Abstract
Background/Objective:
The recent rapid increase in childhood obesity rates suggests that a consideration of the role of the schools in addressing this problem is necessary. ‘Fits me’ program functions to promote eating daily and healthy breakfast among elementary school children.
Methods:
Separate children groups were sampled each year by clusters from seven regions around Israel. They filled a self-administered questionnaire at the beginning of 2003, before the program started, and in 2003–2005, after the program. A separate sample was collected in 2006 in a case–control structure. The answer to the question: ‘what do you eat for breakfast?’ considered as a healthy breakfast if it included one of the following food items: A sandwich (not including chocolate, jam or butter), cereals, vegetable, fruit, egg and dairy product.
Results:
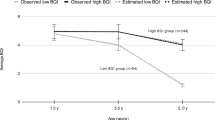
As compared with 2003 before the program, more children reported eating daily breakfast over the years (51–65% before and until 2005, respectively, P for trend<0.01). Odds ratio (OR) and 95% confidence interval (95% CI) for eating a healthy breakfast, in 2006 in the intervention (n=417) vs controls (n=572), adjusted for sex and age were OR=1.53 (95% CI: 1.15–2.04). However, only a third of 75% of the children who ate a healthy breakfast in the intervention group estimated that they were eating a healthy breakfast.
Conclusions:
After implementation an educational program to promote daily and healthy breakfast eating, the goal of a healthier breakfast was achieved. However, one should strive to define an exact definition of a healthy breakfast.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Affenito SG (2007). Breakfast: a missed opportunity. JADA 107, 565–569.
Armitage P (1995). Test for linear trends in Proportions and Frequencies. Biometrics 11, 375–386.
Bellisle F, Rolland-Cachera MF (2007). Commentary on Bellisle F, Rolland-Cachera, MF and the Kellogg Scientific Advisory Committee ‘Child and Nutrition’ (2000) Three consecutive (1993, 1995, 1997) surveys of food intake, nutritional attitudes and knowledge, and lifestyle in 1000 French children, aged 9–11 years. J Hum Nutr Diet 13, 101–111.
Cartwright M, Wardle J, Steggles N, Simon AE, Croker H, Jarvis MJ (2003). Stress and dietary practices in adolescents. Health Psychol 22, 362–369.
Chen X, Sekine M, Hamanishi S, Wang H, Gaina A, Yamagami T (2005). Lifestyles and health-related quality of life in Japanese school children: a cross-sectional study. Prev Med 40, 668–678.
Cho S, Dietrich M, Brown CJ, Clark CA, Block G (2003). The effect of breakfast type on total daily energy intake and body mass index: results from the Third National Health and Nutrition Examination Survey (NHANES III). J Am Coll Nutr 22, 296–302.
Condon EM, Crepinsek MK, Fox MK (2009). School meals: types of foods offered to and consumed by children at lunch and breakfast. J Am Diet Assoc 109 (Suppl 2), S67–S78.
Eliakim A, Nemet D, Balakirski Y, Epstein Y (2007). The effects of nutritional-physical activity school-based intervention on fatness and fitness in preschool children. J Pediatr Endocrinol Metab 20, 711–718.
Gleason PM, Dodd AH (2009). School breakfast program but not school lunch program participation is associated with lower body mass index. J Am Diet Assoc 109 (Suppl 2), S118–S128.
Gonzalez-Suarez C, Worley A, Grimmer-Somers K, Dones V (2009). School-based interventions on childhood obesity: a meta-analysis. Am J Prev Med 37, 418–427.
Grantham-McGregor S (2005). Can the provision of breakfast benefit school performance? Food Nutr Bull 26, 144S–158S.
Hosmer DW, Lemeshow S (2000) In: Chichester, Wiley (ed). Applied Logistic Regression, 2nd ed New York; 2000; ISBN 0-471-35632-8.
Huerta M, Gdalevich M, Haviv J, Bibi H, Scharf S (2006). Ten-year trends in obesity among Israeli schoolchildren: 1990–2000. Acta Paediatrica 95, 444–449.
