Abstract
Increasing importance is being given to the stimulation of Th1 response in cancer immunotherapy because its presence can shift the direction of adaptive immune responses toward protective immunity. Based on chemokine receptor expression, CXCR3+CCR4-CD4+ T cells as Th1-type cells were investigated its capacity in monocyte-derived dendritic cell (DC) maturation and polarization, and induction of antigen specific cytotoxic T lymphocytes (CTL) in vitro. The levels of IL-4, IL-5 and IL-10 were decreased to the basal level compared with high production of IFN-γ, TNF-α, and IL-2 in CXCR3+CCR4-CD4+ T cells stimulated with anti-CD3 and anti-CD28 antibodies. Co-incubation of activated CD4+ or CXCR3+CCR4-CD4+ T cells with DC (CD4+/DC or CXCR3+CD4+/DC, respectively) particularly up-regulated IL-12 and CD80 expression compared with DC matured with TNF-α and LPS (mDC). Although there was no significant difference between the effects of the CXCR3+CCR4-CD4+ and CD4+ T cells on DC phenotype expression, CXCR3+CD4+/DC in CTL culture were able to expand number of CD8+ T cells and increased frequencies of IFN-γ secreting cells and overall cytolytic activity against tumor antigen WT-1. These results demonstrated that the selective addition of CXCR3+CCR4-CD4+ T cells to CTL cultures could enhance the induction of CTLs by DC in vitro, and implicated on a novel strategy for adoptive T cell therapy.
Similar content being viewed by others
Introduction
Adoptive transfer of ex vivo generated cytotoxic T cell lines (CTLs) against tumor associated antigen (TAA) or viral antigen can reconstitute immune system and has shown great promise for eradication of malignancy and control of virus infection (Knutson et al., 2005; Mocellin et al., 2005; Palucka et al., 2005). In contrast to previous studies focused on antitumor responses by CD8+ T cells, recent reports have demonstrated the essential role of CD4+ T cells both in the aspects of APC activation and controlling CD8+ T mediated tumor eradication (Nishimura et al., 1999; Surman et al., 2000; Janssen et al., 2005). In physiology, APCs delivers costimulatory signals to CD4+ T cells for activation, which reciprocally activates APCs via costimulatory molecules, especially CD40-CD40L interaction (Prilliman et al., 2002). This interaction eventually primes naïve CD8+ T cells. Mice deficient of functional CD4+ T cells generated lower frequency of antigen specific CTLs and deteriorate antitumor responses (Gao et al., 2002). Moreover, it has been reported that activated CD4+ T cells express costimulatory molecules on the surface including CD27, 4-1BB and MHC II which sustains activity of CTLs and long-term survival (Giuntoli et al., 2002).
DC has been a choice of APC for its potency in antigen uptake, presentation and delivering costimulatory signals. However, without signals to activate and differentiate to matured form, DCs are more likely to generate tolerance (Lutz et al., 2002). Despite the widespread use of maturation cocktail providing danger signals, the limited clinical success of DC vaccines requires improved methodology for sustained production of IL-12 to mediate Th1 polarization. CD40-CD40L interaction has been mainly responsible for IL-12 synthesis and factors including TGF-β and IL-10 inhibit the production (Lyakh et al., 2005; Larmonier et al., 2007). Resembling the in vivo environments, activated CD4+ T cells expressing CD40L used to mature DC in replacement of maturation reagents and demonstrated augmented secretion of IL-12 indicating type I helper T cells (Th1) polarization capacity of DCs (Sato et al., 2004).
Among the subsets of CD4+ T cells, the introduction of Th1 cells enhances interaction between APC and T cells and triggers naïve CD8+ T cells into tumor specific CTLs in the tumor draining lymph nodes. Moreover it has been reported that the preconditioning of PBL towards Th1 significantly augmented vitality and cytotoxic activity by antigen specific CD8+ T cells in cultures (Chattopadhyay et al., 2005) and the injection of Th1 cells as adjuvant inhibited accumulation of regulatory T (Tr) cells in tumor draining lymph nodes (Zhang et al., 2007), respectively. Th1 and Th2 cells has been distinctively defined based on chemokine receptor expression on the surface, CCR5, CXCR3 and CXCR6, and CCR3, CCR4, CCR7, CCR8, CRTh2 and CXCR5, respectively (Mosmann et al., 1989; Mackay et al., 1996; Ward et al., 1998; Lukacs et al., 2001). Despite overlapping expression of chemokine receptors, the classification of Th1/Th2 cells can be based on the representative marker expression of CXCR3+ and CCR4- and the validity was confirmed with cytokine profile of each subset (Kim et al., 2003).
Considering the known capacity of CXCR3+CCR4-CD4+ T cells, this study demonstrates that the selective addition of Th1 cells in CTL cultures provides potent maturation signals to DCs and enhances efficiency in generation of CTLs specific for tumor-associated antigen in vitro.
