Abstract
Objectives:
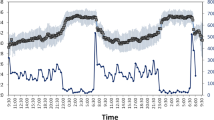
Some of the major challenges associated with successful dietary weight management include the identification of individuals not responsive to specific interventions. The aim was to investigate the potential relationship between weight loss and circadian rhythmicity, using wrist temperature and actimetry measurements, in women undergoing a weight-loss program, in order to assess whether circadian rhythmicity could be a marker of weight-loss effectiveness.
Methods:
Participants were 85 overweight and obese women (body mass index, BMI: 30.24±4.95 kg m−2) subjected to a weight-reduction program. Efficacy of the treatment was defined as total weight loss, percentage of initial weight and weekly weight loss rates. Circadian rhythmicity in wrist temperature motor activity and position were analyzed using different sensors.
Results:
Lower weight loss was related with a more flattened pattern measured as amplitude from cosinor (r=0.235, P=0.032), a higher fragmentation of rhythms determined by higher intradaily variability (IV) (r=−0.339, P=0.002), and an impaired wrist temperature circadian rhythm determined by the means of Circadian Function Index (r=0.228, P=0.038). Further analyses showed that low responders displayed lower amplitude (0.71±0.36 versus 1.24±0.62, P=0.036) and higher fragmentation of the circadian rhythm (0.24±0.11 versus 0.15±0.07, P=0.043) than high responders. Whereas we did not find significant differences in total activity rates between high responders and low responders, we found significant differences for the mean values of body position for high responders (39.12±3.79°) as compared with low responder women (35.31±2.53°, P=0.01).
Conclusions:
Circadian rhythms at the beginning of the treatment are good predictors of future weight loss. Further treatment should consider chronobiological aspects to diagnose obesity and effectiveness of treatments.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Bacon L, Aphramor L . Weight science: evaluating the evidence for a paradigm shift. Nutr J 2011; 10: 9.
Elfhag K, Rossner S . Who succeeds in maintaining weight loss? A conceptual review of factors associated with weight loss maintenance and weight regain. Obes Rev 2005; 6: 67–85.
Teixeira PJ, Palmeira AL, Branco TL, Martins SS, Minderico CS, Barata JT et al. Who will lose weight? A reexamination of predictors of weight loss in women. Int J Behav Nutr Phys Activity 2004; 1: 12.
Teixeira PJ, Silva MN, Coutinho SR, Palmeira AL, Mata J, Vieira PN et al. Mediators of weight loss and weight loss maintenance in middle-aged women. Obesity (Silver Spring) 2010; 18: 725–735.
Ordovas JM . Genotype-phenotype associations: modulation by diet and obesity. Obesity (Silver Spring) 2008; 16 (Suppl 3): S40–S46.
Garaulet M, Corbalan MD, Madrid JA, Morales E, Baraza JC, Lee YC et al. CLOCK gene is implicated in weight reduction in obese patients participating in a dietary programme based on the Mediterranean diet. Int J Obes (Lond) 2010; 34: 516–523.
Bandin C, Martinez-Nicolas A, Ordovas JM, Ros Lucas JA, Castell P, Silvente T et al. Differences in circadian rhythmicity in CLOCK 3111T/C genetic variants in moderate obese women as assessed by thermometry, actimetry and body position. Int J Obes (Lond) 2012; 37: 1044–1050.
Marcheva B, Ramsey KM, Affinati A, Bass J . Clock genes and metabolic disease. J Appl Physiol (Bethesda, Md: 1985) 2009; 107: 1638–1646.
Wyse CA . Does human evolution in different latitudes influence susceptibility to obesity via the circadian pacemaker?: migration and survival of the fittest in the modern age of lifestyle-induced circadian desynchrony. Bioessays 2012; 34: 921–924.
Corbalán-Tutau MD, Madrid JA, Ordovás JM, Smith CE, Nicolás F, Garaulet M . Differences in daily rhythms of wrist temperature between obese and normal-weight women: associations with metabolic syndrome features. Chronobiol Int 2011; 28: 425–433.
Bland IM, Guthrie-Jones A, Taylor RD, Hill J . Dog obesity: veterinary practices' and owners' opinions on cause and management. Prev Vet Med 2010; 94: 310–315.
Van Cauter ETF The endocrine system In: McEwen BSHandbook of Physiology. Oxford University Press: New York, NY, USA, 2000. pp 313–330.
Buijs RM, Kalsbeek A . Hypothalamic integration of central and peripheral clocks. Nat Rev Neurosci 2001; 2: 521–526.
Duguay D, Cermakian N . The crosstalk between physiology and circadian clock proteins. Chronobiol Int 2009; 26: 1479–1513.
Stratmann M, Schibler U . Properties, entrainment, and physiological functions of mammalian peripheral oscillators. J Biol Rhythms 2006; 21: 494–506.
