Abstract
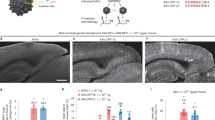
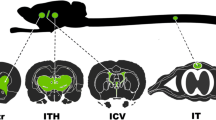
Injection of adeno-associated virus (AAV) into the cerebrospinal fluid (CSF) offers a means to achieve widespread transgene delivery to the central nervous system, where the doses can be readily translated from small to large animals. In contrast to studies with other serotypes (AAV2, AAV4 and AAV5) in rodents, we report that a naturally occurring capsid (AAV9) and rationally engineered capsid (AAV2.5) are able to achieve broad transduction throughout the brain and spinal cord parenchyma following a single injection into the CSF (via cisterna magna or lumbar cistern) in non-human primates (NHP). Using either vector at a dose of ∼2 × 1012 vector genome (vg) per 3–6 kg animal, approximately 2% of the entire brain and spinal cord was transduced, covering all regions of the central nervous system (CNS). AAV9 in particular displayed efficient transduction of spinal cord motor neurons. The peripheral organ biodistribution was highly reduced compared with intravascular delivery, and the presence of circulating anti-AAV-neutralizing antibodies up to a 1:128 titer had no inhibitory effect on CNS gene transfer. Intra-CSF delivery effectively translates from rodents to NHPs, which provides encouragement for the use of this approach in humans to treat motor neuron and lysosomal storage diseases.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Change history
04 April 2013
This article has been corrected since online publication and a corrigendum is also printed in this issue.
References
Duque S, Joussemet B, Riviere C, Marais T, Dubreil L, Douar AM et al. Intravenous administration of self-complementary AAV9 enables transgene delivery to adult motor neurons. Mol Ther 2009; 17: 1187–1196.
Foust KD, Nurre E, Montgomery CL, Hernandez A, Chan CM, Kaspar BK . Intravascular AAV9 preferentially targets neonatal neurons and adult astrocytes. Nat Biotechnol 2009; 27: 59–65.
Gray SJ, Matagne V, Bachaboina L, Yadav S, Ojeda SR, Samulski RJ . Preclinical differences of intravascular AAV9 delivery to neurons and glia: a comparative study of adult mice and nonhuman primates. Mol Ther 2011; 19: 1058–1069.
Gray SJ, Blake BL, Criswell HE, Nicolson SC, Samulski RJ, McCown TJ et al. Directed evolution of a novel adeno-associated virus (AAV) vector that crosses the seizure-compromised blood–brain barrier (BBB). Mol Ther 2010; 18: 570–578.
Samaranch L, Salegio EA, San Sebastian W, Kells AP, Foust KD, Bringas JR et al. Adeno-associated virus serotype 9 transduction in the central nervous system of nonhuman primates. Hum Gene Ther 2012; 23: 382–389.
Davidson BL, Stein CS, Heth JA, Martins I, Kotin RM, Derksen TA et al. Recombinant adeno-associated virus type 2, 4, and 5 vectors: transduction of variant cell types and regions in the mammalian central nervous system. Proc Natl Acad Sci USA 2000; 97: 3428–3432.
Liu G, Martins IH, Chiorini JA, Davidson BL . Adeno-associated virus type 4 (AAV4) targets ependyma and astrocytes in the subventricular zone and RMS. Gene Therapy 2005; 12: 1503–1508.
Ghodsi A, Stein C, Derksen T, Martins I, Anderson RD, Davidson BL . Systemic hyperosmolality improves beta-glucuronidase distribution and pathology in murine MPS VII brain following intraventricular gene transfer. Exp Neurol 1999; 160: 109–116.
Storek B, Harder NM, Banck MS, Wang C, McCarty DM, Janssen WG et al. Intrathecal long-term gene expression by self-complementary adeno-associated virus type 1 suitable for chronic pain studies in rats. Mol Pain 2006; 2: 4.
Towne C, Pertin M, Beggah AT, Aebischer P, Decosterd I . Recombinant adeno-associated virus serotype 6 (rAAV2/6)-mediated gene transfer to nociceptive neurons through different routes of delivery. Mol Pain 2009; 5: 52.
Vulchanova L, Schuster DJ, Belur LR, Riedl MS, Podetz-Pedersen KM, Kitto KF et al. Differential adeno-associated virus mediated gene transfer to sensory neurons following intrathecal delivery by direct lumbar puncture. Mol Pain 2010; 6: 31.
Kao JH, Chen SL, Ma HI, Law PY, Tao PL, Loh HH . Intrathecal delivery of a mutant micro-opioid receptor activated by naloxone as a possible antinociceptive paradigm. J Pharmacol Exp Ther 2010; 334: 739–745.
Snyder BR, Gray SJ, Quach ET, Huang JW, Leung CH, Samulski RJ et al. Comparison of adeno-associated viral vector serotypes for spinal cord and motor neuron gene delivery. Hum Gene Ther 2011; 22: 1129–1135.
Storek B, Reinhardt M, Wang C, Janssen WG, Harder NM, Banck MS et al. Sensory neuron targeting by self-complementary AAV8 via lumbar puncture for chronic pain. Proc Natl Acad Sci USA 2008; 105: 1055–1060.
Federici T, Taub JS, Baum GR, Gray SJ, Grieger JC, Matthews KA et al. Robust spinal motor neuron transduction following intrathecal delivery of AAV9 in pigs. Gene Therapy 2011; 19: 852–859.
Gray SJ, Foti SB, Schwartz JW, Bachaboina L, Taylor-Blake B, Coleman J et al. Optimizing promoters for recombinant adeno-associated virus-mediated gene expression in the peripheral and central nervous system using self-complementary vectors. Hum Gene Ther 2011; 22: 1143–1153.