Results
Chemokine receptor characterizes CXCR3+CD4+ T cells as Th1-type cells
To evaluate whether chemokine receptors can be a critical factor defining different helper T cell subsets, CD4+ T cells were isolated from three different healthy individuals for analysis of chemokine receptor expression on the surface and type of cytokine secretion upon stimulation. There were notable differences in frequencies of helper T cells expressing each chemokine receptors. As shown in Figure 1A, a range of 18 to 21% of CD4+ T cells from three individuals expressed CXCR3, a representative molecule of Th1-type subsets, whereas CCR4 positive subpopulations, known to be expressed by Th2-type subsets, ranged from 21 to 33% (Kim et al., 2003). A large population within helper T cells still remained undifferentiated without any expression of CXCR3 or CCR4 and a few expressed both (data not shown).
Analysis of chemokine receptor expression of CD4+ T cells. (A) Peripheral CD4+ T cells isolated from three different donors were assessed for surface expression of different chemokine receptors, CXCR3 and CCR4 by flow cytometry. (B) CXCR3+CCR4-CD4+ T cells were sorted by FACs VANTAGE and the sorted populations were reexamined for purity (> 95%).
Since there is overlapping of CCR4 expression for both Th1- and Th2-type cells, we preferred CRTH2 as a Th2 marker to measure the expression pattern of cytokines upon activation in subpopulations of CD4+ T cells (Cosmi et al., 2000; Kim et al., 2001). We isolated subpopulations of CD4+ T cells using CXCR3 and CCR4 for Th1-type cells and CRTH2 for Th2-type cells by VANTAGE sorting (Figure 1B) and tracked comparative cytokine expression after stimulation for 48 h. Although the production of IFN-γ, TNF-α, and IL-2 were not significantly altered between the CD4+ and isolated CXCR3+CCR4-CD4+ T subpopulations, the level of type II cytokines secreted by CXCR3+ CCR4-CD4+ T cells including IL-4, IL-5 and IL-10 was significantly decreased down to the basal level (Figure 2). The type of cytokines secreted by CRTH2+CD4+ T cells was mainly IL-4 and IL-5 and IL-10, but IFN-γ and TNF-α were rarely detected after stimulation. Even after Vantage sorting, a small percentage of populations, CXCR3-CCR4-CD4+ T cells, were still present, however the populations were confirmed not to influence the results because of no cytokine expression after activation (data not shown).
Cytokine profile of CXCR3+CCR4-CD4+ T cells compared to total CD4+ T cells. After VANTAGE sorting based on CXCR3+ expression, cells (5 × 103/well) were stimulated with anti-CD3/CD28 beads (1 bead/1 cell) for 48 h. Comparative cytokine analysis between CD4+ T cells and isolated CXCR3+CCR4-CD4+ T cells was examined by Th1/Th2 CBA. The graphs show the mean of triplicate values ± SD of one representing experiment of three performed from three different donors.
DC activated with CXCR3+CCR4-CD4+ T cells potently induces proliferation of IFN-γ producing and cytolytic CD8+ T cells
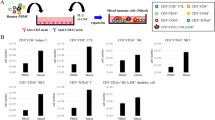
To speculate the effect of CXCR3+CCR4-CD4+ T cells, immature DCs were activated with CXCR3+CCR4-CD4+ T cells (CXCR3+CD4+/DC) and used to induce proliferation and cytotoxicity of CD8+ T cells against the tumor antigen, WT-1. Figure 3A shows naive CD8+ T lymphocytes stimulated with CXCR3+CD4+/DC expanded about 2.5 folds against WT-1 antigen compared to DCs treated with either total CD4+ T cells (CD4+/DC) or maturation cocktail (MC) incuding LPS and TNF-alpha (mDC) (P = 0.031), indicating superior capacity of CXCR3+CD4+/DC for priming naïve T cells. The expanded populations did not contain non-specific CD8+CD56+ T cells as analyzed by flow cytometry (data not shown).
Stimulation of antigen-specific CTLs by CXCR3+CD4+/DCs. Freshly isolated CD8+ T cells were weekly stimulated with autologous DCs pulsed with WT-1 peptide, as described in Methods. (A) The total viable cell count for thrice (21 days for WT-1) stimulation culture was determined by trypan blue dye exclusion. The data is a representative of three independent experiments. An asterisk indicates that the number of spots obtained when CTLs were generated with CXCR3+CD4+/DC was significantly higher than the mDC and CD4+/DC (*P = 0.031). (B) The CTLs (as responders) were tested against peptide or empty loaded LCLs as stimulators at a ratio of 10:1. Spots were counted by computer-assisted image analysis. Asterisks indicate that the number of spots obtained when CTLs were generated with CXCR3+CD4+/DC was significantly higher (*P = 0.05 compared to mDC; **P = 0.0092 compared to CD4+/DC). A representative IFN-γ ELISPOT experiment of three performed is shown.
To examine the proliferated T cells are antigen specific, the frequency of IFN-γ secreting CD8+ T cells against WT-1-peptide loaded targets was measured by ELISPOT assay to further assess the relative priming activity of DCs matured with CXCR3+CCR4-CD4+ T cells. As shown in Figure 3B, the highest frequency of IFN-γ secreting CD8+ T cells specific for WT-1 was observed from the CTLs generated with CXCR3+CD4+/DCs (53 ± 4 spots forming cells per 104 cells), whereas relatively lower IFN-γ spots were formed by those stimulated with mDC (31.5 ± 2 spots) (P = 0.05) and CD4+/DC (22 ± 3 spots) (P < 0.0092), respectively.
