Abstract
Background/objectives:
Household-level food spending data are not suitable for population-based studies of the economics of nutrition. This study compared three methods of deriving diet cost at the individual level.
Subjects/methods:
Adult men and women (n=164) completed 4-day diet diaries and a food frequency questionnaire (FFQ). Food expenditures over 4 weeks and supermarket prices for 384 foods were obtained. Diet costs (US$/day) were estimated using: (1) diet diaries and expenditures; (2) diet diaries and supermarket prices; and (3) FFQs and supermarket prices. Agreement between the three methods was assessed on the basis of Pearson correlations and limits of agreement. Income-related differences in diet costs were estimated using general linear models.
Results:
Diet diaries yielded mean (s.d.) diet costs of $10.04 (4.27) based on Method 1 and $8.28 (2.32) based on Method 2. FFQs yielded mean diet costs of $7.66 (2.72) based on Method 3. Correlations between energy intakes and costs were highest for Method 3 (r2=0.66), lower for Method 2 (r2=0.24) and lowest for Method 1 (r2=0.06). Cost estimates were significantly associated with household incomes.
Conclusion:
The weak association between food expenditures and food intake using Method 1 makes it least suitable for diet and health research. However, merging supermarket food prices with standard dietary assessment tools can provide estimates of individual diet cost that are more closely associated with food consumed. The derivation of individual diet cost can provide insights into some of the economic determinants of food choice, diet quality and health.
Similar content being viewed by others
Introduction
The cost of a nutritious diet is an important and complex issue for public health.1, 2, 3 Real or perceived inability to afford healthful foods can be a barrier to dietary change.4, 5, 6 Lower-cost foods tend to be energy-dense but nutrient-poor.7, 8 Such foods are often consumed by groups of lower socioeconomic status (SES) who are also more likely to be obese.9, 10
Epidemiologic analyses have drawn a direct link between measures of diet quality and estimated diet cost.11, 12, 13, 14 However, studies on nutrition economics have been hampered by the lack of appropriate methods and tools.15 Studies on food purchases have typically dealt with food expenditures at the household level5, 10, 16 and could not provide individual estimates of food consumed. Although such data can be used to impute individual food expenditures, by dividing by the number of household members, they may be problematic if applied to individual level studies on diets and health. By contrast, most studies on diet and chronic diseases, always conducted at the individual level, provided no data on the cost of foods consumed.
Individual-level diet costs have been estimated by linking dietary intake data from 24 h recalls or diet diaries to national or local food prices.17, 18, 19 More typically, diet costs are estimated by linking prices to diet history or food frequency questionnaires (FFQs). Following this approach, studies conducted in Europe,12, 14, 20 the USA11, 21, 22 and Japan13, 23, 24 have produced diet cost estimates based on fixed tables of food prices containing 57–384 foods. However, costs estimated from FFQs might not be directly comparable to those obtained with diet diaries. Furthermore, costs estimated using prevailing supermarket price data might not reflect the individual’s own food expenditures.
This study compared three different methods of estimating individual-level diet costs that were derived from: (1) 4-day diet diaries and individual food expenditures; (2) diet diaries and supermarket prices; and (3) FFQ data and supermarket prices. The three diet cost data sets were compared to each other, to estimated energy intakes and to self-reported household incomes.
Materials and methods
Study sample
The study was based on a stratified sample of faculty and staff of a large public university in Washington state, USA.22 Eligible respondents were aged 25–65 years and had the primary or shared responsibility for food purchasing and preparation and not on a medically prescribed diet. Data were collected between June 2005 and September 2006. All study procedures were reviewed and approved by the university's institutional review board.
Recruitment and study procedures
As described previously,22 a total of 3000 recruitment letters were sent to potential participants by campus mail. Because the 3000 invitations mailed out were based solely on salary strata from the university payroll office, an unknown fraction of the 3000 invitations were sent to individuals who may not have been eligible because of our three inclusion criteria. Out of 350 who responded positively to the letter, 91 were ineligible on account of at least one of the inclusion criteria. The 259 eligible respondents enrolled and 185 completed the 4-week study.
