Abstract
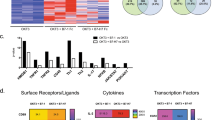
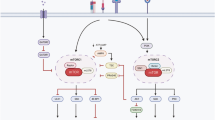
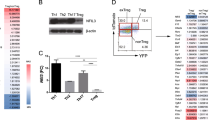
Transforming growth factor-β (TGF-β) maintains self-tolerance through a constitutive inhibitory effect on T-cell reactivity. In most physiological situations, the tolerogenic effects of TGF-β depend on the canonical signaling molecule Smad3. To characterize how TGF-β/Smad3 signaling contributes to maintenance of T-cell tolerance, we characterized the transcriptional landscape downstream of TGF-β/Smad3 signaling in resting or activated CD4 T cells. We report that in the presence of TGF-β, Smad3 modulates the expression of >400 transcripts. Notably, we identified 40 transcripts whose expression showed Smad3 dependence in both resting and activated cells. This ‘signature’ confirmed the non-redundant role of Smad3 in TGF-β biology and identified both known and putative immunoregulatory genes. Moreover, we provide genomic and functional evidence that the TGF-β/Smad3 pathway regulates T-cell activation and metabolism. In particular, we show that TGF-β/Smad3 signaling dampens the effect of CD28 stimulation on T-cell growth and proliferation. The impact of TGF-β/Smad3 signals on T-cell activation was similar to that of the mTOR inhibitor Rapamycin. Considering the importance of co-stimulation on the outcome of T-cell activation, we propose that TGF-β-Smad3 signaling may maintain T-cell tolerance by suppressing co-stimulation-dependent mobilization of anabolic pathways.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Accession codes
Change history
07 March 2013
This article has been corrected since Advance Online Publication and an erratum is also printed in this issue.
References
Newfeld SJ, Wisotzkey RG, Kumar S . Molecular evolution of a developmental pathway: phylogenetic analyses of transforming growth factor-beta family ligands, receptors and Smad signal transducers. Genetics 1999; 152: 783–795.
Schmierer B, Hill CS . TGFbeta-SMAD signal transduction: molecular specificity and functional flexibility. Nat Rev Mol Cell Biol 2007; 8: 970–982.
Li MO, Wan YY, Sanjabi S, Robertson AK, Flavell RA . Transforming growth factor-beta regulation of immune responses. Annu Rev Immunol 2006; 24: 99–146.
Li MO, Flavell RA . TGF-beta: a master of all T cell trades. Cell 2008; 134: 392–404.
Gorelik L, Flavell RA . Abrogation of TGFbeta signaling in T cells leads to spontaneous T cell differentiation and autoimmune disease. Immunity 2000; 12: 171–181.
Letterio JJ, Geiser AG, Kulkarni AB, Dang H, Kong L, Nakabayashi T et al. Autoimmunity associated with TGF-beta1-deficiency in mice is dependent on MHC class II antigen expression. J Clin Invest 1996; 98: 2109–2119.
Marie JC, Liggitt D, Rudensky AY . Cellular mechanisms of fatal early-onset autoimmunity in mice with the T cell-specific targeting of transforming growth factor-beta receptor. Immunity 2006; 25: 441–454.
Zhang N, Bevan MJ . TGF-beta signaling to T cells inhibits autoimmunity during lymphopenia-driven proliferation. Nat Immunol 2012; 13: 667–673.
Classen S, Zander T, Eggle D, Chemnitz JM, Brors B, Buchmann I et al. Human resting CD4+ T cells are constitutively inhibited by TGF beta under steady-state conditions. J Immunol 2007; 178: 6931–6940.
Feng XH, Derynck R . Specificity and versatility in tgf-beta signaling through Smads. Annu Rev Cell Dev Biol 2005; 21: 659–693.
Letterio JJ . TGF-beta signaling in T cells: roles in lymphoid and epithelial neoplasia. Oncogene 2005; 24: 5701–5712.
Li L, Iwamoto Y, Berezovskaya A, Boussiotis VA . A pathway regulated by cell cycle inhibitor p27Kip1 and checkpoint inhibitor Smad3 is involved in the induction of T cell tolerance. Nat Immunol 2006; 7: 1157–1165.
