Abstract
We conducted a survey of malaria diagnoses and glucose-6-phosphate dehydrogenase (G6PD) testing in remote areas of Cambodia. Blood specimens from 670 people were collected by the finger-prick method. Of these people, 24.9% were found to have malaria, and 7.0% of people were G6PD deficient. In the Khmer, the largest ethnical population in Cambodia, the G6PD deficiency rate of males was 12.6% (25/199) whereas the rates in the minorities of the Tum Pun and the Cha Ray were 1.1% (1/93) and 3.2% (2/63), respectively. Of the G6PD-deficient subjects, 97.9% (46/47) were G6PD Viangchan (871G>A), and only one case (2.1%) was G6PD Union (1360C>T). Since G6PD Mahidol (487G>A) is common in Myanmar according to our previous study, the current finding suggests that the Cambodian population is derived from homogeneous ancestries and is different from the Myanmar population. All G6PD Viangchan cases were linked to two other mutations of 1311C>T and IVS-11 nt93T>C in the G6PD gene.
Similar content being viewed by others
Introduction
We have introduced rapid diagnosis methods for malaria (Kawamoto and Billingsley 1992) and glucose-6-phosphate dehydrogenase (G6PD) deficiency (Hirono et al. 1998; Tantular and Kawamoto 2003) to malaria endemic areas in Southeast Asian countries. Using these methods, patients are notified of the results of blood examination within 30 min and are able to receive antimalarial medicine, including primaquine (Tantular et al. 1999; Jalloh et al. 2004). Primaquine can kill gametocytes, the sexual stage of malaria parasites, which are the cause of malaria transmission to mosquitoes. Once primaquine is introduced in a community, new malaria cases decrease because the number of malaria-infective mosquitoes decreases (Matsuoka et al. 1987). However, when G6PD-deficient persons take primaquine, a hemolytic attack can occur. Without G6PD, erythrocytes cannot prepare a sufficient amount of reduced pyridine nucleotide, and reduced glutathione and cannot prevent oxidant attack by primaquine. Thus, primaquine should not be administered to malaria patients before confirming their G6PD activity status.
G6PD deficiency is one of the most frequent hereditary abnormalities. The G6PD gene exists on the X-chromosome distributed in 13 exons (Chen et al. 1991). Almost all G6PD deficiencies are caused by one amino-acid change caused by a point mutation of the genomic DNA, and 140 molecular variants of the G6PD genotype have been identified (Beutler and Vulliamy 2002). The incidence of G6PD deficiency is said to be high in malaria-endemic areas. More than 10% of the male population is G6PD deficient in African and Southeast Asian countries where malignant malaria Plasmodium falciparum is endemic. In contrast, in Japan, northern China and north European countries, where falciparum malaria is historically not endemic, the incidence of G6PD deficiency is less than 0.1%.
During the surveys of malaria and G6PD deficiency, we collected G6PD-deficient blood samples after receiving informed consent and read the genomic DNA of G6PD. We have described G6PD variants in various countries or ethnic groups in Asian countries (Iwai et al. 2001; Matsuoka et al. 2003a, b, 2004). In Cambodia, the rapid tests for malaria and G6PD activity have not been introduced yet. We intended to introduce these methods in remote areas in Cambodia. We also tried to obtain genomic information on the G6PD molecule. This report is the first description of G6PD variants in Cambodian people.
Materials and methods
Between 2003 and 2004, surveys were conducted by the National Malaria Center, Cambodia, at 12 villages in three provinces in Cambodia. These were Battambang Province, Kampot Province, and Rattanakiri Province. A small test unit was opened at each site, and local staff announced to the residents that we would perform rapid, on-site examinations for malaria and G6PD activity. This study was approved by the Department of Health, Cambodia.
