Abstract
Background/Objectives:
Although fish consumption may have an influence on specific mortality of major chronic diseases, the relationship between fish consumption and all-cause mortality remains inconsistent.
Subjects/Methods:
We performed a systematic search of publications using PubMed and Web of science up to 31 December 2014. Summary relative risk (RR) for the highest versus lowest category of fish consumption on risk of all-cause mortality was calculated by using a random effects model. Potential nonlinear relation was tested by modeling fish intake using restricted cubic splines with three knots at fixed percentiles of the distribution.
Results:
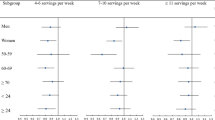
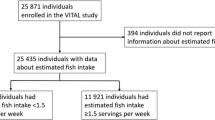
Twelve prospective cohort studies with 672 389 participants and 57 641 deaths were included in this meta-analysis. Compared with the lowest category, the highest category of fish intake was associated with about a 6% significantly lower risk of all-cause mortality (RR=0.94, 95% confidence interval (CI): 0.90, 0.98; I2=39.1%, P=0.06). The dose–response analysis indicated a nonlinear relationship between fish consumption and all-cause mortality. Compared with never consumers, consumption of 60 g of fish per day was associated with a 12% reduction (RR=0.88, 95% CI: 0.83, 0.93) in risk of total death.
Conclusions:
These results imply that fish consumption was associated with a reduced risk of all-cause mortality.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Ezzati M, Riboli E . Can noncommunicable diseases be prevented? Lessons from studies of populations and individuals. Science 2012; 337: 1482–1487.
Mozaffarian D, Appel LJ, Van Horn L . Components of a cardioprotective diet: new insights. Circulation 2011; 123: 2870–2891.
Li YH, Zhou CH, Pei HJ, Zhou XL, Li LH, Wu YJ et al. Fish consumption and incidence of heart failure: a meta-analysis of prospective cohort studies. Chin Med J (Engl) 2013; 126: 942–948.
Konig A, Bouzan C, Cohen JT, Connor WE, Kris-Etherton PM, Gray GM et al. A quantitative analysis of fish consumption and coronary heart disease mortality. Am J Prev Med 2005; 29: 335–346.
Whelton SP, He J, Whelton PK, Muntner P . Meta-analysis of observational studies on fish intake and coronary heart disease. Am J Cardiol 2004; 93: 1119–1123.
Larsson SC, Orsini N . Fish consumption and the risk of stroke: a dose-response meta-analysis. Stroke 2011; 42: 3621–3623.
Zhang M, Picard-Deland E, Marette A . Fish and marine omega-3 polyunsatured fatty acid consumption and incidence of type 2 diabetes: a systematic review and meta-analysis. Int J Endocrinol 2013; 2013: 501015.
Song J, Su H, Wang BL, Zhou YY, Guo LL . Fish consumption and lung cancer risk: systematic review and meta-analysis. Nutr Cancer 2014; 66: 539–549.
Luo J, Yang Y, Liu J, Lu K, Tang Z, Liu P et al. Systematic review with meta-analysis: meat consumption and the risk of hepatocellular carcinoma. Aliment Pharmacol Ther 2014; 39: 913–922.
Salehi M, Moradi-Lakeh M, Salehi MH, Nojomi M, Kolahdooz F . Meat, fish, and esophageal cancer risk: a systematic review and dose-response meta-analysis. Nutr Rev 2013; 71: 257–267.
Wu S, Feng B, Li K, Zhu X, Liang S, Liu X et al. Fish consumption and colorectal cancer risk in humans: a systematic review and meta-analysis. Am J Med 2012; 125: 551–559.
Kolahdooz F, van der Pols JC, Bain CJ, Marks GC, Hughes MC, Whiteman DC et al. Meat, fish, and ovarian cancer risk: results from 2 Australian case-control studies, a systematic review, and meta-analysis. Am J Clin Nutr 2010; 91: 1752–1763.
Lee JE, McLerran DF, Rolland B, Chen Y, Grant EJ, Vedanthan R et al. Meat intake and cause-specific mortality: a pooled analysis of asian prospective cohort studies. Am J Clin Nutr 2013; 98: 1032–1041.
Zheng J, Huang T, Yu Y, Hu X, Yang B, Li D . Fish consumption and CHD mortality: an updated meta-analysis of seventeen cohort studies. Public Health Nutr 2012; 15: 725–737.
Bell GA, Kantor ED, Lampe JW, Kristal AR, Heckbert SR, White E . Intake of long-chain omega-3 fatty acids from diet and supplements in relation to mortality. Am J Epidemiol 2014; 179: 710–720.
Chapkin RS, Davidson LA, Ly L, Weeks BR, Lupton JR, McMurray DN . Immunomodulatory effects of (n-3) fatty acids: Putative link to inflammation and colon cancer. J Nutr 2007; 137: 200S–204S.