During the initial visit, participants completed the FFQ and were instructed in the keeping of diet diaries and recording food spending. Participants recorded food expenditures and kept receipts for all foods purchased for home consumption in grocery stores during all 4 weeks. During weeks 3 and 4, receipts for ‘away-from-home’ foods, including foods from restaurants, take-out and delivery were also saved. Diet diaries and food expenditures were reviewed by a registered dietitian upon study completion and participants were compensated for their participation.
Dietary intake assessment
4-Day diet diaries
Diet diaries were completed on 4 nonconsecutive days (including one weekend day) during week 4. For each food item consumed, participants indicated place purchased, details (including brand name, cooking methods, package size or quantity) and amount consumed. Diet diaries were entered, coded and analyzed for energy and nutrient values using Food Processor 8.1 (ESHA Research, Salem, OR, USA).
Food frequency questionnaire
All participants completed a semi-quantitative 152-item FFQ developed by the Fred Hutchinson Cancer Research Center (FHCRC) and used in prior studies on diet and health.25, 26 The reference period for reporting was the previous 12 months. Completed and reviewed FFQs were analyzed using the FHCRC Nutrition Assessment Shared Resource using the Minnesota database.26
Assessing diet costs
The mean daily diet cost (US$) was derived for each participant using the three methods described below.
Method 1: diet diaries and food expenditures
All foods and beverages reported in each participant’s coded 4-day diet diary were linked to corresponding items in the participant’s receipts, collected during weeks 1–4 of the study. To compute the expenditure for each food portion of food or beverage consumed, the gram weight consumed was multiplied by the ratio of the purchase price over total grams purchased, correcting for edible portion (EP):

For example, the expenditure associated with a 1 cup portion (109 g) of fresh apple that was purchased for $1.49/pound (454 g) was 109 g × $1.99/(454 g × 0.90)=$0.531. Overall, approximately 80% of all foods and beverages consumed were accounted for in the participants’ receipts. For missing receipt data, expenditures were imputed using food prices collected by study staff. The posted price was recorded for the product and matched for details provided by the participant. The key details were product brand, type, package size and the retail outlet from which it was purchased. When product or retail outlet information was not available, the closest match was identified from among three major supermarket chains (described below) and the lowest price was recorded. Expenditures were calculated for each day and were averaged over the 4 days.
Method 2: diet diaries and supermarket prices
Each item in the coded 4-day diet diary was matched with one of the foods in the database of supermarket prices for 384 foods and beverages in 152 categories. The database has been described before and contains lowest, non-sale prices collected from three major supermarket chains in the region as described previously.22, 27 In brief, prices were collected from May to July 2006 from Safeway, Albertson’s and Quality Food Centers (a subsidiary of Kroger), which were selected because of their large market share in the region. Prices were obtained during in-store visits and from supermarket home shopping websites (Safeway and Albertson’s), which reported to list the same prices as those available to in-store customers. When no exact match from the 384 products was available, the closest match from among the broader food categories was used. As in Method 1, daily totals were computed and 4-day means were derived.
Method 3: FFQ data and supermarket prices
The same database of supermarket prices used in Method 2 was used to derive diet cost from the FFQ, using methods described previously.21, 22
Analytic approach
All analyses of dietary energy, nutrients and monetary cost included all reported foods and beverages, except drinking water. We used parametric statistics throughout as all diet cost estimates appeared to follow standard log-normal distributions. The Pearson product–moment correlation was used to measure the agreement between estimates of nutrient intake in Methods 1 and 3 and between all three diet cost estimates. Nutrient and diet cost variables were natural log transformed before conducting Pearson correlations. Energy adjustments were based on the method of residuals.11, 28 The association between energy intakes and estimates of diet cost was based on linear least squares regression. The agreement among all three crude (not transformed or energy-adjusted) diet cost estimates was assessed using the limits of agreement. This method provided a mean difference between values from any two methods and the range of difference values within which 95% of all differences between methods will be expected to fall.29 Estimates of diet cost across income groups were based on a general linear model to adjust for energy intake, age, sex and number of adults and children in the household. Analyses of variance were used to test for differences across groups. Four income groups were defined to keep numbers of respondents similar. All analyses were conducted using SPSS 18.0 for Mac (IBM, Chicago, IL, USA).
Results
The final analytic sample of 164 (103 women and 61 men) provided complete FFQ and diet diary data, all questionnaires and shopping and restaurant receipts over 4 weeks.
