Abstract
Growing evidence suggests a distinction between water intake necessary for maintaining a euhydrated state, and water intake considered to be adequate from a perspective of long-term health. Previously, we have proposed that maintaining a 24-h urine osmolality (UOsm) of ⩽500 mOsm/kg is a desirable target for urine concentration to ensure sufficient urinary output to reduce renal health risk and circulating vasopressin. In clinical practice and field monitoring, the measurement of UOsm is not practical. In this analysis, we calculate criterion values for urine-specific gravity (USG) and urine color (UCol), two measures which have broad applicability in clinical and field settings. A receiver operating characteristic curve analysis performed on 817 urine samples demonstrates that a USG ⩾1.013 detects UOsm>500 mOsm/kg with very high accuracy (AUC 0.984), whereas a subject-assessed UCol⩾4 offers high sensitivity and moderate specificity (AUC 0.831) for detecting UOsm >500 m Osm/kg.
Similar content being viewed by others
Introduction
Water is essential to life, represents the largest single nutrient in terms of intake, and must be replenished daily through food and fluid consumption. Adequate intakes have been established based upon population median data. However, adequate intakes are not linked to specific health outcomes, and daily water needs are highly individual and depend upon environment, activity, diet and other factors. Thus, a dietary reference value for the general population is unlikely to have much relevance for the individual. Various biomarkers of urine concentration allow for individual-level daily hydration monitoring. Specifically, urine osmolality (UOsm) is the most precise, non-invasive biomarker available to evaluate the 24-h hydration process, as it represents the net sum of water gains, losses and neuroendocrine responses that act to maintain body water homeostasis, and responds rapidly to changes in daily water intake.1, 2 Recently, we proposed a 24-h UOsm of ⩽500 mOsm/kg as a reasonable target for urine concentration, reflecting sufficient total water intake to compensate daily losses, reduce circulating vasopressin and ensure sufficient urinary output to reduce the risk of some renal health outcomes.3 However, one limitation to a target based upon UOsm is that it is not easily measured day to day; moreover, clinicians, coaches and dietitians lack the possibility to measure UOsm within their practices or in the field, limiting its utility as a hydration monitoring tool for the larger population. Two alternate methods for measuring urine concentration with greater clinical and field applicability are urine-specific gravity (USG), which can easily be measured by clinicians, and urine color (UCol), which may be self-assessed. To date, no criterion values for USG nor UCol, corresponding to a UOsm of 500 mOsm/kg, have been published. Thus, the objective of this analysis was to calculate the criterion values for USG and subject-assessed UCol, which would have the best diagnostic accuracy for identifying UOsm>500 mOsm/kg.
Methods
Eighty-two healthy French adults (23.6±2.9 years; 22.2±1.5 kg/m2; 41 women) provided informed consent (CPP Est-III, Nancy, France) and collected all individual voids produced over 1–4 consecutive days as part of a larger study (NCT02044679). On collection days, subjects woke up before 0700 hours, voided and discarded this first morning sample. Subsequent voids were collected in individual, clear plastic containers, including the first morning void of the following morning at 0700 hours. For each void, participants self-evaluated UCol using Armstrong et al.’s color scale, under consistent lighting conditions.4 Once samples were returned to the laboratory, USG (Pen Urine S.G.; Atago, Japan) and UOsm (Advanced Model 2020 Multi-Sample Osmometer; Advanced Instruments, Inc., Norwood, MA, USA) were measured.
Logistic regression curves were generated with USG and UCol as predictor variables, and UOsm as a binary outcome variable, with UOsm >500 mOsm/kg defined as ‘condition present’, and UOsm⩽500 mOsm/kg as ‘condition absent’. The optimal cutoffs for USG and UCol for identifying UOsm >500 mOsm/kg were determined by receiver operating characteristic (ROC) curve analysis. We were equally interested in evaluating sensitivity (if UOsm is >500 mOsm/kg, how often will USG, UCol be at or above the cutoff values?) and specificity (if UOsm is ⩽500 mOsm/kg, how often will USG, UCol be below the cutoff values?); thus, our analysis favored neither sensitivity nor specificity.
Results
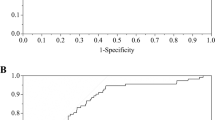
A total of 817 urine samples were analyzed for UOsm and USG. One sample had a missing value for UCol (816 samples). The mean (5th; 95th percentile) for UOsm, USG and UCol, respectively, were 436 (192; 938) mOsm/kg, 1.012 (1.003; 1.025) and 4 (1; 7). The ROC analysis revealed the optimal USG cutoff for identifying UOsm >500 mOsm/kg was 1.013 (AUC 0.984), whereas the cutoff for UCol was 4 (AUC 0.831) (Figure 1). A USG of ⩾1.013 offered very high sensitivity and high specificity; whereas a UCol of ⩾4 had good sensitivity and moderate specificity (Table 1).