Maggio-Price L, Treuting P, Zeng W, Tsang M, Bielefeldt-Ohmann H, Iritani BM . Helicobacter infection is required for inflammation and colon cancer in SMAD3-deficient mice. Cancer Res 2006; 66: 828–838.
Giroux M, Delisle JS, Gauthier SD, Heinonen KM, Hinsinger J, Houde B et al. SMAD3 prevents graft-versus-host disease by restraining Th1 differentiation and granulocyte-mediated tissue damage. Blood 2011; 117: 1734–1744.
Giroux M, Delisle JS, O’Brien A, Hebert MJ, Perreault C . T cell activation leads to protein kinase C theta-dependent inhibition of TGF-beta signaling. J Immunol 2010; 185: 1568–1576.
Tone Y, Furuuchi K, Kojima Y, Tykocinski ML, Greene MI, Tone M . Smad3 and NFAT cooperate to induce Foxp3 expression through its enhancer. Nat Immunol 2008; 9: 194–202.
Iwashima M . Kinetic perspectives of T cell antigen receptor signaling. A two-tier model for T cell full activation. Immunol Rev 2003; 191: 196–210.
Rutz S, Noubade R, Eidenschenk C, Ota N, Zeng W, Zheng Y et al. Transcription factor c-Maf mediates the TGF-beta-dependent suppression of IL-22 production in T(H)17 cells. Nat Immunol 2011; 12: 1238–1245.
Zou L, Barnett B, Safah H, Larussa VF, Evdemon-Hogan M, Mottram P et al. Bone marrow is a reservoir for CD4+CD25+ regulatory T cells that traffic through CXCL12/CXCR4 signals. Cancer Res 2004; 64: 8451–8455.
Sugita S, Horie S, Nakamura O, Maruyama K, Takase H, Usui Y et al. Acquisition of T regulatory function in cathepsin L-inhibited T cells by eye-derived CTLA-2alpha during inflammatory conditions. J Immunol 2009; 183: 5013–5022.
Solomon BD, Mueller C, Chae WJ, Alabanza LM, Bynoe MS . Neuropilin-1 attenuates autoreactivity in experimental autoimmune encephalomyelitis. Proc Natl Acad Sci USA 2011; 108: 2040–2045.
Ondr JK, Pham CT . Characterization of murine cathepsin W and its role in cell-mediated cytotoxicity. J Biol Chem 2004; 279: 27525–27533.
Harada Y, Elly C, Ying G, Paik JH, Depinho RA, Liu YC . Transcription factors Foxo3a and Foxo1 couple the E3 ligase Cbl-b to the induction of Foxp3 expression in induced regulatory T cells. J Exp Med 2010; 207: 1381–1391.
Subramanian A, Tamayo P, Mootha VK, Mukherjee S, Ebert BL, Gillette MA et al. Gene set enrichment analysis: a knowledge-based approach for interpreting genome-wide expression profiles. Proc Natl Acad Sci USA 2005; 102: 15545–15550.
Jones RG, Thompson CB . Revving the engine: signal transduction fuels T cell activation. Immunity 2007; 27: 173–178.
Araki K, Turner AP, Shaffer VO, Gangappa S, Keller SA, Bachmann MF et al. mTOR regulates memory CD8 T-cell differentiation. Nature 2009; 460: 108–112.
Chi H . Regulation and function of mTOR signalling in T cell fate decisions. Nat Rev Immunol 2012; 12: 325–338.
Powell JD, Pollizzi KN, Heikamp EB, Horton MR . Regulation of immune responses by mTOR. Annu Rev Immunol 2012; 30: 39–68.
Pearce EL, Walsh MC, Cejas PJ, Harms GM, Shen H, Wang LS et al. Enhancing CD8 T-cell memory by modulating fatty acid metabolism. Nature 2009; 460: 103–107.
Fox CJ . Hammerman PS & Thompson CB. Fuel feeds function: energy metabolism and the T-cell response. Nat Rev Immunol 2005; 5: 844–852.
Zheng Y, Delgoffe GM, Meyer CF, Chan W, Powell JD . Anergic T cells are metabolically anergic. J Immunol 2009; 183: 6095–6101.