Sample characteristics
Mean age was 42.2 years for women and 38.0 years for men (range 25–65 years). Most men (92%) and most women (85%) had completed a bachelor’s degree or higher. A majority of women (60%) and half the men (51%) had annual household incomes of $55 000 and above. Most men (85%) and women (82%) identified themselves as white, with the rest being Asian or Pacific Islander and African American. Demographic and SES data are summarized in Table 1.
Estimates of energy and nutrient intakes
On the basis of diet diaries, mean (s.d.) intakes overall were 2134 (508) kcal/day (8.93 MJ), with a range of 1192–3796 kcal/day (5.0–15.9 MJ). Men consumed 2426 kcal/day (10.2 MJ) and women 1960 kcal/day (8.2 MJ). The FFQ showed a lower overall mean but more variance than the diet diary estimates. Average daily energy intake for the whole sample was 1894 (641) kcal/day (7.9 MJ) and intakes ranged from 689 to 4110 kcal/day (2.9–17.2 MJ). Men reported energy intakes of 2088 kcal/day (8.7 MJ) and women 1779 kcal/day (7.4 MJ).
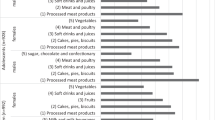
Crude nutrient intakes from the two instruments are summarized in Table 2. As with energy intake, macronutrient intakes from 4-day diet diaries were generally higher than the estimates produced by the FFQ. However, for crude micronutrient intakes, estimates from diet diaries tended to be lower than those from the FFQ. Among both macronutrients and micronutrients, the magnitude of differences in estimated mean nutrient intake between the diet diaries and FFQs varied from as low as 2% for fiber (diet diary estimate higher) to 46% for magnesium (diet diary estimate lower). Pearson correlations for energy-adjusted nutrient intake estimates from the two instruments ranged from 0.27 (vitamin B1) to 0.7 (fiber).
Estimates of crude and energy-adjusted diet costs
Mean (s.d.) diet costs based on 4-day diet diaries and food expenditures (Method 1) were $10.04 (4.27)/day (range $2.09–24.90/day). Despite the difference in estimated energy intake between the two sexes, men and women spent a similar amount of money on food per day; $9.97/day versus $10.08/day, respectively. However, on a per-2000 kcal (8.38 MJ) basis expenditures were $8.37 for men and $10.47 for women. The overall energy-adjusted diet cost was $9.70 (4.06).
The top panel in Figure 1 shows the association between diet costs estimated using Method 1 and estimates of dietary energy for all 164 participants. Diet costs based on food expenditures showed much greater inter-subject variability than did energy intakes. Although food expenditures varied by more than 10-fold, energy varied only by a factor of four. Diet cost was only weakly associated with food intake, with dietary energy accounting for 6% of the variation in food expenditure.
Scatter plots showing estimated diet cost and energy intake (1 kcal=4.18 kJ) based on three methods, n=164. Top panel, Method 1 based on 4-day diet diaries with food expenditures. Middle panel, Method 2 based on 4-day diet diaries linked to a database of supermarket prices. Bottom panel, Method 3 based on FFQ with the same food price database. Energy estimates were based on each corresponding instrument. Least squares regression indicated weakest association between cost and energy for Method 1 and strongest for Method 3.
Mean (s.d.) diet costs based on 4-day diet diaries and standard supermarket prices (Method 2) were estimated at $8.28 (2.32)/day. Relative to Method 1, the range was greatly reduced at $4.05–14.74/day. The estimated diet cost was higher for men ($8.59/day) than for women ($8.09/day) before adjusting for energy. Diet cost per 2000 kcal was $7.21 for men and $8.37 for women with an overall mean of $7.94 (2.19). Relative to Method 1, the association between diet cost and energy was stronger (r2=0.24; Figure 1, middle panel).
Mean (s.d.) diet costs based on FFQ data and standard supermarket prices (Method 3) were $7.66 (2.72) per day, ranging from $2.03 to $18.11/day. Diet cost was $8.12/day for men and 7.39/day for women. Diet cost per 2000 kcal was $7.73 for men and $8.44 for women with an overall mean of $8.19 (1.68). Figure 1 bottom panel shows that the association between diet cost and energy was robust (r2=0.66).