Saravanan P, Davidson NC, Schmidt EB, Calder PC . Cardiovascular effects of marine omega-3 fatty acids. Lancet 2010; 376: 540–550.
Nanri A, Mizoue T, Noda M, Takahashi Y, Matsushita Y, Poudel-Tandukar K et al. Fish intake and type 2 diabetes in Japanese men and women: The Japan Public Health Center-based Prospective Study. Am J Clin Nutr 2011; 94: 884–891.
Kappeler R, Eichholzer M, Rohrmann S . Meat consumption and diet quality and mortality in NHANES III. Eur J Clin Nutr 2013; 67: 598–606.
Takata Y, Zhang X, Li H, Gao YT, Yang G, Gao J et al. Fish intake and risks of total and cause-specific mortality in 2 population-based cohort studies of 134,296 men and women. Am J Epidemiol 2013; 178: 46–57.
Olsen A, Egeberg R, Halkjaer J, Christensen J, Overvad K, Tjonneland A . Healthy aspects of the Nordic diet are related to lower total mortality. J Nutr 2011; 141: 639–644.
Yamagishi K, Iso H, Date C, Fukui M, Wakai K, Kikuchi S et al. Fish, omega-3 polyunsaturated fatty acids, and mortality from cardiovascular diseases in a nationwide community-based cohort of Japanese men and women the JACC (Japan collaborative cohort study for evaluation of cancer risk) study. J Am Coll Cardiol 2008; 52: 988–996.
Ness AR, Maynard M, Frankel S, Smith GD, Frobisher C, Leary SD et al. Diet in childhood and adult cardiovascular and all cause mortality: the boyd orr cohort. Heart 2005; 91: 894–898.
Folsom AR, Demissie Z . Fish intake, marine omega-3 fatty acids, and mortality in a cohort of postmenopausal women. Am J Epidemiol 2004; 160: 1005–1010.
Nagata C, Takatsuka N, Shimizu H . Soy and fish oil intake and mortality in a japanese community. Am J Epidemiol 2002; 156: 824–831.
Gillum RF, Mussolino M, Madans JH . The relation between fish consumption, death from all causes, and incidence of coronary heart disease. The NHANES i epidemiologic follow-up study. J Clin Epidemiol 2000; 53: 237–244.
Albert CM, Hennekens CH, O'Donnell CJ, Ajani UA, Carey VJ, Willett WC et al. Fish consumption and risk of sudden cardiac death. JAMA 1998; 279: 23–28.
Daviglus ML, Stamler J, Orencia AJ, Dyer AR, Liu K, Greenland P et al. Fish consumption and the 30-year risk of fatal myocardial infarction. N Engl J Med 1997; 336: 1046–1053.
Schisterman EF, Cole SR, Platt RW . Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology 2009; 20: 488–495.
Aune D, Greenwood DC, Chan DSM, Vieira R, Vieira AR, Navarro Rosenblatt DA et al. Body mass index, abdominal fatness and pancreatic cancer risk: a systematic review and non-linear dose-response meta-analysis of prospective studies. Ann Oncol 2012; 23: 843–852.
DerSimonian R, Laird N . Meta-analysis in clinical trials. Control Clin Trials 1986; 7: 177–188.
Jackson D, White IR, Thompson SG . Extending DerSimonian and Laird's methodology to perform multivariate random effects meta‐analyses. Stat Med 2010; 29: 1282–1297.
Greenland S, Longnecker MP . Methods for trend estimation from summarized dose-response data, with applications to meta-analysis. Am J Epidemiol 1992; 135: 1301–1309.
Orsini N, Bellocco R, Greenland S . Generalized least squares for trend estimation of summarized dose-response data. Stata Journal 2006; 6: 40–57.
Liu Q, Cook NR, Bergstrom A, Hsieh C . A two-stage hierarchical regression model for meta-analysis of epidemiologic nonlinear dose-response data. Comput Stat Data Anal 2009; 53: 4157–4167.
Orsini N, Li R, Wolk A, Khudyakov P, Spiegelman D . Meta-analysis for linear and nonlinear dose-response relations: examples, an evaluation of approximations, and software. Am J Epidemiol 2012; 175: 66–73.
Higgins JP, Thompson SG, Deeks JJ, Altman DG . Measuring inconsistency in meta-analyses. BMJ 2003; 327: 557–560.
Egger M, Davey SG, Schneider M, Minder C . Bias in meta-analysis detected by a simple, graphical test. BMJ 1997; 315: 629–634.
Begg CB, Mazumdar M . Operating characteristics of a rank correlation test for publication bias. Biometrics 1994; 50: 1088–1101.
Caygill CP, Hill MJ . Fish n-3 fatty acids and human colorectal and breast cancer mortality. Eur J Cancer Prev 1995; 4: 329–332.
