Abstract
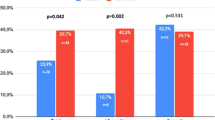
No oral medication has proved to be clearly beneficial for Peyronie's disease (PD). We investigated the safety and efficacy of coenzyme Q10 (CoQ10) supplementation in patients with early chronic PD. We conducted a randomized clinical trial of 186 patients with chronic early PD. Patients were randomly assigned to either 300 mg CoQ10 daily (n=93) or similar regimen of placebo (n=93) for 24 weeks. Erectile function (EF), pain during erection, plaque volume, penile curvature and treatment satisfaction using patient versions of the Erectile Dysfunction Inventory of Treatment Satisfaction (EDITS) questionnaire were assessed at baseline and every 4 weeks during study period. EF was assessed using International Index of Erectile Function (IIEF-5), and pain was evaluated with a visual analog scale (VAS, 0–10). All patients also responded to a Global Assessment Question, ‘Has the treatment you have been taking during this study improved your erections?’ After 24 weeks, mean IIEF-5 score, mean VAS score and mean EDITS score improved significantly in patients receiving CoQ10 (all P<0.01). Mean plaque size and mean penile curvature degree were decreased in the CoQ10 group, whereas a slight increase was noted in the placebo group (both P=0.001). Mean index of IIEF-5 in 24-week treatment period was 17.8±2.7 in the CoQ10 group and 8.8±1.5 in the placebo group (P=0.001). Of the patients in CoQ10 group, 11 (13.6%) had disease progression vs 46 (56.1%) in placebo group (P=0.01). In patients with early chronic PD, CoQ10 therapy leads plaque size and penile curvature reduction and improves EF.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Pryor J, Akkus E, Alter G, Jordan G, Lebret T, Levine L et al. Peyronie's disease. J Sex Med 2004; 1: 110–115.
Lindsay MB, Schain DM, Grambsch P, Benson RC, Beard CM, Kurland LT . The incidence of Peyronie's disease in Rochester, Minnesota, 1950 through 1984. J Urol 1991; 146: 1007–1009.
Savoca G, Trombetta C, Ciampalini S, De Stefani S, Buttazzi L, Belgrano E . Long-term results with Nesbit's procedure as treatment of Peyronie's disease. Int J Impot Res 2000; 12: 289–293.
Erdogru T, Savas M, Yilmaz N, Faruk Usta M, Koksal T, Ates M et al. Evaluation of penile hemodynamic status and adjustment of treatment alternatives in Peyronie's disease. Asian J Androl 2002; 4: 187–190.
Kadioglu A, Tefekli A, Erol B, Oktar T, Tunc M, Tellaloglu S . A retrospective review of 307 men with Peyronie's disease. J Urol 2002; 168: 1075–1079.
Biagiotti G, Cavallini G . Acetyl-Lcarnitine vs tamoxifen in the oral therapy of Peyronie's disease: a preliminary report. BJU Int 2001; 88: 63–67.
Haag SM, Hauck EW, Szardening-Kirchner C, Diemer T, Cha ES, Weidner W et al. Alterations in the transforming growth factor (TGF)-β pathway as a potential factor in the pathogenesis of Peyronie's disease. Eur Urol 2007; 51: 255–261.
Bivilacqua TJ, Champion HC, Hellstrom WJG . Implications of nitric oxide synthase isoforms in the pathophysiology of Peyronie's disease. Int J Impotence Res 2002; 14: 345–352.
Ernster L, Dallner G . Biochemical, physiological and medical aspects of ubiquinone function. Biochim Biophys Acta 1995; 1271: 195–202.
Mukai K, Tokunaga A, Itoh S, Kanesaki Y, Ohara K, Nagaoka S et al. Structure activity relationship of the free-radical-scavenging reaction by vitamin E (α-, β-, γ-, δ-tocopherols) and ubiquinol-10: pH dependence of the reaction rates. J Phys Chem B 2007; 111: 652–662.
