Abstract
Although radiation therapy is a cornerstone of modern management of malignancies, various side effects are inevitably linked to abdominal and pelvic cancer after radiotherapy. Radiation-mediated gastrointestinal (GI) toxicity impairs the life quality of cancer survivors and even shortens their lifespan. Hydrogen has been shown to protect against tissue injuries caused by oxidative stress and excessive inflammation, but its effect on radiation-induced intestinal injury was previously unknown. In the present study, we found that oral gavage with hydrogen-water increased the survival rate and body weight of mice exposed to total abdominal irradiation (TAI); oral gavage with hydrogen-water was also associated with an improvement in GI tract function and the epithelial integrity of the small intestine. Mechanistically, microarray analysis revealed that hydrogen-water administration upregulated miR-1968-5p levels, thus resulting in parallel downregulation of MyD88 expression in the small intestine after TAI exposure. Additionally, high-throughput sequencing showed that hydrogen-water oral gavage resulted in retention of the TAI-shifted intestinal bacterial composition in mice. Collectively, our findings suggested that hydrogen-water might be used as a potential therapeutic to alleviate intestinal injury induced by radiotherapy for abdominal and pelvic cancer in preclinical settings.
Similar content being viewed by others
Introduction
After the bone marrow, the gastrointestinal (GI) tract ranks as the second-most sensitive organ to irradiation injury during cancer therapy.1 During radiotherapy of abdominal and pelvic malignancies, ionizing radiation destroys the mucosal surface of the GI tract, thus leading to symptoms that may impair the course of treatment and even cause death.2 Even for healthy populations, unexpected irradiation exposure also leads to severe life-threatening intestinal injury.3 Therefore, irradiation-induced GI tract toxicity remains a conundrum that urgently requires effective therapy.
A growing body of evidence indicates that hydrogen (H2), as a novel antioxidant, scavenges hydroxyl radical and peroxynitrite.4 In contrast to other antioxidants, gaseous molecular hydrogen efficiently penetrates cytoplasmic membranes and targets intracellular organelles, largely owing to its small size and neutral electricity.5 Intracellularly, it selectively neutralizes cytotoxic reactive oxygen species (ROS) such as OH in living cells instead of reacting with other ROS that possess physiological roles. As a result, hydrogen has been considered an ideal therapeutic agent for a wide array of diseases, including cardiovascular, cerebrovascular, metabolic disorders and certain types of cancer.6 Hydrogen can be administered in many different ways, among which hydrogen-water is a promising hydrogen usage, owing to its convenience and safety. Moreover, hydrogen-water has been reported to mitigate the hematological injury induced by irradiation through the suppression of radiation-induced caspase 3 activation beyond rescuing the radiation-induced depletion of platelets.7 To date, it has been unknown whether hydrogen-water might confer protection against radiation-mediated intestinal toxicity in preclinical experimental settings.
Toll-like receptors (TLRs), one of the most well-characterized pattern recognition receptors, recognize microbial pathogens for the innate immune system through recognizing pathogen-associated molecular patterns.8, 9 MyD88 (myeloid differentiation primary response gene 88) is a central adaptor protein for many TLRs, and it serves as an essential modulator of the innate immune response to microbial pathogens.10, 11 MyD88 has been reported to mediate immunopathology and gut microbiota dynamics in intestinal graft-versus-host disease involving TLR9.12 Animals deficient in MyD88 within the T-cell compartment experience perturbed microbiota (dysbiosis) in the mucosal compartment and develop severe intestinal inflammation,13 thus suggesting an important role of MyD88 in maintaining the mutualism between hosts and microbiota in healthy conditions.14 However, whether hydrogen-water affects the expression of MyD88 in irradiated animals remains enigmatic.
In this study, we sought to investigate whether hydrogen-water might ameliorate radiation-mediated small intestinal toxicity by using mouse models. We found that oral gavage with hydrogen-water improved GI tract function and the epithelial integrity of small intestine tissue, thus resulting in an increase in the survival rate and body weight of mice after TAI. Administration of hydrogen-water increased the level of miR-1968-5p targeting MyD88 in small intestine tissues and preserved the intestinal bacterial composition structure in irradiated mice. Thus our findings provide new insights into the therapeutic potential and protective mechanism of hydrogen-water in ameliorating TAI-induced GI toxicity in preclinical settings.
Materials and methods
Animals
All experiments were carried out in accordance with procedures approved by the Daegu-Gyeongbuk Medical Innovation Foundation Institutional Animal Care and Use Committee. All procedures and animal handling were performed by following the ethical guidelines for animal studies. Male C57BL/6 mice (approximately 20 g) were housed under standard conditions (ambient temperature 22±2 °C, air humidity 40–70% and a 12/12-h light/dark cycle) and were given continuous access to a standard diet and water according to the guidelines established by the National Institutes of Health Guide for the Care and Use of Laboratory Animals. All mice in this study were male and were of a pure C57BL/6 genetic background.
Irradiation study
A Gammacell 40 Exactor (Best Theratronics Ltd., Kanata, ON, Canada) was used for all experiments. In this study, male mice were treated with a single gamma-ray dose of 15 Gy at a rate of 1.0 Gy min−1 total abdominal irradiation (TAI). The weight of the mice treated with TAI or TAI with hydrogen-water was assessed for 5 days.
Experimental protocol
The animals were separated into two groups. (1) TAI group: mice were treated with 15 Gy TAI. Normal water (0.2 ml) was force-fed into each mouse’s stomach using gavage two times per day; and (2) TAI+HW (hydrogen-water) group: mice were treated with 15 Gy TAI. Hydrogen-water (0.2 ml) was force-fed into each mouse’s stomach using gavage two times per day.
