Abstract
Background:
The Mediterranean diet has been consistently associated with reduced mortality risk. Few prospective studies have examined whether the benefits from a Mediterranean diet are equally shared by obese individuals with varying metabolic health.
Objective:
The objective of this study was to investigate the association between Mediterranean diet, metabolic phenotypes and mortality risk in a representative obese US population.
Methods:
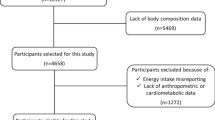
Data from 1739 adults aged 20–88 years were analyzed from participants of the National Health and Nutrition Examination Survey III, 1988–1994 followed up for deaths until 31 December 2011 in a prospective cohort analysis. Mediterranean Diet Scores (MDS) were created to assess the adherence to Mediterranean diet. Participants were classified as metabolically healthy obese (MHO) phenotype (0 or 1 metabolic abnormality) or metabolically unhealthy obese (MUO) phenotype (two or more metabolic abnormalities), based on high glucose, insulin resistance, blood pressure, triglycerides, C-reactive protein and low high-density lipoprotein cholesterol.
Results:
The MHO phenotype (n=598) was observed in 34.8% (s.e., 1.7%) of those who were obese (mean body mass index was 33.4 and 34.8 in MHO and MUO phenotypes, respectively). During a median follow-up of 18.5 years, there were 77 (12.9%) and 309 (27.1%) deaths in MHO and MUO individuals, respectively. In MHO individuals, the multivariable-adjusted hazard ratio (HR) of all-cause mortality in the highest tertile compared with the first tertile of MDS was 0.44 (95% confidence interval (CI), 0.26–0.75; P for trend <0.001), after adjustment for potential confounders. A five-point (1 s.d.) increment in the adherence to MDS was associated with a 41% reduction in the risk of all-cause mortality (HR, 0.59; 95% CI, 0.37–0.94). Similar findings were obtained when we restricted our analyses to those with or without prevalent diabetes mellitus and hypertension. We did not observe mortality risk reduction in either individuals with MUO phenotype or all obese participants combined.
Conclusions:
Adherence to a Mediterranean dietary pattern appears to reduce mortality in the MHO phenotype, but not among the MUO phenotype in an obese population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Trichopoulou A, Costacou T, Bamia C, Trichopoulos D . Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med 2003; 348: 2599–2608.
Estruch R, Ros E, Salas-Salvadó J, Covas M-I, Corella D, Arós F et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med 2013; 368: 1279–1290.
Kastorini C-M, Milionis HJ, Esposito K, Giugliano D, Goudevenos JA, Panagiotakos DB . The effect of mediterranean diet on metabolic syndrome and its componentsa meta-analysis of 50 studies and 534,906 individuals. J Am Coll Cardiol 2011; 57: 1299–1313.
Sofi F, Cesari F, Abbate R, Gensini GF, Casini A . Adherence to Mediterranean diet and health status: meta-analysis. BMJ 2008; 337: a1344.
Kim CS, Ko SH, Kwon HS, Kim NH, Kim JH, Lim S et al. Prevalence, awareness, and management of obesity in Korea: data from the Korea national health and nutrition examination survey (1998-2011). Diabetes Metab J 2014; 38: 35–43.
Guh DP, Zhang W, Bansback N, Amarsi Z, Birmingham CL, Anis AH . The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health 2009; 9: 88.
Karelis AD, St-Pierre DH, Conus F, Rabasa-Lhoret R, Poehlman ET . Metabolic and body composition factors in subgroups of obesity: what do we know? J Clin Endocrinol Metab 2004; 89: 2569–2575.
Kim HY, Kim CW, Lee CD, Choi JY, Park CH, Bae SH et al. Can "healthy" normal alanine aminotransferase levels identify the metabolically obese phenotype? Findings from the Korea national health and nutrition examination survey 2008-2010. Dig Dis Sci 2014; 59: 1330–1337.
Primeau V, Coderre L, Karelis AD, Brochu M, Lavoie ME, Messier V et al. Characterizing the profile of obese patients who are metabolically healthy. Int J Obes (Lond) 2011; 35: 971–981.
Lee SH, Han K, Yang HK, Kim MK, Yoon KH, Kwon HS et al. Identifying subgroups of obesity using the product of triglycerides and glucose: the Korea National Health and Nutrition Examination Survey, 2008-2010. Clin Endocrinol 2015; 82: 213–220.
Ortega FB, Lee DC, Katzmarzyk PT, Ruiz JR, Sui X, Church TS et al. The intriguing metabolically healthy but obese phenotype: cardiovascular prognosis and role of fitness. Eur Heart J 2013; 34: 389–397.
Buckland G, Bach A, Serra-Majem L . Obesity and the Mediterranean diet: a systematic review of observational and intervention studies. Obes Rev 2008; 9: 582–593.
Camhi SM, Whitney Evans E, Hayman LL, Lichtenstein AH, Must A . Healthy eating index and metabolically healthy obesity in U.S. adolescents and adults. Prev Med 2015; 77: 23–27.