The specific lysis of CTLs generated with CXCR3+CD4+/DCs against WT-1 antigen reached relatively higher than that with mDCs and CD4+/DCs (P = 0.04), respectively, at an effector to target ratio of 40:1 (Figure 4A). When the finding from Figure 3A and 4A were combined to represent the overall lytic activity of the CTLs, the differences in the overall lytic potential induced by CXCR3+CD4+/DC became even more prominent. The overall lytic units represent total number of CD8+ T cells possessing cytotoxic activity are generated in a single culture. As shown in Figure 4B, the stimulation of CD8+ T cells with CXCR3+CD4+/DC resulted strongly increased overall effector activity against WT-1 antigen as measured by the total number of lytic units per culture. In contrast, stimulation of effectors with mDC resulted in more than 3 folds lower lytic capacity against WT-1 while CD8+ T cells stimulated with CD4+/DCs elicited about 4 folds lesser capacity than CXCR3+CD4+/DCs against both WT-1. These results demonstrate CXCR3+CD4+/DCs efficiently prime naive T cells against certain weakly immunogenic tumor antigens as measured by the total number of lytic units per culture.
Induction of overall cytolytic activity by CXCR3+CD4+/DCs. WT-1-specific CTL was generated from normal donors, as described in Methods. (A) Cytotoxicity of T-cells generated with three types of DCs against WT-1 were tested in response to peptide-pulsed LCLs (10 µg/ml) at E:T ratios ranging from 40:1 to 20:1 in a standard 4-h 51Cr release assay. Results are expressed as percentage of specific lysis; the percentage of lysis in the presence of peptide (filled) and the percentage of lysis in the absence of peptide (empty). Asterisk indicates that the cytolytic activity of CTLs generated with CXCR3+CD4+/DC at E:T ratio of 40:1 was significantly higher than that obtained with CD4+/DC (*P = .04). (B) Lytic units against WT-1 were calculated from cocultures. The data from Figure 3A and 4A were combined to represent the lytic units resulting from the exposure of effectors to targets. One lytic unit is defined as 30% specific lysis. The calculated lytic unit is the yield of effectors (from Figure 3A) divided by the number of cells required to achieve a single lytic unit. One representative experiment of three performed is shown.
Potency of CXCR3+CD4+/DC in priming CD8+ T cells is due to induction of Th-1 and reduction of immune suppressive cytokine by DC
Given that CXCR3+CD4+/DC was more efficient in CTL generation (Figure 3 and 4), we attempted to characterize the factors that are responsible for such potency. Focusing on the maturation status of DCs, we used flow cytometry to analyze the expression profile of costimulatory and MHC molecules. After 48 h of incubation, both the number of DC expressing maturation markers and the level of expression intensity were increased compared to iDC (Figure 5A). Among the markers examined, CD80 expression was highly upregulated when cocultured with cellular stimuli, including CXCR3+CCR4-CD4+ or CD4+ T cells, than with MC. However, there was no significant difference between the effects of the CXCR3+CCR4-CD4+ and CD4+ T cells on phenotypic expression of DC.
Analysis of maturation markers and type of cytokine secretion by DCs. (A) Immature DCs (1 × 105 cells) were cultured for 48 h with various stimuli. For each marker, expression was plotted for % of marker positive cells (bar graph) and the mean fluorescence intensity (MFI, line) obtained in different conditions. (B) Simultaneous quantification of three cytokines (IL-6, IL-10 and IL-12p70) was performed with CBA assay from 48-h supernatants of DCs (5 × 103 cells). The net concentration is presented here after subtracting the amount secreted by either CXCR3+CCR4-CD4+ or CD4+ T cells themselves. Samples were in triplicate, and the means ± SD of lymphokine levels are shown. The experiments were conducted at least twice with similar results and a representative set of data is presented. An asterisk indicates statistical significance compared between mDC and CXCR3+CD4+/DC (*P = 0.009 and 0.003 for IL-12 and IL-6, respectively) or CD4+/DC (*P = 0.007 for IL-12 and 0.002 for IL-6, respectively).
Next we examined whether activated CXCR3+CCR4-CD4+ T cells influence a pattern of proinflammatory cytokines by DC. As shown in Figure 5B, both of CXCR3+CCR4-CD4+ and CD4+ T cells highly induced secretion of Th-1 polarizing cytokine IL-12p70 compared to mDC (P = 0.009 compared to CXCR3+CD4+/DC and P = 0.03 compared to CD4+/DC). However, considering the level of IL-10 production by mDC as control, the secretion by CXCR3+CD4+/DC was reduced to half while CD4+/DC remained as mDC, despite CD4+ T cells significantly secrete IL-10 as shown in Figure 2A. IL-6 was only measured in supernatants of DCs matured with MC and was rarely detectable in those matured with cellular stimuli (P = 0.007 compared to CXCR3+CD4+/DC and P = 0.002 compared to CD4+/DC). Because T cells also contribute in lymphokines production, the data is presented after subtracting the cytokine production of T cells alone, so that DC is mainly responsible for cytokine production.
