Abstract
We describe a 9-year-old male patient with a 15q14 microdeletion including MEIS2. The patient was born with a ventricular septal defect and submucosal cleft. Mild developmental disability and autism spectrum disorder diagnosed in childhood were also considered to be consequences of MEIS2 haploinsufficiency. The relatively mild developmental delay and lack of additional phenotypic features in this patient indicate that only MEIS2 plays an important role in the observed phenotypic features in the heterozygous state.
Similar content being viewed by others
Meis homeobox 2 (MEIS2) is known to contribute to developmental programs. Recently, two patients with de novo MEIS2 mutations have been reported.1,2 Both patients presented cleft palate, congenital heart septal defects and developmental delay. From these findings, MEIS2 was determined to be the gene responsible for chromosome 15q14 deletion syndrome (MIM #616898). We report here an additional patient with a 15q14 microdeletion that involves MEIS2.
The patient is a 9-year-old boy who was born at term, measuring 51 cm in length (+1.0 s.d.), 2,976 g in weight (−0.2 s.d.) and 31 cm in occipitofrontal circumference (OFC) (−1.7 s.d.). Ventricular septal defect (VSD), which was detected through auscultation of heart murmur, later spontaneously closed. Otitis media with effusion was recurrently observed. He did not walk until 20 months, and his language development was delayed. Because of his language delay, he received special education for children with disabilities.
At present, his height is 126.4 cm (−0.6 s.d.), weight is 22.6 kg (−1.0 s.d.) and OFC is 53.5 cm (+0.7 s.d.). His intelligence quotient was evaluated by the Kyoto Scale of Psychological Development. Although there was no abnormality in his motor development, his language development score was 63, indicating mild developmental delay. His speech has a nasal sound caused by a submucosal cleft. Echolalia is frequently observed. Although he can write characters and numbers, he cannot read properly. When he cannot perform tasks according to his expectations, he exhibits behavior such as tantrums, irritability and self-injury. He does not have many friends at school, which might be due to his impaired communication skills. These behaviors suggest characteristics of autism spectrum disorder.
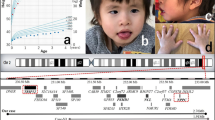
This study was approved by the ethics committee at our institution. After obtaining written informed consent, a blood sample was acquired and genomic DNA was extracted from the patient’s blood. Target resequencing using the TruSight One Sequencing panel (Illumina, San Diego, CA, USA) was performed to detect disease-causing mutations; however, there were no possible disease-causing variants. Subsequently, eXome Hidden Markov Model analysis using a BAM file extracted through next-generation sequencing identified a possible microdeletion in the 15q14 region (Figure 1a,b).3 Microarray chromosomal testing was performed for reconfirmation of the identified finding.3 For this purpose, an Agilent Technologies Catalog 60 K microarray system (Agilent Technologies, Santa Clara, CA, USA) was used. The result showed a 3.17 Mb deletion in the 15q14 region (15q14:34,105,933-37,270,012) [hg19], which is depicted in Figure 1c. The genes involved in the 3.2 Mb deletion region are summarized in Supplementary Table S1. Because parental samples were also analyzed and they did not contain any abnormalities, a de novo origin was considered, although a rare segmental translocation of 15q14 in the parents cannot be excluded.
Genome map around 15q14 with the deletion regions in the reported patients. (a) Region of interest around 15q14 is shown by a red rectangle on the image of chromosome 15, captured from the UCSC genome browser (https://genome.ucsc.edu/). (b) XHMM shows a possible microdeletion in the 15q14 region. The x and y axes indicate the z-scores and genomic positions, respectively. (c) Data were extracted through chromosomal microarray testing. A GeneView created by Agilent Genomic Workbench (Agilent Technologies) is shown. The aberrant region is indicated by a blue transparent rectangle. (d) The locations, regions and directions of the genes are shown. (e) Previously reported deletions are shown with blue rectangles. MEIS2 is partially involved in the deletion region identified in the present patient, which is shown with a red rectangle. XHMM, eXome Hidden Markov Model.
The deletion regions identified in the previously reported patients are depicted in the genome map (Figure 1d,e). The clinical features of this patient are summarized in Table 1 and are compared with those of the previously reported patients with 15q14 deletions4,5,6, 7,8 and MEIS2 mutations.1,2 As shown, various degrees of developmental delay are commonly observed in the patients with MEIS2 haploinsufficiency.2 VSD and cleft palate are also reported in many patients. The present patient showed mild developmental delay. VSD was also identified, although it spontaneously closed later. A submucosal cleft (rather than an open cleft palate) was diagnosed in this patient, and was also reported in the previous patients. On the basis of these findings, most of the clinical features observed in the present patient were considered to be due to MEIS2 haploinsufficiency.