People were first registered by names, ages, genders, and ethnicity. Next, three drops of blood were collected from the fingertip: one for malaria diagnosis, one for hemoglobin concentration, and one for G6PD test. Malaria was diagnosed by the acridine orange staining method (Kawamoto and Billingsley 1992), and hemoglobin concentration was measured using a battery-powered HemoCue machine (Angelhorm, Sweden). For G6PD activity test, we used the G6PD Assay Kit (Dojindo Laboratories, Tokyo, Japan). Five microliters of blood was added to a G6PD test tube containing 800 μl of sample reagent. The contents were vigorously mixed to destroy red blood cells in the tube and incubated for 20 min at ambient temperature. When G6PD activity was normal, orange color appeared and became dark. When G6PD activity was deficient, the faint red color of hemoglobin did not change during the incubation time. The reaction was stopped by adding 10 μl of 1 N HCl. Judgment was made by comparison of the color with positive and negative control tubes (Tantular and Kawamoto 2003).
Anemia is a potential cause of misdiagnosis of G6PD deficiency. In this field study, we measured hemoglobin concentration as well as G6PD activity. When we met a case showing low G6PD activity and low hemoglobin level (less than 8.0 g/dl), we tested for G6PD activity again using an increased amount of blood in the G6PD test tube. For instance, 10 μl of blood was added when the Hb level was 6.0 g/dl; 7.5 μl of blood was added when the Hb level was 8.0 g/dl. With this alteration, we could divide individuals into (1) full activity of G6PD, (2) partial deficiency group, and (3) complete deficiency group.
All results were reported to each individual within 30 min after taking blood. When malaria patients were found, we gave them artesunate and mefloquine. We did not give primaquine to malaria patients in these surveys because the national health policy of Cambodia does not currently allow administration of primaquine to malaria patients.
When we found a person whose G6PD activity was low, we asked the person if we could take 0.2 ml of venous blood to read the G6PD gene. We explained the purpose of the investigation and received informed consent. Blood samples collected were stored at 4°C and brought back to Japan, and G6PD activity was confirmed by another G6PD test developed by Fujii et al. (1984). The DNA sequence of G6PD was then identified. Since genomic G6PD consists of 13 exons, we prepared primers for each exon (Hirono et al. 1994), amplified the exon by PCR, and read the DNA sequence (ABI PRISM 310; PE Biosystems, CT, USA). Both strands of each exon were sequenced.
Results and discussion
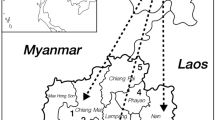
We conducted malaria diagnosis and treatment with G6PD activity testing in remote areas of Cambodia. Blood samples from 670 people were collected by the finger-prick method at 13 sites in four provinces (Fig. 1). Among those tested, we found 167 malaria cases and 47 cases of G6PD deficiency (Table 1). We detected 29 complete G6PD-deficient cases among 360 males (8.1%) and two completely and 16 partially G6PD-deficient cases among 310 females (5.8%). In the Khmer, representing more than 90% of the population of Cambodia, the G6PD deficiency rate among males was 12.6% (25/199) and that among females 13.8% (17/123).
Distribution and frequencies of glucose-6-phosphate dehydrogenase (G6PD) variants in Southeast Asian countries. Each number indicates the number of G6PD-deficient cases confirmed by sequence analysis. Data of Laos, Myanmar, are from our previous reports (Iwai et al. 2001; Matsuoka et al. 2004). Data of Thailand are from the report by Nuchprayoon et al. (2002)
Partial G6PD deficiency in females was difficult to find because anemia is common in malaria-endemic areas. Anemic cases show partial G6PD deficiency because the number of red blood cells in the sample volume (5 μl) in an anemic case is lower than that in a nonanemic case. Thus, we tried to adjust the sample volume by measuring the hemoglobin level. We measured hemoglobin levels in each person. When we met a subject who showed low G6PD activity and low hemoglobin level (less than 8.0 g/dl), we tested her G6PD activity one more time, increasing the amount of blood added to the G6PD test tube. In this way, we could separate the group that showed G6PD deficiency due to anemia and succeeded in diagnosing partial deficiency in the female group.
