Abstract
Background:
Within the lung, sympathetic nerve activity (SNA) has an important role in facilitating pulmonary vasodilation. As SNA is elevated in obesity, we aimed to assess the impact of sympathetic hyper-excitation on pulmonary vascular homeostasis in obesity, and its potential role in ameliorating the severity of pulmonary hypertension (PH); the well-documented ‘obesity paradox’ phenomenon.
Methods:
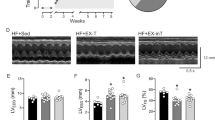
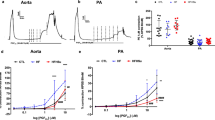
Zucker obese and lean rats were exposed to normoxia or chronic hypoxia (CH-10% O2) for 2 weeks. Subsequently, pulmonary SNA (pSNA) was recorded (electrophysiology), or the pulmonary microcirculation was visualized using Synchrotron microangiography. Acute hypoxic pulmonary vasoconstriction (HPV) was assessed before and after blockade of β1-adrenergic receptors (ARs) (atenolol, 3 mg kg–1) and β1+β2-adrenergic (propranolol, 2 mg kg–1).
Results:
pSNA of normoxic obese rats was higher than lean counterparts (2.4 and 0.5 μV s, respectively). SNA was enhanced following the development of PH in lean rats, but more so in obese rats (1.7 and 6.8 μV s, respectively). The magnitude of HPV was similar for all groups (for example, ~20% constriction of the 200–300 μm vessels). Although β-blockade did not modify HPV in lean rats, it significantly augmented the HPV in normoxic obese rats (β1 and β2 blockade), and more so in obese rats with PH (β2-blockade alone). Western blots showed, while the expression of pulmonary β1-ARs was similar for all rats, the expression of β2-ARs was downregulated in obesity and PH.
Conclusions:
This study suggests that sympathetic hyper-excitation in obesity may have an important role in constraining the severity of PH and, thus, contribute in part to the ‘obesity paradox’ in PH.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Parameswaran K, Todd DC, Soth M . Altered respiratory physiology in obesity. Can Respir J 2006; 13: 203–210.
Sztrymf B, Ioos V, Sitbon O, Parent F, Simonneau G, Humbert M . Pulmonary hypertension and obesity. Rev Pneumol Clin 2002; 58: 104–110.
Dela Cruz CS, Matthay RA . Role of obesity in cardiomyopathy and pulmonary hypertension. Clin Chest Med 2009; 30: 509–523 ix.
Badheka AO, Rathod A, Kizilbash MA, Garg N, Mohamad T, Afonso L et al. Influence of obesity on outcomes in atrial fibrillation: yet another obesity paradox. Am J Med 2010; 123: 646–651.
Strandberg TE, Strandberg AY, Salomaa VV, Pitkala KH, Tilvis RS, Sirola J et al. Explaining the obesity paradox: cardiovascular risk, weight change, and mortality during long-term follow-up in men. Eur Heart J 2009; 30: 1720–1727.
Dixon JB, Lambert GW . The obesity paradox - a reality that requires explanation and clinical interpretation. Atherosclerosis 2013; 226: 47–48.
Ozeke O, Ozer C, Gungor M, Celenk MK, Dincer H, Ilicin G . Chronic intermittent hypoxia caused by obstructive sleep apnea may play an important role in explaining the morbidity-mortality paradox of obesity. Med Hypotheses 2011; 76: 61–63.
Lavie CJ, Milani RV, Artham SM, Patel DA, Ventura HO . The obesity paradox, weight loss, and coronary disease. Am J Med 2009; 122: 1106–1114.
Romero-Corral A, Montori VM, Somers VK, Korinek J, Thomas RJ, Allison TG et al. Association of bodyweight with total mortality and with cardiovascular events in coronary artery disease: a systematic review of cohort studies. Lancet 2006; 368: 666–678.
Zafrir B, Adir Y, Shehadeh W, Shteinberg M, Salman N, Amir O . The association between obesity, mortality and filling pressures in pulmonary hypertension patients; the "obesity paradox". Respir Med 2013; 107: 139–146.
Schwenke DO, Pearson JT, Kangawa K, Umetani K, Shirai M . Changes in macrovessel pulmonary blood flow distribution following chronic hypoxia: assessed using synchrotron radiation microangiography. J Appl Physiol 2008; 104: 88–96.
Mueller PJ, Mischel NA, Scislo TJ . Differential activation of adrenal, renal, and lumbar sympathetic nerves following stimulation of the rostral ventrolateral medulla of the rat. Am J Physiol Regul Integr Comp Physiol 2011; 300: R1230–R1240.
Moral-Sanz J, Menendez C, Moreno L, Moreno E, Cogolludo A, Perez-Vizcaino F . Pulmonary arterial dysfunction in insulin resistant obese Zucker rats. Respir Res 2011; 12: 51.
Shirai M, Tsuchimochi H, Nagai H, Gray E, Pearson JT, Sonobe T et al. Pulmonary vascular tone is dependent on the central modulation of sympathetic nerve activity following chronic intermittent hypoxia. Basic Res Cardiol 2014; 109: 432.
Schwenke DO, Tokudome T, Kishimoto I, Horio T, Cragg PA, Shirai M et al. One dose of ghrelin prevents the acute and sustained increase in cardiac sympathetic tone after myocardial infarction. Endocrinology 2012; 153: 2436–2443.
Schwenke DO, Tokudome T, Shirai M, Hosoda H, Horio T, Kishimoto I et al. Early ghrelin treatment after myocardial infarction prevents an increase in cardiac sympathetic tone and reduces mortality. Endocrinology 2008; 149: 5172–5176.
