Abstract
Objective:
The aim of this study was to examine the association of body mass index (BMI) and weight gain with eating at restaurants and similar establishments or eating at work among 10 European countries of the European Prospective Investigation into Cancer and Nutrition (EPIC) study.
Subjects:
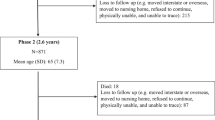
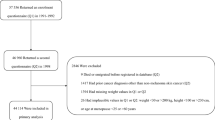
This study included a representative sample of 24 310 randomly selected EPIC participants.
Methods:
Single 24-h dietary recalls with information on the place of consumption were collected using standardized procedures between 1995 and 2000. Eating at restaurants was defined to include all eating and drinking occasions at restaurants, cafeterias, bars and fast food outlets. Eating at work included all eating and drinking occasions at the workplace. Associations between eating at restaurants or eating at work and BMI or annual weight changes were assessed using sex-specific linear mixed-effects models, controlling for potential confounders.
Results:
In southern Europe energy intake at restaurants was higher than intake at work, whereas in northern Europe eating at work appeared to contribute more to the mean daily intake than eating at restaurants. Cross-sectionally, eating at restaurants was found to be positively associated with BMI only among men (β=+0.24, P=0.003). Essentially no association was found between BMI and eating at work among both genders. In a prospective analysis among men, eating at restaurants was found to be positively, albeit nonsignificantly, associated with weight gain (β=+0.05, P=0.368). No association was detected between energy intake at restaurants and weight changes, controlling for total energy intake.
Conclusion:
Among men, eating at restaurants and similar establishments was associated with higher BMI and possibly weight gain.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
World Health Organization. Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organ Tech Rep Ser 2000; 894: i–253.
Branca F, Nikogocian H, Lobstein T (eds) The Challenge of Obesity in the WHO European Region and the Strategies for Response. WHO Regional Office for Europe: Copenhagen, Denmark, 2007.
Clemens LH, Slawson DL, Klesges RC . The effect of eating out on quality of diet in premenopausal women. J Am Diet Assoc 1999; 99: 442–444.
Binkley JK, Eales J, Jekanowski M . The relation between dietary change and rising US obesity. Int J Obes 2000; 24: 1032–1039.
French SA, Harnack L, Jeffery RW . Fast food restaurant use among women in the Pound of Prevention study: dietary, behavioral and demographic correlates. Int J Obes 2000; 24: 1353–1359.
French SA, Story M, Neumark-Sztainer D, Fulkerson JA, Hannan P . Fast food restaurant use among adolescents: associations with nutrient intake, food choices and behavioral and psychosocial variables. Int J Obes 2001; 25: 1823–1833.
Burns C, Jackson M, Gibbons C, Stoney RM . Foods prepared outside the home: association with selected nutrients and body mass index in adult Australians. Public Health Nutr 2002; 5: 441–448.
Nielsen SJ, Siega-Riz AM, Popkin BM . Trends in energy intake in US between 1977 and 1996: similar shifts seen across age groups. Obesity Res 2002; 10: 370–378.
Kant AK, Graubard BI . Eating out in America, 1987–2000: trends and nutritional correlates. Prev Med 2004; 38: 243–249.
O'Dwyer NA, Gibney MJ, Burke SJ, McCarthy SN . The influence of eating location on nutrient intakes in Irish adults: implications for food-based dietary guidelines. Public Health Nutr 2005; 8: 262–269.
Pereira MA, Kartashov AI, Ebbeling CB, Van Horn L, Slattery ML, Jacobs Jr DR et al. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet 2005; 365: 36–42.
Duffey KJ, Popkin BM . Shifts in patterns and consumption of beverages between 1965 and 2002. Obesity (Silver Spring) 2007; 15: 2739–2747.
Schröder H, Fïto M, Covas MI, REGICOR investigators. Association of fast food consumption with energy intake, diet quality, body mass index and the risk of obesity in a representative Mediterranean population. Br J Nutr 2007; 98: 1274–1280.
Marín-Guerrero AC, Gutiérrez-Fisac JL, Guallar-Castillón P, Banegas JR, Rodríguez-Artalejo F . Eating behaviours and obesity in the adult population of Spain. Br J Nutr 2008; 100: 1142–1148.
Bezerra IN, Sichieri R . Eating out of home and obesity: a Brazilian nationwide study. Public Health Nutr 2009; 12: 2037–2043.
Duffey KJ, Gordon-Larsen P, Jacobs DR, Williams OD, Popkin BM . Differential associations of fast food and restaurant food consumption with 3-y change in body mass index: the Coronary Artery Risk development in young adults study. Am J Clin Nutr 2007; 85: 201–208.
