Abstract
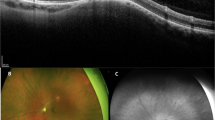
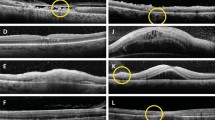
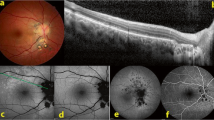
The clinical course of 47 patients with posterior scleritis is reviewed. Though clinical presentation varied widely, 73% of the patients presented with a visual acuity of 6/18 or less. Because the posterior scleritis was not always associated with pain or with anterior scleritis, the diagnosis was often not considered when the patient was first seen. The most common findings in the fundus were disc swelling, retinal detachment, and macular oedema and the most useful investigation was B scan ultrasound. No common aetiology was found, although 60% had a systemic disorder which was accompanied by a vasculitis. Those who were diagnosed and treated with the minimum delay had the most satisfactory visual outcome. However, there appears to be a group of patients with no underlying systemic disease who fail to respond to intensive therapy, and lose vision. A new sub-group of West Indians with the disease is described. The histopathology of 7 cases confirmed the presence of scleral vasculitis of the vessels in and around the sclera in all the specimens. Other significant findings include inflammatory swelling and focal loss of pigment epithelium together with choroidal vascular closure. This could account for the fluorescein angiographic findings.
Similar content being viewed by others
Article PDF
References
Chavis RM, Garner A, Wright JE : Inflammatory Orbital pseudotumour. A clinico-pathologic study. Arch ophthalmol 1978; 96: 1817–22.
Rootman J, and Nugent R : The classification and management of acute orbital pseudotumours. Ophthalmol 1982; 89: 1040–8
Bertelsen TI : Acute sclerotenonitis and ocular myositis complicated by papillitis, retinal detachment and glaucoma. Acta Ophthalmol 1960; 38: 136–52.
Watson PG : The nature and treatment of scleral inflammation. Trans Ophthalmol Soc UK 1982; 102: 257–81.
Benson WE, Shields JA, Tasman W, Crandall AS : Posterior Scleritis. A cause of diagnostic confusion. Arch Ophthalmol 1979; 97: 1482–6.
Fraunfelder FT and Watson PG : Evaluation of eyes enucleated for scleritis. Br J Ophthalmol 1976; 60: 227–30.
Sears ML : Choroidal and retinal detachments associated with scleritis. Am J Ophthalmol 1964; 58, 764–6.
Feldon SE, Singleman J, Albert DM, Smith TR : Clinical manifestations of brawny scleritis. Am J Ophthalmol 1978; 85: 781–7.
Yeo JH, Jakobiec FA, Iwamoto T, Brown R, Harrison W : Metastatic carcinoma masquerading as scleritis. Ophthalmology 1983; 90: 184–94.
Watson PG and Hayreh SS : Scleritis and episcleritis. Br J Ophthalmol 1976; 60: 163–91.
McGavin DDM, Williamson J, Forrester JV, Foulds WS, et al: Episcleritis and scleritis: a study of their clinical manifestations and association with rheumatoid arthritis. Br J Ophthalmol 1976; 60: 192–233.
Singh G, Guthoff R, Foster CS : Observations on longterm follow-up of posterior scleritis. Am J Ophthalmol 1986; 101: 570–5.
Quinlan MP and Hitchings RA : Angle-closure glaucoma secondary to posterior scleritis. Br J Ophthalmol 1978; 62: 330–5.
Wilhelmus KR, Grierson I, Watson PG : Histopathologic and clinical associations of scleritis and glaucoma. Am J Ophthalmol 1981; 91: 697–705.
Cleary PE, Watson PG, McGill JI, Hamilton AM : Visual loss due to posterior segment disease in scleritis. Trans Ophthalmol Soc UK 1975; 95: 297–300.
Berger B and Reeser F : Retinal pigment epithelial detachments in posterior scleritis. Am J Ophthalmol 1980; 90: 604–6.
Cappaert WE, Purnell EW, Frank KE . Use of B-Sector scan ultrasound in the diagnosis of benign choroidal folds. Am J Ophthalmol 1977; 84: 375–9.
Rocheis R and Reis G : Echographie bei skleritis posterior. Klin Mbl Augenheilk 1980; 177: 611–13.
Foster CS : Immunosuppressive therapy for external ocular inflammatory disease. Ophthalmol 1980; 87: 140–9.
Wakefield D, McCluskey P, Penny R . Intravenous pulse Methylprednisolone therapy in severe inflammatory eye disease. Arch Ophthalmol 1986; 104: 847–51.
McCluskey P and Wakefield D : Intravenous Pulse Methylprednisolone in Scleritis. Arch Ophthalmol 1987; 105: 793–7.
Myer PA, Watson PG, Franks W, Dubord P . ‘Pulsed‘ Immunosuppressive Therapy in the treatment of immunologically induced corneal and scleral disease. Eye 1987; 1: 487–95.
Young RD and Watson PG : Microscopical studies of necrotising scleritis. 1. Cellular aspects. Br J Ophthalmol 1984; 6: 770–80.
Askenase PW and Van Loveren H : Delayed-type hypersensitivity: activation of mast cells by antigen specific T-cell factors initiates the cascade of cellular interactions. Immunology Today 1983; 4: 259–64.
Young RD and Watson PG : Microscopical studies of necrotising scleritis. 11. Collagen degradation in the scleral stroma. Br J Ophthalmol 1984; 68: 781–9.
Sevel D : Necrogranulomatous scleritis: clinical and histological features. Am J Ophthalmol 1967; 64: 1125–34.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Calthorpe, C., Watson, P. & McCartney, A. Posterior scleritis: A clinical and histological survey. Eye 2, 267–277 (1988). https://doi.org/10.1038/eye.1988.52
Issue Date:
DOI: https://doi.org/10.1038/eye.1988.52
This article is cited by
-
Alterations in choroidal circulatory dynamics and choroidal thickness before and after treatment in posterior scleritis
BMC Ophthalmology (2023)
-
Comparison of the clinical features between posterior scleritis with exudative retinal detachment and Vogt–Koyanagi–Harada disease
International Ophthalmology (2022)
-
Outcomes of Escalating Immunosuppressive Treatments for Recalcitrant Noninfectious Posterior Scleritis
Ophthalmology and Therapy (2022)
-
Choroidal involvement in non-infectious posterior scleritis
Journal of Ophthalmic Inflammation and Infection (2021)
-
Effectiveness of pharmacological agents for the treatment of non-infectious scleritis: a systematic review protocol
Systematic Reviews (2020)