Hydrogen-water administration
H2 gas was generated from a hydrogen gas generator (SHC-300, Saikesaisi HW Energy, Shandong, China) and bubbled into 500 ml of sterile water at a rate of 150 ml min−1 for 20 min. The concentration of H2 in the water was detected with a dissolved hydrogen meter (Trustlex ENH-1000, Osaka suita, Japan). Each day, we used a fresh preparation of hydrogen-water, aiming to reach the overall saturation level of 0.8 mM.
Formed fecal collection
For this study, six mice (6–8-week-old male or female C57BL/6J mice) were fed in one cage. They were kept under the same environment as the other experimental mice. Formed feces were collected every 2 days from the first day of irradiation. Then we counted the number of formed stools in every group.
Peripheral blood cell counts
One hundred microliters of peripheral blood was obtained from the orbital sinus by using a micro-pipette coated with the anticoagulant K2EDTA 15 days after 15 Gy TAI. The cell counts included white blood cells and hemoglobin and were counted using a Celltac E hemocytometer (Nihon Kohden, Tokyo, Japan).
Plasmid construction
A ~400 bp fragment of the MyD88 3′-untranslated region (3′UTR) was cloned into pGL3-control vector (Promega, Madison, WI, USA) immediately downstream of the stop codon of the luciferase gene to generate pGL3-MyD88. A mutant construct of the conserved seed region of MyD88 3′UTR (named pGL3-MyD88-mut), carrying a substitution of 8 nucleotides within the core seed sequence of miR-1968-5p, was generated by using overlapping extension PCR. The primers are listed in Supplementary Table S1.
Cell culture
The 3T3 cells were maintained in DMEM (Gibco, Grand Island, NY, USA). The cells were cultured with heat-inactivated 10% fetal bovine serum (Gibco), 100 U ml−1 penicillin and 100 mg ml−1 streptomycin and grown at 5% CO2 and 37 °C.
Cell transfection
The cells were cultured in 6- or 24-well plates for 24 h and then were transfected with microRNA (miRNA) or small interfering RNAs, respectively. All transfections were performed using linear polyethylenimine (Sigma-Aldrich, Saint Quentin-Fallavier, France) according to the manufacturer’s protocol. miR-1968-5p and anti-miR-1968-5p were synthesized by RiboBio (Guangzhou, China).
Luciferase reporter assays
Luciferase reporter assays were performed using the Dual-Luciferase Reporter Assay System (Promega) according to the manufacturer’s instructions. Cells were cultured in 24-well plates at approximately 3 × 104 cells per well. After 24 h, the cells were transiently co-transfected with the pRL-TK plasmid (Promega) containing the Renilla luciferase gene, which was used for internal normalization, and with the construct carrying the seed sequence of MyD88 3′UTR (or pGL3-control). All experiments were performed at least three times.
Quantitative reverse transcriptase-PCR
Total RNA was separated from mouse tissues using Trizol (Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s protocol. For mature miR-1968-5p detection, total RNA was polyadenylated by poly (A) polymerase (Ambion, Austin, TX, USA), as described previously.15 cDNA was produced by using poly(A)-tailed total RNA and reverse transcription primer with ImPro-IIReverse Transcriptase (Promega) according to the manufacturer’s instructions. Quantitative reverse transcriptase-PCR was performed according to the instructions of Fast Start Universal SYBR Green Master Mix (Rox) (Roche Diagnostics GmbH, Mannheim, Germany). The primers are listed in Supplementary Table S1. GAPDH (glyceraldehyde 3-phosphate dehydrogenase) and U6 were used as controls.
Western blotting analysis
The expression of MyD88, MDA and HO-1 was examined using western blotting analysis. Ice-cold radio-immuno-precipitation assay buffer supplemented with phosphatase and protease inhibitors was used for protein extraction. Total protein samples were separated via sodium dodecyl sulfate-polyacrylamide gel electrophoresis (12% acrylamide gel) using a Bio-Rad Trans-Blot system (Hercules, CA, USA) and were transferred to membranes. Later, specific antibodies to MyD88 (ab135693), MDA (ab27642) and HO-1 (Proteintech Group, Chicago, IL, USA) were used at a dilution of 1:500. Additionally, membranes were incubated with anti-GAPDH (Proteintech Group), which served as the internal control. The readout was detected by using ChemiDoc XRS+ with the Image Lab Software (Bio-Rad).
Hematoxylin and eosin
The mice in the experiment were dissected; their small intestines were immediately placed in freshly prepared 4% formaldehyde in phosphate-buffered saline and fixed overnight with rocking at 4 °C. The tissues were sectioned into 5-μm sections and stained.
Measurement of malondialdehyde by enzyme-linked immunosorbent assay
The level of malondialdehyde (MDA) in the small intestine was determined using a detection kit from Solarbio (Beijing Solarbio Science & Technology Co., Ltd., Beijing, China) according to the manufacturer’s instructions. Levels of MDA were evaluated and calculated by the following formula, according to the manufacturer’s instructions:

Bacterial diversity analysis
Stool samples were freshly collected and stored at −80 °C before use. DNA was extracted from the stool by using a Power Fecal DNA Isolation Kit (MoBio, Carlsbad, CA, USA). The DNA was recovered with 30 ml of buffer in the kit. The 16S ribosomal RNA (rRNA) gene was analyzed to evaluate the bacterial diversity by using the Illumina Hiseq platform (Novogene Bioinformatics Technology Co., Ltd., Madison, WI, USA).