Discussion
In this study, CXCR3+CCR4-CD4+ T cells were used to improve CTL generation as well as DC maturation in replacement of typical maturation reagents in vitro. Despite the essential role of Th1-conditioning in CTL cultures, there should be more defined protocol in driving Th1-type responses. Here, the parameter used for distinguishing Th1-type subsets from CD4+ T cells was strictly based on the surface expression of CXCR3+CCR4-chemokine receptor. A small proportion of CXCR3-positive cells (~10%) were found among freshly isolated naive CD4+ T cells, however CXCR3-positive cells were increased to a range of 18 to 21% after seven days without any stimuli given. Although it is not clear of exact mechanism for the change in this receptor expression, in vitro culture environments including fetal calf serum and pH might affect T cells. Nevertheless the change did not alter its original property as confirmed by cytokine profiles after activation with magnetic anti-CD3/CD28 beads. Particularly, the levels of type II cytokines including IL-4, IL-5 and IL-10 were significantly decreased to the basal level in CXCR3+CCR4-CD4+ T cells (Figure 2). Because there has been no definite surface marker to distinguish Th1 cells from the whole CD4+ T cells yet, CXCR3+CCR4- marker was used only to exclude Th2 subpopulations, but not to absolutely purify Th1 cells from the whole CD4+ T cells (Kim et al., 2001). CXCR3+CCR4-CD4+ T subpopulation may include both Th1 and non-Th2 cells which explains the amount of Th1 cytokines produced by CXCR3+CCR4-CD4+ T cells is relatively lower than that of the unsorted CD4+ T cells. However, in spite of the impurity, we assumed that the absence of Th2 cytokines by CXCR3+CCR4-CD4+ T cells enhanced the generation of cytotoxic T cells stimulated by DCs in vitro.
In addition to efficient contribution to CTL generation (Figure 3 and 4), the use of activated CXCR3+CCR4-CD4+ T cells efficiently induced DC differentiation to mature form as determined by upregulation of phenotypic markers and types of cytokine secretion (Figure 5). This approach replaces typically used maturation stimuli including bacterial products, proinflammatory cytokines, and recombinant CD40L (Sato et al., 2004; Palucka et al., 2005; Voigtlander et al., 2006). Because previous studies including our own observation (data not shown) indicated that PGE-2 inhibits IL-12 secretion by DC, we excluded PGE-2 from maturation cocktail and only used LPS and TNF-α. In this way, any external factors that would artificially modulate IL-12 production were avoided, so that a parallel comparison on cytokine pattern of DCs could be done. DC treated with maturation cocktail secreted a significant amount of IL-6, moderate IL-10 and a basal level of IL-12 in contrast to CXCR3+CD4+/DC that secreted a basal level of IL-6, low IL-10 and high IL-12. IL-6 induces differentiation of bystander DC into a semi-matured state when secreted by semi-matured DC, which inhibit the induction of proinflammatory Th1 responses. Moreover, when T cells are cultured in accumulated IL-6, IL-4 expression and differentiation of Th2-polarized T cell was observed (Frick et al., 2006). CXCR3+CD4+ T cells did not promote IL-10 production compared to the level secreted by mDC and CD4+/DC, while IL-12p70 was continuously secreted in high level. The use of Th1 cells in DC maturation provides an alternative way to overcome the lack of sustained IL-12 synthesis associated with bacterial stimulus.
In spite of the emphasis on the CXCR3+CCR4-CD4+ T subpopulations, this purified population did not show dramatic differences in inducing DC maturation compared with total CD4+ T cells (Figure 5). Moreover, unsorted CD4+ T cells induced IL-12 as efficiently as CXCR3+CCR4-CD4+ T cells (Figure 5B). Based on the previous study by Hoffmann et al, we attribute such observation to the two factors, IFN-γ and CD40L. Despite there is a mixture of population in CD4+ T cells, the activated CD4+ T cells also secrete IFN-γ and express CD40L (data not shown) which induces significant production of IL-12 by DC. A previous study demonstrated that the production of IL-12 was blocked by an anti-CD40L antibody or by separation of the DC and activated T cell fractions by a permeable membrane (Kim et al., 2003). However when the idea was tested further for CTL generation, CXCR3+CD4+/DC used in the CTL culture resulted in a significant increase in the yield of cell numbers, and the overall lytic unit of these CTLs compared to CD4+/DC (Figure 3 and 4). Although the difference in IFN-γ production shown in Figure 3B seems to be statistically significant, the difference in cytotoxity is only minor when CTLs were expanded with CXCR3+CD4-/DCs. We reason the discrepancy that ELISPOT assay is known as more sensitive and quantitative than cytotoxicity assay. Recently, IFN-γ ELISPOT assay has gained increasing popularity for monitoring clinical trials due to its great sensitivity. However IFN-γ ELISPOT alone may not be sufficient because noncytotoxic cells can secrete IFN-γ whereas CTL with lytic activity do not always secrete IFN-γ. This observation is correlated with the previous study that a diverse pool of CTLs with different clonal origins can exert identical cytotoxic effector function against target cells, but exhibit qualitatively different functional behaviors in terms of proliferation and cytokine secretion (Lim et al., 2000). In addition to providing Th1 signals to DCs, the costimulatory molecules on the surface of CXCR3+CCR4-CD4+ T cells might have also provided Th1 signals to CD8+ T cells by cross-linking with the known CTL surface molecules such as TCR, CD70 and CD137 (4-1BB) during the CTL culture, resulting in their expansion and increased overall cytolytic function compared to other conditions (Kim et al., 2003). It has been reported that stimulation with antibodies specific to MHC class II, CD27 and CD147 enhanced the proliferate response of CTLs to TCR activation (Giuntoli et al., 2002). In contrast, two possible factors can be suggested to speculate how the presence of the whole CD4+ T cells exerts these opposing effects on the CTLs. The first is the type of stimulus given to CD4+ T cells. In contrast to previous studies on tetanus toxoid induced T-cell help (Ostankovitch et al., 1997; Eiz-Vesper et al., 2006), we used anti-CD3/28 magnetic beads to activate freshly isolated CD4+ T cells resulting in nonspecific activation of nonspecific subpopulations. The second is the inhibitory factors produced by the subpopulations including Th2 and regulatory T cells within CD4+ T cells, resulting in reduction of CTL proliferation and the relatively low quality of their effector function (Jin et al., 2000; Osada et al., 2005).
