Abstract
Background/Objectives:
Low blood levels of 25-hydroxyvitamin D (25OHD) have been associated with cardiometabolic disease but results are inconsistent. The objective of the study was to investigate the association of 25OHD with metabolic syndrome in a population at increased risk for diabetes.
Subjects/Methods:
Using baseline data from the placebo and lifestyle intervention arms of the Diabetes Prevention Program (N=2000), multivariable logistic regression models were used to estimate the odds of prevalent metabolic syndrome and each of its individual components across 25OHD tertiles. Multivariable linear regression was used to estimate the adjusted mean difference of insulin secretion and sensitivity across the same 25OHD tertiles. In participants free of metabolic syndrome at baseline (N=546), incident metabolic syndrome in the first 2 years of follow-up was assessed using discrete-time proportional hazards regression to test its association with 25OHD concentration.
Results:
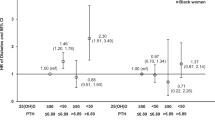
After multivariate adjustment, participants in the highest tertile of 25OHD had lower odds of prevalent metabolic syndrome (odds ratio=0.62; 95% confidence interval (CI)=0.45–0.84), smaller waist circumference, higher high-density lipoprotein and lower fasting plasma glucose compared with participants in the lowest tertile of 25OHD. Higher plasma 25OHD concentration was associated with greater insulin sensitivity and lower insulin secretion. After multivariate adjustment, there was a nonsignificant lower risk of metabolic syndrome in the highest tertile of 25OHD (hazard ratio=0.79; 95% CI=0.48–1.32) compared with the lowest tertile.
Conclusions:
In a population at increased risk for diabetes, higher plasma 25OHD concentration was inversely associated with prevalent metabolic syndrome and nonsignificantly with incident metabolic syndrome.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Dobnig H, Pilz S, Scharnagl H, Renner W, Seelhorst U, Wellnitz B et al. Independent association of low serum 25-hydroxyvitamin d and 1,25-dihydroxyvitamin d levels with all-cause and cardiovascular mortality. Arch Intern Med 2008; 168: 1340–1349.
Wang TJ, Pencina MJ, Booth SL, Jacques PF, Ingelsson E, Lanier K et al. Vitamin D deficiency and risk of cardiovascular disease. Circulation 2008; 117: 503–511.
Lu L, Yu Z, Pan A, Hu FB, Franco OH, Li H et al. Plasma 25-hydroxyvitamin D concentration and metabolic syndrome among middle-aged and elderly Chinese individuals. Diabetes Care 2009; 32: 1278–1283.
Beydoun MA, Boueiz A, Shroff MR, Beydoun HA, Wang Y, Zonderman AB . Associations among 25-hydroxyvitamin D, diet quality, and metabolic disturbance differ by adiposity in adults in the United States. J Clin Endocrinol Metab 2010; 95: 3814–3827.
Kayaniyil S, Vieth R, Harris SB, Retnakaran R, Knight JA, Gerstein HC et al. Association of 25(OH)D and PTH with metabolic syndrome and its traditional and nontraditional components. J Clin Endocrinol Metab 2011; 96: 168–175.
Ganji V, Zhang X, Shaikh N, Tangpricha V . Serum 25-hydroxyvitamin D concentrations are associated with prevalence of metabolic syndrome and various cardiometabolic risk factors in US children and adolescents based on assay-adjusted serum 25-hydroxyvitamin D data from NHANES 2001-2006. Am J Clin Nutr 2011; 94: 225–233.
Lee DM, Rutter MK, O'Neill TW, Boonen S, Vanderschueren D, Bouillon R et al. Vitamin D, parathyroid hormone and the metabolic syndrome in middle-aged and older European men. Eur J Endocrinol 2009; 161: 947–954.
He JL, Scragg RK . Vitamin D, parathyroid hormone, and blood pressure in the National Health and Nutrition Examination Surveys. Am J Hypertens 2011; 24: 911–917.