Microarray analysis
These samples were used to synthesize double-stranded complementary DNA (cDNA) and the cDNA was labeled and hybridized to the Affymetrix Genechip microarray 4.0 (CapitalBio Corp, Beijing, China) according to the manufacturer’s instructions. The data from the microarray were used to analyze data summarization, normalization and quality control by using the Gene Spring software V11.5 (Agilent, Santa Clara, CA, USA). The differentially expressed microRNAs were selected if the change of threshold values were >2.0-fold and if Benjamini–Hochberg corrected P-values were <0.05. The data were normalized and hierarchically clustered with the CLUSTER 3.0 software (Sun Microsystems, Palo Alto, CA, USA). The data visualization was performed with the Java Tree view software (Oracle, Redwood Shores, CA, USA).
Statistical analysis
The data are presented as the mean ±s.e.m. with respect to the number of samples (n) in each group. Statistical significance between multiple treatment groups was determined by analysis of variance and Tukey’s t-test. The survival rates were analyzed using Kaplan–Meier survival test. Results with P<0.05 were considered statistically significant.
Results
Hydrogen-water administration protects mice against radiation-induced GI toxicity
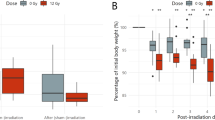
We prepared hydrogen-rich water solution and monitored the hydrogen release kinetics under room temperature. Freshly prepared hydrogen-water showed an initial maximum H2 concentration approximately 0.7 mM, but the H2 concentration progressively decreased to 0.2 mM within 8 h (Figure 1a). Thus we routinely prepared fresh hydrogen-water immediately before each experiment. As shown in Figure 1b, the abdomens of TAI-treated mice exhibited radiation-induced alopecia within 2 months, thus validating the feasibility of the TAI system for inducing gut injury. After exposure to 15 Gy TAI, the animal survival rate was decreased by 50% in the control vehicle group, but it was decreased by only 10% in animals receiving the hydrogen-water (via oral gavage, Figure 1c). Moreover, hydrogen-water administration also significantly increased the body weights of the irradiated mice (Figure 1d), thus indicating that hydrogen-water protects against TAI-induced mortality and weight loss. Then the antioxidant function of hydrogen-water was explored. In irradiated animals, the oxidative stress marker MDA was significantly increased in the small intestine, but it showed a marked decrease in the hydrogen-water group (Figure 1e and Supplementary Figure 1b). Given that nuclear factor erythroid 2 related factor 2 (Nrf2) and heme oxygenase-1(HO-1) have important roles in the antioxidative stress response,16 we further observed that the intestinal levels of Nrf2 and HO-1 increased after TAI exposure, but hydrogen-water administration slightly blunted the changes (Figure 1f and Supplementary Figure 1b).
Oral gavage with hydrogen-water protects mice against radiation-induced toxicity. Mice were treated with hydrogen-water 2 days before and 7 days after receiving 15 Gy TAI. (a) Direct examination of H2 concentrations over an 8-h period. (b) A mouse treated with 15 Gy TAI (left) and its littermate without irradiation (right). Note the change in fur color in the irradiated lower body. (c) Kaplan–Meier analysis of hydrogen-water- and normal water-treated mice after 15 Gy TAI. P<0.05 by log-rank test between TAI-exposed mice with or without hydrogen-water treatment, n=12. (d) Body weight was compared between hydrogen-water- and saline-treated mice after 15 Gy TAI. n=12; **P<0.01; Student’s t-test. (e) The level of MDA in the small intestine was compared among the healthy control, 12 Gy TAI and hydrogen-water groups. n=12; *P<0.05; **P<0.01;***P<0.005; Student’s t-test. (f) The expression levels of Nrf2 were assessed in small intestine tissue from the healthy control, 12 Gy TAI and hydrogen-water groups. n=12; *P<0.05; Student’s t-test.
Exposure to a high dose of irradiation in a short time is associated with acute radiation syndrome, which manifests as severe diarrhea and fluid loss.17 To explore whether hydrogen-water might relieve radiation-induced GI toxicity, we quantified the total amount of stool pellets in the cage bedding. As shown in Figures 2a and b, the TAI-exposed animals had fewer stool pellets than did mice treated with hydrogen-water at day 6 after irradiation. Oral gavage with hydrogen-water mitigated TAI-induced GI injury. As shown in Figure 2c, abdominal irradiation caused the intestinal contents to thin down, and watery diarrhea appeared. However, hydrogen-water treatment mitigated the injury and kept the intestinal contents close to the normal state-containing stool pellets. Hematoylin and eosin staining of small intestine further revealed a dramatic decrease in the number of intact intestinal villi in irradiated animals, and this effect was significantly rescued by oral gavage with hydrogen-water (Figure 2d), thus suggesting that hydrogen-water confers protection against irradiation injury by restoring both GI tract functions and epithelial integrity. In agreement with the essential role of solute carrier family 2 member 1(Glut 1/Slc2a1) phosphoglycerate kinase 1 (Pgk1) and multi-drug resistance protein 1 (MDR1) in maintaining epithelial integrity after toxic stimuli,18, 19 we validated that hydrogen-water treatment dramatically increased the expression levels of Glut1, Pgk1 and MDR1 in the small intestine tissues of TAI-treated mice (Figures 2e–g). In sharp contrast, oral gavage with hydrogen-water did not significantly alter peripheral white blood cell counts after TAI (Supplementary Figure 1a). Together, our observations demonstrated that hydrogen-water improves GI tract functions and epithelial integrity, thus leading to an increase in the survival rate of TAI-treated mice.
Hydrogen-water administration improves GI function and epithelial integrity of irradiated mice. (a and b) Counts of droppings removed from the cage bedding each day from representative cages, n=6 mice per cage. Statistically significant differences are indicated: ***P<0.005; Student’s t-test. (c) Examples of intestinal tract from a total abdominal irradiated mouse and a TAI-exposed mouse with hydrogen-water treatment. (d) The morphology of small intestine in radiation-induced mice treated with normal water or hydrogen-water is shown by H&E staining. (e–g) The expression levels of Glut1, Pgk1 and MDR1 were assessed by qRT-PCR in small intestine tissue from TAI mice without or with hydrogen-water treatment. Statistically significant differences are indicated: ***P<0.005; Student’s t-test.
