Abstract
The 20q11.2 microdeletion is a rare chromosomal aberration characterized by intellectual disability (ID), motor developmental delay, neonatal feeding problems, and facial dysmorphism. Here, a 2-year- and 6-month-old Japanese girl with a 1.2 Mb microdeletion of 20q11.2 showed ID, motor developmental delay, and distinctive facial features without feeding problems. The deleted region was identified by array-based comparative genomic hybridization and is the smallest reported for a 20q11.2 microdeletion.
Similar content being viewed by others
Interstitial microdeletion of the long arm of chromosome 20 (20q) is a rare condition. Indeed, to the best of our knowledge, 20q11.2 microdeletions, as confirmed by array-based comparative genomic hybridization, have only been found in a few patients.1–4 These patients show intellectual disability (ID), perinatal feeding problems, and facial dysmorphic features. Jedraszak et al.4 suggested the concept of ‘20q11.2 microdeletion syndrome,’ with the responsible genes being GDF5, EPB41L1, and SAMHD1. Here we present a patient with the smallest reported de novo 20q11.2 microdeletion, which does not include GDF5, EPB41L1, or SAMHD1.
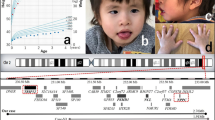
A 2-year and 6-month-old Japanese girl was referred to our hospital, to investigate the cause of her facial dysmorphism and ID. She was the second child from unrelated parents. Her parents and elder brother were healthy. Her gestational age was 36 weeks and her Apgar score was 7 (at 1 min). She showed transient tachypnea and required temporary non-invasive respiratory support. Her birth weight was 2.460 g (50–75th percentile), height was 51.4 cm (>97th percentile), and head circumference was 33 cm (50–75th percentile). She exhibited facial dysmorphic features, namely, bilateral epicanthus, ptosis, a depressed nasal bridge, anteverted nares, and retrognathia. She had global motor developmental delay. She could hold her head up at 7 months, roll over at 9 months, and sit on her own at 12 months but could not stand up at 2 years and 6 months. She had reduced hip abduction and significant constipation without evidence for any organic intestinal disorders such as Hirschsprung disease. She showed no apparent feeding problems and had no growth disturbance. At 2 years and 6 months old, her weight was 12.5 kg (25–50th percentile), height was 88 cm (25–50th percentile), and head circumference was 49.0 cm (50–75th percentile). Her blood tests were normal. Her karyotype, determined by chromosomal G-band testing, was 46, XX. Brain magnetic resonance imaging, electroencephalogram, electrocardiogram, and 24 h Holter electrocardiogram monitoring were all normal. Her total developmental quotient evaluated on the Kyoto Scale of Psychological Development 20015 was 49 (Postural-Motor developmental quotient, 25; Cognitive-Adaptive developmental quotient, 57; and Language-Social developmental quotient 60) at 2 years and 5 months of age. She was unable to speak any significant words at 2 years and 10 months.
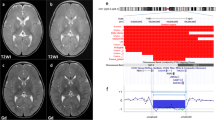
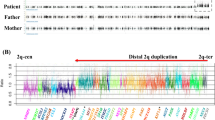
To confirm her molecular diagnosis, we performed array-based comparative genomic hybridization after obtaining written informed consent from her parents. All procedures were reviewed and approved by the Institutional Review Board of Kobe University School of Medicine (86) and Hyogo Prefectural Kobe children’s hospital (28-4), and were in accordance with the ethical standards of the Declaration of Helsinki. We used the Agilent 180 K Human Genome CGH Microarray Platform (Agilent Technologies, Santa Clara, CA) according to the manufacturer’s instructions. We identified an ~1.2 Mb heterozygous deletion on chromosome 20q11.2: arr[GRCh38] 20q11.21q11.22 (32383693_33563791)x1 (Figure 1a). This region includes 21 RefSeq genes: ASXL1, NOL4L, LOC101929698, LOC149950, C20orf203, COMMD7, DNMT3B, MAPRE1, SUN5, BPIFB2, BPIFB6, BPIFB3, BPIFB4, BPIFA2, BPIFA4P, BPIFA3, BPIFA1, BPIFB1, CDK5RAP1, SNTA1, and CBFA2T2 (Figure 1b and Supplementary Table 1). The deletion was not detected in parental samples and therefore shows de novo occurrence.
