Abstract
Background/Objectives:
Consuming the evening meal in the company of others has been associated with overall diet quality. Nevertheless, studies on the association between type of company at dinner and diet quality in adults are scarce.
Subjects/Methods:
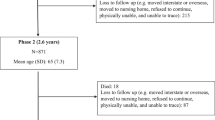
Dutch men (n=895) and women (n=845) aged between 20 and 70 years, included in a population-based observational study, were studied. Dietary intake was assessed by multiple 24-h recalls (6013 recalls) to estimate the Dutch Healthy Diet index (0–80 points) representing daily diet quality. Sex-specific linear mixed models adjusting for covariates were calculated. Out-of-home dinners and company at dinner were strongly associated (r=0.66), and hence in additional analyses, out-of-home dinners were excluded to avoid multicollinearity.
Results:
Among men, daily diet quality was similar when dinners were consumed in company or consumed alone, but higher when dinner was accompanied by family (mean 46.0, s.e. 0.3) than when dinner was accompanied by others (mean 42.3, s.e. 0.7; P=0.001). Adjustment for dinner location attenuated this association, but it remained significant when excluding out-of-home dinners. Among women, daily diet quality was lower when dinner was consumed in company (mean 48.9, s.e. 0.3) than when consumed alone (mean 51.1, s.e. 0.6; P<0.001). Dinners consumed in the company of family were associated with higher daily diet quality (mean 49.3, s.e. 0.4) than dinners consumed with others (mean 45.7, s.e. 0.6; P=0.001). These associations persisted when excluding out-of-home dinners.
Conclusions:
Only among women, dinners consumed alone as compared with dinners in company were associated with higher diet quality. In both men and women, dinners consumed with family were associated with higher diet quality as compared with dinners with others.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Sobal J, Nelson MK . Commensal eating patterns: a community study. Appetite 2003; 41: 181–190.
Reicks M, Degeneffe D, Rendahl A, Smith Edge M, Burns K, O'Meara B et al. Associations between eating occasion characteristics and age, gender, presence of children and BMI among U.S. adults. J Am Coll Nutr 2014; 33: 315–327.
Holme L Family meals. In: Kjaernes U (ed), Eating Patterns: A Day in the Lives of Nordic Peoples. National Institute for Consumer Research: Lysaker, 2001, pp 199–212. SIFO report.
Sobal J, Hanson K . Family dinner frequency, settings and sources, and body weight in US adults. Appetite 2014; 78: 81–88.
Liu JL, Han B, Cohen DA . Associations between eating occasions and places of consumption among adults. Appetite 2015; 87: 199–204.
Cruwys T, Bevelander KE, Hermans RC . Social modeling of eating: a review of when and why social influence affects food intake and choice. Appetite 2015; 86: 3–18.
Herman CP . The social facilitation of eating. A review. Appetite 2015; 86: 61–73.
Fulkerson JA, Larson N, Horning M, Neumark-Sztainer D . A review of associations between family or shared meal frequency and dietary and weight status outcomes across the lifespan. J Nutr Educ Behav 2014; 46: 2–19.
Wirfält E, Drake I, Wallström P . What do review papers conclude about food and dietary patterns? Food Nutr Res 2013, e-pub ahead of print 4 March 2013 doi:10.3402/fnr.v57i0.20523.
Schwingshackl L, Hoffmann G . Diet quality as assessed by the Healthy Eating Index, the Alternate Healthy Eating Index, the Dietary Approaches to Stop Hypertension score, and health outcomes: a systematic review and meta-analysis of cohort studies. J Acad Nutr Diet 2015; 115: 780–800e5.
Woodruff SJ, Hanning RM, McGoldrick K, Brown KS . Healthy eating index-C is positively associated with family dinner frequency among students in grades 6-8 from Southern Ontario, Canada. Eur J Clin Nutr 2010; 64: 454–460.
Veugelers PJ, Fitzgerald AL, Johnston E . Dietary intake and risk factors for poor diet quality among children in Nova Scotia. Can J Public Health 2005; 96: 212–216.
Holm L, Lund TB, Niva M . Eating practices and diet quality: a population study of four Nordic countries. Eur J Clin Nutr 2015; 69: 791–798.
Sobal J, Hanson K . Family meals and body weight in US adults. Public Health Nutr 2011; 14: 1555–1562.
Conway JM, Ingwersen LA, Vinyard BT, Moshfegh AJ . Effectiveness of the US Department of Agriculture 5-step multiple-pass method in assessing food intake in obese and nonobese women. Am J Clin Nutr 2003; 77: 1171–1178.