Hydrogen-water decreases the level of MyD88 in the mouse small intestine
Given the important role of MyD88 in the integrity of small intestine,20 we examined the effect of hydrogen-water administration on the expression of MyD88 in small intestine tissues. Although TAI exposure decreased MyD88 mRNA expression, hydrogen-water administration further decreased the expression level (Figure 3a). Western blotting analysis further validated the results (Figure 3b). To elucidate the underlying molecular mechanism, we assessed the microRNA expression profile in small intestine tissues by using a microarray chip. Microarray and bioinformatics analysis (RNA 22, https://cm.jefferson.edu/rna22/) revealed that the expression of a spectrum of miRNAs had fluctuated, such as the expression of miRNA-1968-5p, which has been predicted to target a number of essential signaling molecules, including MyD88 (Figure 3c and Supplementary Figure 2). Thus the upregulation of miRNA-1968-5p by TAI and further elevation by hydrogen-water was confirmed by quantitative real-time PCR (Figure 3d), thus indicating that miR-1968-5p might be involved in the hydrogen-water-mediated protection against irradiation-induced injury. Correlation analysis between MyD88 mRNA and miR-1968-5p levels exhibited an inverse correlation (Figure 3e), thus supporting the possibility that miR-1968-5p might target MyD88 to inhibit its mRNA stability. Given that TLR4 and TLR5 are expressed in the mouse small intestine dependent on the adaptor MyD88,21, 22 we further evaluated the expression of TLR4 and TLR5 in the small intestine in this system. Our data revealed that total body irradiation decreased the expression of TLR4 and TLR5. Hydrogen-water treatment further decreased their expression to a significantly different level (Figures 3f and g). Together, our data suggested that hydrogen-water ameliorates TAI-induced GI toxicity partly through upregulating miR-1968-5p, which might target MyD88.
Hydrogen-water upregulates the level of MyD88-targeting miR-1968-5p in the mouse small intestines. (a) The expression level of MyD88 was examined in the aforementioned small intestine tissues by qRT-PCR. Statistically significant differences are indicated: **P<0.01; ***P<0.005; Student’s t-test. (b) The expression of MyD88 was examined by western blotting in TAI-exposed mice with or without hydrogen-water treatment. (c) Alterations in miRNA expression in small intestine tissues from mice without or with TAI were assessed using microarray analysis. (d) The expression level of miR-1968-5p was examined by qRT-PCR in small intestine tissues from mice without TAI (Control, n=20), mice with TAI (TAI, n=20) and mice with hydrogen-water treatment after TAI (TAI+HW, n=20) individually. Statistically significant differences are indicated: *P<0.05; **P<0.01; Student’s t-test. (e) The correlation between MyD88 mRNA expression and miR-1968-5p level was examined by qRT-PCR in 20 cases of small intestine tissues from mice with hydrogen-water treatment after TAI. **P<0.01; Pearson correlation coefficient, r=−0.7296. (f) The expression level of TLR4 was examined in the aforementioned small intestine tissues by qRT-PCR. Statistically significant differences are indicated: *P<0.05; ***P<0.005; Student’s t-test. (g) The expression level of TLR5 was examined in the aforementioned small intestine tissues by qRT-PCR. Statistically significant differences are indicated: *P<0.05; Student’s t-test.
MiR-1968-5p inhibits the expression of MyD88 by targeting its 3′UTR
To test this hypothesis, we analyzed the effect of miR-1968-5p supplementation on MyD88 expression through luciferase reporter assays. On the basis of bioinformatics analysis (https://cm.jefferson.edu/rna22/), we predicted position 1595–1602 as one of the three possible binding sites for miR-1968-5p in the 3′UTR of MyD88 (Figures 4a and b). Indeed, luciferase reporter assays revealed that miR-1968-5p downregulated the luciferase activity of a construct carrying the seed region of the MyD88 3′UTR in a dose-dependent manner (position 1595–1602, pGL3-MyD88) (Figure 4c). In contrast, miR-1968-5p did not decrease the luciferase activity of a construct containing the MyD88 3′UTR seed region with complementary sequence (mutant in same position 1595–1602, pGL3-MyD88-mut) (Figure 4c). Reciprocally, anti-miR-1968-5p increased the luciferase activity of pGL3-MyD88 but not that of the pGL3-MyD88 mutant (Figure 4d), thus suggesting that miR-1968-5p directly binds to the 3′UTR of MyD88 mRNAs. Similarly, supplementation with miR-1968-5p led to dose-dependent suppression of MyD88 expression in 3T3 cells (Figure 4e), whereas supplementation with anti-miR-1968-5p resulted in elevation of MyD88 expression in these cells (Figure 4f). Together, these data confirmed that miR-1968-5p indeed suppresses the expression of MyD88 by targeting the 3′UTR of its mRNA.
MiR-1968-5p inhibits the expression of MyD88 by targeting its 3′UTR. (a and b) MiR-1968-5p inhibits the expression of MyD88 by targeting the predicted conserved miR-1968-5p-binding site at nucleotides 1595–1602 of the MyD88 3′UTR. The generated mutation sites at the MyD88 3′UTR seed region are indicated. The wild-type MyD88 3′UTR (or mutant) was inserted into the downstream of luciferase reporter gene in the pGL3-control vector. (c and d) The effect of miR-1968-5p (or anti-miR-1968-5p) on pGL3-MyD88 and pGL3- MyD88-mut reporters in 3T3 cells was measured by luciferase reporter assays. Statistically significant differences are indicated: *P<0.05; **P<0.01; Student’s t-test. (e and f) The effect of miR-1968-5p (or anti-miR-1968-5p) on the expression of MyD88 in 3T3 cells was measured by western blotting. Each experiment was repeated at least three times. NS, not significant.