Nohl H, Gille L, Kozlov AV . Antioxidant-derived prooxidant formation from ubiquinol. Free Radic Biol Med 1998; 25: 666–675.
Folkers K, Osterborg A, Nylander M, Morita M, Mellstedt H . Activities of vitamin Q10 in animal models and a serious deficiency in patients with cancer. Biochem Biophys Res Commun 1997; 234: 296–299.
Yamamoto Y, Yamashita S, Fujisawa A, Kokura S, Yoshikawa T . Oxidative stress in patients with hepatitis, cirrhosis, and hepatoma evaluated by plasma antioxidants. Biochem Biophys Res Commun 1998; 247: 166–170.
Usta MF, Bivalacqua TJ, Jabren GW, Myers L, Sanabria J et al. Relationship between the severity of penile curvature and the presence of comorbidities in men with Peyronie's disease. J Urol 2004; 171: 775–779.
Hoppe U, Bergemann J, Diembeck W, Ennen J, Gohla S, Harris I et al. Coenzyme Q10, a cutaneous antioxidant and energizer. Biofactors 1999; 9: 371–378.
Choi HK, Pokharel YR, Lim SC, Han HK, Ryu CS, Kim SK et al. Inhibition of liver fibrosis by solubilized coenzyme Q10: role of Nrf2 activation in inhibiting transforming growth factor-beta1 expression. Toxicol Appl Pharmacol 2009; 240: 377–384.
NIH Consensus Development Panel on Impotence. NIH Consensus Conference. Impotence. NIH Consensus Development Panel on Impotence. JAMA 1993; 270: 83–90.
Rosen RC, Capelleri JC, Smith MD . Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile function. Int J Impot Res 1999; 11: 319–326.
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A . The international index of erectile function (IIEF): a multidimensional scale for assessment of erectile function. Urology 1997; 49: 822–830.
Rosen RC, Cappelleri JC, Smith MD, Lipsky J, Pena BM . Development and evaluation of an abridged, 5-item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 1999; 11: 319–326.
Safarinejad MR, Hosseini SY, Kolahi AA . Comparison of vitamin E and propionyl-L-carnitine, separately or in combination, in patients with early chronic Peyronie's disease: a double-blind, placebo controlled, randomized study. J Urol 2007; 178: 1398–1403.
Montorsi F, Guazzoni G, Bergamaschi F, Consonni P, Rigatti P, Pizzini G et al. Vascular abnormalities in Peyronie's disease. The role of color Doppler sonography. J Urol 1994; 151: 373–375.
Wilkins CJ, Sriprasad S, Sidhu PS . Colour Doppler ultrasound of the penis. Clin Radiol 2003; 58: 514–523.
Kelami A . Classification of congenital and acquired penile deviation. Urol Int 1983; 38: 229–233.
Safarinejad MR . Therapeutic effects of colchicine in the management of Peyronie's disease: a randomized double-blind, placebo-controlled study. Int J Impot Res 2004; 16: 238–243.
Althof SE, Corty EW, Levine SB, Levine F, Burnett AL, McVary K et al. EDITS: development of questionnaires for evaluating satisfaction with treatments for erectile dysfunction. Urology 1999; 53: 793–799.
Safarinejad MR . Efficacy and safety of omega-3 for treatment of early-stage Peyronie's disease: a prospective, randomized, double-blind placebo-controlled study. J Sex Med 2009; 6: 1743–1754.
Lewis R, Bennett CJ, Borkon WD, Boykin WH, Althof SE, Stecher VJ et al. Patient and partner satisfaction with Viagra (sildenafil citrate) treatment as determined by the erectile dysfunction inventory of treatment satisfaction questionnaire. Urology 2001; 57: 960–965.
Mulhall JP, Schiff J, Guhring P . An analysis of the natural history of Peyronie's disease. J Urol 2006; 175: 2115–2118.