The present patient did not show any symptoms of gastroesophageal reflux, which is reported in patients with nucleotide alterations in MEIS2 (Table 1). The developmental delay in the present patient is milder than the delay commonly reported in patients with MEIS2 mutations. This difference might be due to phenotypic variability.
The relatively mild developmental delay and lack of additional phenotypic features in this patient indicate that the neighboring genes involved in the deletion region do not play important roles in the observed phenotypic features in the heterozygous state. Defects in the actin alpha cardiac muscle 1 gene (ACTC1; MIM #102540) have been associated with idiopathic dilated cardiomyopathy and familial hypertrophic cardiomyopathy in an autosomal dominant trait.9 However, the present patient did not show any related finding, indicating the low penetrance of this gene.
The present patient showed behavior abnormalities related to autism spectrum disorder. Because some patients with MEIS2 haploinsufficiency showed similar features to this disorder (Table 1), our findings might contribute to investigations of this condition.
References
References
Louw JJ, Corveleyn A, Jia Y, Hens G, Gewillig M, Devriendt K . MEIS2 involvement in cardiac development, cleft palate, and intellectual disability. Am J Med Genet A 2015; 167A: 1142–1146.
Fujita A, Isidor B, Piloquet H, Corre P, Okamoto N, Nakashima M et al. De novo MEIS2 mutation causes syndromic developmental delay with persistent gastro-esophageal reflux. J Hum Genet 2016; 61: 835–838.
Yamamoto T, Shimojima K, Ondo Y, Imai K, Chong PF, Kira R et al. Challenges in detecting genomic copy number aberrations using next-generation sequencing data and the eXome Hidden Markov Model: a clinical exome-first diagnostic approach. Hum Genome Var 2016; 3: 16025.
Brunetti-Pierri N, Sahoo T, Frioux S, Chinault C, Zascavage R, Cheung SW et al. 15q13q14 deletions: phenotypic characterization and molecular delineation by comparative genomic hybridization. Am J Med Genet A 2008; 146A: 1933–1941.
Roberti MC, Surace C, Digilio MC, D'Elia G, Sirleto P, Capolino R et al. Complex chromosome rearrangements related 15q14 microdeletion plays a relevant role in phenotype expression and delineates a novel recurrent syndrome. Orphanet J Rare Dis 2011; 6: 17.
Johansson S, Berland S, Gradek GA, Bongers E, de Leeuw N, Pfundt R et al. Haploinsufficiency of MEIS2 is associated with orofacial clefting and learning disability. Am J Med Genet A 2014; 164A: 1622–1626.
Chen CP, Chen CY, Chern SR, Wu PS, Chen YN, Chen SW et al. Prenatal diagnosis and molecular cytogenetic characterization of a de novo 4.858-Mb microdeletion in 15q14 associated with ACTC1 and MEIS2 haploinsufficiency and tetralogy of Fallot. Taiwan J Obstet Gynecol 2016; 55: 270–274.
Crowley MA, Conlin LK, Zackai EH, Deardorff MA, Thiel BD, Spinner NB . Further evidence for the possible role of MEIS2 in the development of cleft palate and cardiac septum. Am J Med Genet A 2010; 152A: 1326–1327.
Olson TM, Michels VV, Thibodeau SN, Tai YS, Keating MT . Actin mutations in dilated cardiomyopathy, a heritable form of heart failure. Science 1998; 280: 750–752.
Data Citations
Yamamoto, Toshiyuki HGV Database (2017) http://dx.doi.org/10.6084/m9.figshare.hgv.1376
Acknowledgements
We are grateful to the patients and their families for their cooperation. This research was supported by the Practical Research Project for Rare/Intractable Diseases from the Japan Agency for Medical Research and Development (AMED) and the Japan Society for the Promotion of Science (JSPS) KAKENHI grant number 15K09631 (TY).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information for this article can be found on the Human Genome Variation website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/4.0/
About this article
Cite this article
Shimojima, K., Ondo, Y., Okamoto, N. et al. A 15q14 microdeletion involving MEIS2 identified in a patient with autism spectrum disorder. Hum Genome Var 4, 17029 (2017). https://doi.org/10.1038/hgv.2017.29
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/hgv.2017.29
This article is cited by
-
MEIS2 (15q14) gene deletions in siblings with mild developmental phenotypes and bifid uvula: documentation of mosaicism in an unaffected parent
Molecular Cytogenetics (2021)
-
Transcriptome analysis of neural progenitor cells derived from Lowe syndrome induced pluripotent stem cells: identification of candidate genes for the neurodevelopmental and eye manifestations
Journal of Neurodevelopmental Disorders (2020)
-
Heterozygous loss-of-function variants of MEIS2 cause a triad of palatal defects, congenital heart defects, and intellectual disability
European Journal of Human Genetics (2019)