Hydrogen-water treatment has no effect on the abundance of enteric bacteria
MyD88 ‘tunes’ the symbiotic enteric microbes, and our previous studies have reported that gut microbiota affect the radioresistance of hosts.23, 24 Thus we performed 16S rRNA sequencing to analyze the gut bacterial community in mice after TAI exposure with or without hydrogen-water oral gavage. As shown in Figure 5a, 15 Gy gamma-ray TAI exposure significantly increased the observed species number in irradiated mice with or without hydrogen-water treatment. However, Shannon and Simpson index analysis did not indicate significant differences among controls, TAI-exposed mice and TAI-exposed mice with hydrogen-water administration (Figures 5b and c). In detail, TAI treatment caused a lower relative abundance of Bacteroidetes and higher relative abundance of Proteobacteria at the phylum level; however; oral gavage with hydrogen-water restored the abundance to a level close to that of the control group (Figure 5d). Together, our observations demonstrated that hydrogen-water has no effect on the abundance of enteric bacteria in TAI-exposed mice.
Hydrogen-water treatment has no effect on the abundance of enteric bacteria. (a) The observed species number of intestinal bacteria in con and TAI-treated mice (with or without hydrogen-water oral gavage) was examined by 16S rRNA high-throughput sequencing after 5 days of TAI exposure. (b and c) The Shannon (b) and Simpson (c) diversity indices of intestinal bacteria in con and TAI-treated mice (with or without hydrogen-water oral gavage) were assessed by 16S rRNA high-throughput sequencing after 5 days of TAI exposure. For panels (a–c), the top and bottom boundaries of each box indicate the 75th and 25th quartile values, respectively, and lines within each box represent the 50th quartile (median) value. Ends of whiskers mark the lowest and highest diversity values in each instance. (d) The relative abundance of enteric bacteria at the phylum level in con and TAI-treated mice (with or without oral gavage of hydrogen-water) was assessed using 16S high-throughput sequencing after irradiation at day 5. Statistically significant differences are indicated: Student’s t-test, n=4 per group.
Oral gavage with hydrogen-water results in retention of the intestinal bacterial composition pattern impaired by TAI
Next, Principal Coordinate Analysis was used to further determine the role of hydrogen-water in shaping the intestinal bacterial flora profile. As shown in Figure 6a, the intestinal bacterial composition profile substantially changed after TAI treatment as well as hydrogen-water treatment. Statistically, unweighted unifrac analysis revealed that TAI drove a marked difference in gut microbiota composition, whereas hydrogen-water treatment eliminated the difference (Figures 6b and c), thus suggesting that hydrogen-water might preserve the TAI-shifted bacterial composition to perform radioprotection. Specifically, TAI treatment caused a lower abundance of Bacteroidia, Betaproteobacteria and Coriobacteria and a higher relative abundance of Phycisphaerae, Planctomycetia and Sphingobacteria at the genus level, whereas hydrogen-water treatment reversed these changes (Figures 6d and e). Comparing the gut bacteria at the genus level by using linear discriminant analysis effect size calculation, we found many taxa to be different in abundance between the TAI group and hydrogen-water treatment cohorts. For instance, the S24_7 was most abundant after TAI treatment compared with the hydrogen-water treatment group, which had a greater abundance of Bacteroides (Figure 6f). Together, our data indicated that hydrogen-water treatment preserves the intestinal bacterial composition shaping from TAI exposure.
Oral gavage with hydrogen-water retains the intestinal bacterial composition pattern impaired by TAI. (a–c) Principal component and β diversity analyses were used to measure the shift in the intestinal bacterial composition profile in con and TAI-treated mice (with or without hydrogen-water oral gavage) after irradiation at day 5. Statistically significant differences are indicated: *P<0.05, ***P<0.001; Student’s t-test, n=4. For panel (b), the top and bottom boundaries of each box indicate the 75th and 25th quartile values, respectively, and lines within each box represent the 50th quartile (median) value. Ends of whiskers mark the lowest and highest diversity values in each instance. (d) Alterations in intestinal bacterial patterns at the genus level in con and TAI-treated mice (with or without hydrogen-water oral gavage) were assessed using 16S high-throughput sequencing after irradiation at day 5, n=4. The heatmap is color coded on the basis of row Z-scores. The mice with the highest and lowest bacterial levels are in red and blue, respectively. (e) The relative abundance of the top 10 bacteria at the genus level in con and TAI-treated mice (with or without hydrogen-water oral gavage) was assessed using 16S high-throughput sequencing after irradiation at day 5, n=4. (f) Linear discriminant analysis (LDA) effect size (LEfSe) results showed that the bacteria were significantly different in abundance between the TAI and hydrogen-water groups and indicated the effect size of each differentially abundant bacterial taxon in the small intestine (n=4). Statistically significant differences are indicated: Student’s t-test.
