Abstract
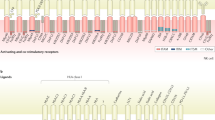
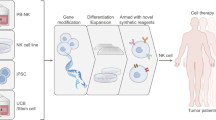
Natural killer (NK) cells play critical roles in host immunity against cancer. In response, cancers develop mechanisms to escape NK cell attack or induce defective NK cells. Current NK cell-based cancer immunotherapy aims to overcome NK cell paralysis using several approaches. One approach uses expanded allogeneic NK cells, which are not inhibited by self histocompatibility antigens like autologous NK cells, for adoptive cellular immunotherapy. Another adoptive transfer approach uses stable allogeneic NK cell lines, which is more practical for quality control and large-scale production. A third approach is genetic modification of fresh NK cells or NK cell lines to highly express cytokines, Fc receptors and/or chimeric tumor-antigen receptors. Therapeutic NK cells can be derived from various sources, including peripheral or cord blood cells, stem cells or even induced pluripotent stem cells (iPSCs), and a variety of stimulators can be used for large-scale production in laboratories or good manufacturing practice (GMP) facilities, including soluble growth factors, immobilized molecules or antibodies, and other cellular activators. A list of NK cell therapies to treat several types of cancer in clinical trials is reviewed here. Several different approaches to NK-based immunotherapy, such as tissue-specific NK cells, killer receptor-oriented NK cells and chemically treated NK cells, are discussed. A few new techniques or strategies to monitor NK cell therapy by non-invasive imaging, predetermine the efficiency of NK cell therapy by in vivo experiments and evaluate NK cell therapy approaches in clinical trials are also introduced.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Borghaei H, Smith MR, Campbell KS . Immunotherapy of cancer. Eur J Pharmacol 2009; 625: 41–54.
Becker Y . Molecular immunological approaches to biotherapy of human cancers—a review, hypothesis and implications. Anticancer Res 2006; 26: 1113–1134.
Catchpole B, Gould SM, Kellett-Gregory LM, Dobson JM . Immunosuppressive cytokines in the regional lymph node of a dog suffering from oral malignant melanoma. J Small Anim Pract 2002; 43: 464–467.
Zagury D, Gallo RC . Anti-cytokine Ab immune therapy: present status and perspectives. Drug Discov Today 2004; 9: 72–81.
Morse MA, Mosca PJ, Clay TM, Lyerly HK . Dendritic cell maturation in active immunotherapy strategies. Expert Opin Biol Ther 2002; 2: 35–43.
Yamaguchi T, Sakaguchi S . Regulatory T cells in immune surveillance and treatment of cancer. Semin Cancer Biol 2006; 16: 115–123.
Salih HR, Goehlsdorf D, Steinle A . Release of MICB molecules by tumor cells: mechanism and soluble MICB in sera of cancer patients. Hum Immunol 2006; 67: 188–195.
Salih HR, Rammensee HG, Steinle A . Cutting edge: down-regulation of MICA on human tumors by proteolytic shedding. J Immunol 2002; 169: 4098–4102.
Waldhauer I, Steinle A . Proteolytic release of soluble UL16-binding protein 2 from tumor cells. Cancer Res 2006; 66: 2520–2526.
Green DR, Bissonnette RP, Glynn JM, Shi Y . Activation-induced apoptosis in lymphoid systems. Semin Immunol 1992; 4: 379–388.
Saff RR, Spanjaard ES, Hohlbaum AM, Marshak-Rothstein A . Activation-induced cell death limits effector function of CD4 tumor-specific T cells. J Immunol 2004; 172: 6598–6606.
Baxevanis CN, Perez SA, Papamichail M . Cancer immunotherapy. Crit Rev Clin Lab Sci 2009; 46: 167–189.
Zhao E, Xu H, Wang L, Kryczek I, Wu K, Hu Y et al. Bone marrow and the control of immunity. Cell Mol Immunol 2012; 9: 11–19.
Herberman RB, Nunn ME, Lavrin DH . Natural cytotoxic reactivity of mouse lymphoid cells against syngeneic acid allogeneic tumors. I. Distribution of reactivity and specificity. Int J Cancer 1975; 16: 216–229.
Kiessling R, Klein E, Wigzell H . “Natural” killer cells in the mouse. I. Cytotoxic cells with specificity for mouse Moloney leukemia cells. Specificity and distribution according to genotype. Eur J Immunol 1975; 5: 112–117.
Jiang X, Chen Y, Peng H, Tian Z . Single line or parallel lines: NK cell differentiation driven by T-bet and Eomes. Cell Mol Immunol 2012; 9: 193–194.
di Santo JP . Natural killer cell developmental pathways: a question of balance. Annu Rev Immunol 2006; 24: 257–286.
Gregoire C, Chasson L, Luci C, Tomasello E, Geissmann F, Vivier E et al. The trafficking of natural killer cells. Immunol Rev 2007; 220: 169–182.
Cooper MA, Fehniger TA, Caligiuri MA . The biology of human natural killer-cell subsets. Trends Immunol 2001; 22: 633–640.