Bes-Rastrollo M, Basterra-Gortari FJ, Sánchez-Villegas A, Marti A, Martínez JA, Martínez-González MA . A prospective study of eating away-from-home meals and weight gain in a Mediterranean population: the SUN (Seguimiento Universidad de Navarra) cohort. Public Health Nutr 2009. E-pub ahead of print 3 December 2009; 1–8.
Kearney JM, Hulshof KFAM, Gibney MJ . Eating patterns—temporal distribution, converging and diverging foods, meals eaten inside and outside of the home—implications for developing FBDG. Public Health Nutr 2003; 4: 693–698.
Orfanos P, Naska A, Trichopoulos D, Slimani N, Ferrari P, van Bakel M et al. Eating out of home and its correlates in 10 European countries. The European Prospective Investigation into Cancer and nutrition (EPIC) study. Public Health Nutr 2007; 10: 1515–1525.
Orfanos P, Naska A, Trichopoulou A, Grioni S, Boer JM, van Bakel MM et al. Eating out of home: energy, macro- and micronutrient intakes in 10 European countries. The European Prospective Investigation into Cancer and Nutrition. Eur J Clin Nutr 2009; 63 (Suppl 4): S239–S262.
Bingham S, Riboli E . Diet and cancer—the European Prospective Investigation into Cancer and Nutrition. Nat Rev Cancer 2004; 4: 206–215.
Riboli E, Kaaks R . The EPIC Project: rationale and study design. European Prospective Investigation into Cancer and Nutrition. Int J Epidemiol 1997; 26 (Suppl 1): S6–S14.
Riboli E, Hunt KJ, Slimani N, Ferrari P, Norat T, Fahey M et al. European prospective investigation into cancer and nutrition (EPIC): study populations and data collection. Public Health Nutr 2002; 5: 1113–1124.
Haftenberger M, Lahmann PH, Panico S, Gonzalez CA, Seidell JC, Boeing H et al. Overweight, obesity and fat distribution in 50- to 64-year-old participants in the European Prospective Investigation into Cancer and Nutrition (EPIC). Public Health Nutr 2002; 5: 1147–1162.
Haftenberger M, Schuit AJ, Tormo MJ, Boeing H, Wareham N, Bueno-de-Mesquita HB et al. Physical activity of subjects aged 50-64 years involved in the European Prospective Investigation into Cancer and Nutrition (EPIC). Public Health Nutr 2002; 5: 1163–1176.
Friedenreich C, Cust A, Lahmann PH, Steindorf K, Boutron-Ruault MC, Clavel-Chapelon F et al. Physical activity and risk of endometrial cancer: the European Prospective Investigation into Cancer and Nutrition. Int J Cancer 2007; 121: 347–355.
Slimani N, Kaaks R, Ferrari P, Casagrande C, Clavel-Chapelon F, Lotze G et al. European prospective investigation into cancer and nutrition (EPIC) calibration study: rationale, design and population characteristics. Public Health Nutr 2002; 5: 1125–1145.
Ferrari P, Slimani N, Ciampi A, Trichopoulou A, Naska A, Lauria C et al. Evaluation of under- and overreporting of energy intake in the 24-h diet recalls in the European Prospective Investigation into Cancer and Nutrition (EPIC). Public Health Nutr 2002; 5: 1329–1345.
Slimani N, Deharveng G, Charrondiere R, van Kappel AL, Ocké MC, Welch A et al. Structure of the standardized computerized 24-h diet recall interview used as reference method in the 22 centers participating in the EPIC project. European Prospective Investigation into Cancer and Nutrition. Comput Methods Programs Biomed 1999; 58: 251–266.
Brustad M, Skeie G, Braaten T, Slimani N, Lund E . Comparison of telephone vs face-to-face interviews in the assessment of dietary intake by the 24 h recall EPIC SOFT program—the Norwegian calibration study. Eur J Clin Nutr 2007; 57: 107–113.
Slimani N, Deharveng G, Unwin I, Southgate DA, Vignat J, Skeie G et al. The EPIC nutrient database project (ENDB): a first attempt to standardize nutrient databases across the 10 European countries participating in the EPIC study. Eur J Clin Nutr 2007; 61: 1037–1056.
Besson H, Ekelund U, Luan J, May AM, Sharp S, Travier N et al. A cross-sectional analysis of physical activity and obesity indicators in European participants of the EPIC-PANACEA study. Int J Obes (Lond) 2009; 33: 497–506.
