jagomägi K, Raamat R, Talts J, Länsimies E, Jurvelin J . Effect of deep breathing test on finger blood pressure. Blood Press Monit 2003; 8: 211–214.
Bowers EJ, Murray A . Interaction between cardiac beat-to-beat interval changes and systolic blood pressure changes. Clin Auton Res 2004; 14: 92–98.
Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves J, Hill MN et al. Recommendations for blood pressure measurement in humans and experimental animals. Part 1: blood pressure measurement in humans. A statement for professionals from the subcommittee of professional and public education of the American Heart Association Council on high blood pressure research. Hypertension 2005; 45: 142–161.
Grossman E, Grossman A, Schein MH, Zimlichman R, Gavish B . Breathing-control lowers blood pressure. J Hum Hypertens 2001; 15: 263–269.
Liehr P . Uncovering a hidden language: the effects of listening and talking on blood pressure and heart rate. Arch Psychiatr Nurs 1992; 6: 306–311.
Parati G, Carretta R . Device-guided slow breathing as a non-pharmacological approach to antihypertensive treatment: efficacy, problems and perspectives. J Hypertens 2007; 25: 57–61.
Graves JW, Tibor M, Murtagh B, Klein L, Sheps SG . The Accoson Greenlight 300TM, the first non-automated mercury free blood pressure device to pass the International Protocol for blood pressure measuring devices in adults. Blood Press Monit 2003; 9: 13–17.
Williams B, Poulter NR, Brown MJ, Davis M, McInnes GT, Potter JF et al. British hypertension society. Guidelines for management of hypertension: report of the fourth working party of the British hypertension society. J Hum Hypertens 2004; 18: 139–185.
Bernardi L, Porta C, Spicuzza L . Slow breathing increases arterial baroreflex sensitivity in patients with chronic heart failure. Circulation 2002; 105: 143–145.
Rosenthal T, Alter A, Peleg E, Gavish B . Device-guided breathing exercises reduce blood pressure: ambulatory and home measurements. Am J Hypertens 2001; 14: 74–76.
Meles E, Giannattasio C, Failla M, Gentile G, Capra A, Mancia G . Non-pharmacological treatment of hypertension by respiratory exercise in the home setting. Am J Hypertens 2004; 17: 370–374.
Laude D, Goldman M, Escourrou P, Elghozi JL . Effect of breathing pattern on blood pressure and heart rate oscillations in humans. Clin Exp Pharmacol Physiol 1993; 20: 619–626.
Schulze MB, Kroke A, Bergmann MM, Boeing H . Differences of blood pressure estimates between consecutive measurements on one occasion: implications for inter-study comparability of epidemiologic studies. Eur J Epidemiol 2000; 16: 891–898.
Acknowledgements
We acknowledge the funding support from the Engineering and Physical Sciences Research Council (EPSRC). Dr Dingchang Zheng and Roberto Giovannini are funded by the Engineering and Physical Sciences Research Council.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zheng, D., Giovannini, R. & Murray, A. Effect of respiration, talking and small body movements on blood pressure measurement. J Hum Hypertens 26, 458–462 (2012). https://doi.org/10.1038/jhh.2011.53
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2011.53
Keywords
This article is cited by
-
Effect of respiratory pattern on automated clinical blood pressure measurement: an observational study with normotensive subjects
Clinical Hypertension (2017)
-
Respiratory modulation of oscillometric cuff pressure pulses and Korotkoff sounds during clinical blood pressure measurement in healthy adults
BioMedical Engineering OnLine (2016)
-
Effect of respiration on Korotkoff sounds and oscillometric cuff pressure pulses during blood pressure measurement
Medical & Biological Engineering & Computing (2014)