Ford ES, Ajani UA, McGuire LC, Liu S . Concentrations of serum vitamin D and the metabolic syndrome among U.S. adults. Diabetes Care 2005; 28: 1228–1230.
Botella-Carretero JI, Alvarez-Blasco F, Villafruela JJ, Balsa JA, Vazquez C, Escobar-Morreale HF . Vitamin D deficiency is associated with the metabolic syndrome in morbid obesity. Clin Nutr 2007; 26: 573–580.
Hypponen E, Boucher BJ, Berry DJ, Power C . 25-Hydroxyvitamin D, IGF-1, and metabolic syndrome at 45 years of age: a cross-sectional study in the 1958 British Birth Cohort. Diabetes 2008; 57: 298–305.
Reis JP, von Muhlen D, Kritz-Silverstein D, Wingard DL, Barrett-Connor E . Vitamin D, parathyroid hormone levels, and the prevalence of metabolic syndrome in community-dwelling older adults. Diabetes Care 2007; 30: 1549–1555.
Hjelmesaeth J, Hofso D, Aasheim ET, Jenssen T, Moan J, Hager H et al. Parathyroid hormone, but not vitamin D, is associated with the metabolic syndrome in morbidly obese women and men: a cross-sectional study. Cardiovasc Diabetol 2009; 8: 7.
McGill AT, Stewart JM, Lithander FE, Strik CM, Poppitt SD . Relationships of low serum vitamin D3 with anthropometry and markers of the metabolic syndrome and diabetes in overweight and obesity. Nutr J 2008; 7: 4.
Rueda S, Fernandez-Fernandez C, Romero F, Martinez de Osaba J, Vidal J . Vitamin D, PTH, and the metabolic syndrome in severely obese subjects. Obes Surg 2008; 18: 151–154.
Bell NH, Greene A, Epstein S, Oexmann MJ, Shaw S, Shary J . Evidence for alteration of the vitamin D-endocrine system in blacks. J Clin Invest 1985; 76: 470–473.
The Diabetes Prevention Program. Design and methods for a clinical trial in the prevention of type 2 diabetes. Diabetes Care 1999; 22: 623–634.
Hankinson SE, London SJ, Chute CG, Barbieri RL, Jones L, Kaplan LA et al. Effect of transport conditions on the stability of biochemical markers in blood. Clin Chem 1989; 35: 2313–2316.
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA et al. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation 2005; 112: 2735–2752.
Phillips DI, Clark PM, Hales CN, Osmond C . Understanding oral glucose tolerance: comparison of glucose or insulin measurements during the oral glucose tolerance test with specific measurements of insulin resistance and insulin secretion. Diabet Med 1994; 11: 286–292.
Hanson RL, Pratley RE, Bogardus C, Narayan KM, Roumain JM, Imperatore G et al. Evaluation of simple indices of insulin sensitivity and insulin secretion for use in epidemiologic studies. Am J Epidemiol 2000; 151: 190–198.
Kitabchi AE, Temprosa M, Knowler WC, Kahn SE, Fowler SE, Haffner SM et al. Role of insulin secretion and sensitivity in the evolution of type 2 diabetes in the diabetes prevention program: effects of lifestyle intervention and metformin. Diabetes 2005; 54: 2404–2414.
Utzschneider KM, Prigeon RL, Faulenbach MV, Tong J, Carr DB, Boyko EJ et al. Oral disposition index predicts the development of future diabetes above and beyond fasting and 2-h glucose levels. Diabetes Care 2009; 32: 335–341.
Kriska AM, Caspersen CJ . Introduction to a collection of physical activity questionnaires. Med Sci Sports Exerc 1997; 29 (Suppl), S5–S9.
Mayer-Davis EJ, Sparks KC, Hirst K, Costacou T, Lovejoy JC, Regensteiner JG et al. Dietary intake in the diabetes prevention program cohort: baseline and 1-year post randomization. Ann Epidemiol 2004; 14: 763–772.
