Abstract
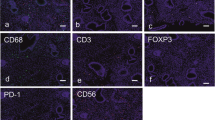
Enhanced endometrial proliferation correlates obesity to type-I (estrogen-dependent) endometrial cancer (EC). Our aim was to distinguish obese women (without EC) with differing endometrial proliferation. Endometrial and blood samples were obtained from normal-weight and obese women without EC. Type-I EC samples were obtained from obese patients. On measuring endometrial proliferation (Ki67 and phosphorylated histone H3 (p-H3)), two groups of obese women without EC were identified: obeseHigh Proliferating (OHP) and obeseLow Proliferating (OLP). Increased Ki67 (88.5%, P<0.001), p-H3 (62.6%, P<0.01), 17β-estradiol/progesterone ratio (46.3%, P<0.01) and endometrial estrogen receptor alpha (ERα) (82.2%, P<0.001) were observed in OHP compared with OLP patients. ECs possessed similar ERα and enhanced proliferation as OHP, suggesting that OHP women are at higher risk of type-I EC. OLP women were indistinguishable from normal-weight women regarding these determinants of endometrial proliferation, ERα and 17β-estradiol/progesterone ratio. Our data may further define the obesity phenotype in regards to type-I EC risk and may help identify obese women more susceptible to develop type-I EC, allowing early intervention and a potential reduction in mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Ogden CL, Yanovski SZ, Carroll MD, Flegal KM . The epidemiology of obesity. Gastroenterology 2007; 132: 2087–2102.
World Health Organization (WHO). Obesity and Overweight, 2011, http://www.who.int/mediacentre/factsheets/fs311/en/ (accessed 30 May 2011).
Calle EE, Kaaks R . Overweight, obesity and cancer: epidemiological evidence and proposed mechanisms. Nat Rev Cancer 2004; 4: 579–591.
Kaaks R, Lukanova A, Kurzer MS . Obesity, endogenous hormones, and endometrial cancer risk: a systematic review. Cancer Epidemiol Biomarkers Prev 2002; 11: 1531–1543.
von Gruenigen VE, Gil KM, Frasure HE, Jenison EJ, Hopkins MP . The impact of obesity and age on quality of life in gynecologic surgery. Am J Obstet Gynecol 2005; 193: 1369–1375.
Potischman N, Hoover RN, Brinton LA, Siiteri P, Dorgan JF, Swanson CA et al. Case-control study of endogenous steroid hormones and endometrial cancer. J Natl Cancer Inst 1996; 88: 1127–1135.
Zang H, Sahlin L, Masironi B, Hirschberg AL . Effects of testosterone and estrogen treatment on the distribution of sex hormone receptors in the endometrium of postmenopausal women. Menopause 2008; 15: 233–239.
Key TJA, Pike MC . The dose-effect relationship between unopposed estrogens and endometrial mitotic rate: its central role in explaining and predicting endometrial cancer risk. Br J Cancer 1988; 57: 205–212.
Altekruse SF, Kosary CL, Krapcho M, Neyman N, Aminou R, Waldron W et al. (Eds). SEER Cancer Statistics Review 1975–2007. National Cancer Institute: Bethesda, MD. http://seer.cancer.gov/csr/1975_2007/,based on November 2009 SEER data submission, posted to the SEER web site, 2010.
Noyes RW, Hertig AT, Rock J . Dating the endometrial biopsy. Am J Obstet Gynecol 1975; 122: 262–263.
Burton BT, Foster WR, Hirsch J, Van Itallie TB . Health implications of obesity: an NIH Consensus Development Conference. Int J Obes 1985; 9: 155–170.
Villavicencio A, Aguilar G, Argüello G, Dünner C, Gabler F, Soto E et al. The effect of overweight and obesity on proliferation and activation of AKT and ERK in human endometria. Gynecol Oncol 2010; 117: 96–102.
Villavicencio A, Bacallao K, Avellaira C, Gabler F, Fuentes A, Vega M . Androgen and estrogen receptors and co-regulators levels in endometria from patients with polycystic ovarian syndrome with and without endometrial hyperplasia. Gynecol Oncol 2006; 103: 307–314.
Wallace RB, Sherman BM, Bean JA, Leeper JP, Treloar AE . Menstrual cycle patterns and breast cancer risk factors. Cancer Res 1978; 38: 4021–4024.
Davidson BJ, Gambone JC, Lagasse LD, Castaido JW, Hammond GL, Siiteri PK et al. Free estradiol in postmenopausal women with and without endometrial cancer. J Clin Endocrinol Metab 1981; 52: 404–408.
Judd HL, Lucas WE, Yen SS . Serum 17β-estradiol and estrone levels in postmenopausal women with and without endometrial cancer. J Clin Endocrinol Metab 1976; 43: 272–278.
Karelis AD, St-Pierre DH, Conus F, Rabasa-Lhoret R, Poehlman ET . Metabolic and body composition factors in subgroups of obesity: what do we know? J Clin Endocrinol Metab 2004; 89: 2569–2575.
Sims EA . Are there persons who are obese, but metabolically healthy? Metabolism 2001; 50: 1499–1504.
Mumford SL, Dasharathy S, Pollack AZ, Schisterman EF . Variations in lipid levels according to menstrual cycle phase: clinical implications. Clin Lipidol 2011; 6: 225–234.
Rock CL, Flatt SW, Thomson CA, Stefanick ML, Newman VA, Jones LA et al. Effects of a high-fiber, low-fat diet intervention on serum concentrations of reproductive steroid hormones in women with a history of breast cancer. J Clin Oncol 2004; 22: 2379–2387.
Key TJ, Appleby PN, Reeves GK, Roddam A, Dorgan JF, Longcope C et al. Body mass index, serum sex hormones, and breast cancer risk in postmenopausal women. J Natl Cancer Inst 2003; 95: 1218–1226.
Ashrafian H, Ahmed K, Rowland SP, Patel VM, Gooderham NJ, Holmes E et al. Metabolic surgery and cancer: protective effects of bariatric procedures. Cancer 2011; 117: 1788–1799.
Sjöström L, Gummesson A, Sjöström CD, Narbro K, Peltonen M, Wedel H et al. Effects of bariatric surgery on cancer incidence in obese patients in Sweden (Swedish Obese Subjects Study): a prospective, controlled intervention trial. Lancet Oncol 2009; 10: 653–662.
Brown KA, Hunger NI, Docanto M, Simpson ER . Metformin inhibits aromatase expression in human breast adipose stromal cells via stimulation of AMP-activated protein kinase. Breast Cancer Res Treat 2010; 123: 591–596.
Xie Y, Wang YL, Yu L, Hu Q, Ji L, Zhang Y et al. Metformin promotes progesterone receptor expression via inhibition of mammalian target of rapamycin (mTOR) in endometrial cancer cells. J Steroid Biochem Mol Biol 2011; 126: 113–120.
Acknowledgements
We thank the women who donated blood and endometrial samples. This study was supported by Grant No. 1110232 from the Fondo Nacional de Desarrollo Científico y Tecnológico.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Villavicencio, A., Aguilar, G., Acuña, J. et al. The identification of two subgroups of obese women with differing endometrial proliferation levels: potential consequences in the development of endometrial cancer. Int J Obes 36, 1012–1015 (2012). https://doi.org/10.1038/ijo.2011.189
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2011.189