Kant AK, Andon MB, Angelopoulos TJ, Rippe JM (2008). Association of breakfast energy density with diet quality and body mass index in American adults: National Health and Nutrition Examination Surveys, 1999–2004. Am J Clin Nutr 88, 1396–1404.
Keski-Rahkonen A, Kaprio J, Rissanen A, Virkkunen M, Rose RJ (2003). Breakfast skipping and health-compromising behaviors in adolescents and adults. Eur J Clin Nutr 57, 842–853.
Nicklas TA, Myers L, Reger C, Beech B, Berenson GS (1998). Impact of breakfast consumption on nutritional adequacy of the diets of young adults in Bogalusa, Louisiana: ethnic and gender contrasts. J Am Diet Assoc 98, 1432–1438.
O’Dea JA, Caputi P (2007). Association between socioeconomic status, weight, age and gender, and the body image and weight control practices of 6- to 19-year-old children and adolescents. Health Education Research 16, 521–532.
Pearson N, Biddle SJ, Gorely T (2009). Family correlates of breakfast consumption among children and adolescents. A systematic review. Appetite 52, 1–7.
Pollitt E, Cueto S, Jacoby ER (1998). Fasting and cognition in well- and undernourished schoolchildren: a review of three experimental studies. Am J Clin Nutr. 67, 779S–784S.
Rampersaud GC, Pereira MA, Girard BL, Adams J, Metzl JD (2005). Breakfast habits, nutritional status, body weight, and academic performance in children and adolescents. J Am Diet Assoc 105, 743–760.
Siega-Riz AM, Popkin BM, Carson T (2000). Differences in food patterns at breakfast by sociodemographic characteristics among a nationally representative sample of adults in the United States. Prev Med 30, 415–424.
Song WO, Chun OK, Obayashi S, Cho S, Chung CE (2005). Is consumption of breakfast associated with body mass index in US adults? J Am Diet Assoc 105, 1373–1382.
Summerbell CD, Moody RC, Shanks J, Stock MJ, Geissler C (1996). Relationship between feeding pattern and body mass index in 220 free-living people in four age groups. Eur J Clin Nutr 50, 513–519.
Tapper K, Murphy S, Lynch R, Clark R, Moore GF, Moore L (2008). Development of a scale to measure 9-11-year-olds’ attitudes towards breakfast. Eur J Clin Nutr 62, 511–518.
Vereecken C, Dupuy M, Rasmussen M, Kelly C, Nansel TR, Al Sabbah H, et al., HBSC Eating and Dieting Focus Group (2009). Breakfast consumption and its socio-demographic and lifestyle correlates in schoolchildren in 41 countries participating in the HBSC study. Int J Public Health 54 (Suppl 2), S180–S190.
Widenhorn-Müller K, Hille K, Klenk J, Weiland U (2008). Influence of having breakfast on cognitive performance and mood in 13- to 20-year-old high school students: results of a crossover trial. Pediatrics 22, 279–284.
Williams P (2007). Breakfast and the diets of Australian children and adolescents: an analysis of data from the 1995 National Nutrition Survey. Int J Food Sci 58, 201–216.
Acknowledgements
‘Fits me’ (Tafur Alay) is a joint project the Ministry of Health, Israel Association of Family Physicians, Israel Pediatrics Association, Israel Heart Society, Israel Pediatric Dentistry Association, the Association for Advancement of Nursing in Israel's Public Health, Atid – Association for Advancing Nutrition and Diet in Israel, Elective Parents Associations and approved by the Ministry of Education. This study was supported by Unilever Israel – Telma. We thank Prolog Entrepreneurship and Marketing for concept and management. We also thank Orna Levy, chief dietitian, Unilever, Israel for initiating and Israela Herbelin, CEO prolog initiation and marketing CSM for developing and implementing the program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Eilat-Adar, S., Koren-Morag, N., Siman-Tov, M. et al. School-based intervention to promote eating daily and healthy breakfast: A survey and a case–control study. Eur J Clin Nutr 65, 203–209 (2011). https://doi.org/10.1038/ejcn.2010.247
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2010.247
Keywords
This article is cited by
-
Hydration and meal habits of physicians and medical learners: a literature review
European Journal of Nutrition (2022)