The G6PD deficiency rates in males in malaria-endemic areas were 10.5% (45/430) in Myanmar and 3.9% (25/648) in Indonesia (Jalloh et al. 2004). Compared with these rates, the rate of 8.1% (29/331) in Cambodian males was reasonable. Comparing ethnic groups, 12.6% (25/199) in Khmer males was statistically higher whereas the rates in minorities of the Tum Pun and the Cha Ray were 1.1% (1/93) and 3.2% (2/63), respectively (P<0.01). Everett et al. (1977) reported that the rate of G6PD deficiency in Khmer males was 14.2% (15/106). Compared with their report, our result of 12.6% was reasonable. We cannot explain at present why the rates of G6PD deficiency in the Tum Pun and the Cha Ray were low. There is a hypothesis that the rate of G6PD deficiency becomes high in places where falciparum malaria is endemic (Ruwende et al. 1995). If this hypothesis is correct, the Tum Pun and the Cha Ray perhaps moved from malaria-free areas in recent years. Or perhaps falciparum malaria was introduced in their habitant areas in the recent years.
During these activities, we received informed consent from G6PD-deficient persons to analyze their G6PD gene. We analyzed 47 cases and found that 46 (97.9%) were G6PD Viangchan (871G>A) (Table 1). These results indicate that the Cambodian population was derived from a homogeneous ancestry. Among 47 cases of G6PD Viangchan, 42 were Khmer, two were Tum Pun, two were Cha Ray, and one was Indian. This is the first case of G6PD Viangchan found from an Indian. He did not know when his ancestor moved from India to Cambodia or whether one of his ancestors married with a Khmer person. We found one case of G6PD Union heterozygote (1360C>C/T). Her mother was Khmer and her father was from Laos. We could not obtain further information on her parents.
In Myanmar, we carried out malaria diagnosis and G6PD activity test in remote areas. We analyzed 80 cases of G6PD variant from Myanmar and obtained a result that 91.3% (73/80) of G6PD variants were G6PD Mahidol (487G>A) (Matsuoka et al. 2004). This suggests that the Myanmar population is derived from homogeneous ancestries. Interestingly, we found no cases of G6PD Viangchan in Myanmar. Similarly, we found no cases of G6PD Mahidol in Cambodia in the present study, indicating that Myanmar and Cambodian people are different from each other in terms of G6PD variant.
In Thailand, G6PD Viangchan (871G>A) was the most common variant in the Thai population (Nuchprayoon et al. 2002). In that study, 21 cases of G6PD Viangchan (67.7%) were found among 31 cases of G6PD deficiency while G6PD Mahidol comprised 9.7% (3/31). When we compare that report and our results, we conclude that the Thai population might consist of people from Myanmar and people from the Khmer.
In Malaysia, Ainoon et al. (2003) demonstrated nine G6PD variants among 84 cases of G6PD deficiency in Malaysian Malays. The main variants were G6PD Viangchan (38.1%), G6PD Mediterranean (27.4%), and G6PD Mahidol (15.5%). They concluded that Malaysian Malays had various ancestral contributions.
In Indonesia, we reported that people in Flores Island showed a heterogeneous ancestry (Matsuoka et al. 2003b) because we found five G6PD variants among 15 G6PD-deficient persons. Flores Island belongs to the Sunda Archipelago where people might have come from Eurasian countries, African countries, Philippine Islands, and Pacific Islands. Historically, Flores Island might have accepted many tribes from different origins. Thus, people in Thailand, Malaysia, and Indonesia are of heterozygous ancestry. However Myanmar and Cambodians show homozygous ancestries in terms of G6PD variant.