Agreement among estimates of diet cost
The association between diet costs estimated using Method 1 and those estimated using Method 3 was weak. Crude daily food expenditures were an average of 31% higher than diet costs estimated using Method 3. The Pearson correlation coefficient between the two crude measures was 0.21 and limits of agreement analysis indicated a mean difference of $2.37/day (Method 1 higher) with a 95% confidence interval (CI) for the difference of $1.67, $3.08. The weakness of the association was partly attributed to differences in the energy estimates from the two instruments. Adjusting for energy based on residuals yielded a Pearson correlation of 0.30. Adjusting crude diet costs on a per-8.38 MJ (2000 kcal) basis narrowed the difference in estimated diet costs to 18% and yielded a correlation of 0.33 (Table 2).
By contrast, we found higher correlations between diet costs derived using Method 1 and Method 2. Method 1 and Method 2 shared the same instrument of dietary intake assessment, but differed in the use of actual food expenditures versus supermarket prices. The mean (95% CI) difference between the crude estimates was $1.76/day ($1.21, $2.31, Method 1 higher) and the Pearson correlation coefficient for energy-adjusted estimates was 0.49. Diet costs obtained using Methods 2 and 3 were also significantly correlated. Methods 2 and 3 used different methods of dietary intake assessment, but the same price database. The mean (95% CI) difference between the crude estimates was $0.62/day ($−0.16, $1.07, Method 2 higher) and the Pearson correlation coefficient for energy-adjusted estimates was 0.39. The comparison of the resulting three estimates of diet cost and the Pearson correlation of energy-adjusted estimates is illustrated in Figure 2.
Diet cost by household income
Although all three estimates of diet cost showed positive associations with household income, an indicator of SES, the strength of the association was different for the three estimates. Figure 3 presents covariate-adjusted means and standard errors for each of the three measures of diet cost across four levels of household income. Diet cost estimates based on Method 1 showed the strongest gradient with income, with the highest income group showing a daily diet cost that was 34% higher than the daily costs for participants in the lowest income group (difference of $2.98/day, P=0.004). Method 2 showed a 16% difference between the highest and the lowest income groups ($1.24/day, P=0.015), whereas Method 3 showed a 15% difference ($1.08/day, P=0.007) between the highest and the lowest income groups.
Estimates of mean and standard errors of diet cost using three methods by income level, n=164. Sample sizes in each income level given in Table 1. Means are adjusted for age, gender, energy intake and number of adults and children residing in the household. Method 1 based on 4-day diet diaries with food expenditures. Method 2 based on 4-day diet diaries with a database of supermarket prices. Method 3 based on FFQ with the same price database. Trend tests across income levels were significant for all three diet cost measures. *P<0.05; **P<0.01; ***P<0.005.
Discussion
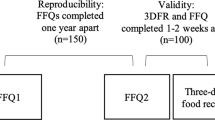
Estimates of daily diet costs at the individual level can be obtained by joining dietary intake data with prevailing food price data, from local supermarkets, or individual price data, from each participant’s own food expenditures. The present goal was to test the performance of alternative methods, following the design of previous inter-method reliability and validity studies.26, 29, 30
Comparisons were therefore conducted both across and within two dietary assessment instruments: diet diaries (Methods 1 and 2) and FFQ (Method 3). In Method 3, FFQ data were combined with area food prices, a widely used approach internationally.11, 12, 13, 14 Method 2, combining 4-day diet diaries with area food prices, was similar to the approach used in earlier studies in Japan31 and Sweden19 that linked 4-day diaries to national and local food prices. A variation of this approach has been the application of national food prices to 24-h recalls of adults18 and children17 in the USA.
Method 1, which derived expenditures for food consumed, has to our knowledge not been previously reported and might be described as closest to a ‘true’ indication of diet cost. In fact, the present estimate of $10.04 was similar to the $10.12 per capita food expenditures imputed by the US Department of Agriculture using household food expenditure data for 2006.32 However, two factors limit the usefulness of Method 1 for diet and nutrition research. First, for reasons discussed below, this diet cost estimate showed little association with the total amount of food consumed (Figure 1, top panel), which would likely attenuate any association of diet cost with diet composition. Second, estimating individual diet costs by using individual food expenditures is highly labor intensive, requiring 4–8 h to link each coded 4-day diet diary to receipt data and adjust purchased products for edible portion.