NEVO-tabel, Dutch Food Composition Table 2011/version 3. 2011, RIVM/Dutch Nutrition Centre.
van Lee L, Feskens EJ, Hooft van Huysduynen EJ, de Vries JH, van't Veer P, Geelen A . The Dutch Healthy Diet index as assessed by 24 h recalls and FFQ: associations with biomarkers from a cross-sectional study. J Nutr Sci 2013; 2: e40.
van Lee L, Geelen A, van Huysduynen EJ, de Vries JH, van't Veer P, Feskens EJ . The Dutch Healthy Diet index (DHD-index): an instrument to measure adherence to the Dutch Guidelines for a Healthy Diet. Nutr J 2012; 11: 49.
Health Council of the Netherlands, Guidelines for a healthy diet 2006. 2006, Health Council of the Netherlands: The Hague.
Wendel-Vos GCW, Schuit AJ, Saris WH, Kromhout D . Reproducibility and relative validity of the short questionnaire to assess health-enhancing physical activity. J Clin Nutr 2003; 56: 1163–1169.
Greenland S, Pearl J, Robins JM . Causal diagrams for epidemiologic research. Epidemiology 1999; 10: 37–48.
CBS. Statistics Netherlands. 2014 [accessed at November 2015]; Available from http://www.cbs.nl/en-GB/menu/home/default.htm.
van Lee L, Geelen A, Kiefte-de Jong JC, Witteman JC, Hofman A, Vonk N et al. Adherence to the Dutch dietary guidelines is inversely associated with 20-year mortality in a large prospective cohort study. Eur J Clin Nutr 2016; 70: 262–268.
Tumin R, Anderson SE . The epidemiology of family meals among Ohio’s adults. Public Health Nutr 2015; 18: 1474–1481.
Larson N, Fulkerson J, Story M, Neumark-Sztainer D . Shared meals among young adults are associated with better diet quality and predicted by family meal patterns during adolescence. Public Health Nutr 2013; 16: 883–893.
Shahar D, Shai I, Vardi H, Fraser D . Dietary intake and eating patterns of elderly people in Israel: who is at nutritional risk? Eur J Clin Nutr 2003; 57: 18–25.
Eagly AH . Sex differences in influenceability. Psychol Bull 1978; 85: 86–116.
Beagan BL, Chapman GE . Family influences on food choice: context of surviving breast cancer. J Nutr Educ Behav 2004; 36: 320–326.
Reimer K, Smith C, Reicks M, Henry H, Thomas R, Atwell J . Child-feeding strategies of African American women according to stage of change for fruit and vegetable consumption. Public Health Nutr 2004; 7: 505–512.
Inglis V, Ball K, Crawford D . Why do women of low socioeconomic status have poorer dietary behaviours than women of higher socioeconomic status? A qualitative exploration. Appetite 2005; 45: 334–343.
de Castro JM . When, how much and what foods are eaten are related to total daily food intake. Br J Nutr 2009; 102: 1228–1237.
Mancino L, Todd J, Lin B-H . Separating what we eat from where: measuring the effect of food away from home on diet quality. Food Policy 2009; 34: 557–562.
Illner A-K, Freisling H, Boeing H, Huybrechts I, Crispim SP, Slimani N . Review and evaluation of innovative technologies for measuring diet in nutritional epidemiology. Int J Epidemiol 2012; 41: 1187–1203.
Touvier M, Kesse-Guyot E, Méjean C, Pollet C, Malon A, Castetbon K et al. Comparison between an interactive web-based self-administered 24 h dietary record and an interview by a dietitian for large-scale epidemiological studies. Br J Nutr 2011; 105: 1055–1064.
Kirkpatrick SI, Subar AF, Douglass D, Zimmerman TP, Thompson FE, Kahle LL et al. Performance of the automated self-administered 24-hour recall relative to a measure of true intakes and to an interviewer-administered 24-h recall. Am J Clin Nutr 2014; 100: 233–240.
Acknowledgements
The work was supported by ZonMw (Grant Number 115100007), The Netherlands Organization for Health Research and Development, The Hague. The NQplus study was funded by ZonMw (Grant Number 91110030) and Wageningen University. The sponsors had no role in study design, data collection, analysis and interpretation of the data and writing of the report.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
van Lee, L., Geelen, A., Hooft van Huysduynen, E. et al. Associations between company at dinner and daily diet quality in Dutch men and women from the NQplus study. Eur J Clin Nutr 70, 1368–1373 (2016). https://doi.org/10.1038/ejcn.2016.123
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2016.123