Abstract
Objective:
High BMI at midlife is associated with increased risk of dementia as well as faster decline in cognitive function. In late-life, however, high BMI has been found to be associated with both increased and decreased dementia risk. The objective of this study was to investigate the neural substrates of this age-related change in body mass index (BMI) risk.
Methods:
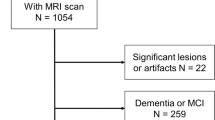
We measured longitudinal cortical thinning over the whole brain, based on magnetic resonance imaging scans for 910 individuals aged 44–66 years at baseline. Subjects were sampled from a large population study (PATH, Personality and Total Health through Life). After attrition and exclusions, the final analysis was based on 792 individuals, including 387 individuals aged 60–66 years and 405 individuals aged 44–49 years. A mixed-effects model was used to test the association between cortical thinning and baseline BMI, as well as percentage change in BMI.
Results:
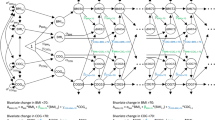
Increasing BMI was associated with increased cortical thinning in posterior cingulate at midlife (0.014 mm kg−1 m−2, confidence interval; CI=0.005, 0.023, P<0.05 false discovery rate (FDR) corrected). In late-life, increasing BMI was associated with reduced cortical thickness, most prominently in the right supramarginal cortex (0.010 mm kg−1 m−2, CI=0.005–0.016, P<0.05 FDR corrected), as well as frontal regions. In late-life, decreasing BMI was also associated with increased cortical thinning, including right caudal middle frontal cortex (0.014 mm kg−1 m−2 (CI=0.006–0.023, P<0.05 FDR corrected).
Conclusions:
The pattern of cortical thinning—in association with increasing BMI at both midlife and late-life—is consistent with known obesity-related dementia risk. Increased cortical thinning in association with decreasing BMI at late-life may help explain the ‘obesity paradox’, where high BMI in midlife appears to be a risk factor for dementia, but high BMI in late-life appears, at times, to be protective.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Anstey K, Cherbuin N, Budge M, Young J . Body mass index in midlife and late‐life as a risk factor for dementia: a meta‐analysis of prospective studies. Obes Rev 2011; 12: e426–e437.
Loef M, Walach H . Midlife obesity and dementia: meta‐analysis and adjusted forecast of dementia prevalence in the united states and china. Obesity 2013; 21: E51–E55.
Dahl AK, Hassing LB, Fransson EI, Gatz M, Reynolds CA, Pedersen NL . Body mass index across midlife and cognitive change in late life. Int J Obes 2013; 37: 296–302.
Raji CA, Ho AJ, Parikshak NN, Becker JT, Lopez OL, Kuller LH et al. Brain structure and obesity. Hum Brain Map 2010; 31: 353–364.
Weinstein G, Beiser AS, DeCarli C, Au R, Wolf PA, Seshadri S . Brain imaging and cognitive predictors of stroke and Alzheimer disease in the Framingham Heart Study. Stroke 2013; 44: 2787–2794.
Jack CR, Knopman DS, Jagust WJ, Petersen RC, Weiner MW, Aisen PS et al. Tracking pathophysiological processes in Alzheimer's disease: an updated hypothetical model of dynamic biomarkers. Lancet Neurol 2013; 12: 207–216.
Shaw ME, Sachdev PS, Anstey KJ, Cherbuin N . Age-related cortical thinning in cognitively healthy individuals in their 60s: the PATH Through Life study. Neurobiol Aging 2016; 39: 202–209.
Pacheco J, Goh JO, Kraut MA, Ferrucci L, Resnick SM . Greater cortical thinning in normal older adults predicts later cognitive impairment. Neurobiol Aging 2015; 36: 903–908.
Dickerson B, Stoub T, Shah R, Sperling R, Killiany R, Albert M et al. Alzheimer-signature MRI biomarker predicts AD dementia in cognitively normal adults. Neurology 2011; 76: 1395–1402.