Shirai M, Schwenke DO, Tsuchimochi H, Umetani K, Yagi N, Pearson JT . Synchrotron radiation imaging for advancing our understanding of cardiovascular function. Circ Res 2013; 112: 209–221.
Huber DA, Schreihofer AM . Attenuated baroreflex control of sympathetic nerve activity in obese Zucker rats by central mechanisms. J Physiol 2010; 588: 1515–1525.
Alvarez GE, Beske SD, Ballard TP, Davy KP . Sympathetic neural activation in visceral obesity. Circulation 2002; 106: 2533–2536.
Calbet JA . Chronic hypoxia increases blood pressure and noradrenaline spillover in healthy humans. J Physiol 2003; 551: 379–386.
Hansen J, Sander M . Sympathetic neural overactivity in healthy humans after prolonged exposure to hypobaric hypoxia. J Physiol 2003; 546: 921–929.
Moraes DJ, Zoccal DB, Machado BH . Medullary respiratory network drives sympathetic overactivity and hypertension in rats submitted to chronic intermittent hypoxia. Hypertension 2012; 60: 1374–1380.
Neubauer JA, Sunderram J . Heme oxygenase-1 and chronic hypoxia. Respir Physiol Neurobiol 2012; 184: 178–185.
Costa-Silva JH, Zoccal DB, Machado BH . Chronic intermittent hypoxia alters glutamatergic control of sympathetic and respiratory activities in the commissural NTS of rats. Am J Physiol Regul Integr Comp Physiol 2012; 302: R785–R793.
Marina N, Tang F, Figueiredo M, Mastitskaya S, Kasimov V, Mohamed-Ali V et al. Purinergic signalling in the rostral ventro-lateral medulla controls sympathetic drive and contributes to the progression of heart failure following myocardial infarction in rats. Basic Res Cardiol 2013; 108: 317.
Sharpe AL, Calderon AS, Andrade MA, Cunningham JT, Mifflin SW, Toney GM . Chronic intermittent hypoxia increases sympathetic control of blood pressure: role of neuronal activity in the hypothalamic paraventricular nucleus. Am J Physiol Heart Circ Physiol 2013; 305: H1772–H1780.
Hausberg M, Morgan DA, Mitchell JL, Sivitz WI, Mark AL, Haynes WG . Leptin potentiates thermogenic sympathetic responses to hypothermia: a receptor-mediated effect. Diabetes 2002; 51: 2434–2440.
Mark AL, Agassandian K, Morgan DA, Liu X, Cassell MD, Rahmouni K . Leptin signaling in the nucleus tractus solitarii increases sympathetic nerve activity to the kidney. Hypertension 2009; 53: 375–380.
Shirai M, Matsukawa K, Nishiura N, Kawaguchi AT, Ninomiya I . Changes in efferent pulmonary sympathetic nerve activity during systemic hypoxia in anesthetized cats. Am J Physiol Regul Integr Comp Physiol 1995; 269: R1404–R1409.
Nagai H, Kuwahira I, Schwenke DO, Tsuchimochi H, Nara A, Inagaki T et al. Beta2-adrenergic receptor-dependent attenuation of hypoxic pulmonary vasoconstriction prevents progression of pulmonary arterial hypertension in intermittent hypoxic rats. PLoS One 2014; 9: e110693.
Schwenke DO, Pearson JT, Kangawa K, Shirai M . Does central nitric oxide chronically modulate the acute hypoxic ventilatory response in conscious rats? Acta Physiol 2006; 186: 309–318.
Bristow MR . Changes in myocardial and vascular receptors in heart failure. J Am Coll Cardiol 1993; 22: 61A–71A.
Nikolaev VO, Moshkov A, Lyon AR, Miragoli M, Novak P, Paur H et al. Beta2-adrenergic receptor redistribution in heart failure changes cAMP compartmentation. Science 2010; 327: 1653–1657.
Lefkowitz RJ, Rockman HA, Koch WJ . Catecholamines, cardiac beta-adrenergic receptors, and heart failure. Circulation 2000; 101: 1634–1637.
Kacimi R, Richalet JP, Corsin A, Abousahl I, Crozatier B . Hypoxia-induced downregulation of beta-adrenergic receptors in rat heart. J Appl Physiol (1985) 1992; 73: 1377–1382.
Nijkamp FP, Engels F, Henricks PA, Van Oosterhout AJ . Mechanisms of beta-adrenergic receptor regulation in lungs and its implications for physiological responses. Physiol Rev 1992; 72: 323–367.
Sharma V, McNeill JH . Parallel effects of beta-adrenoceptor blockade on cardiac function and fatty acid oxidation in the diabetic heart: confronting the maze. World J Cardiol 2011; 3: 281–302.
Acknowledgements
The SR experiments were performed at the BL28B2 in the SPring-8 with the approval of the Japan Synchrotron Radiation Research Institute (proposal no. 2012B1233 and 2013A1124). This study was supported by the Department of Physiology, Otago University, New Zealand, and by Intramural Research Fund (22-2-3 and 25-3-1) for Cardiovascular Diseases of National Cerebral nd Cardiovascular Center, and a Grant-in Aid for Scientific Research (#E056, 26670413) from the Ministry of Education, Culture, Sports, Sciences, and Technology of Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Diong, C., Jones, P., Tsuchimochi, H. et al. Sympathetic hyper-excitation in obesity and pulmonary hypertension: physiological relevance to the ‘obesity paradox’. Int J Obes 40, 938–946 (2016). https://doi.org/10.1038/ijo.2016.33
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2016.33