Chromosomal comparative genomic hybridization (CGH) microarray of the patient. An ~1.2 Mb microdeletion on the long arm of chromosome 20 was identified (a). This region includes 21 RefSeq genes (b). CytoGenomics ver. 4.0.3 (Agilent Technologies) was used to create a, b. Five patients with overlapping deleted regions were compared using the University of California, Santa Cruz (UCSC) Genome Browser (https://genome.ucsc.edu/). The three genes (GDF5, EPB41L1, and SAMHD1) underlined in red were suggested to be the critical genes of 20q11.2 microdeletion syndrome by Jedraszak et al.4 (c). P5, patient 5.
Four patients with deleted regions confirmed by array-based comparative genomic hybridization analysis overlapped with our patient (Figure 1c). Hiraki et al.1 reported a Japanese boy with a 6.5 Mb microdeletion of 20q11.2-q12. He had moderate ID and motor developmental delay, feeding problems, growth disturbance, and retinal dysplasia. Iourov et al.2 reported a boy with mild ID and dysmorphic features, but no growth disturbance. Posmyk et al.3 reported a girl with a 5.7 Mb microdeletion on 20q11.21-q11.23. She had ID, motor developmental delay, growth disturbance, and dysmorphic facial features. Jedraszak et al.4 reported six patients with 20q11.2 microdeletions, with one of the patients (Patient 5) exhibiting a chromosomal deletion on 20q11.21-q11.22. Patient 5 was a 20-year-old woman with mild ID and facial dysmorphism, namely, deep-set eyes and mid-face dysplasia. Of these four patients, our patient has the smallest deletion (Table 1). An additional seven patients with 20q11.2 deletions have been reported by Callier et al.,6 Iqbal and Al-Owain,7 and Jedraszak et al.,4 although the deleted regions do not overlap and were more distal than the region in our patient. Most of these patients showed feeding problems and growth disturbances. Jedraszak et al.4 suggested that the facial appearance of a high forehead, frontal bossing, enophthalmos, and midface hypoplasia are typical features of 20q11.2 microdeletion syndrome, with the 1.62 Mb crucial deleted region including GDF5, EPB41L1, and SAMHD1. The deleted region in our patient does not include these three genes (Figure 1c), but the clinical phenotypes are similar.
In addition, sex combs-like 1 (ASXL1) and syntrophin alpha-1 (SNTA1) are included in the deleted region of our patient as an autosomal dominant disease phenotype (Supplementary Table 1). ASXL1 is the causative gene of Bohring-Opitz syndrome (BOS, #605039), which is characterized by severe ID; prominent eyes; nevi flammei at the forehead, philtrum, or nape of neck; upslanting palpebral fissures; and severe feeding problems.8 BOS usually occurs in patients with ASXL1 nonsense or frameshift variants. The deleted region in our patient includes ASXL1 at the 3′-side marginal region. The patients reported by Iourov and Posmyk have deletions of the entire ASXL1 gene. Iourov et al.2 suggested that the ASXL1 whole gene deletion may cause a milder BOS phenotype. Our patient has deep-set eyes and no growth disturbance, which is distinct from BOS. The precise reason why our patient did not show any facial features such as BOS is not clear, but the ASXL1 truncation may have contributed to her ID and motor developmental delay. SNTA1 encodes a gene that is responsible for long QT syndrome 12 (LQT12, 612955) in an autosomal-dominant manner. LQT12 is a rare disease and all three reported LQT12 patients have SNTA1 missense mutations.9 Our patient does not show any cardiac abnormalities by echocardiogram and 24 h electrocardiogram, but more careful observation of the patient for cardiac problems should be undertaken.
Other genes included in the deleted region might affect her phenotype. DNMT3B (DNA methyltransferase 3β) is the causative gene of immunodeficiency-centromeric instability-facial anomalies syndrome 1, which is an autosomal recessive disorder. Instability-facial anomalies syndrome is characterized by immunodeficiency, chromosome instability, failure to thrive, and mild facial anomalies, which include a flat face, flat nasal bridge, small upturned nose, hypertelorism, epicanthal folds, low-set ears, macroglossia, and micrognathia.10 Our patient showed facial dysmorphic features, but her face was unlike that of instability-facial anomalies syndrome. In addition, she did not show any increased vulnerability to infection and allelic loses of DNMT3B can be benign in some patients.2 CBFA2/RUNX1 translocation partner 2 (CBFA2T2) was partially deleted in our patient and Patient 5 in the study by Jedraszak et al.4 CBFA2T2 is associated with acute myeloid leukemia and recently it has been reported that CBFA2T2 is important for maintaining embryonic stem cell pluripotency via binding to PR domain-containing protein 14.11 The high pLI score (1.00) in ExAC Browser suggests haploinsufficiency of CBFA2T2 (http://exac.broadinstitute.org/gene/ENSG00000078699). The two patients were similar in facial features. The cause of this similarity remains unknown. The role of CBFA2T2 in human germline disorders is still unclear, and further study is essential.