Bowles DE, McPhee SW, Li C, Gray SJ, Samulski JJ, Camp AS et al. Phase 1 gene therapy for Duchenne muscular dystrophy using a translational optimized AAV vector. Mol Ther 2012; 20: 443–455.
Boutin S, Monteilhet V, Veron P, Leborgne C, Benveniste O, Montus MF et al. Prevalence of serum IgG and neutralizing factors against adeno-associated virus (AAV) types 1, 2, 5, 6, 8, and 9 in the healthy population: implications for gene therapy using AAV vectors. Hum Gene Ther 2010; 21: 704–712.
Swindle MM . Swine in the Laboratory: Surgery, Anesthesia, Imaging, and Experimental Techniques 2nd ed CRC Press Boca Raton, FL, 2007: 471.
Morgan CJ, Pyne-Geithman GJ, Jauch EC, Shukla R, Wagner KR, Clark JF et al. Bilirubin as a cerebrospinal fluid marker of sentinel subarachnoid hemorrhage: a preliminary report in pigs. J Neurosurg 2004; 101: 1026–1029.
Pardridge WM . Transnasal and Intraventricular Delivery of Drugs. Peptide Drug Delivery to the Brain. Raven Press New York, 1991.
Pardridge WM . Drug transport in brain via the cerebrospinal fluid. Fluids Barriers CNS 2011; 8: 7.
Snyder BR, Gray SJ, Quach ET, Huang JW, Leung CH, Samulski RJ et al. Comparison of adeno-associated viral vector serotypes for spinal cord and motor neuron gene delivery. Hum Gene Ther 2011; 22: 1129–1135.
McCarty DM, Fu H, Monahan PE, Toulson CE, Naik P, Samulski RJ . Adeno-associated virus terminal repeat (TR) mutant generates self-complementary vectors to overcome the rate-limiting step to transduction in vivo. Gene Therapy 2003; 10: 2112–2118.
McCarty DM, Monahan PE, Samulski RJ . Self-complementary recombinant adeno-associated virus (scAAV) vectors promote efficient transduction independently of DNA synthesis. Gene Therapy 2001; 8: 1248–1254.
Xiao X, Li J, Samulski RJ . Production of high-titer recombinant adeno-associated virus vectors in the absence of helper adenovirus. J Virol 1998; 72: 2224–2232.
Grieger JC, Choi VW, Samulski RJ . Production and characterization of adeno-associated viral vectors. Nat Protoc 2006; 1: 1412–1428.
Paxinos G, Watson C . The Rat Brain in Stereotaxic Coordinates 6th edn Academic Press/Elsevier Amsterdam; Boston, 2007.
Hylden JL, Wilcox GL . Intrathecal morphine in mice: a new technique. Eur J Pharmacol 1980; 67: 313–316.
Sowa NA, Street SE, Vihko P, Zylka MJ . Prostatic acid phosphatase reduces thermal sensitivity and chronic pain sensitization by depleting phosphatidylinositol 4,5-bisphosphate. J Neurosci 2010; 30: 10282–10293.
Acknowledgements
This work was supported by generous grants from Hannah’s Hope Fund (to SJG), Award Number UL1RR025747 from the National Center for Research Resources (to SJG), the Senator Paul D Wellstone Muscular Dystrophy Cooperative Research Center Grant U54-AR056953 (to RJS), NIH Research Grant 5R01AI072176-05 (to RJS) and NIH Research Grant NS35633 (to TJM), as well as a kind gift from the Jasper Against Batten Foundation at Partnership for Cures (for support of SJG’s research). We are extremely thankful to MPI Research for the quality and timeliness of the work and for help with study design; in particular, we would like to acknowledge the roles of Mark Johnson, Missy Peet and David Serota. We thank the UNC Vector Core, in particular Josh Grieger, for technical assistance with vector production. We also thank Lavanya Bachaboina, Huijing Sun and Erica Jones for help with tissue sectioning and IHC, Brendan Fitzpatrick and Jennifer Coleman in Mark Zylka’s laboratory (UNC) for help with intrathecal mouse injections and Swati Yadav and Hung-Jui ‘Sophia’ Shih for running qPCR reactions. We would also like to acknowledge Jim Wilson’s group at the University of Pennsylvania for the discovery of AAV9, and thank Xiao Xiao at UNC and the UNC Vector Core for providing the AAV9 helper plasmid.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Gene Therapy website
Supplementary information
Rights and permissions
About this article
Cite this article
Gray, S., Nagabhushan Kalburgi, S., McCown, T. et al. Global CNS gene delivery and evasion of anti-AAV-neutralizing antibodies by intrathecal AAV administration in non-human primates. Gene Ther 20, 450–459 (2013). https://doi.org/10.1038/gt.2012.101
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gt.2012.101
Keywords
This article is cited by
-
Assessment of AAV9 distribution and transduction in rats after administration through Intrastriatal, Intracisterna magna and Lumbar Intrathecal routes
Gene Therapy (2023)
-
AAV-based in vivo gene therapy for neurological disorders
Nature Reviews Drug Discovery (2023)
-
Extension of the Lifespan of a Mouse Model of Rett Syndrome by Intracerebroventricular Delivery of MECP2
Neuroscience Bulletin (2023)
-
Adeno-associated viral vectors for functional intravenous gene transfer throughout the non-human primate brain
Nature Nanotechnology (2023)
-
Human in silico trials for parametric computational fluid dynamics investigation of cerebrospinal fluid drug delivery: impact of injection location, injection protocol, and physiology
Fluids and Barriers of the CNS (2022)