Methods 2 and 3, which applied a standard database of supermarket prices, have parallels in nutritional epidemiology, where estimates of energy and nutrient intakes for individuals are derived from common nutrient composition tables. For example, the vitamin C content of fresh, raw apples consumed by participants in the National Health and Nutrition Examination Surveys is set at 4.6 mg per 100 g edible portion,33 regardless of the vitamin C content of the apples that were actually consumed. The addition of a price variable was analogous to the inclusion of new nutrient-based variables in the FFQ nutrient database.34
All three estimates of diet cost were positively and monotonically associated with household income, consistent with past studies on incomes and household food expenditures.5, 10, 35 Diet cost estimates based on expenditures (Method 1) were not only the highest but also showed the largest differences across income strata. It is likely that diet costs estimated using a standard prices database (Methods 2 and 3) underestimate the true differences in purchasing power across income groups.
Methodological considerations and sources of bias between estimates
A number of factors may have biased the results of this methodological study. First, analyses were based on a convenience sample of mostly white adults of higher SES, that although small, was similar in size to samples used in previous reliability studies of dietary assessment.26, 29, 30 The socioeconomic profile of the sample was one factor that made the present estimates of diet cost substantially higher than estimates based on a representative sample of adults in the USA: $7.94 per 2000 kcal (Method 2) versus $–5 per 2000 kcal in NHANES. Samples primarily composed of higher SES persons would have implications for bias in diet cost estimates using either Methods 2 or 3. Our analyses of all three measures of diet cost by household income (Figure 3) indicated that underestimation of food expenditures using either Methods 2 or 3 was greatest for higher-income people. Another consideration is that eligibility required either having primary or shared responsibility for food purchasing. Finally, following precedent,36 Methods 2 and 3 made the assumption that all foods were purchased at retail and prepared at home.
The home preparation assumption was one factor that led to systematically lower estimates in Methods 2 and 3 relative to Method 1, which accounted for away-from-home consumption. The costs of away-from-home foods reflect not only the cost of food and drink but also the cost of services provided.37 For instance, in Method 1, the cost of plain brewed coffee depended on whether it was prepared at home ($0.09/100 g) or purchased prepared from a coffee shop (>$1.67/100 g). By comparison, our standard database price for prepared coffee (applied to Methods 2 and 3) was $0.04/100 g. The use of standard prices (Methods 2 and 3) also ignored for the possibility that different participants may have paid different prices for the same foods, which can vary substantially by brand and by retail outlet.38 Furthermore, differences in diet cost estimates also were imposed by the inherent difference between the diet diary and FFQ.
Conclusions
There is a growing recognition that the quality of individual diets is closely tied to energy-adjusted diet costs. Given the apparent systematic and positive associations between diet cost and diet quality, the higher cost of favorable dietary patterns in nutritional epidemiology11, 12, 13, 14 may represent a form of confounding that is not entirely addressed through adjustment for indicators of SES.28 Estimates of diet cost can enrich nutrition surveillance by providing quantitative insights into a recognized determinant of food choice in the population.39 The application of food prices to standard dietary assessment tools is a practical way to derive diet costs in the context of dietary research and public health surveillance.
References
De Schutter O The right to an adequate diet: the agriculture-food-health nexus, Report presented at the 19th Session of the United Nations Human Rights Council: United Nations General Assembly, Council HR; 2011. Report No.: A/HRC/19/59.
Lee JH, Ralston RA, Truby H . Influence of food cost on diet quality and risk factors for chronic disease: a systematic review. Nutr Diet 2011; 68: 248–261.
Chan M . Statement at the High-level Conference on World Food Security. World Health Organization: Rome, Italy, 2008.
Beydoun MA, Wang Y . How do socio-economic status, perceived economic barriers and nutritional benefits affect quality of dietary intake among US adults? Eur J Clin Nutr 2008; 62: 303–313.
Turrell G, Hewitt B, Patterson C, Oldenburg B, Gould T . Socioeconomic differences in food purchasing behaviour and suggested implications for diet-related health promotion. J Hum Nutr Diet 2002; 15: 355–364.
Giskes K, Turrell G, Patterson C, Newman B . Socio-economic differences in fruit and vegetable consumption among Australian adolescents and adults. Public Health Nutr 2002; 5: 663–669.
Drewnowski A . The cost of US foods as related to their nutritive value. Am J Clin Nutr 2010; 92: 1181–1188.
