Abstract
Purpose To determine whether the outcome of primary retinal reattachment surgery in a subregion is improved by surgery being performed in a specialist vitreoretinal unit (VRU).
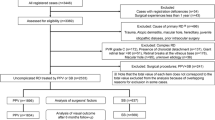
Methods A subregional, population-based, retrospective audit cycle of primary retinal reattachment surgery was conducted by independent investigators. The subregion was defined as the catchment area of a teaching hospital (TH) with a specialist VRU and three neighbouring district general hospitals (DGHs). During the initial audit period (January 1989 to December 1990), 142 cases were treated at all four hospitals: THNRU (83), DGH-A (15), DGH-B (13), and DGH-C (31). Policy changes after the initial audit led to primary retinal reattachment surgery being predominantly performed by the VRU. During the re-audit period (September 1995 to August 1997), 160 cases were treated at two hospitals: VRU (148) and DGH-C (12). The outcome measure employed was complete retinal reattachment after a single procedure with a minimum follow-up of 12 months. Results The success rate for primary retinal reattachment surgery in the subregion improved from 76.1% to 88.8% (p = 0.006) following the policy changes. The success rate of the vitreoretinal specialists in the VRU (90%) was greater than the general ophthalmologists in the DGHs (ranging from 47% to 77%), despite case selection by the general ophthalmologists. The number of cases treated by the VRU increased by 156% in the 6.5 year interval between the two audits due to a widespread change in the model of care for primary retinal detachments (both within and outside the subregion). During the re-audit period, the VRU treated 348 primary retinal detachments (including referrals from outside the subregion), achieving a success rate of 86.8% with a single procedure and 97.4% with further surgery. This primary success rate included 35 cases (10%) treated by vitrectomy with silicone oil tamponade who did not undergo silicone oil removal. Conclusions The outcome of primary retinal reattachment surgery can be improved if surgery is performed by a specialist VRU. It is suggested that the current standard for retinal reattachment with a single procedure should be set in the region of 85% to 90%. Changing the model of care so that primary retinal reattachment surgery is predominantly performed by a specialist VRU has important resource implications.
Similar content being viewed by others
Article PDF
References
Duke-Elder S, Dobree JH . Detachment and folding of the retina. In: Duke-Elder S, editor. System of ophthalmology, vo1. 10. Diseases of the retina. St Louis: Mosby-Year Book, 1967:771.
Conin J . Le décollement de la rétine. Lausanne: Payot et Cie, 1934.
Schepens CL . A new ophthalmoscope demonstration. Trans Am Acad Ophthalmol Otolaryngol 1947;51:298.
Custodis E . Die Behandlung der Netzhautablosung durch umschriebene Diathermiekoagulation und einer mittels Plombenaufnahung erzeugten Eindellung der Sklera im Bereich des Risses. Klin Monatsbl Augenheilkd 1956;129:476.
Cibis PA, Becker B, Okun E, Canaan S . The use of liquid silicone in retinal reattachment surgery. Arch Ophthalmol 1962;68:590–9
Norton EW . Intraocular gas in the management of selected retinal detachments. Trans Am Acad Ophthalmol Otolaryngol 1973;77:85–98
Machemer R, Buettner H, Norton EW, Parel JM . Vitrectomy: a pars plana approach. Trans Am Acad Ophthalmol Otolaryngol 1971;75:813.
Wilkinson CP, Rice TA . Michels retinal detachment, 2nd ed. St Louis: Mosby, 1997.
Chignell AH, Fison LG, Davies EW, Hartley RE, Gundry MF . Failure in retinal detachment surgery. Br J Ophthalmol 1973;57:525–30
Rachal WF, Burton TC . Changing concepts of failures after retinal detachment surgery. Arch Ophthalmol 1979;97:480–3
Grizzard WS, Hilton GF, Hammer ME, Taren D . A multivariate analysis of anatomic success of retinal detachments treated with scleral buckling. Graefes Arch Clin Exp Ophthalmol 1994;232:1–7
Hilton GF, McLean EB, Brinton DA . Retinal detachment: principles and practice, 2nd ed. San Francisco: American Academy of Ophthalmology, 1995.