Anfossi N, Andre P, Guia S, Falk CS, Roetynck S, Stewart CA et al. Human NK cell education by inhibitory receptors for MHC class I. Immunity 2006; 25: 331–342.
Ferlazzo G, Munz C . NK cell compartments and their activation by dendritic cells. J Immunol 2004; 172: 1333–1339.
Roder JC, Pross HF . The biology of the human natural killer cell. J Clin Immunol 1982; 2: 249–263.
Cerwenka A, Lanier LL . Natural killer cells, viruses and cancer. Nat Rev Immunol 2001; 1: 41–49.
Miller JS . The biology of natural killer cells in cancer, infection, and pregnancy. Exp Hematol 2001; 29: 1157–1168.
Vitale M, Sivori S, Pende D, Augugliaro R, di Donato C, Amoroso A et al. Physical and functional independency of p70 and p58 natural killer (NK) cell receptors for HLA class I: their role in the definition of different groups of alloreactive NK cell clones. Proc Natl Acad Sci USA 1996; 93: 1453–1457.
Vivier E, Tomasello E, Baratin M, Walzer T, Ugolini S . Functions of natural killer cells. Nat Immunol 2008; 9: 503–510.
Kumar V, McNerney ME . A new self: MHC-class-I-independent natural-killer-cell self-tolerance. Nat Rev Immunol 2005; 5: 363–374.
Karlhofer FM, Ribaudo RK, Yokoyama WM . MHC class I alloantigen specificity of Ly-49+ IL-2-activated natural killer cells. Nature 1992; 358: 66–70.
Colonna M, Samaridis J . Cloning of immunoglobulin-superfamily members associated with HLA-C and HLA-B recognition by human natural killer cells. Science 1995; 268: 405–408.
Walzer T, Dalod M, Robbins SH, Zitvogel L, Vivier E . Natural-killer cells and dendritic cells: “l'union fait la force”. Blood 2005; 106: 2252–2258.
Waldhauer I, Steinle A . NK cells and cancer immunosurveillance. Oncogene 2008; 27: 5932–5943.
Wu L, Zhang C, Zhang J . HMBOX1 negatively regulates NK cell functions by suppressing the NKG2D/DAP10 signaling pathway. Cell Mol Immunol 2011; 8: 433–440.
Paust S, von Andrian UH . Natural killer cell memory. Nat Immunol; 12: 500–508.
Sun JC, Lanier LL . NK cell development, homeostasis and function: parallels with CD8+ T cells. Nat Rev Immunol 2011; 11: 645–657.
Herberman RB, Holden HT . Natural cell-mediated immunity. Adv Cancer Res 1978; 27: 305–377.
Riccardi C, Santoni A, Barlozzari T, Puccetti P, Herberman RB . In vivo natural reactivity of mice against tumor cells. Int J Cancer 1980; 25: 475–486.
Barlozzari T, Reynolds CW, Herberman RB . In vivo role of natural killer cells: involvement of large granular lymphocytes in the clearance of tumor cells in anti-asialo GM1-treated rats. J Immunol 1983; 131: 1024–1027.
Hayakawa Y, Smyth MJ . Innate immune recognition and suppression of tumors. Adv Cancer Res 2006; 95: 293–322.
Kim S, Iizuka K, Aguila HL, Weissman IL, Yokoyama WM . In vivo natural killer cell activities revealed by natural killer cell-deficient mice. Proc Natl Acad Sci USA 2000; 97: 2731–2736.
Smyth MJ, Hayakawa Y, Takeda K, Yagita H . New aspects of natural-killer-cell surveillance and therapy of cancer. Nat Rev Cancer 2002; 2: 850–861.
Wu J, Lanier LL . Natural killer cells and cancer. Adv Cancer Res 2003; 90: 127–156.
Imai K, Matsuyama S, Miyake S, Suga K, Nakachi K . Natural cytotoxic activity of peripheral-blood lymphocytes and cancer incidence: an 11-year follow-up study of a general population. Lancet 2000; 356: 1795–1799.
Coca S, Perez-Piqueras J, Martinez D, Colmenarejo A, Saez MA, Vallejo C et al. The prognostic significance of intratumoral natural killer cells in patients with colorectal carcinoma. Cancer 1997; 79: 2320–2328.
Ishigami S, Natsugoe S, Tokuda K, Nakajo A, Che X, Iwashige H et al. Prognostic value of intratumoral natural killer cells in gastric carcinoma. Cancer 2000; 88: 577–583.
Villegas FR, Coca S, Villarrubia VG, Jimenez R, Chillon MJ, Jareno J et al. Prognostic significance of tumor infiltrating natural killer cells subset CD57 in patients with squamous cell lung cancer. Lung Cancer 2002; 35: 23–28.
Ljunggren HG, Malmberg KJ . Prospects for the use of NK cells in immunotherapy of human cancer. Nat Rev Immunol 2007; 7: 329–339.
Ljunggren HG, Karre K . Host resistance directed selectively against H-2-deficient lymphoma variants. Analysis of the mechanism. J Exp Med 1985; 162: 1745–1759.