In this work, we provide evidence that Th1-type cells expressing CXCR3+CCR4-CD4+ molecules make more Th1-type cytokines and influence DC activation, and thus results in enhancement of CD8+ effector T cell activity. To our belief, this is the first study showing that the selective use of Th1-type cells assist DC maturation towards Th1-type response and DC matured by Th1-type cells showed stronger capacity of inducing antigen specific CTLs in vitro. However, we realize that the precise mechanism that leads to the enhancement of CD8+ response is not directly addressed here and were only able to present the representative data that IL-12 induces Th1-type response and IL-10 and IL-6 possibly inhibit CD8+ response. However, we can conclude that the effect of Th1 T cells is more likely mediated by both soluble factors secreted by Th1 cells and cell-to-cell interaction, and the cytokine profile of DC was changed towards Th1-type response when activated with CXCR3+CCR4-CD4+ T cells (Figure 5), resulting in enhancement of CD8+ response. In spite of similar changes in the phenotype of the DC, the effect of CXCR3+CD4+/DC on CD8+ response correlates with the previous report that CTL responses can be enhanced in vitro when the expression of IL-10 in DC stimulated with LPS and TNF-α was silenced by RNAi instead of blocking anti-IL-10 antibodies even though was no change on MHC class II, CD86, and CD54 expression (Gentao et al., 2004). Moreover DC cultured with type I soluble cytokines including IL-12 and IFN-γ induced the differentiation of IFN-γ-producing Th1 cells, which are essential for the generation of CTL against tumor (Steinbrink et al., 1997). Nonetheless, we strongly believe that the precise molecular mechanism should be defined further.
The findings here propose that the efficient generation of CTLs result from the ability of CXCR3+CCR4-CD4+ T cells to provide Th1 skewed signals. This work also highlights the importance of a physiological relevant system for CTL generation and APC maturation to augment antitumor responses in vitro. Further studies for efficient isolation of Th1 cells, involved immune molecules and in vivo animal model should be performed to translate this approach to clinical applications.
Methods
Blood samples and cell separation
PBMC from HLA A2+healthy individuals was isolated by Ficoll density gradient centrifugation (Amersham Pharmacia, Piscataway, NJ). CD14+ monocytes and CD4+, CD8+ T lymphocytes were isolated from PBMCs using marker specific microbeads with AutoMACS (Miltenyi Biotec, Bergisch Gladbach, Germany). Each MACS purification was done by positive selection. The purity of subpopulation cells was 95.5% (SD, 0.9%). Consent forms and approval for this study were obtained from the donors and the institutional review board of The Catholic University of Korea, College of Medicine.
Culture conditions and DC generation
Culture experiments were performed in RPMI 1640 with 10% FBS (Sigma-Aldrich, St. Louis, MO). For DC generation, isolated CD14+ cells were cultured for 6 days in RPMI complete medium containing 100 ng/ml GM-CSF (Endogen, Woburn, MA) and 500 U/ml IL-4 (Genzyme, Cambridge, MA). 75 to 80% of the cells showed morphologic and immunophenotypical features of typical DCs, which included the expression of MHC class I and class II molecules and CD86. The medium was replenished with cytokines after 3-4 days. On day 6, final maturation was induced by the addition of either maturation cocktail including 1000 U/ml TNF-α and 1 µg/ml LPS (Sigma-Aldrich, St. Louis, MO), or helper T cells at a ratio of 1:5 in the presence of anti-CD3/CD28 magnetic beads (Dynal Biotech, Lake Success, NY) for an additional 48 h.
Flow cytometry studies
For cell surface staining, cells were processed following standard procedures, and analysis was performed on a FACSCalibur flow cytometer (BD Biosciences, San Jose, CA). The mAbs to CD4, CD8, CD80, CD83, CD86, HLA-ABC and HLA-DR were purchased from BD Pharmingen (San Diego, CA). After CD4+ T cells isolation using microbeads (Miltenyi, Auburn, CA), cells were stained with fluorescence-conjugated monoclonal antibodies against CXCR3 and CCR4 from BD Pharmingen (San Diego, CA). Populations of cells enriched for CXCR3+CCR4- Th1 subsets were isolated by FACs vantage. This produced isolates containing predominantly CXCR3high/CCR4low.