Wareham NJ, Jakes RW, Rennie KL, Schuit J, Mitchell J, Hennings S et al. Validity and repeatability of a simple index derived from the short physical activity questionnaire used in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Public Health Nutr 2003; 6: 407–413.
Agudo A, Slimani N, Ocke MC, Naska A, Miller AB, Kroke A et al. Consumption of vegetables, fruit and other plant foods in the European Prospective Investigation into Cancer and Nutrition (EPIC) cohorts from 10 European countries. Public Health Nutr 2002; 5: 1179–1196.
Trichopoulos D, Hsieh CC, MacMahon B, Lin TM, Lowe CR, Mirra AP et al. Age at any birth and breast cancer risk. Int J Cancer 1983; 31: 701–704.
Miettinen OS . Theoritical Epidemiology: Principles of Occurrence Research in Medicine. Wiley: New York, NY, 1985.
Goldberg GR, Black AE, Jebb SA, Cole TJ, Murgatroyd PR, Coward WA et al. Critical evaluation of energy intake data using fundamental principles of energy physiology: 1. Derivation of cut-off limits to identify under-recording. Eur J Clin Nutr 1991; 45: 569–581.
Bowman SA, Vinyard BT . Fast food consumption of US adults: impact on energy and nutrient intakes and overweight status. J Am Coll Nutr 2004; 23: 163–168.
Jeffery RW, French SA . Epidemic obesity in the United States: are fast foods and television viewing contributing? Am J Public Health 1998; 88 (2): 277–280.
Heitmann BL, Lissner L, Osler M . Do we eat less fat, or just report so? Int J Obes 2000; 24: 435–442.
Lafay L, Basdevant A, Charles MA, Vray M, Balkau B, Borys JM et al. Determinants and nature of dietary underreporting in a free-living population: the Fleurbaix Laventie Ville Sante (FLVS) Study. Int J Obes 1997; 21: 567–573.
Willett WC . Correction for the effects of measurement error. In: Willett WC (ed). Nutritional Epidemiology 2nd edn Oxford University Press: New York, 1998. pp 302–320.
Acknowledgements
This publication arises from the EPIC-PANACEA project, which has received funding from the European Union, in the framework of the Public Health Program (Project Number 2005328). This work was further financially supported by the European Commission: Public Health and Consumer Protection Directorate 1993–2004; Research Directorate-General 2005; Ligue contre le Cancer, Societé 3M, Mutuelle Générale de l'Education Nationale, Institut National de la Santé et de la Recherche Médicale (INSERM) (France); German Cancer Aid, German Cancer Research Center, Federal Ministry of Education and Research (Germany); Danish Cancer Society (Denmark); Health Research Fund (FIS) of the Spanish Ministry of Health, the participating regional governments and institutions and the ISCIII of the Spanish Ministry of Health (RETICC DR06/0020) (Spain); Cancer Research UK, Medical Research Council, Stroke Association, British Heart Foundation, Department of Health, Food Standards Agency, the Wellcome Trust (United Kingdom); Greek Ministry of Health and Social Solidarity, Hellenic Health Foundation and Stavros Niarchos Foundation (Greece); Italian Association for Research on Cancer, National Research Council (Italy); Dutch Ministry of Public Health, Welfare and Sports (VWS), Netherlands Cancer Registry (NKR), LK Research Funds, Dutch Prevention Funds, Dutch ZON (Zorg Onderzoek Nederland), World Cancer Research Fund (WCRF) (The Netherlands); Swedish Cancer Society, Swedish Scientific Council, Regional Government of Skane (Sweden); Nordforsk (Norway).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Naska, A., Orfanos, P., Trichopoulou, A. et al. Eating out, weight and weight gain. A cross-sectional and prospective analysis in the context of the EPIC-PANACEA study. Int J Obes 35, 416–426 (2011). https://doi.org/10.1038/ijo.2010.142
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2010.142
Keywords
This article is cited by
-
Pooled prevalence of food away from home (FAFH) and associated non-communicable disease (NCD) markers: a systematic review and meta-analysis
Journal of Health, Population and Nutrition (2022)
-
Stressed females, rather than males, tend to eat away from home
European Journal of Clinical Nutrition (2022)
-
Energy intake and energy contributions of macronutrients and major food sources among Chinese adults: CHNS 2015 and CNTCS 2015
European Journal of Clinical Nutrition (2021)
-
Walkability and its association with prevalent and incident diabetes among adults in different regions of Germany: results of pooled data from five German cohorts
BMC Endocrine Disorders (2020)
-
Restaurant-based intervention to facilitate healthy eating choices and the identification of allergenic foods at a family-oriented resort and a campground
BMC Public Health (2017)