Abstract
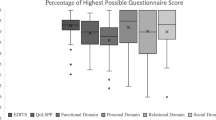
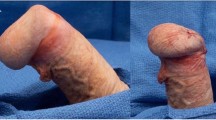
The malleable prosthetic implant is widely accepted among patients and physicians owing to a lower degree of surgical complexity, its rare mechanic failures and lower cost. We have compared the degree of satisfaction with malleable prosthetic implant in 60 patients, 36 with Spectra (AMS) and 24 with Genesis (Coloplast). For assessment purposes, we implemented the Erectile Dysfunction Inventory of Treatment Satisfaction (EDITS) satisfaction questionnaire adapted for penile prosthetic implants. The mean age and follow-up was 61.7 years (31–82) and 19.9 months (1–61), respectively. Mean EDITS scores did not indicate superiority of one implant over the other, overall satisfaction index being 77.1% and 75.6% for Genesis and Spectra prosthesis, respectively (P=0.4970). Our results revealed that these two models of malleable prostheses present a high level of satisfaction and confirm that the malleable prosthetic implant is an excellent option to treat patients with ED refractory to medical treatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Montorsi F, Adaikan G, Becher E, Giuliano F, Khoury S, Lue TF et al. Summary of the recommendations on sexual dysfunctions in men. J Sex Med 2010; 7: 3572–3588.
Vitarelli A, Divenuto L, Fortunato F, Falco A, Pagliarulo V, Antonini G et al. Long term patient satisfaction and quality of life with AMS700CX inflatable penile prosthesis. Arch Ital Urol Androl 2013; 85: 133–137.
Rajpurkar A, Dhabuwala CB . Comparison of satisfaction rates and erectile function in patients treated with Sildenafil, intracavernous prostaglandin E1 and penile implant surgery for erectile dysfunction in urology practice. J Urol 2003; 170: 159–163.
Martinez DR, Terlecki R, Brant W . The evolution and utility of the Small-Carrion prosthesis, its impact, and progression to the modern-day malleable penile prosthesis. J Sex Med 2015; 12 (Suppl 7): 423–430.
Bertero EB, Antunes D . Surgical treatment of erectile dysfunction. Sex Med Rev 2015; 3: 316–327.
Habous M . Malleable (semi-rigid) penile prosthesis. Surgical techniques. J Sex Med 2015; 12: 1984–1988.
Wilson SK, Cleves M, Delk JR 2nd . Long term results with Hydroflex and Dynaflex penile prostheses: device survival comparison to multicomponent inflatables. J Urol 1996; 5: 1621–1623.
Bernal RM, Henry GD . Contemporary patient satisfaction rates for three-piece inflatable penile prostheses. Adv Urol 2012; 2012: 1–5.
Althof SE, Corty EW, Levine SB, Levine F, Burnett AL . EDITS: development of questionnaires for evaluating satisfaction with treatments for erectile dysfunction. Urology 1999; 53: 793–799.
Levine L, Estrada C, Morgentaler A . Mechanical reliability and safety of and patient satisfaction with the Ambicor inflatable penile prosthesis: results of a 2 center study. J Urol 2001; 166: 932–937.
Trost LW, Baum N, Hellstrom WJ . Managing the difficult penile prosthesis patient. J Sex Med 2013; 10: 893–906.
Carvalheira A, Santana R, Pereira N . Why are men satisfied or dissatisfied with penile implants? A mixed method study on satisfaction with penile prosthesis implantation. J Sex Med 2015; 12: 2474–2480.
Natali A, Olianas R, Fisch M . Penile implantation in Europe: successes and complications with 253 implants in Italy and Germany. J Sex Med 2008; 5: 1503–1512.
Salama N . Satisfaction with the malleable penile prosthesis among couples from the Middle East: is it different from that reported elsewhere? Int J Impot Res 2004; 16: 175–180.
Falcone M, Rolle L, Ceruti C, Timpano M, Sedigh O, Preto M et al. Prospective analysis of the surgical outcomes and patients’ satisfaction rate after the AMS Spectra penile prosthesis implantation. Urology 2013; 82: 373–376.
Al Ansari A, Talib R, Canguven O, Shamsodini A . Axial penile rigidity influences patient and partner satisfaction after penile prosthesis implantation. Arch Ital Urol Androl 2013; 85: 138–142.
Mulhall JP, Ahmed A, Branch J, Parker M . Serial assessment of efficacy and satisfaction profiles following penile prosthesis surgery. J Urol 2003; 169: 1429–1433.
Wilson SK, Delk JR 2nd . A new treatment for Peyronie’s disease: modeling the penis over an inflatable penile prosthesis. J Urol 1994; 152: 1121–1123.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Casabé, A., Sarotto, N., Gutierrez, C. et al. Satisfaction assessment with malleable prosthetic implant of Spectra (AMS) and Genesis (Coloplast) models. Int J Impot Res 28, 228–233 (2016). https://doi.org/10.1038/ijir.2016.33
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2016.33
This article is cited by
-
A narrative review on malleable and inflatable penile implants: choosing the right implant for the right patient
International Journal of Impotence Research (2023)
-
Is there still a place for malleable penile implants in the United States? Wilson’s Workshop #18
International Journal of Impotence Research (2023)
-
Current Status for Semirigid Penile Prosthetic Devices
Current Urology Reports (2021)
-
Lebensqualität von Patienten mit hydraulischen penilen Implantaten bei erektiler Dysfunktion in Bezug auf die sexuelle Zufriedenheit des Patienten und seinem/seiner Partner/Partnerin
Der Urologe (2021)
-
Two-piece inflatable and semi-rigid penile implants: an effective alternative?
International Journal of Impotence Research (2020)