Phillips CM, Dillon C, Harrington JM, McCarthy VJ, Kearney PM, Fitzgerald AP et al. Defining metabolically healthy obesity: role of dietary and lifestyle factors. PLoS One 2013; 8: e76188.
Hankinson AL, Daviglus ML, Van Horn L, Chan Q, Brown I, Holmes E et al. Diet composition and activity level of at risk and metabolically healthy obese American adults. Obesity (Silver Spring) 2013; 21: 637–643.
Kimokoti RW, Judd SE, Shikany JM, Newby PK . Food intake does not differ between obese women who are metabolically healthy or abnormal. J Nutr 2014; 144: 2018–2026.
Dalzill C, Nigam A, Juneau M, Guilbeault V, Latour E, Mauriege P et al. Intensive lifestyle intervention improves cardiometabolic and exercise parameters in metabolically healthy obese and metabolically unhealthy obese individuals. Can J Cardiol 2014; 30: 434–440.
Karelis AD, Messier V, Brochu M, Rabasa-Lhoret R . Metabolically healthy but obese women: effect of an energy-restricted diet. Diabetologia 2008; 51: 1752–1754.
Liu RH, Wharton S, Sharma AM, Ardern CI, Kuk JL . Influence of a clinical lifestyle-based weight loss program on the metabolic risk profile of metabolically normal and abnormal obese adults. Obesity (Silver Spring) 2013; 21: 1533–1539.
Hankinson AL, Daviglus ML, Horn LV, Chan Q, Brown I, Holmes E et al. Diet composition and activity level of at risk and metabolically healthy obese American adults. Obesity 2013; 21: 637–643.
United States. National Center for Health Statistics. Plan and Operation of the Third National Health and Nutrition Examination Survey, 1988–94. US Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention: Hyattsville, MD, Washington, DC 1994.
Panagiotakos DB, Pitsavos C, Stefanadis C . Dietary patterns: a Mediterranean diet score and its relation to clinical and biological markers of cardiovascular disease risk. Nutr Metab Cardiovasc Dis 2006; 16: 559–568.
Panagiotakos DB, Pitsavos C, Arvaniti F, Stefanadis C . Adherence to the Mediterranean food pattern predicts the prevalence of hypertension, hypercholesterolemia, diabetes and obesity, among healthy adults; the accuracy of the MedDietScore. Prev Med 2007; 44: 335–340.
Carter SJ, Roberts MB, Salter J, Eaton CB . Relationship between Mediterranean Diet Score and atherothrombotic risk: findings from the Third National Health and Nutrition Examination Survey (NHANES III), 1988-1994. Atherosclerosis 2010; 210: 630–636.
Mila-Villarroel R, Bach-Faig A, Puig J, Puchal A, Farran A, Serra-Majem L et al. Comparison and evaluation of the reliability of indexes of adherence to the Mediterranean diet. Public Health Nutr 2011; 14: 2338–2345.
Fung TT, McCullough ML, Newby P, Manson JE, Meigs JB, Rifai N et al. Diet-quality scores and plasma concentrations of markers of inflammation and endothelial dysfunction. Am J Clin Nutr 2005; 82: 163–173.
Ronksley PE, Brien SE, Turner BJ, Mukamal KJ, Ghali WA . Association of alcohol consumption with selected cardiovascular disease outcomes: a systematic review and meta-analysis. BMJ 2011; 342: d671.
Rimm EB, Klatsky A, Grobbee D, Stampfer MJ . Review of moderate alcohol consumption and reduced risk of coronary heart disease: is the effect due to beer, wine, or spirits? BMJ 1996; 312: 731–736.
Liangpunsakul S, Crabb DW, Qi R . Relationship among alcohol intake, body fat, and physical activity: a population-based study. Ann Epidemiol 2010; 20: 670–675.
Fung TT, Rexrode KM, Mantzoros CS, Manson JE, Willett WC, Hu FB . Mediterranean diet and incidence of and mortality from coronary heart disease and stroke in women. Circulation 2009; 119: 1093–1100.
Kuk JL, Ardern CI . Are metabolically normal but obese individuals at lower risk for all-cause mortality? Diabetes Care 2009; 32: 2297–2299.
Wildman RP, Muntner P, Reynolds K, McGinn AP, Rajpathak S, Wylie-Rosett J et al. The obese without cardiometabolic risk factor clustering and the normal weight with cardiometabolic risk factor clustering: prevalence and correlates of 2 phenotypes among the US population (NHANES 1999-2004). Arch Intern Med 2008; 168: 1617–1624.
Haskell WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Circulation 2007; 116: 1081–1093.
Hinnouho G-M, Czernichow S, Dugravot A, Batty GD, Kivimaki M, Singh-Manoux A . Metabolically healthy obesity and risk of mortality does the definition of metabolic health matter? Diabetes Care 2013; 36: 2294–2300.
George SM, Ballard-Barbash R, Manson JE, Reedy J, Shikany JM, Subar AF et al. Comparing indices of diet quality with chronic disease mortality risk in postmenopausal women in the Women's Health Initiative Observational Study: evidence to inform national dietary guidance. Am J Epidemiol 2014; 180: 616–625.