Kiliaan AJ, Arnoldussen IA, Gustafson DR . Adipokines: a link between obesity and dementia? Lancet Neurol 2014; 13: 913–923.
Gustafson D, Rothenberg E, Blennow K, Steen B, Skoog I . An 18-year follow-up of overweight and risk of Alzheimer disease. Arch Int Med 2003; 163: 1524–1528.
Fitzpatrick AL, Kuller LH, Lopez OL, Diehr P, O’Meara ES, Longstreth W et al. Midlife and late-life obesity and the risk of dementia: cardiovascular health study. Arch Neurol 2009; 66: 336–342.
Dahl AK, Löppönen M, Isoaho R, Berg S, Kivelä SL . Overweight and obesity in old age are not associated with greater dementia risk. J Am Geriatr Soc 2008; 56: 2261–2266.
Hughes T, Borenstein A, Schofield E, Wu Y, Larson E . Association between late-life body mass index and dementia The Kame Project. Neurology 2009; 72: 1741–1746.
Atti AR, Palmer K, Volpato S, Winblad B, De Ronchi D, Fratiglioni L . Late‐life body mass index and dementia incidence: nine‐year follow‐up data from the Kungsholmen Project. J Am Geriatr Soc 2008; 56: 111–116.
Bailey-Downs LC, Tucsek Z, Toth P, Sosnowska D, Gautam T, Sonntag WE et al. Aging exacerbates obesity-induced oxidative stress and inflammation in perivascular adipose tissue in mice: a paracrine mechanism contributing to vascular redox dysregulation and inflammation. The J Gerontol A Bio Sci Med Sci 2013; 68: 780–792.
Yu R, Wong M, Leung J, Lee J, Auyeung TW, Woo J . Incidence, reversibility, risk factors and the protective effect of high body mass index against sarcopenia in community‐dwelling older Chinese adults. Geriatr Gerontol Int 2014; 14: 15–28.
Jackson AS, Janssen I, Sui X, Church TS, Blair SN . Longitudinal changes in body composition associated with healthy ageing: men, aged 20–96 years. Br J Nutr 2012; 107: 1085–1091.
Schaap LA, Pluijm SM, Deeg DJ, Visser M . Inflammatory markers and loss of muscle mass (sarcopenia) and strength. The Am J Med 2006; 119: 526. e9–e17.
Anstey KJ, Christensen H, Butterworth P, Easteal S, Mackinnon A, Jacomb T et al. Cohort Profile: The PATH through life project. Int J Epidemiol 2012; 41: 951–960.
Cherbuin N, Sargent-Cox K, Fraser M, Sachdev P, Anstey K . Being overweight is associated with hippocampal atrophy: the PATH Through Life Study. Int J Obes 2015; 39: 1509.
Jette M, Sidney K, Blümchen G . Metabolic equivalents (METS) in exercise testing, exercise prescription, and evaluation of functional capacity. Clin Cardiol 1990; 13: 555–565.
Lamont AJ, Mortby ME, Anstey KJ, Sachdev PS, Cherbuin N . Using sulcal and gyral measures of brain structure to investigate benefits of an active lifestyle. NeuroImage 2014; 91: 353–359.
Fischl B . FreeSurfer. Neuroimage 2012; 62: 774–781.
Reuter M, Schmansky NJ, Rosas HD, Fischl B . Within-subject template estimation for unbiased longitudinal image analysis. Neuroimage 2012; 61: 1402–1418.
Bernal-Rusiel JL, Greve DN, Reuter M, Fischl B, Sabuncu MR . Statistical analysis of longitudinal neuroimage data with linear mixed effects models. Neuroimage 2013; 66: 249–260.
Desikan RS, Ségonne F, Fischl B, Quinn BT, Dickerson BC, Blacker D et al. An automated labeling system for subdividing the human cerebral cortex on MRI scans into gyral based regions of interest. Neuroimage 2006; 31: 968–980.