Discussion
Hydrogen-water has been reported to be administered as an antioxidant in biological systems.25 Research on the health benefits of hydrogen-water has demonstrated that hydrogen-water has long-term effects; clinical studies on humans indicate that hydrogen-water may be used to treat metabolic syndrome and diabetes and to enhance the therapeutic effect of anticancer drugs.26, 27, 28 Radiotherapy for malignant pelvic and abdominal tumors may cause acute and late complications due to the side effects of irradiation, which are the main challenge for radiation oncologists, medical physicists and radiobiologists. On the basis of previous studies, we speculated that hydrogen-water might be a curative scheme to treat GI toxicity induced by radiotherapy for abdominal and pelvic malignancies. To test our hypothesis, we performed several experiments using mouse models. Notably, our observations revealed that oral gavage with hydrogen-water significantly increased the survival rate and body weight of TAI-exposed mice. Moreover, hydrogen-water treatment improved GI tract functions and epithelial integrity after TAI exposure. The mechanism of radiation-induced GI toxicity partly results from damage due to oxidative stress and the production of ROS.29 Membrane lipids are the major targets of ROS and the free radical chain reaction.30 Increases in lipid peroxidation products such as MDA are indices of lipid damage.31 In the present study, intestinal MDA increased after TAI exposure; however, hydrogen-water administration reverted the changes, thus suggesting that hydrogen-water performed its radioprotective role partly by decreasing the production of ROS and effectively inhibiting oxidative reactions. Nrf2 is a redox-sensitive transcription factor that has an important role in cellular antioxidant defense.32 After stimulation, Nrf2 translocates to the nucleus and initiates transcription of cytoprotective genes, such as HO-1. Hydrogen-water was protective against ROS and oxidative reactions, thereby removing stress. Thus the TAI-upregulated Nrf2 and HO-1 expression was downregulated after hydrogen-water consumption. Together, our data provided novel insights into the function of hydrogen-water in clinical application, demonstrating that hydrogen-water can be used as a therapeutic strategy during radiotherapy for abdominal and pelvic carcinoma.
The TLR family, one of the characterized families of innate immune receptors, induces innate immune responses that resist pathogens and recognize microbial components. Previous studies have identified a protective function of TLRs against irradiation injuries to the GI tract.20 MyD88 is a key signaling adaptor for almost all TLRs and manipulates diverse physiological and pathological states, such as the development of liver and pancreatic cancer and colon carcinogenesis, as well as sarcomagenesis.33 Conditional deletion of MyD88 from intestinal epithelial cell renders mice more tolerant to local ischemic/reperfusion insult than wild-type controls,34 thus suggesting an important role of MyD88 in the regulation of gut injury. Moreover, deletion of MyD88 enhances the radioresistance in a mouse model, as compared with wild type.35 Therefore, we focused on MyD88 to determine the molecular mechanism by which hydrogen-water mitigated TAI-induced GI toxicity. Intriguingly, our observations revealed that oral gavage with hydrogen-water predominantly downregulated the expression of MyD88 in small intestine tissues from irradiated mice by upregulating the level of miRNA-1968-5p, thus suggesting that this radioprotection effect might depend on miRNA-1968-5p/MyD88 signaling. Interestingly, MyD88 deletion in intestinal epithelial cells protects mice against high-fat-diet-promoted obesity, diabetes and low-grade inflammation.36 Thus hydrogen-water might be used to treat MyD88-mediated obesity, diabetes and low-grade inflammation in clinical settings, although further study is required.
The GI tract is inhabited by a dense population of organized and highly specialized microbial flora that collectively modulate host immunity and metabolism.37 Disturbances in host–microbe interaction are associated with many diseases, including obesity, malnutrition, inflammatory bowel disease, liver disease and cancers.38 Given that MyD88 affects the composition of intestinal microbiota through sophisticated mechanisms,39 and differences in initial microbial colonization are linked to the susceptibility or protection against radiotherapy,40 we speculated that hydrogen-water might shape the intestinal bacterial community and alleviate TAI-induced GI toxicity. As expected, interrogation of microbiota composition by 16S RNA sequencing showed that oral gavage with hydrogen-water resulted in retention of the intestinal bacterial composition in irradiated mice. Manipulation of the gut microbiota has been shown to be an effective therapeutic approach to prevent radiotherapy-mediated GI toxicity.23, 41 On the basis of our findings, hydrogen-water might be a novel agent for patients after radiotherapy. Recent mounting evidence indicates that the composition of gut microbiota is associated with the gene expression profile of hosts.42 Thus hydrogen-water-educated gut microbiota might elicit upregulation of miR-1968-5p after TAI, a possibility that requires further study. Together, our observations provide potential mechanisms by which hydrogen-water ameliorates TAI-induced GI tract toxicity and suggest that hydrogen-water might serve as a therapy for dysbacteriosis-mediated diseases.
In aggregation, hydrogen-water alleviates and protects against TAI-induced small intestinal toxicity in a mouse model. Oral gavage with hydrogen-water markedly improved the GI tract functions and epithelial integrity after TAI exposure. Mechanistically, hydrogen-water increases the level of miR-1968-5p in the mouse small intestine, thereby downregulating the expression of MyD88 through directly targeting its 3′UTR. Moreover, hydrogen-water treatment results in retention of the intestinal bacterial composition structure after irradiation. Thus our findings provide novel insights into the function and mechanism of hydrogen-water mitigating TAI-induced GI injury and pave the way for use of hydrogen-water in clinical practice to improve the prognosis after abdominal and pelvic cancer radiotherapy.
References
Ciorba MA, Riehl TE, Rao MS, Moon C, Ee X, Nava GM et al. Lactobacillus probiotic protects intestinal epithelium from radiation injury in a TLR-2/cyclo-oxygenase-2-dependent manner. Gut 2012; 61: 829–838.
Taniguchi CM, Miao YR, Diep AN, Wu C, Rankin EB, Atwood TF et al. PHD inhibition mitigates and protects against radiation-induced gastrointestinal toxicity via HIF2. Sci Transl Med 2014; 6: 236ra64.
Burdelya LG, Krivokrysenko VI, Tallant TC, Strom E, Gliberman AS, Gupta D et al. An agonist of toll-like receptor 5 has radioprotective activity in mouse and primate models. Science 2008; 320: 226–230.
Runtuwene J, Amitani H, Amitani M, Asakawa A, Cheng KC, Inui A . Hydrogen-water enhances 5-fluorouracil-induced inhibition of colon cancer. PeerJ 2015; 3: e859.