Martinez-Nicolas A, Ortiz-Tudela E, Madrid JA, Rol MA . Crosstalk between environmental light and internal time in humans. Chronobiol Int 2011; 28: 617–629.
Sarabia JA, Rol MA, Mendiola P, Madrid JA . Circadian rhythm of wrist temperature in normal-living subjects A candidate of new index of the circadian system. Physiol Behav 2008; 95: 570–580.
Martinez-Nicolas A, Ortiz-Tudela E, Rol MA, Madrid JA . Uncovering different masking factors on wrist skin temperature rhythm in free-living subjects. PloS One 2013; 8: e61142.
Bonmati-Carrion MA, Middleton B, Revell V, Skene DJ, Rol MA, Madrid JA . Circadian phase asessment by monitoring in humans: correlation with dim light melatonin onset. Chronobiol Int 2013; e-pub ahead of print 28 October 2013.
Garaulet M, Pérez-Llamas F, Zamora S, Tebar FJ . Weight loss and possible reasons for dropping out of a dietary/behavioural programme in the treatment of overweight patients. J Human Nutr Diet 1999; 12: 219–227.
Serra-Majem L, Aranceta J . Nutritional objectives for the Spanish population. Consensus from the Spanish Society of Community Nutrition. Public Health Nutr 2001; 4: 1409–1413.
Cooper Z, Christopher GF, Hawker DM . Cognitive-behavioral Treatment of Obesity: A Clinician's Guide. The Guilford Press: New York, NY, USA, 2003.
Ortiz-Tudela E, Martinez-Nicolas A, Campos M, Rol MA, Madrid JA . A new integrated variable based on thermometry, actimetry and body position (TAP) to evaluate circadian system status in humans. PLoS Comput Biol 2010; 6: e1000996.
van Someren EJ, Mirmiran M, Swaab DF . Non-pharmacological treatment of sleep and wake disturbances in aging and Alzheimer's disease: chronobiological perspectives. Behav Brain Res 1993; 57: 235–253.
Kistler A, Mariauzouls C, von Berlepsch K . Fingertip temperature as an indicator for sympathetic responses. Int J Psychophysiol 1998; 29: 35–41.
Corbalan-Tutau MD, Madrid JA, Ordovas JM, Smith CE, Nicolas F, Garaulet M . Differences in daily rhythms of wrist temperature between obese and normal-weight women: associations with metabolic syndrome features. Chronobiol Int 2011; 28: 425–433.
Huang YL, Liu RY, Wang QS, Van Someren EJ, Xu H, Zhou JN . Age-associated difference in circadian sleep-wake and rest-activity rhythms. Physiol Behav 2002; 76: 597–603.
Van Someren EJ, Swaab DF, Colenda CC, Cohen W, McCall WV, Rosenquist PB . Bright light therapy: improved sensitivity to its effects on rest-activity rhythms in Alzheimer patients by application of nonparametric methods. Chronobiol Int 1999; 16: 505–518.
Carvalho-Bos SS, Riemersma-van der Lek RF, Waterhouse J, Reilly T, Van Someren EJ . Strong association of the rest-activity rhythm with well-being in demented elderly women. Am J Geriatr Psychiatr 2007; 15: 92–100.
Huang W, Ramsey KM, Marcheva B, Bass J . Circadian rhythms, sleep, and metabolism. J Clin Investig 2011; 121: 2133–2141.
Garaulet M, Gomez-Abellan P, Alburquerque-Bejar JJ, Lee YC, Ordovas JM, Scheer FA . Timing of food intake predicts weight loss effectiveness. Int J Obes (Lond) 2013; 37: 604–611.
Garaulet M, Sanchez-Moreno C, Smith CE, Lee YC, Nicolas F, Ordovas JM . Ghrelin, sleep reduction and evening preference: relationships to CLOCK 3111 T/C SNP and weight loss. PloS One 2011; 6: e17435.
Gallant AR, Lundgren J, Drapeau V . The night-eating syndrome and obesity. Obes Rev 2012; 13: 528–536.
Acknowledgements
We want to thank all the patients for their participation in this study, and also José Cánovas Lorente for his support and help in data collection and processing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Bandín, C., Martinez-Nicolas, A., Ordovás, J. et al. Circadian rhythmicity as a predictor of weight-loss effectiveness. Int J Obes 38, 1083–1088 (2014). https://doi.org/10.1038/ijo.2013.211
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2013.211
Keywords
This article is cited by
-
Association between CLOCK 3111 T/C polymorphism with ghrelin, GLP-1, food timing, sleep and chronotype in overweight and obese Iranian adults
BMC Endocrine Disorders (2022)
-
Reproducibility and associations with obesity and insulin resistance of circadian-rhythm parameters in free-living vs. controlled conditions during the PREVIEW lifestyle study
International Journal of Obesity (2021)
-
Meal timing affects glucose tolerance, substrate oxidation and circadian-related variables: A randomized, crossover trial
International Journal of Obesity (2015)