Maillot M, Darmon N, Darmon M, Lafay L, Drewnowski A . Nutrient-dense food groups have high energy costs: an econometric approach to nutrient profiling. J Nutr 2007; 137: 1815–1820.
Darmon N, Drewnowski A . Does social class predict diet quality? Am J Clin Nutr 2008; 87: 1107–1117.
Ricciuto LE, Tarasuk VS . An examination of income-related disparities in the nutritional quality of food selections among Canadian households from 1986-2001. Soc Sci Med 2007; 64: 186–198.
Bernstein AM, Bloom DE, Rosner BA, Franz M, Willett WC . Relation of food cost to healthfulness of diet among US women. Am J Clin Nutr. 2010; 92: 1197–1203.
Lopez CN, Martinez-Gonzalez MA, Sanchez-Villegas A, Alonso A, Pimenta AM, Bes-Rastrollo M . Costs of Mediterranean and western dietary patterns in a Spanish cohort and their relationship with prospective weight change. J Epidemiol Community Health 2009; 63: 920–927.
Murakami K, Sasaki S, Okubo H, Takahashi Y, Hosoi Y, Itabashi M . Monetary costs of dietary energy reported by young Japanese women: association with food and nutrient intake and body mass index. Public Health Nutr 2007; 10: 1430–1439.
Schröder H, Marrugat J, Covas MI . High monetary costs of dietary patterns associated with lower body mass index: a population-based study. Int J Obes (Lond) 2006; 30: 1574–1579.
Improving data to analyze food and nutrition policies. Committee on National Statistics, National Research Council of the National Academies. National Academies Press: Washington, D.C. http://www.nap.edu/openbook.php?isbn=0309100054 (accessed 9 September 2013).
Ransley JK, Donnelly JK, Botham H, Khara TN, Greenwood DC, Cade JE . Use of supermarket receipts to estimate energy and fat content of food purchased by lean and overweight families. Appetite 2003; 41: 141–148.
Monsivais P, Rehm CD . Potential nutritional and economic effects of replacing juice with fruit in the diets of children in the United States. Arch Pediatr Adolesc Med 2012.
Rehm CD, Monsivais P, Drewnowski A . The quality and monetary value of diets consumed by adults in the United States. Am J Clin Nutr 2011; 166: 459–464.
Ryden PJ, Hagfors L . Diet cost, diet quality and socio-economic position: how are they related and what contributes to differences in diet costs? Public Health Nutr 2011; 24: 1–13.
Cade J, Upmeier H, Calvert C, Greenwood D . Costs of a healthy diet: analysis from the UK Women's Cohort Study. Public Health Nutr 1999; 2: 505–512.
Townsend MS, Aaron GJ, Monsivais P, Keim NL, Drewnowski A . Less-energy-dense diets of low-income women in California are associated with higher energy-adjusted diet costs. Am J Clin Nutr 2009; 89: 1220–1226.
Monsivais P, Drewnowski A . Lower-energy-density diets are associated with higher monetary costs per kilocalorie and are consumed by women of higher socioeconomic status. J Am Diet Assoc 2009; 109: 814–822.
Murakami K, Sasaki S, Takahashi Y, Uenishi K . Monetary cost of dietary energy is negatively associated with BMI and waist circumference, but not with other metabolic risk factors, in young Japanese women. Public Health Nutr 2008; 23: 1–7.
Murakami K, Sasaki S, Takahashi Y, Uenishi K . Monetary cost of self-reported diet in relation to biomarker-based estimates of nutrient intake in young Japanese women. Public Health Nutr 2009; 12: 1290–1297.
Beresford SA, Johnson KC, Ritenbaugh C, Lasser NL, Snetselaar LG, Black HR et al. Low-fat dietary pattern and risk of colorectal cancer: the Women's Health Initiative Randomized Controlled Dietary Modification Trial. JAMA 2006; 295: 643–654.
Neuhouser ML, Kristal AR, McLerran D, Patterson RE, Atkinson J . Validity of short food frequency questionnaires used in cancer chemoprevention trials: results from the Prostate Cancer Prevention Trial. Cancer Epidemiol Biomarkers Prev 1999; 8: 721–725.
Monsivais P, Drewnowski A . The rising cost of low-energy-density foods. J Am Diet Assoc 2007; 107: 2071–2076.