Ohsawa I, Ishikawa M, Takahashi K, Watanabe M, Nishimaki K, Yamagata K et al. Hydrogen acts as a therapeutic antioxidant by selectively reducing cytotoxic oxygen radicals. Nat Med 2007; 13: 688–694.
Zhang Y, Su WJ, Chen Y, Wu TY, Gong H, Shen XL et al. Effects of hydrogen-rich water on depressive-like behavior in mice. Sci Rep 2016; 6: 23742.
Yang Y, Li B, Liu C, Chuai Y, Lei J, Gao F et al. Hydrogen-rich saline protects immunocytes from radiation-induced apoptosis. Med Sci Monit 2012; 18: Br144–Br148.
Wang JQ, Jeelall YS, Ferguson LL, Horikawa K . Toll-Like receptors and cancer: MYD88 mutation and inflammation. Front Immunol 2014; 5: 367.
Fitzgerald KA, Palsson-McDermott EM, Bowie AG, Jefferies CA, Mansell AS, Brady G et al. Mal (MyD88-adapter-like) is required for Toll-like receptor-4 signal transduction. Nature 2001; 413: 78–83.
Zhang LM, Liu JH, Xue CB, Jefferies CA, Mansell AS, Brady G et al. Pharmacological inhibition of MyD88 homodimerization counteracts renal ischemia reperfusion-induced progressive renal injury in vivo and in vitro. Sci Rep 2016; 6: 26954.
O'Reilly S . Innate immunity in systemic sclerosis pathogenesis. Clin Sci (Lond) 2014; 126: 329–337.
Heimesaat MM, Nogai A, Bereswill S, Plickert R, Fischer A, Loddenkemper C et al. MyD88/TLR9 mediated immunopathology and gut microbiota dynamics in a novel murine model of intestinal graft-versus-host disease. Gut 2010; 59: 1079–1087.
Araki A, Kanai T, Ishikura T, Makita S, Uraushihara K, Iiyama R et al. MyD88-deficient mice develop severe intestinal inflammation in dextran sodium sulfate colitis. J Gastroenterol 2005; 40: 16–23.
Kubinak JL, Petersen C, Stephens WZ, Soto R, Bake E, O'Connell RM et al. MyD88 signaling in T cells directs IgA-mediated control of the microbiota to promote health. Cell Host Microbe 2015; 17: 153–163.
Cui M, Xiao Z, Wang Y, Zheng M, Song T, Cai X et al. Long noncoding RNA HULC modulates abnormal lipid metabolism in hepatoma cells through an miR-9-mediated RXRA signaling pathway. Cancer Res 2015; 75: 846–857.
Li Y, Li Q, Chen H, Wang T, Liu L, Wang G et al. Hydrogen gas alleviates the intestinal injury caused by severe sepsis in mice by increasing the expression of heme oxygenase-1. Shock 2015; 44: 90–98.
Kirsch DG, Santiago PM, di Tomaso E, Sullivan JM, Hou WS, Dayton T et al. p53 controls radiation-induced gastrointestinal syndrome in mice independent of apoptosis. Science 2010; 327: 593–596.
Winkler EA, Nishida Y, Sagare AP, Rege SV, Bell RD, Perlmutter D et al. GLUT1 reductions exacerbate Alzheimer's disease vasculo-neuronal dysfunction and degeneration. Nat Neurosci 2015; 18: 521–530.
Kelly CJ, Glover LE, Campbell EL, Kominsky DJ, Ehrentraut SF, Bowers BE et al. Fundamental role for HIF-1alpha in constitutive expression of human beta defensin-1. Mucosal Immunol 2013; 6: 1110–1118.
Takemura N, Kawasaki T, Kunisawa J, Sato S, Lamichhane A, Kobiyama K et al. Blockade of TLR3 protects mice from lethal radiation-induced gastrointestinal syndrome. Nat Commun 2014; 5: 3492.
Abreu MT . Toll-like receptor signalling in the intestinal epithelium: how bacterial recognition shapes intestinal function. Nat Rev Immunol 2010; 10: 131–144.
Brandao I, Hormann N, Jackel S, Reinhardt C . TLR5 expression in the small intestine depends on the adaptors MyD88 and TRIF, but is independent of the enteric microbiota. Gut Microbes 2015; 6: 202–206.
Cui M, Xiao H, Li Y, Zhou L, Zhao S, Luo D et al. Faecal microbiota transplantation protects against radiation-induced toxicity. EMBO Mol Med 2017; 9: 448–461.
Cui M, Xiao H, Luo D, Zhang X, Zhao S, Zheng Q et al. Circadian rhythm shapes the gut microbiota affecting host radiosensitivity. Int J Mol Sci 2016; 17: E1786.
Iuchi K, Imoto A, Kamimura N, Nishimaki K, Ichimiya H, Yokota T et al. Molecular hydrogen regulates gene expression by modifying the free radical chain reaction-dependent generation of oxidized phospholipid mediators. Sci Rep 2016; 6: 18971.
Wang C, Li J, Liu Q, Yang R, Zhang JH, Cao YP et al. Hydrogen-rich saline reduces oxidative stress and inflammation by inhibit of JNK and NF-kappaB activation in a rat model of amyloid-beta-induced Alzheimer's disease. Neurosci Lett 2011; 491: 127–132.
Kajiyama S, Hasegawa G, Asano M, Hosoda H, Fukui M, Nakamura N et al. Supplementation of hydrogen-rich water improves lipid and glucose metabolism in patients with type 2 diabetes or impaired glucose tolerance. Nutr Res 2008; 28: 137–143.