Discussion
Insufficient water intake or low urinary output has been associated with health outcomes, including recurrent kidney stones, increased risk of renal insufficiency and impaired glucose regulation.5, 6, 7 A UOsm of less than 500 mOsm/kg has been proposed as a reasonable target for ‘optimal hydration’,3 but UOsm is not a practical field measure and to date, no corresponding values for USG nor UCol have been published. In this analysis, we demonstrate that both UCol and USG may be used as surrogates for UOsm to identify individuals above or below the 500 mOsm/kg target. USG is both sensitive and specific, suggesting its utility for health care professionals and clinicians within their daily practice. Subject-assessed UCol demonstrated good sensitivity and moderate specificity. To our knowledge, this is the first subject-self-assessment of UCol by healthy adults, confirming UCol as a practical field measure with utility in day-to-day individual hydration monitoring.
These findings confirm and build upon recent work by McKenzie et al.,8 who validated a UCol of 4 or greater as a practical field measure for detecting UOsm>500 mOsm/kg in pregnant and breastfeeding women. Moreover, our USG and UCol criterion values for detecting UOsm >500 mOsm/kg (1.013 or higher, and 4 or higher, respectively) are similar to those first published by Armstrong et al., who reported that in a sample of young, mostly male college students, for a sample with UCol of 3 or lower, the respective mean UOsm and USG were less than 520 mOsm/kg and 1.014.4
Finally, the USG and UCol criterion values for UOsm <500 mOsm/kg continue to build upon a new but growing distinction between the hydration state (acute dehydration), the upper limit of euhydration and being well-hydrated from the perspective of disease risk. Cheuvront et al.’s decision levels for detecting dehydration (body mass loss of 3.7±1.0%) based upon UOsm and USG were 1018 ±245 mOsm/kg and 1.028 ±0.006, respectively,9 whereas an acceptable euhydration cutoff has been reported as <70010 to <8301 mOsm/kg for UOsm and <1.020 for USG.10 This paper complements the existing literature by providing calculated cutoff values for USG (⩾1.013) and self-assessed UCol (⩾4) that accurately detect UOsm>500 mOsm/kg. Given the recent associations between low water intake, low urine output and some renal and metabolic health outcomes,5, 6, 7 we propose remaining below these cutoff values as a target for being well or optimally hydrated.
References
Manz F, Wentz A . 24-h hydration status: parameters, epidemiology and recommendations. Eur J Clin Nutr 2003; 57 (Suppl 2), S10–S18.
Perrier ET, Armstrong LE, Daudon M, Kavouras S, Lafontan M, Lang F et al. From state to process: defining hydration. Obes Facts 2014; 7 (Suppl 2), 6–12.
Perrier ET, Buendia-Jimenez I, Vecchio M, Armstrong LE, Tack I, Klein A . Twenty-four-hour urine osmolality as a physiological index of adequate water intake. Dis Markers 2015; 2015: 231063.
Armstrong LE, Maresh CM, Castellani JW, Bergeron MF, Kenefick RW, LaGasse KE et al. Urinary indices of hydration status. Int J Sport Nutr 1994; 4: 265–279.
Borghi L, Meschi T, Amato F, Briganti A, Novarini A, Giannini A . Urinary volume, water and recurrences in idiopathic calcium nephrolithiasis: a 5-year randomized prospective study. J Urol 1996; 155: 839–843.
Clark WF, Sontrop JM, Macnab JJ, Suri RS, Moist L, Salvadori M et al. Urine volume and change in estimated gfr in a community-based cohort study. Clin J Am Soc Nephrol 2011; 6: 2634–2641.
Roussel R, Fezeu L, Bouby N, Balkau B, Lantieri O, Alhenc-Gelas F et al. Low water intake and risk for new-onset hyperglycemia. Diabetes Care 2011; 34: 2551–2554.
McKenzie AL, Munoz CZ, Ellis LA, Perrier ET, Guelinckx I, Klein A et al. Urine colour as an indicator of urine concentration in pregnant and lactating women. Eur J Nutr. epub ahead of print 16 November 2015 doi:10.1007s00394-015-1085-9.
Cheuvront SN, Sawka MN . Hydration assessment of athletes. Sports Sci Exchange 2005; 18: 1–6.
Sawka MN, Burke LM, Eichner ER, Maughan RJ, Montain SJ, Stachenfeld NS . American College of Sports Medicine position stand. Exercise and fluid replacement. Med Sci Sports Exerc 2007; 39: 377–390.
Acknowledgements
The authors are employees of Danone Research, who funded this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Perrier, E., Bottin, J., Vecchio, M. et al. Criterion values for urine-specific gravity and urine color representing adequate water intake in healthy adults. Eur J Clin Nutr 71, 561–563 (2017). https://doi.org/10.1038/ejcn.2016.269
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.269
This article is cited by
-
Validity of combined hydration self-assessment measurements to estimate a low vs. high urine concentration in a small sample of (tactical) athletes
European Journal of Nutrition (2024)
-
The predictive value of urine specific gravity in the diagnosis of vasovagal syncope in children and adolescents
Italian Journal of Pediatrics (2021)
-
Associations between urinary hydration markers and metabolic dysfunction: a cross-sectional analysis of NHANES data, 2008–2010
European Journal of Nutrition (2021)
-
Hydration for health hypothesis: a narrative review of supporting evidence
European Journal of Nutrition (2021)
-
A lavatory urine color (LUC) chart method can identify hypohydration in a physically active population
European Journal of Nutrition (2021)