Aggarwal A, Monsivais P, Drewnowski A . Nutrient intakes linked to better health outcomes are associated with higher diet costs in the US. PLoS One 2012; 7: e37533.
Ambrosini GL, Mackerras D, de Klerk NH, Musk AW . Comparison of an Australian food-frequency questionnaire with diet records: implications for nutrition surveillance. Public Health Nutr 2003; 6: 415–422.
Erkkola M, Karppinen M, Javanainen J, Rasanen L, Knip M, Virtanen SM . Validity and reproducibility of a food frequency questionnaire for pregnant Finnish women. Am J Epidemiol 2001; 154: 466–476.
Murakami K, Sasaki S, Takahashi Y, Okubo H, Hirota N, Notsu A, Fukui M, Date C . Comparability of weighed dietary records and a self-administered diet history questionnaire for estimating monetary cost of dietary energy. Environ Health Insights 2008; 1: 35–43.
U.S. Food Expenditures. United States Department of Agriculture, Economic Research Service. http://www.ers.usda.gov/datafiles/Food_Expenditures/2010table13.xls.
USDA food and nutrient database for dietary studies, 1.0. Agricultural Research Service, Food Surveys Research Group: Beltsville, MD 2004.
Neuhouser ML, Tinker LF, Thomson C, Caan B, Horn LV, Snetselaar L et al. Development of a glycemic index database for food frequency questionnaires used in epidemiologic studies. J Nutr 2006; 136: 1604–1609.
Appelhans BM, Milliron BJ, Woolf K, Johnson TJ, Pagoto SL, Schneider KL et al. Socioeconomic status, energy cost, and nutrient content of supermarket food purchases. Am J Prev Med 2012; 42: 398–402.
Carlson A, Lino M, Juan W-Y, Hanson K, Basiotis PP Thrifty Food Plan, 2006, (U.S.) Center for Nutrition Policy and Promotion; 2007. Report No.: CNPP-19.
Canning P A Revised and Expanded Food Dollar Series: A Better Understanding of Our Food Costs: United States Department of Agriculture Service ER; 2011. Report No.: ERR-114..
Drewnowski A, Aggarwal A, Hurvitz PM, Monsivais P, Moudon AV . Obesity and supermarket access: proximity or price? Am J Public Health 2012; 102: e74–e80.
Carlson A, Lino M, Juan WY, Marcoe K, Bente L, Hiza HAB et al Development of the CNPP Prices Database. Center for Nutrition Policy and Promotion: Washington, DC. USDA, 2008 Contract No.: CNPP-22.
Acknowledgements
This work was supported by the National Research Initiative of the US Department of Agriculture Cooperative State Research Education and Extension Service grant 2004-35215-14441, by grant 5R01DK076608-03 from the NIH. Pablo Monsivais received support from the Centre for Diet and Activity Research, a UKCRC Public Health Research Centre of Excellence funded by the British Heart Foundation, Economic and Social Research Council, Medical Research Council, the National Institute for Health Research and the Wellcome Trust. The authors thank Colin Rehm for constructive comments on earlier versions of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of intrest.
Additional information
Contributors: PM assisted in the design of the study, analyzed the data and led the drafting of the manuscript. SA and MP assisted in the design of the study, administered diet diaries and entered data. MP contributed to the drafting of the manuscript. AD conceived of the study and supervised the research. PM had primary responsibility for final content. All authors read and approved the final manuscript.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Monsivais, P., Perrigue, M., Adams, S. et al. Measuring diet cost at the individual level: a comparison of three methods. Eur J Clin Nutr 67, 1220–1225 (2013). https://doi.org/10.1038/ejcn.2013.176
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2013.176
Keywords
This article is cited by
-
Assessing the Cost of Healthy and Unhealthy Diets: A Systematic Review of Methods
Current Nutrition Reports (2022)
-
Food cost and adherence to guidelines for healthy diets: evidence from Belgium
European Journal of Clinical Nutrition (2021)
-
Socioeconomic and ethnic differences in the relation between dietary costs and dietary quality: the HELIUS study
Nutrition Journal (2019)
-
Validating self-reported food expenditures against food store and eating-out receipts
European Journal of Clinical Nutrition (2016)
-
The relation of potassium and sodium intakes to diet cost among US adults
Journal of Human Hypertension (2015)