Tornquist R, Tornquist P . Retinal detachment: a study of a population-based patient material in Sweden 1971-1981. III. Surgical results. Acta Ophthalmol 1988;66:630–6
Laatikainen L, Harju H, Tolppanen EM . Post-operative outcome in rhegmatogenous retinal detachment. Acta Ophthalmol 1985;63:647–55
Wilkinson CP, Bradford RH . Complications of draining subretinal fluid. Retina 1984;4:1–4
Sharma T, Challa JK, Ravishankar KV, Murugesan R . Scleral buckling for retinal detachment: predictors for anatomic failure. Retina 1994;14:338–43
Sullivan PM, Luff AJ, Aylward GW . Results of primary retinal reattachment surgery: a prospective audit. Eye 1997;11:869–71
George ND, Callear AB, Halkias A, Ruigrok A . Moore AT. Should all primary retinal detachments be referred to a specialist vitreoretinal unit for surgery? Presented at the Royal College of Ophthalmologists Annual Congress, 1994.
The Retina Society Terminology Committee. The classification of retinal detachment with proliferative vitreoretinopathy. Ophthalmology 1983;90:121–5
Irvine D, Irvine S, editors. How to do it: data and methods 1. In: Making sense of audit. Oxford: Radcliffe Medical Press, 1991:55.
Roethlisberger FJ, Dickson WJ . In: Management and the worker. An account of a research program conducted by the Western Electric Company, Hawthorne Works, Chicago. Cambridge, MA: Harvard University Press, 1943:526–8.
Leaver PK . Retinal detachments: when to refer. Identifying the complicated case. Eye 1989;3:754–8
Leaver P . Expanding the role of vitrectomy in retinal reattachment surgery. Br J Ophthalmol 1993;77:197.
The Silicone Study Group. Vitrectomy with silicone oil or perfluoropropane gas in eyes with severe proliferative vitreoretinopathy: results of a randomised clinical trial. Silicone Study Report 2. Arch Ophthalmol 1992;110:780–92
Billington BM, Leaver PK . Vitrectomy and fluid/silicone oil exchange for giant retinal tears: results at 18 months. Graefes Arch Clin Exp Ophthalmol 1986;224:7–10
Gonvers M, Machemer R . A new approach to treating retinal detachments with macular hole. Am J Ophthalmol 1982;94:468–72
Gartry DS, Chignell AH, Franks WA, Wong D . Pars plana vitrectomy for the treatment of rhegmatogenous retinal detachment uncomplicated by advanced proliferative vitreoretinopathy. Br J Ophthalmol 1993;77:199–203
Hakin KN, Lavin MJ, Leaver PK . Primary vitrectomy for rhegmatogenous retinal detachment. Graefes Arch Clin Exp Ophthalmol 1993;231:344–6
Wong D, Billington BM, Chignell AH . Pars plana vitrectomy for retinal detachment with unseen retinal holes. Graefes Arch Clin Exp Ophthalmol 1987;225:269–71
Bartz-Schmidt KU, Kirchhof B, Heimann K . Primary vitrectomy for pseudophakic retinal detachment. Br J Ophthalmol 1996;80:346–9
Scott JD . Silicone oil as an instrument. In: Ryan SJ, editor. Retina, vol 3. St Louis: CV Mosby, 1994:2181–9.
Wong D, McGalliard J . Are we getting better at treating retinal detachment? Technology, referral pattern or primary care? Eye 1997:11:763–70.
Ramsay A, Cottrell DC . Triple cycle audit of retinal detachment surgery. Presented at the Royal College of Ophthalmologists Audit Meeting, 1998.
Author information
Authors and Affiliations
Additional information
Funding: None
Proprietary or financial interests: None
Rights and permissions
About this article
Cite this article
Comer, M., Newman, D., George, N. et al. Who should manage primary retinal detachments?. Eye 14, 572–578 (2000). https://doi.org/10.1038/eye.2000.145
Received:
Revised:
Issue Date:
DOI: https://doi.org/10.1038/eye.2000.145
Keywords
This article is cited by
-
Ablatiochirurgie: Trends über 15 Jahre
Der Ophthalmologe (2022)
-
The learning curve of retinal detachment surgery
Graefe's Archive for Clinical and Experimental Ophthalmology (2021)
-
Controlled drainage of subretinal fluid during scleral buckling surgery for rhegmatogenous retinal detachment: the pigment stream sign
International Ophthalmology (2019)
-
Surgeon age and operative outcomes for primary rhegmatogenous retinal detachment: a 3-year nationwide population-based study
Eye (2010)
-
Trends and outcomes of treatment for primary rhegmatogenous retinal detachment: a 9-year nationwide population-based study
Eye (2009)