Gerriets VA, Rathmell JC . Metabolic pathways in T cell fate and function. Trends Immunol 2012; 33: 168–173.
Mondino A, Mueller DL . mTOR at the crossroads of T cell proliferation and tolerance. Semin Immunol 2007; 19: 162–172.
Song J, Salek-Ardakani S, So T, Croft M . The kinases aurora B and mTOR regulate the G1-S cell cycle progression of T lymphocytes. Nat Immunol 2007; 8: 64–73.
Gudmundsdottir H, Wells AD, Turka LA . Dynamics and requirements of T cell clonal expansion in vivo at the single-cell level: effector function is linked to proliferative capacity. J Immunol 1999; 162: 5212–5223.
McKarns SC, Schwartz RH . Distinct effects of TGF-beta 1 on CD4+ and CD8+ T cell survival, division, and IL-2 production: a role for T cell intrinsic Smad3. J Immunol 2005; 174: 2071–2083.
Rathmell JC, Elstrom RL, Cinalli RM, Thompson CB . Activated Akt promotes increased resting T cell size, CD28-independent T cell growth, and development of autoimmunity and lymphoma. Eur J Immunol 2003; 33: 2223–2232.
Dowling RJ, Topisirovic I, Alain T, Bidinosti M, Fonseca BD, Petroulakis E et al. mTORC1-mediated cell proliferation, but not cell growth, controlled by the 4E-BPs. Science 2010; 328: 1172–1176.
Caron E, Vincent K, Fortier MH, Laverdure JP, Bramoulle A, Hardy MP et al. The MHC I immunopeptidome conveys to the cell surface an integrative view of cellular regulation. Mol Syst Biol 2011; 7: 533.
Choo AY, Yoon SO, Kim SG, Roux PP, Blenis J . Rapamycin differentially inhibits S6Ks and 4E-BP1 to mediate cell-type-specific repression of mRNA translation. Proc Natl Acad Sci USA 2008; 105: 17414–17419.
Baron C, Somogyi R, Greller LD, Rineau V, Wilkinson P, Cho CR et al. Prediction of graft-versus-host disease in humans by donor gene-expression profiling. PLoS Med 2007; 4: 69–83.
Park D, Estevez A, Riddle DL . Antagonistic Smad transcription factors control the dauer/non-dauer switch in C. elegans. Development 2010; 137: 477–485.
Rahimi RA, Andrianifahanana M, Wilkes MC, Edens M, Kottom TJ, Blenis J et al. Distinct roles for mammalian target of rapamycin complexes in the fibroblast response to transforming growth factor-beta. Cancer Res 2009; 69: 84–93.
Wu L, Derynck R . Essential role of TGF-beta signaling in glucose-induced cell hypertrophy. Dev Cell 2009; 17: 35–48.
Sartori R, Milan G, Patron M, Mammucari C, Blaauw B, Abraham R et al. Smad2 and 3 transcription factors control muscle mass in adulthood. Am J Physiol Cell Physiol 2009; 296: C1248–C1257.
Chabanon A, Desterke C, Rodenburger E, Clay D, Guerton B, Boutin L et al. A cross-talk between stromal cell-derived factor-1 and transforming growth factor-beta controls the quiescence/cycling switch of CD34(+) progenitors through FoxO3 and mammalian target of rapamycin. Stem Cells 2008; 26: 3150–3161.
Delgoffe GM, Kole TP, Zheng Y, Zarek PE, Matthews KL, Xiao B et al. The mTOR kinase differentially regulates effector and regulatory T cell lineage commitment. Immunity 2009; 30: 832–844.
Song K, Cornelius SC, Reiss M, Danielpour D . Insulin-like growth factor-I inhibits transcriptional responses of transforming growth factor-beta by phosphatidylinositol 3-kinase/Akt-dependent suppression of the activation of Smad3 but not Smad2. J Biol Chem 2003; 278: 38342–38351.
Song K, Wang H, Krebs TL, Danielpour D . Novel roles of Akt and mTOR in suppressing TGF-beta/ALK5-mediated Smad3 activation. EMBO J 2006; 25: 58–69.