Cytokine assay
Immature DCs were stimulated in 96-well culture plates (5 × 103 cells/well in 200 µl vol.) or 24-well culture plates (2 × 104 cells/well in 1 ml vol.) in the presence of maturation cocktail (MC) or helper T cells with anti-CD3/CD28 magnetic beads at a ratio of 1:5 (DC:helper T cells), and cultured for 48 h at 37℃. The 50 µl of cultured supernatants were removed and stored at -20℃, and analyzed for cytokine production with a Cytometric Bead Array (CBA) kit (BD Biosciences, San Diego, CA), Bio-Plex Cytokine Assays (BioRad, CA) or ELISA (Pierce, Rockford, IL) according to the manufacturer's instructions. The lower limit of detection for each cytokine was 20 pg/ml.
CBA analysis
Th1 (IL-2, IFN-γ, TNF-α) and Th2 cytokines (IL-4, IL-5 and IL-10) were quantified simultaneously using a Human Th1/Th2 cytokine Cytometric bead array kit and CBA software (BD Pharmingen, San Jose, CA). This array kit provides a mixture of five microbeads. Inflammatory cytokines (IL-6) was also simultaneously quantified using a CBA Flex Set and FCAP Array software (BD Pharmingen, San Jose, CA). Populations with distinct fluorescent intensities (FL-3) are pre coated with antibodies specific for each cytokine. Fifty microliters of serum and the provided standard cytokines were added to the premixed microbeads in 12 × 75 mm Falcon tubes (BD Biosciences, San Jose, CA). Mixture of catching beads with samples were incubated for two hours and after the addition of 50 µl of a mixture of PE conjugated antibodies against the cytokines, the mixture was further incubated for 2 h in the dark at the room temperature. This mixture was washed and centrifuged at 500 × g for 5 min and the pellet was resuspended in 300 µl of wash buffer. The FACSCalibur flow cytometer (BD Biosciences, San Jose, CA) was calibrated with setup beads and 1200 events were acquired for each sample. Individual cytokine concentration ratios were indicated by picogram per milliliter.
Generation of WT-1 specific CTLs with autologous DCs
The DCs matured with various stimuli were pulsed with HLA-A02-restricted Wilm's Tumor antigen 1 (WT-1) peptide (RMFPNAPYL) at 10 µg/ml for 2 h, and then irradiated with a dose of irradiation (25 Gy) that entirely prevented outgrowth of matured DCs and added Th cells in the control. The irradiated matured DCs and activated Th cells were seeded into 24-well plates at 1 × 105 and 2 × 105 cells per well. The purified CD8+ T cells were then added to make a 1:10 ratio of DC to T cells per well. After 7 days of coculturing, the stimulated cells were harvested and resuspended at 1 × 106 per well. They were then restimulated with 1 × 105 peptide-pulsed irradiated DCs and 2 × 105 of Th cells. After the second stimulation, every 3 to 4 days, the cells were fed with 10 U/ml interleukin 2 (IL-2; Genzyme, Cambridge, MA) and interleukin 15 (IL-15; R&D Systems, Minneapolis, MN). The cells were harvested either 14 or 21 days later since the initial stimulation and assayed immediately.
IFN-γ ELISPOT assay
The ELISPOT assay was performed as described in the manufacturer's instructions (BD Biosciences, San Diego, CA). Briefly, peptide pulsed autologous Lymphoblastoid cell line (LCL) expressing HLA-A02 as stimulator cells and antigen specific T-cells as responder cells were plated at 1 × 103 and 1 × 104/well, respectively. Responder cell populations were seeded across a range of concentrations to achieve 10 to 100 spots/well so as to facilitate accurate and reproducible counting. All cells were cultured in RPMI-FBS 10% supplemented to a final volume of 100 µl/well. After undisturbed incubation for 20 to 24 h at 37℃, with 5% CO2, plates were washed 4 times with PBS containing 0.05% Tween 20 (PBS/0.05% Tw). Wells were incubated with biotinylated "detection" antibody against IFN-γ (BD Biosciences, San Diego, CA). The plates were washed 4 times with PBS/0.05% Tw. Avidin-peroxidase-complex (AEC, 100 µl; prepared according to manufacturer's instructions; BD Biosciences, San Diego, CA) was added per well for 1 h at room temperature. The plates were washed 3 times with PBS/0.05% Tw, followed by 3 washes with PBS. AEC substrate (BD Biosciences, San Diego, CA) was prepared according to the manufacturer's instructions and filtered through a 0.45-µM filter prior to use. Per well, 100 µl was added. After 5 to 60 min the reaction was stopped with deionized water and the plates were dried completely prior to membrane removal. The spot number was determined in an independent blinded fashion (AID, Germany). In each experiment, the result was expressed as spots/10000 cells and the results of 3 experiments were used to calculate means and standard deviations.