Orchard TJ, Temprosa M, Goldberg R, Haffner S, Ratner R, Marcovina S et al. The effect of metformin and intensive lifestyle intervention on the metabolic syndrome: the Diabetes Prevention Program randomized trial. Ann Int Med 2005; 142: 611–619.
Eckel RH, Grundy SM, Zimmet PZ . The metabolic syndrome. Lancet 2005; 365: 1415–1428.
Maestro B, Molero S, Bajo S, Davila N, Calle C . Transcriptional activation of the human insulin receptor gene by 1,25-dihydroxyvitamin D(3). Cell Biochem Funct 2002; 20: 227–232.
Dunlop TW, Vaisanen S, Frank C, Molnar F, Sinkkonen L, Carlberg C . The human peroxisome proliferator-activated receptor delta gene is a primary target of 1alpha,25-dihydroxyvitamin D3 and its nuclear receptor. J Mol Biol 2005; 349: 248–260.
Kadowaki S, Norman AW . Dietary vitamin D is essential for normal insulin secretion from the perfused rat pancreas. J Clin Invest 1984; 73: 759–766.
Tanaka Y, Seino Y, Ishida M, Yamaoka K, Yabuuchi H, Ishida H et al. Effect of vitamin D3 on the pancreatic secretion of insulin and somatostatin. Acta Endocrinol (Copenh) 1984; 105: 528–533.
Cade C, Norman AW . Vitamin D3 improves impaired glucose tolerance and insulin secretion in the vitamin D-deficient rat in vivo. Endocrinology 1986; 119: 84–90.
Johnson JA, Grande JP, Roche PC, Kumar R . Immunohistochemical localization of the 1,25(OH)2D3 receptor and calbindin D28k in human and rat pancreas. Am J Physiol 1994; 267 (3 Pt 1), E356–E360.
Bland R, Markovic D, Hills CE, Hughes SV, Chan SL, Squires PE et al. Expression of 25-hydroxyvitamin D3-1alpha-hydroxylase in pancreatic islets. J Steroid Biochem Mol Biol 2004; 89-90: 121–125.
Sergeev IN, Rhoten WB . 1,25-Dihydroxyvitamin D3 evokes oscillations of intracellular calcium in a pancreatic beta-cell line. Endocrinology 1995; 136: 2852–2861.
Reis JP, von Muhlen D, Miller 3rd ER . Relation of 25-hydroxyvitamin D and parathyroid hormone levels with metabolic syndrome among US adults. Eur J Endocrinol 2008; 159: 41–48.
Kim MK, Il Kang M, Won OhK, Kwon HS, Lee JH, Lee WC et al. The association of serum vitamin D level with presence of metabolic syndrome and hypertension in middle-aged Korean subjects. Clin Endocrinol (Oxf) 2010; 73: 330–338.
Kayaniyil S, Vieth R, Retnakaran R, Knight JA, Qi Y, Gerstein HC et al. Association of vitamin D with insulin resistance and beta-cell dysfunction in subjects at risk for type 2 diabetes. Diabetes Care 2010; 33: 1379–1381.
Chacko SA, Song Y, Manson JE, Van Horn L, Eaton C, Martin LW et al. Serum 25-hydroxyvitamin D concentrations in relation to cardiometabolic risk factors and metabolic syndrome in postmenopausal women. Am J Clin Nutr 2011; 94: 209–217.
Forouhi NG, Luan J, Cooper A, Boucher BJ, Wareham NJ . Baseline serum 25-hydroxy vitamin d is predictive of future glycemic status and insulin resistance: the Medical Research Council Ely Prospective Study 1990-2000. Diabetes 2008; 57: 2619–2625.
Gagnon C, Lu ZX, Magliano DJ, Dunstan DW, Shaw JE, Zimmet PZ et al. Low serum 25-hydroxyvitamin D is associated with increased risk of the development of the metabolic syndrome at five years: results from a national, population-based prospective study (The Australian Diabetes, Obesity and Lifestyle Study: AusDiab). J Clin Endocrinol Metab 2012; 97: 1953–1961.