Zhang J, Temme EH, Kesteloot H . Fish consumption is inversely associated with male lung cancer mortality in countries with high levels of cigarette smoking or animal fat consumption. Int J Epidemiol 2000; 29: 615–621.
Szymanski KM, Wheeler DC, Mucci LA . Fish consumption and prostate cancer risk: a review and meta-analysis. Am J Clin Nutr 2010; 92: 1223–1233.
Mozaffarian D, Rimm EB . Fish intake, contaminants, and human health: Evaluating the risks and the benefits. JAMA 2006; 296: 1885–1899.
Tavani A, Pelucchi C, Parpinel M, Negri E, Franceschi S, Levi F et al. N-3 polyunsaturated fatty acid intake and cancer risk in Italy and Switzerland. Int J Cancer 2003; 105: 113–116.
Pilz S, Tomaschitz A, Drechsler C, Zittermann A, Dekker JM, Marz W . Vitamin D supplementation: a promising approach for the prevention and treatment of strokes. Curr Drug Targets 2011; 12: 88–96.
He K, Merchant A, Rimm EB, Rosner BA, Stampfer MJ, Willett WC et al. Folate, vitamin B-6, and B-12 intakes in relation to risk of stroke among men. Stroke 2004; 35: 169–174.
Militante JD, Lombardini JB . Treatment of hypertension with oral taurine: experimental and clinical studies. Amino Acids 2002; 23: 381–393.
Moncada S, Higgs A . The L-arginine-nitric oxide pathway. N Engl J Med 1993; 329: 2002–2012.
D'Elia L, Barba G, Cappuccio FP, Strazzullo P . Potassium intake, stroke, and cardiovascular disease a meta-analysis of prospective studies. J Am Coll Cardiol 2011; 57: 1210–1219.
Hoption CS . Hypothesis: dietary iodine intake in the etiology of cardiovascular disease. J Am Coll Nutr 2006; 25: 1–11.
He K, Rimm EB, Merchant A, Rosner BA, Stampfer MJ, Willett WC et al. Fish consumption and risk of stroke in men. JAMA 2002; 288: 3130–3136.
Hu FB, Bronner L, Willett WC, Stampfer MJ, Rexrode KM, Albert CM et al. Fish and omega-3 fatty acid intake and risk of coronary heart disease in women. JAMA 2002; 287: 1815–1821.
Engeset D, Braaten T, Teucher B, Kühn T, Bueno-de-Mesquita HB, Leenders M et al. Fish consumption and mortality in the European Prospective Investigation into Cancer and Nutrition cohort. Eur J Epidemiol 2014; 30: 57–70.
Osler M, Andreasen AH, Hoidrup S . No inverse association between fish consumption and risk of death from all-causes, and incidence of coronary heart disease in middle-aged, Danish adults. J Clin Epidemiol 2003; 56: 274–279.
Nakamura Y, Ueshima H, Okamura T, Kadowaki T, Hayakawa T, Kita Y et al. Association between fish consumption and all-cause and cause-specific mortality in Japan: NIPPON DATA80, 1980-99. Am J Med 2005; 118: 239–245.
Egger M, Schneider M, Davey SG . Spurious precision? Meta-analysis of observational studies. BMJ 1998; 316: 140–144.
Weiss NS . All-cause mortality as an outcome in epidemiologic studies: proceed with caution. Eur J Epidemiol 2014; 29: 147–149.
Acknowledgements
We thank the original studies for the contribution to conduct our meta-analysis. This study was supported by the fund of Shanghai Health Bureau Key Disciplines and Specialties Foundation. Y-BX obtained the funding, conducted the research design and also had primary responsibility for the final content; L-GZ, J-WS and YY analyzed the data and interpreted the results; L-GZ drafted first manuscript; all authors critically reviewed and approved the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhao, LG., Sun, JW., Yang, Y. et al. Fish consumption and all-cause mortality: a meta-analysis of cohort studies. Eur J Clin Nutr 70, 155–161 (2016). https://doi.org/10.1038/ejcn.2015.72
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.72
This article is cited by
-
Trends in energy and macronutrient intake among Taiwanese older adults in 1999–2000, 2005–2008 and 2013–2016 periods
BMC Public Health (2023)
-
Association of oily fish and nonoily fish intakes with all-cause mortality and cause-specific mortality: a large population-based prospective study
Journal of Translational Medicine (2023)
-
Dietary protein intake and all-cause mortality: results from The Kawasaki Aging and Wellbeing Project
BMC Geriatrics (2023)
-
Animal foods and mobility limitations in community-dwelling young-old adults: longitudinal analysis of the EpiDoC cohort
BMC Geriatrics (2022)
-
Impact of fish consumption on all-cause mortality in older people with and without dementia: a community-based cohort study
European Journal of Nutrition (2022)