Cytotoxic assay
The cytotoxic activity of CTLs was measured by a 4 h 51chronium release assay. Briefly, peptide pulsed autologous LCLs (1 × 104 cells) were used as target cells with antigen specific T-cells as effector cells at different effectortarget cell ratios (20:1 to 40:1). Experiments were performed in triplicates and the percentage of lysis was calculated as 100% × (experimental release-spontaneous release)/(maximum release-spontaneous release). Maximum release was obtained by adding 100 µl of 0.2% Triton X-100 to the 100 µl medium containing target cells. Where indicated, data is represented as lytic units 30 (LU30), where one lytic unit is the number of cells derived from the culture necessary to achieve 30% specific lysis of targets. The total number of lytic units was obtained by the formula: [total no. of effectors obtained after the secondary culture]/[no. of effectors required to achieve 30% lysis (LU30)]. SD is derived from the maximum and minimum slopes of lines through the mean ± SD of the percent specific lysis in the specific region of curve.
Statistical analysis
Control values for each experiment were derived from pooled data on a number of control individuals so that each experiment has a single control value, mean, and standard deviation. Each mean variance was then compared against the control response for each experiment and analyzed for statistical significance using a one-tail unpaired t test, assuming unequal variance between the experimental groups. Significant differences are indicated by asterisks.
Abbreviations
- APC:
-
antigen presenting cell
- DC:
-
dendritic cell
- CTL:
-
cytotoxic T lymphocyte
References
Chattopadhyay S, Chakraborty NG . Continuous presence of Th1 conditions is necessary for longer lasting tumor-specific CTL activity in stimulation cultures with PBL . Hum Immunol 2005 ; 66 : 884 - 891
Cosmi L, Annunziato F, Galli MIG, Maggi RME, Nagata K, Romagnani S . CRTH2 is the most reliable marker for the detection of circulating human type 2 Th and type 2 T cytotoxic cells in health and disease . Eur J Immunol 2000 ; 30 : 2972 - 2979
Eiz-Vesper B, Horn PA, Daubert C, Khattab B, Blasczyk R . Tetanus toxoid provides efficient T-cell help for the induction of HA-1(H) cytotoxic T cells . Transfusion 2006 ; 46 : 1210 - 1220
Frick JS, Zahir N, Muller M, Kahl F, Bechtold O, Lutz MB, Kirschning CJ, Reimann J, Jilge B, Bohn E, Autenrieth IB . Colitogenic and non-colitogenic commensal bacteria differentially trigger DC maturation and Th cell polarization: An important role for IL-6 . Eur J Immunol 2006 ; 36 : 1537 - 1547
Gao FG, Khammanivong V, Liu WJ, Leggatt GR, Frazer IH, Fernando GJ . Antigen-specific CD4+ T-cell help is required to activate a memory CD8+ T cell to a fully functional tumor killer cell . Cancer Res 2002 ; 62 : 6438 -
Gentao L, Hiushan N, Yasuharu A, Xiangpeng Y, Moneeb E, Dong Y, Keith LB, John SY . Small interference RNA modulation of IL-10 in human monocyte-derived dendritic cells enhances the Th1 response . Eur J Immunol 2004 ; 34 : 1680 - 1687
Giuntoli RL, Lu J, Kobayashi H, Kennedy R, Celis E . Direct costimulation of tumor-reactive CTL by helper T cells potentiate their proliferation, survival, and effector function . Clin Cancer Res 2002 ; 8 : 922 - 931
Hoffmann TK, Meidenbauer N, Muller-Berghaus J, Storkus WJ, Whiteside TL . Proinflammatory cytokines and CD40 ligand enhance cross-presentation and cross-priming capability of human dendritic cells internalizing apoptotic cancer cells . J Immunother 2001 ; 24 : 162 - 171
Janssen EM, Droin NM, Lemmens EE, Pinkoski MJ, Bensinger SJ, Ehst BD, Griffith TS, Green DR, Schoenberger SP . CD4+ T-cell help controls CD8+ T-cell memory via TRAIL-mediated activation-induced cell death . Nature 2005 ; 434 : 88 -
Jin Y, Fuller L, Wei Y, Blomberg BB, Miller J, Esquenazi V . Bone marrow cells promote TH2 polarization and inhibit virus-specific CTL generation . Hum Immunol 2000 ; 61 : 1233 - 1241
Kim CH, Rott L, Kunkel EJ, Genovese MC, Andrew DP, Wu L, Butcher EC . Rules of chemokine receptor association with T cell polarization in vivo . J Clin Invest 2001 ; 108 : 1331 - 1339
Kim CH, Nagata K, Butcher EC . Dendritic cells support sequential reprogramming of chemoattractant receptor profiles during naive to effector T cell differentiation . J Immunol 2003a ; 171 : 152 - 158
Kim J, Choi SP, La S, Seo JS, Kim KK, Nam SH, Kwon B . Constitutive expression of 4-1BB on T cells enhances CD4+ T cell responses . Exp Mol Med 2003b ; 35 : 509 - 517
Knutson KL, Disis ML . Tumor antigen-specific T helper cells in cancer immunity and immunotherapy . Cancer Immunol Immunother 2005 ; 54 : 721 - 728