Harris SS . Does vitamin D deficiency contribute to increased rates of cardiovascular disease and type 2 diabetes in African Americans? Am J Clin Nutr 2011; 93: 1175S–1178SS.
Liu E, Meigs JB, Pittas AG, McKeown NM, Economos CD, Booth SL et al. Plasma 25-hydroxyvitamin d is associated with markers of the insulin resistant phenotype in nondiabetic adults. J Nutr 2009; 139: 329–334.
Scragg R, Sowers M, Bell C . Serum 25-hydroxyvitamin D, diabetes, and ethnicity in the Third National Health and Nutrition Examination Survey. Diabetes Care 2004; 27: 2813–2818.
Pinelli NR, Jaber LA, Brown MB, Herman WH . Serum 25-hydroxy vitamin d and insulin resistance, metabolic syndrome, and glucose intolerance among Arab Americans. Diabetes Care 2010; 33: 1373–1375.
Gulseth HL, Gjelstad IM, Tierney AC, Lovegrove JA, Defoort C, Blaak EE et al. Serum vitamin D concentration does not predict insulin action or secretion in European subjects with the metabolic syndrome. Diabetes Care 2010; 33: 923–925.
Pittas AG, Nelson J, Mitri J, Hillmann W, Garganta C, Nathan DM et al. Plasma 25-hydroxyvitamin D and progression to diabetes in patients at risk for diabetes: an ancillary analysis in the Diabetes Prevention Program. Diabetes Care 2012; 35: 565–573.
Shoben AB, Kestenbaum B, Levin G, Hoofnagle AN, Psaty BM, Siscovick DS et al. Seasonal variation in 25-hydroxyvitamin d concentrations in the cardiovascular health study. Am J Epidemiol 2011; 174: 1363–1372.
Acknowledgements
We thank David Kent, MD MSc, Associate Professor of Medicine, Director of the Clinical and Translational Science MS/PhD Program at the Sackler School, for his valuable input into interpretation of the results. We also acknowledge the commitment and dedication of the DPP participants. A portion of the work was presented at the 2012 Endocrine Society meeting as an oral presentation, on 23 June 2012, in Houston, TX. This study was supported by research grants R01DK79003, U34DK091958 and U01DK098245 (to AGP) from the National Institute of Diabetes and Digestive and Kidney Disease, the Office Of The Director—National Institutes of Health, and the National Institutes of Health Office of Dietary Supplements; UL1RR025752 (to Tufts University) from the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health. The US Department of Agriculture Agreement 58-1950-9001 (to BDH); the Marilyn Fishman Grant for Diabetes Research (to JM) from the Endocrine Fellows Foundation; U01DK48489 from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) of the National Institutes of Health to the DPP clinical centers and the Coordinating Center for the design and conduct of the DPP study. The Southwestern American Indian Centers were supported directly by the NIDDK, including its Intramural Research Program, and the Indian Health Service. The General Clinical Research Center Program, National Center for Research Resources, supported data collection at many of the clinical centers. Funding was also provided by the National Institute of Child Health and Human Development, the National Institute on Aging, the National Eye Institute, the National Heart Lung and Blood Institute, the Office of Research on Women’s Health, the National Center for Minority Health and Human Disease, the Centers for Disease Control and Prevention, the Indian Health Service, and the American Diabetes Association. Lipha (Merck-Sante) provided medication. LifeScan Inc., Merck-Medco Managed Care, Inc., and Merck and Co. donated materials, equipment or medicines for concomitant conditions. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH or the above listed institutions.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Mitri, J., Nelson, J., Ruthazer, R. et al. Plasma 25-hydroxyvitamin D and risk of metabolic syndrome: an ancillary analysis in the Diabetes Prevention Program. Eur J Clin Nutr 68, 376–383 (2014). https://doi.org/10.1038/ejcn.2013.293
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2013.293
Keywords
This article is cited by
-
Vitamin D deficiency is associated with risk of developing peripheral arterial disease in type 2 diabetic patients
BMC Cardiovascular Disorders (2019)