Song G, Li M, Sang H, Zhang L, Li X, Yao S et al. Hydrogen-rich water decreases serum LDL-cholesterol levels and improves HDL function in patients with potential metabolic syndrome. J Lipid Res 2013; 54: 1884–1893.
Gambhir L . 1,4-Naphthoquinone, a pro-oxidant, ameliorated radiation induced gastro-intestinal injury through perturbation of cellular redox and activation of Nrf2 pathway. Drug Discov Ther 2016; 10: 93–102.
Mishra KP . Cell membrane oxidative damage induced by gamma-radiation and apoptotic sensitivity. J Environ Pathol Toxicol Oncol 2004; 23: 61–66.
El-Missiry MA, Fayed TA, El-Sawy MR, El-Sayed AA . Ameliorative effect of melatonin against gamma-irradiation-induced oxidative stress and tissue injury. Ecotoxicol Environ Saf 2007; 66: 278–286.
Wang-Sheng C, Jie A, Jian-Jun L, Lan H, Zeng-Bao X, Chang-Qing L . Piperine attenuates lipopolysaccharide (LPS)-induced inflammatory responses in BV2 microglia. Int Immunopharmacol 2017; 42: 44–48.
Salcedo R, Cataisson C, Hasan U, Yuspa SH, Trinchieri G . MyD88 and its divergent toll in carcinogenesis. Trends Immunol 2013; 34: 379–389.
Muhlbauer M, Perez-Chanona E, Jobin C . Epithelial cell-specific MyD88 signaling mediates ischemia/reperfusion-induced intestinal injury independent of microbial status. Inflamm Bowel Dis 2013; 19: 2857–2866.
Lai XY, Egan LJ . Suppression of radiation-induced DNA double-strand break repair by MyD88 is accompanied by apoptosis and crypt loss in mouse colon. Oncogenesis 2013; 2: e62.
Everard A, Geurts L, Caesar R, Van Hul M, Matamoros S, Duparc T et al. Intestinal epithelial MyD88 is a sensor switching host metabolism towards obesity according to nutritional status. Nat Commun 2014; 5: 5648.
Schneeberger M, Everard A, Gomez-Valades AG, Matamoros S, Ramírez S, Delzenne NM et al. Akkermansia muciniphila inversely correlates with the onset of inflammation, altered adipose tissue metabolism and metabolic disorders during obesity in mice. Sci Rep 2015; 5: 16643.
Joice R, Yasuda K, Shafquat A, Morgan XC, Huttenhower C . Determining microbial products and identifying molecular targets in the human microbiome. Cell Metab 2014; 20: 731–741.
Wen L, Ley RE, Volchkov PY, Stranges PB, Avanesyan L, Stonebraker AC et al. Innate immunity and intestinal microbiota in the development of Type 1 diabetes. Nature 2008; 455: 1109–1113.
Manichanh C, Varela E, Martinez C, Antolin M, Llopis M, Doré J et al. The gut microbiota predispose to the pathophysiology of acute postradiotherapy diarrhea. Am J Gastroenterol 2008; 103: 1754–1761.
Ciorba MA, Hallemeier CL, Stenson WF, Parikh PJ . Probiotics to prevent gastrointestinal toxicity from cancer therapy: an interpretive review and call to action. Curr Opin Support Palliat Care 2015; 9: 157–162.
Patrignani P, Tacconelli S, Bruno A . Gut microbiota, host gene expression, and aging. J Clin Gastroenterol 2014; 48 (Suppl 1): S28–S31.
Acknowledgements
This work was supported by grants from the National Natural Science Foundation of China (Nos. 81502664, 81572969 and 81402541), CAMS Innovation Fund for Medical Sciences (CIFMS, 2016-I2M-1-017), Fundamental Research Funds for CAMS/PUMC (2016ZX310200 and 2016ZX310073), the PUMC Youth Fund and the Fundamental Research Funds for the Central Universities (Nos. 33320140187, 3332016099 and 3332016143), the IRM-CAMS Research Fund (Nos. 1547 and 1522), the Technology and Development and Research Projects for Research Institutes, Ministry of Science and Technology (2014EG150134) and the Tianjin Science and Technology Support Plan Project (TJKJZC, 14ZCZDSY00001). H-cW was supported by the U.S. National Center of Complementary and Alternative Medicine (NCCAM, R01AT005076) and the National Institute of General Medical Sciences (NIGMS, R01GM063075). We are grateful to Professor Li-xin Zhou from the Department of Pathology, Peking University Cancer Hospital & Institute and Professor Hai-chao Wang from the Laboratory of Emergency Medicine, Feinstein Institute for Medical Research for their kind support and advice.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information accompanies the paper on Experimental & Molecular Medicine website
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Xiao, Hw., Li, Y., Luo, D. et al. Hydrogen-water ameliorates radiation-induced gastrointestinal toxicity via MyD88’s effects on the gut microbiota. Exp Mol Med 50, e433 (2018). https://doi.org/10.1038/emm.2017.246
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/emm.2017.246
This article is cited by
-
Furfural tolerance of mutant Saccharomyces cerevisiae selected via ionizing radiation combined with adaptive laboratory evolution
Biotechnology for Biofuels and Bioproducts (2024)
-
The gut microbiota as a booster for radiotherapy: novel insights into radio-protection and radiation injury
Experimental Hematology & Oncology (2023)
-
Ameliorating Role of Hydrogen-Rich Water Against NSAID-Induced Enteropathy via Reduction of ROS and Production of Short-Chain Fatty Acids
Digestive Diseases and Sciences (2023)
-
Intestinal mucositis precedes dysbiosis in a mouse model for pelvic irradiation
ISME Communications (2021)
-
Gut microbiota-derived indole 3-propionic acid protects against radiation toxicity via retaining acyl-CoA-binding protein
Microbiome (2020)