In conclusion, 20q11.2 microdeletion may be a recognizable disorder, but the correlation between phenotype and genotype for this disorder needs further study.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
References
Hiraki Y, Nishimura A, Hayashidani M, Terada Y, Nishimura G, Okamoto N et al. A de novo deletion of 20q11.2-q12 in a boy presenting with abnormal hands and feet, retinal dysplasia, and intractable feeding difficulty. Am J Med Genet A 2011; 155A: 409–414.
Iourov IY, Vorsanova SG, Kurinnaia OS, Yurov YB . An interstitial 20q11.21 microdeletion causing mild intellectual disability and facial dysmorphisms. Case Rep Genet 2013, 353028.
Posmyk R, Lesniewicz R, Gogiel M, Chorazy M, Bakunowicz-Lazarczyk A, Sielicka D et al. The smallest de novo deletion of 20q11.21-q11.23 in a girl with feeding problems, retinal dysplasia, and skeletal abnormalities. Am J Med Genet A 2014; 164A: 1056–1061.
Jedraszak G, Demeer B, Mathieu-Dramard M, Andrieux J, Receveur A, Weber A et al. Clinical and molecular characterization of the 20q11.2 microdeletion syndrome: six new patients. Am J Med Genet A 2015; 167A: 504–511.
Society for the Kyoto Scale of Psychological Development. The Kyoto Scale of Psychological Development 2001: Information for Standardization and Administration. Kyoto Kokusai Shakai Fukushi Center: Kyoto, 2002, in Japanese.
Callier P, Faivre L, Marle N, Thauvin-Robinet C, Sanlaville D, Gosset P et al. Major feeding difficulties in the first reported case of interstitial 20q11.22-q12 microdeletion and molecular cytogenetic characterization. Am J Med Genet A 2006; 140A: 1859–1863.
Iqbal MA, Al-Owain M . Interstitial del(20)(q11.2q12)—clinical and molecular cytogenetic characterization. Am J Med Genet A 2007; 143A: 1880–1884.
Hoischen A, van Bon BW, Rodríguez-Santiago B, Gilissen C, Vissers LE, de Vries P et al. De novo nonsense mutations in ASXL1 cause Bohring-Opitz syndrome. Nat Genet 2011; 43: 729–731.
Alders M, Christiaans I. Long QT Syndrome. 20 February 2003 (updated 18 Jun 2015). In: Pagon RA, Adam MP, Ardinger HH et al. (eds). GeneReviews (Internet). University of Washington, Seattle: Seattle (WA), 1993–2017, Available from https://www.ncbi.nlm.nih.gov/books/NBK1129/.
Weemaes CM, van Tol MJ, Wang J, van Ostaijen-ten Dam MM, van Eggermond MC, Thijssen PE et al. Heterogeneous clinical presentation in ICF syndrome: correlation with underlying gene defects. Eur J Hum Genet 2013; 21: 1219–1225.
Tu S, Narendra V, Yamaji M, Vidal SE, Rojas LA, Wang X et al. Co-repressor CBFA2T2 regulates pluripotency and germline development. Nature 2016; 534: 387–390.
Data Citations
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1663 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1666 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1669 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1672 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1675 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1678 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1681 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1684 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1687 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1690 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1693 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1696 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1699 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1702 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1705 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1708 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1711 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1714 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1717 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1720 (2017)
Morisada, Naoya HGV Database http://dx.doi.org/10.6084/m9.figshare.hgv.1723 (2017)
Acknowledgements
We thank the patient and her family. We also thank Mrs Tetsuko Yamanouchi for her excellent technical assistance and Rachel James, PhD, from the Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information for this article can be found on the Human Genome Variation website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Hanafusa, H., Morisada, N., Ishida, Y. et al. The smallest de novo 20q11.2 microdeletion causing intellectual disability and dysmorphic features. Hum Genome Var 4, 17050 (2017). https://doi.org/10.1038/hgv.2017.50
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/hgv.2017.50
This article is cited by
-
Das Mikrodeletionssyndrom 20q11–q12
Monatsschrift Kinderheilkunde (2020)