G6PD Viangchan (871G>A) is said to link to two other mutations in G6PD. One is nucleotide 1311C>T on exon 11 and another is a T>C substitution in intron 11, 93 bp downstream of exon 11 (IVS11 nt93) (Beutler et al. 1992). We read these two points in all cases and confirmed that all cases of G6PD Viangchan (871G>A) had these two mutations. This result is in accordance with the data from the other countries, e.g., Laos (Iwai et al. 2001), Thailand (Nuchprayoon et al. 2002), and Malaysia (Ainoon et al. 2003), describing that all cases of G6PD Viangchan (871G>A) linked to 1311C>T on exon 11 and T>C in nt93 on IVS11. In the case of G6PD Union (1360C>T), G6PD contained the wild type (1311C and IVS-11 nt93T). Moreover, in the 16 cases of G6PD Viangchan heterozygote (871G>G/A), all cases showed a heterozygote pattern (1311C>C/T and IVS-11 nt93T>T/C). These results suggest that G6PD Viangchan (871G>A) is firmly linked to 1311C>T and IVS-11 nt93T>C and that the wild type of Cambodian people has a wild type of 1311C and IVS-11 nt93T.
In this study, we did not give primaquine to malaria patients found in the surveys because the national health policy of Cambodia does not allow administration of primaquine to malaria patients at present. Primaquine is a unique medicine to kill the malaria gametocyte, which is the cause of transmission from malarial patients to mosquitoes. When a malaria patient is confirmed to have normal G6PD activity, he/she should take primaquine together with other malaria medicine. It inhibits the malaria parasites’ transmission to mosquitoes, and it prevents the community from malaria infection. We recognize that there are a great many G6PD-deficient people in Cambodia, so the G6PD activity test is essential before using primaquine on malaria patients.
References
Ainoon O, Yu YH, Amir Muhriz AL, Boo NY, Cheong SK, Hamidah NH (2003) Glucose-6-phosphate dehydrogenase (G6PD) variants in Malaysian Malays. Hum Mutat 21:101
Beutler E, Vulliamy TJ (2002) Hematologically important mutations: glucose-6-phosphate dehydrogenase. Blood Cells Mol Dis 28:93–103
Beutler E, Westwood B, Sipe B (1992) A new polymorphic site in the G6PD gene. Hum Genet 89:485–486
Chen EY, Cheng A, Lee A, Kuang WJ, Hillier L, Green P, Schlessinger D, Ciccodicola A, D’Urso M (1991) Sequence of human glucose-6-phosphate dehydrogenase cloned in plasmids and a yeast artificial chromosome. Genomics 10:792–800
Everett WD, Yoshida A, Pearlman E (1977) Hemoglobin E and glucose-6-phosphate deficiency in the Khmer Air Force (Cambodia). Am J Trop Med Hyg 26:597–601
Fujii H, Takahashi K, Miwa S (1984) A new simple screening method for glucose 6-phosphate dehydrogenase deficiency. Acta Haematol Jpn 47:185–188
Hirono A, Miwa S, Fujii H, Ishida F, Yamada K, Kubota K (1994) Molecular study of eight Japanese cases of glucose-6-phosphate dehydrogenase deficiency by nonradioisotopic single-strand conformation polymorphism analysis. Blood 83:3363–3368
Hirono H, Fujii H, Miwa S (1998) An improved single-step screening method for glucose-6-phosphate dehydrogenase deficiency. Jpn J Trop Med Hyg 26:1–4
Iwai K, Hirono A, Matsuoka H, Kawamoto F, Horie T, Lin K, Tantular IS, Dachlan YP, Notopuro H, Hidayah NI, Salim A M, Fujii H, Miwa S, Ishii A (2001) Distribution of glucose-6-phosphate dehydrogenase mutations in southeast Asia. Hum Genet 108:445–449
Jalloh A, Tantular IS, Pusarawati S, Kawilarang AP, Kerong H, Lin K, Ferreira MU, Matsuoka H, Arai M, Kita K, Kawamoto F (2004) Rapid epidemiologic assessment of glucose-6-phosphate dehydrogenase (G6PD) deficiency in malaria-endemic areas in southeast Asia using a novel diagnostic kit. Trop Med Int Health 9:615–623