Mitrou PN, Kipnis V, Thiébaut AC, Reedy J, Subar AF, Wirfält E et al. Mediterranean dietary pattern and prediction of all-cause mortality in a US population: results from the NIH-AARP Diet and Health Study. Arch Intern Med 2007; 167: 2461–2468.
Lissner L, Troiano RP, Midthune D, Heitmann BL, Kipnis V, Subar AF et al. OPEN about obesity: recovery biomarkers, dietary reporting errors and BMI. Int J Obes (Lond) 2007; 31: 956–961.
Adams KF, Leitzmann MF, Ballard-Barbash R, Albanes D, Harris TB, Hollenbeck A et al. Body mass and weight change in adults in relation to mortality risk. Am J Epidemiol 2014; 179: 135–144.
Hamer M, Stamatakis E . Metabolically healthy obesity and risk of all-cause and cardiovascular disease mortality. J Clin Endocrinol Metab 2012; 97: 2482–2488.
McLaughlin T, Deng A, Yee G, Lamendola C, Reaven G, Tsao PS et al. Inflammation in subcutaneous adipose tissue: relationship to adipose cell size. Diabetologia 2010; 53: 369–377.
MacLaren R, Cui W, Simard S, Cianflone K . Influence of obesity and insulin sensitivity on insulin signaling genes in human omental and subcutaneous adipose tissue. J Lipid Res 2008; 49: 308–323.
Badoud F, Lam KP, DiBattista A, Perreault M, Zulyniak MA, Cattrysse B et al. Serum and adipose tissue amino acid homeostasis in the metabolically healthy obese. J Proteome Res 2014; 13: 3455–3466.
Widmer RJ, Flammer AJ, Lerman LO, Lerman A . The Mediterranean diet, its components, and cardiovascular disease. Am J Med 2015; 128: 229–238.
Kramer CK, Zinman B, Retnakaran R . Are metabolically healthy overweight and obesity benign conditions? A systematic review and meta-analysis. Ann Intern Med 2013; 159: 758–769.
Soriguer F, Gutierrez-Repiso C, Rubio-Martin E, Garcia-Fuentes E, Almaraz MC, Colomo N et al. Metabolically healthy but obese, a matter of time? Findings from the prospective Pizarra study. J Clin Endocrinol Metab 2013; 98: 2318–2325.
Park YM, Sui X, Liu J, Zhou H, Kokkinos PF, Lavie CJ et al. The effect of cardiorespiratory fitness on age-related lipids and lipoproteins. J Am Coll Cardiol 2015; 65: 2091–2100.
Lee DH, Kim YM, Jekal Y, Park S, Kim KC, Naruse M et al. Low levels of physical activity are associated with increased metabolic syndrome risk factors in korean adults. Diabetes Metab J 2013; 37: 132–139.
Lee S, Kim Y . Effects of exercise alone on insulin sensitivity and glucose Tolerance in obese youth. Diabetes Metab J 2013; 37: 225–232.
Phillips CM . Metabolically healthy obesity: definitions, determinants and clinical implications. Rev Endocr Metab Disord 2013; 14: 219–227.
Fukushima Y, Kurose S, Shinno H, Cao Thu H, Takao N, Tsutsumi H et al. Importance of lean muscle maintenance to improve insulin resistance by body weight reduction in female patients with obesity. Diabetes Metab J 2016; 40: 147–153.
Plourde G, Karelis AD . Current issues in the identification and treatment of metabolically healthy but obese individuals. Nutr Metab Cardiovasc Dis 2014; 24: 455–459.
Janiszewski PM, Ross R . Effects of weight loss among metabolically healthy obese men and women. Diabetes Care 2010; 33: 1957–1959.
Freedman LS, Commins JM, Moler JE, Arab L, Baer DJ, Kipnis V et al. Pooled results from 5 validation studies of dietary self-report instruments using recovery biomarkers for energy and protein intake. Am J Epidemiol 2014; 180: 172–188.
Rimm EB, Giovannucci EL, Stampfer MJ, Colditz GA, Litin LB, Willett WC . Reproducibility and validity of an expanded self-administered semiquantitative food frequency questionnaire among male health professionals. Am J Epidemiol 1992; 135: 1114–1126, discussion 1127-36.
Acknowledgements
We are grateful to Dr Alexandra J White for critical review of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Park, YM., Steck, S., Fung, T. et al. Mediterranean diet and mortality risk in metabolically healthy obese and metabolically unhealthy obese phenotypes. Int J Obes 40, 1541–1549 (2016). https://doi.org/10.1038/ijo.2016.114
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2016.114
This article is cited by
-
Metabolically Healthy Obesity: Are Interventions Useful?
Current Obesity Reports (2023)
-
Schizophrenia patients with a metabolically abnormal obese phenotype have milder negative symptoms
BMC Psychiatry (2020)
-
Role of Paced Breathing for Treatment of Hypertension
Current Hypertension Reports (2017)