Remy I, Montmarquette A, Michnick SW . PKB/Akt modulates TGF-beta signalling through a direct interaction with Smad3. Nat Cell Biol 2004; 6: 358–365.
Akdis CA, Joss A, Akdis M, Faith A, Blaser K . A molecular basis for T cell suppression by IL-10: CD28-associated IL-10 receptor inhibits CD28 tyrosine phosphorylation and phosphatidylinositol 3-kinase binding. FASEB J 2000; 14: 1666–1668.
Joss A, Akdis M, Faith A, Blaser K, Akdis CA . IL-10 directly acts on T cells by specifically altering the CD28 co-stimulation pathway. Eur J Immunol 2000; 30: 1683–1690.
Hedrick SM, Hess Michelini R, Doedens AL, Goldrath AW, Stone EL . FOXO transcription factors throughout T cell biology. Nat Rev Immunol 2012; 12: 649–661.
van der Windt GJ, Everts B, Chang CH, Curtis JD, Freitas TC, Amiel E et al. Mitochondrial respiratory capacity is a critical regulator of CD8+ T cell memory development. Immunity 2012; 36: 68–78.
Boussiotis VA, Chen ZM, Zeller JC, Murphy WJ, Berezovskaya A, Narula S et al. Altered T-cell receptor+CD28-mediated signaling and blocked cell cycle progression in interleukin 10 and transforming growth factor-beta-treated alloreactive T cells that do not induce graft-versus-host disease. Blood 2001; 97: 565–571.
Chen CH, Seguin-Devaux C, Burke NA, Oriss TB, Watkins SC, Clipstone N et al. Transforming growth factor beta blocks Tec kinase phosphorylation, Ca2+ influx, and NFATc translocation causing inhibition of T cell differentiation. J Exp Med 2003; 197: 1689–1699.
Smyth GK . Linear models and empirical Bayes methods for assessing differential expression in microarray experiments. Stat Appl Genet Mol Biol 2004; 3: 1544–6115.
Baron C, Meunier MC, Caron E, Cote C, Cameron MJ, Kelvin DJ et al. Asynchronous differentiation of CD8 T cells that recognize dominant and cryptic antigens. J Immunol 2006; 177: 8466–8475.
Saeed AI, Sharov V, White J, Li J, Liang W, Bhagabati N et al. TM4: a free, open-source system for microarray data management and analysis. Biotechniques 2003; 34: 374–378.
Edgar R, Domrachev M, Lash AE . Gene Expression Omnibus: NCBI gene expression and hybridization array data repository. Nucleic Acids Res 2002; 30: 207–210.
Acknowledgements
This work was supported through grants held by JSD (Leukemia/lymphoma society of Canada (LLSC) and the Maisonneuve-Rosemont hospital foundation) as well as by an LLSC grant to CP. JSD holds a career award from the Fonds de recherche du Québec-Santé (FRQS) and Claude Perreault holds a Canada research chair in immunobiology. We would like to thank the animal care facility personnel both at the IRIC and CR-HMR as well as Danièle Gagné, Gaël Dulude and Martine Dupuis for cell sorting.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Genes and Immunity website
Rights and permissions
About this article
Cite this article
Delisle, JS., Giroux, M., Boucher, G. et al. The TGF-β-Smad3 pathway inhibits CD28-dependent cell growth and proliferation of CD4 T cells. Genes Immun 14, 115–126 (2013). https://doi.org/10.1038/gene.2012.63
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gene.2012.63
Keywords
This article is cited by
-
A critical role for Th17 cell-derived TGF-β1 in regulating the stability and pathogenicity of autoimmune Th17 cells
Experimental & Molecular Medicine (2021)
-
Immunosuppressive network promotes immunosenescence associated with aging and chronic inflammatory conditions
Journal of Molecular Medicine (2021)
-
The induction and function of the anti-inflammatory fate of TH17 cells
Nature Communications (2020)
-
Impact of fecal microbiota transplantation on TGF-β1/Smads/ERK signaling pathway of endotoxic acute lung injury in rats
3 Biotech (2020)
-
Immunosenescence is both functional/adaptive and dysfunctional/maladaptive
Seminars in Immunopathology (2020)