Kawamoto F, Billingsley PF (1992) Rapid diagnosis of malaria by fluorescence microscopy. Parasitol Today 8:69–71
Matsuoka H, Ishii A, Panjaitan W (1987) Chemotherapeutic control trial of Plasmodium falciparum with a combination of chloroquine and primaquine on selective age group in a coastal village of North Sumatra, Indonesia. Jpn J Trop Med Hyg 15:257–268
Matsuoka H, Jichun W, Hirai M, Yoshida S, Arai M, Ishii A, Baral MP (2003a) Two cases of glucose-6-phophate dehydrogenase deficient Nepalese belonging to the G6PD Mediterranean-type, not India–Pakistan sub-type but Mediterranean-middle East sub-type. J Hum Genet 48:275–277
Matsuoka H, Arai M, Yoshida S, Tantular IS, Pusarawati S, Kerong H, Kawamoto F (2003b) Five different glucose-6-phophate dehydrogenase (G6PD) variants found among 11 G6PD-deficient persons in Flores Island, Indonesia. J Hum Genet 48:541–544
Matsuoka H, Wang J, Hirai M, Arai M, Yoshida S, Kobayashi T, Jalloh A, Lin K, Kawamoto F (2004) Glucose-6-phosphate dehydrogenase (G6PD) mutations in Myanmar: G6PD Mahidol (487G>A) is the most common variant in the Myanmar population. J Hum Genet 49:544–547
Nuchprayoon I, Sanpavat S, Nuchprayoon S (2002) Glucose-6-phosphate dehydrogenase (G6PD) mutations in Thailand: G6PD Viangchan (871G>A) is the most common deficiency variant in the Thai population. Hum Mutat 19:185
Ruwende C, Khoo SC, Snow RW, Yates SN, Kwiatkowski D, Gupta S, Warn P, Allsopp CE, Gilbert SC, Peschu N, Newbold CI, Greenwood BM, Marsh K, Hill AVS (1995) Natural selection of hemi- and heterozygotes for G6PD deficiency in Africa by resistance to severe malaria. Nature 1376:246–249
Tantular IS, Iwai K, Khin-Lin, Basuki S, Horie T, Htay HH, Matsuoka H, Marwoto H, Wongsrichanalai C, Dachlan YP, Kojima S, Ishii A, Kawamoto F (1999) Field trials of a rapid test for G6PD deficiency in combination with a rapid diagnosis of malaria. Trop Med Int Health 4:245–250
Tantular IS, Kawamoto F (2003) An improved, simple screening method for detection of glucose-6-phosphate dehydrogenase deficiency. Trop Med Int Health 8:569–574
Acknowledgements
We thank Miss Maiko Nakamura for technical assistance. This work was supported by a grant-in-aid for Research on International Medical Cooperation from the Ministry of Health, Labor and Welfare of Japan, and by a grant-in-aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan (14406026 to HM and 15406014 to FK). We also thank the staff of the National Center for Parasitology, Entomology and Malaria Control and field staff for their supporting and excellent collaboration during the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Matsuoka, H., Nguon, C., Kanbe, T. et al. Glucose-6-phosphate dehydrogenase (G6PD) mutations in Cambodia: G6PD Viangchan (871G>A) is the most common variant in the Cambodian population. J Hum Genet 50, 468–472 (2005). https://doi.org/10.1007/s10038-005-0279-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10038-005-0279-z
Keywords
This article is cited by
-
Glucose 6 Phosphate Dehydrogenase (G6PD) quantitation using biosensors at the point of first contact: a mixed method study in Cambodia
Malaria Journal (2022)
-
Population pharmacogenomics: an update on ethnogeographic differences and opportunities for precision public health
Human Genetics (2022)
-
Distribution of G6PD deficiency genotypes among Southeast Asian populations
Tropical Medicine and Health (2021)
-
Prevalence and molecular characterization of glucose-6-phosphate dehydrogenase deficiency in the Lue ethnic group of northern Thailand
Scientific Reports (2021)
-
Investigation of glucose-6-phosphate dehydrogenase (G6PD) deficiency prevalence in a Plasmodium vivax-endemic area in the Republic of Korea (ROK)
Malaria Journal (2020)