Hauck EW, Diemer T, Schmelz HU, Weidner W . A critical analysis of nonsurgical treatment of Peyronie's disease. Eur Urol 2006; 49: 987–997.
Rosen R, Catania J, Lue T, Althof S, Henne J, Hellstrom W et al. Impact of Peyronie's disease on sexual and psychosocial functioning: qualitative findings in patients and controls. J Sex Med 2008; 5: 1977–1984.
Kontush A, Reich A, Baum K, Spranger T, Finckh B, Kohlschütter A et al. Plasma ubiquinol-10 is decreased in patients with hyperlipidaemia. Atherosclerosis 1997; 129: 119–126.
Ohhara H, Kanaide H, Yoshimura R . A protective effect of coenzyme Q10 on ischemia and reperfusion of the isolated perfused rat heart. J Mol Cell Cardiol 1981; 13: 65–74.
Arsalane K, Dubois CM, Muanza T, Bégin R, Boudreau F, Asselin C et al. Transforming growth factor-beta1 is a potent inhibitor of glutathione synthesis in the lung epithelial cell line A549: transcriptional effect on the GSH rate-limiting enzyme gamma-glutamylcysteine synthetase. Am J Respir Cell Mol Biol 1997; 17: 599–607.
Kayanoki Y, Fujii J, Suzuki K, Kawata S, Matsuzawa Y, Taniguchi N . Suppression of antioxidative enzyme expression by transforming growth factor beta 1 in rat hepatocytes. J Biol Chem 1994; 269: 15488–15492.
Bakin AV, Stourman NV, Sekhar KR, Rinehart C, Yan X, Meredith MJ et al. Smad3-ATF3 signaling mediates TGF-beta suppression of genes encoding phase II detoxifying proteins. Free Radic Biol Med 2005; 38: 375–387.
Reddy NM, Kleeberger SR, Yamamoto M, Kensler TW, Scollick C, Biswal S et al. Genetic dissection of the Nrf2-dependent redox signaling regulated transcriptional programs of cell proliferation and cytoprotection. Physiol Genomics 2007; 32: 74–81.
Safarinejad MR . Efficacy and safety of omega-3 for treatment of early-stage Peyronie's disease: a prospective, randomized, double-blind placebo controlled study. J Sex Med 2009; 6: 1743–1754.
Ralph D, Brooks M, Botazzi G . The treatment of Peyronie's disease with tamoxifen. Br J Urol 1992; 70: 648–651.
Safarinejad MR, Asgari MA, Hosseini SY, Dadkhah F . A double-blind placebo-controlled study of the efficacy and safety of pentoxifylline in early chronic Peyronie's disease. BJU Int 2009; 106: 240–248.
Acknowledgements
I thank all the participants for their enthusiastic cooperation, which made this study clinically and scientifically relevant. I thank Shiva Safarinejad and Nayyer Shafiei for their excellent technical assistance, and Saba Safarinejad for her advice regarding collection and statistical evaluation of data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no conflict of interest.
Rights and permissions
About this article
Cite this article
Safarinejad, M. Safety and efficacy of coenzyme Q10 supplementation in early chronic Peyronie's disease: a double-blind, placebo-controlled randomized study. Int J Impot Res 22, 298–309 (2010). https://doi.org/10.1038/ijir.2010.20
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijir.2010.20
Keywords
This article is cited by
-
A systematic review of non-surgical management in Peyronieʼs disease
International Journal of Impotence Research (2023)
-
Peyronie’s Disease: A Review of Etiology, Diagnosis, and Management
Current Sexual Health Reports (2015)
-
Update on Medical Management of Peyronie’s Disease
Current Urology Reports (2014)
-
Medical Management of Peyronie’s Disease: a 2014 Update
Current Sexual Health Reports (2014)
-
Krummer Penis macht Sex zur Qual
MMW - Fortschritte der Medizin (2012)