Bernal-Rusiel JL, Reuter M, Greve DN, Fischl B, Sabuncu MR . Spatiotemporal linear mixed effects modeling for the mass-univariate analysis of longitudinal neuroimage data. NeuroImage 2013; 81: 358–370.
Genovese CR, Lazar NA, Nichols T . Thresholding of statistical maps in functional neuroimaging using the false discovery rate. Neuroimage 2002; 15: 870–878.
Minoshima S, Giordani B, Berent S, Frey KA, Foster NL, Kuhl DE . Metabolic reduction in the posterior cingulate cortex in very early Alzheimer's disease. Ann Neurol 1997; 42: 85–94.
Zhou Y, Dougherty JH, Hubner KF, Bai B, Cannon RL, Hutson RK . Abnormal connectivity in the posterior cingulate and hippocampus in early Alzheimer's disease and mild cognitive impairment. Alzheimer's Dement 2008; 4: 265–270.
Pengas G, Hodges JR, Watson P, Nestor PJ . Focal posterior cingulate atrophy in incipient Alzheimer's disease. Neurobiol Aging 2010; 31: 25–33.
Killiany R, Hyman B, Ta Gomez-Isla, Moss M, Kikinis R, Jolesz F et al. MRI measures of entorhinal cortex vs hippocampus in preclinical AD. Neurology 2002; 58: 1188–1196.
Prado C, Wells J, Smith S, Stephan B, Siervo M . Sarcopenic obesity: a critical appraisal of the current evidence. Clin Nutr 2012; 31: 583–601.
Samaras K, Lutgers HL, Kochan NA, Crawford JD, Campbell LV, Wen W et al. The impact of glucose disorders on cognition and brain volumes in the elderly: the Sydney Memory and Ageing Study. Age 2014; 36: 977–993.
Gustafson D . Adiposity indices and dementia. Lancet Neurol 2006; 5: 713–720.
Biessels GJ, Reijmer YD . Brain changes underlying cognitive dysfunction in diabetes: what can we learn from MRI? Diabetes 2014; 63: 2244–2252.
Foley JM, Salat DH, Stricker NH, McGlinchey RE, Milberg WP, Grande LJ et al. Glucose dysregulation interacts with APOE-€ 4 to potentiate temporoparietal cortical thinning. Am J Alzheimer's Dis Dement 2016; 31: 76–86.
Shaw ME, Abhayaratna WP, Sachdev PS, Anstey KJ, Cherbuin N . Cortical thinning at midlife: the PATH through life study. Brain Topogr 2016; 29: 875–884.
Acknowledgements
We are grateful to Peter Butterworth, Simon Easteal, Helen Christensen, Patricia Jacomb, Karen Maxwell and the PATH interviewers. The study was supported by NHMRC grant No. 973302, 179805, 350833 157125, ARC grant No. 130101705 and the Dementia Collaborative Research Centres. Nicolas Cherbuin is funded by ARC Fellowship No. 12010227 and Kaarin Anstey by and NHMRC Fellowship No.1002560. This research was partly undertaken on the National Computational Infrastructure (NCI) facility in Canberra, Australia, which is supported by the Australian Commonwealth Government.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Shaw, M., Sachdev, P., Abhayaratna, W. et al. Body mass index is associated with cortical thinning with different patterns in mid- and late-life. Int J Obes 42, 455–461 (2018). https://doi.org/10.1038/ijo.2017.254
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.254
This article is cited by
-
Brain functional and structural magnetic resonance imaging of obesity and weight loss interventions
Molecular Psychiatry (2023)
-
Higher body weight-dependent neural activation during reward processing
Brain Imaging and Behavior (2023)
-
Mechanisms linking obesity and its metabolic comorbidities with cerebral grey and white matter changes
Reviews in Endocrine and Metabolic Disorders (2022)
-
Inter-individual body mass variations relate to fractionated functional brain hierarchies
Communications Biology (2021)
-
Cognition, Brain Structure, and Brain Function in Individuals with Obesity and Related Disorders
Current Obesity Reports (2020)