Larmonier N, Marron M, Zeng Y, Cantrell J, Romanoski A, Sepassi M, Thompson S, Chen X, Andreansky S, Katsanis E . Tumor-derived CD4(+)CD25(+) regulatory T cell suppression of dendritic cell function involves TGF-beta and IL-10 . Cancer Immunol Immunother 2007 ; 56 : 48 - 59
Lim D, Bourcier KB, Freeman G . Examination of CD8+ T cell function in humans using MHC class I tetramers: similar cytotoxicity but variable proliferation and cytokine production among different clonal CD8+ T cells specific to a single viral epitope . J Immunol 2000 ; 165 : 6214 - 6220
Lukacs NW . Role of chemokines in the pathogenesis of asthma . Nat Rev Immunol 2001 ; 1 : 108 -
Lutz MB, Schuler G . Immature, semi-mature and fully mature dendritic cells: which signals induce tolerance or immunity ? Trends Immunol 2002 ; 23 : 445 - 449
Lyakh LA, Sanford M, Chekol S, Young HA, Roberts AB . TGF-beta and vitamin D3 utilize distinct pathways to suppress IL-12 production and modulate rapid differentiation of human monocytes into CD83+ dendritic cells . J Immunol 2005 ; 174 : 2061 - 2670
Mackay CR . Chemokine receptors and T cell chemotaxis . J Exp Med 1996 ; 184 : 799 - 802
Mocellin S . Priming anticancer active specific immunotherapy with dendritic cells . Curr Opin Investig Drugs 2005 ; 6 : 576 - 581
Mosmann TR, Coffman RL . TH1 and TH2 cells: different patterns of lymphokine secretion lead to different functional properties . Annu Rev Immunol 1989 ; 7 : 145 - 173
Nishimura T, Iwakabe K, Sekimoto M, Ohmi Y, Yahata T, Nakui M, Sato T, Habu S, Tashiro H, Sato M, Ohta A . Distinct role of antigen-specific T helper type 1 (Th1) and Th2 cells in tumor eradication in vivo . J Exp Med 1999 ; 190 : 617 -
Osada T, Morse MA, Lyerly HK, Clay TM . Ex vivo expanded human CD4+ regulatory NKT cells suppress expansion of tumor antigen-specific CTLs . Int Immunol 2005 ; 17 : 1143 - 1155
Ostankovitch M, Le Gal FA, Connan F, Chassin D, Choppin J, Guillet JG . Generation of Melan-A/MART-1-specific CD8+ cytotoxic T lymphocytes from human naive precursors: helper effect requirement for efficient primary cytotoxic T lymphocyte induction in vitro . Int J Cancer 1997 ; 72 : 987 - 994
Palucka AK, Laupeze B, Aspord C, Saito H, Jego G, Fay J, Paczesny S, Pascual V, Banchereau J . Immunotherapy via dendritic cells . Adv Exp Med Biol 2005 ; 560 : 105 - 114
Prilliman KR, Lemmens EE, Palioungas G, Wolfe TG, Allison JP, Sharpe AH, Schoenberger SP . Cutting edge: a crucial role for B7-CD28 in transmitting T help from APC to CTL . J Immunol 2002 ; 169 : 4094 - 4097
Sato T, Terai M, Yasuda R, Watanabe R, Berd D, Mastrangelo MJ, Hasumi K . Combination of monocyte-derived dendritic cells and activated T cells which express CD40 ligand: a new approach to cancer immunotherapy . Cancer Immunol Immunother 2004 ; 53 : 53 - 61
Steinbrink K, Wolfl M, Jonuleit H, Knop J, Enk AH . Induction of tolerance by IL-10-treated dendritic cells . J Immunol 1997 ; 159 : 4772 - 4780
Surman DR, Dudley ME, Overwijk WW, Restifo NP . Cutting edge: CD4+ T cell control of CD8+ T cell reactivity to a model tumor antigen . J Immunol 2000 ; 164 : 562 -
Voigtlander C, Rossner S, Cierpka E, Theiner G, Wiethe C, Menges M, Schuler G, Lutz MB . Dendritic cells matured with TNF can be further activated in vitro and after subcutaneous injection in vivo which converts their tolerogenicity into immunogenicity . J Immunother 2006 ; 29 : 407 - 415
Ward SG, Bacon K, Westwick J . Chemokines and T lymphocytes: more than an attraction . Immunity 1998 ; 9 : 1 - 11
Zhang Y, Wakita D, Chamoto K, Narita Y, Matsubara N, Kitamura H, Nishimura T . Th1 cell adjuvant therapy combined with tumor vaccination: a novel strategy for promoting CTL responses while avoiding the accumulation of Tregs . Int Immunol 2007 ; 19 : 151 - 161
Acknowledgements
This study was supported by a grant from the National R&D Program for Cancer Control, Ministry of Health and Welfare, Republic of Korea (0620320).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Yoon, S., Yun, S., Park, J. et al. Selective addition of CXCR3+CCR4-CD4+ Th1 cells enhances generation of cytotoxic T cells by dendritic cells in vitro. Exp Mol Med 41, 161–170 (2009). https://doi.org/10.3858/emm.2009.41.3.019
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.3858/emm.2009.41.3.019
Keywords
This article is cited by
-
Phase I clinical trial of multiple-peptide vaccination for patients with advanced biliary tract cancer
Journal of Translational Medicine (2014)
-
Human IP10-scFv and DC-induced CTL synergistically inhibit the growth of glioma in a xenograft model
Tumor Biology (2014)
-
CXCR3 ligands: redundant, collaborative and antagonistic functions
Immunology & Cell Biology (2011)