Karre K, Ljunggren HG, Piontek G, Kiessling R . Selective rejection of H-2-deficient lymphoma variants suggests alternative immune defence strategy. Nature 1986; 319: 675–678.
Ljunggren HG, Karre K . In search of the ‘missing self’: MHC molecules and NK cell recognition. Immunol Today 1990; 11: 237–244.
van den Broek MF, Kagi D, Zinkernagel RM, Hengartner H . Perforin dependence of natural killer cell-mediated tumor control in vivo. Eur J Immunol 1995; 25: 3514–3516.
Smyth MJ, Kelly JM, Baxter AG, Korner H, Sedgwick JD . An essential role for tumor necrosis factor in natural killer cell-mediated tumor rejection in the peritoneum. J Exp Med 1998; 188: 1611–1619.
Smyth MJ, Thia KY, Cretney E, Kelly JM, Snook MB, Forbes CA et al. Perforin is a major contributor to NK cell control of tumor metastasis. J Immunol 1999; 162: 6658–6662.
Kagi D, Ledermann B, Burki K, Seiler P, Odermatt B, Olsen KJ et al. Cytotoxicity mediated by T cells and natural killer cells is greatly impaired in perforin-deficient mice. Nature 1994; 369: 31–37.
Trapani JA, Davis J, Sutton VR, Smyth MJ . Proapoptotic functions of cytotoxic lymphocyte granule constituents in vitro and in vivo. Curr Opin Immunol 2000; 12: 323–329.
Bradley M, Zeytun A, Rafi-Janajreh A, Nagarkatti PS, Nagarkatti M . Role of spontaneous and interleukin-2-induced natural killer cell activity in the cytotoxicity and rejection of Fas+ and Fas- tumor cells. Blood 1998; 92: 4248–4255.
Screpanti V, Wallin RP, Ljunggren HG, Grandien A . A central role for death receptor-mediated apoptosis in the rejection of tumors by NK cells. J Immunol 2001; 167: 2068–2073.
Kayagaki N, Yamaguchi N, Nakayama M, Takeda K, Akiba H, Tsutsui H et al. Expression and function of TNF-related apoptosis-inducing ligand on murine activated NK cells. J Immunol 1999; 163: 1906–1913.
Takeda K, Hayakawa Y, Smyth MJ, Kayagaki N, Yamaguchi N, Kakuta S et al. Involvement of tumor necrosis factor-related apoptosis-inducing ligand in surveillance of tumor metastasis by liver natural killer cells. Nat Med 2001; 7: 94–100.
Cretney E, Takeda K, Yagita H, Glaccum M, Peschon JJ, Smyth MJ . Increased susceptibility to tumor initiation and metastasis in TNF-related apoptosis-inducing ligand-deficient mice. J Immunol 2002; 168: 1356–1361.
Sutlu T, Alici E . Natural killer cell-based immunotherapy in cancer: current insights and future prospects. J Intern Med 2009; 266: 154–181.
Street SE, Cretney E, Smyth MJ . Perforin and interferon-gamma activities independently control tumor initiation, growth, and metastasis. Blood 2001; 97: 192–197.
Smyth MJ, Crowe NY, Pellicci DG, Kyparissoudis K, Kelly JM, Takeda K et al. Sequential production of interferon-gamma by NK1.1(+) T cells and natural killer cells is essential for the antimetastatic effect of alpha-galactosylceramide. Blood 2002; 99: 1259–1266.
Cifone MG, D’Alo S, Parroni R, Millimaggi D, Biordi L, Martinotti S et al. Interleukin-2-activated rat natural killer cells express inducible nitric oxide synthase that contributes to cytotoxic function and interferon-gamma production. Blood 1999; 93: 3876–3884.
Furuke K, Burd PR, Horvath-Arcidiacono JA, Hori K, Mostowski H, Bloom ET . Human NK cells express endothelial nitric oxide synthase, and nitric oxide protects them from activation-induced cell death by regulating expression of TNF-alpha. J Immunol 1999; 163: 1473–1480.
Talmadge JE, Phillips H, Schindler J, Tribble H, Pennington R . Systematic preclinical study on the therapeutic properties of recombinant human interleukin 2 for the treatment of metastatic disease. Cancer Res 1987; 47: 5725–5732.
Trinchieri G . Interleukin-12: a cytokine at the interface of inflammation and immunity. Adv Immunol 1998; 70: 83–243.
Wiltrout RH, Herberman RB, Zhang SR, Chirigos MA, Ortaldo JR, Green KM, Jr et al . Role of organ-associated NK cells in decreased formation of experimental metastases in lung and liver. J Immunol 1985; 134: 4267–4275.
Kodama T, Takeda K, Shimozato O, Hayakawa Y, Atsuta M, Kobayashi K et al. Perforin-dependent NK cell cytotoxicity is sufficient for anti-metastatic effect of IL-12. Eur J Immunol 1999; 29: 1390–1396.
Smyth MJ, Cretney E, Takeda K, Wiltrout RH, Sedger LM, Kayagaki N et al. Tumor necrosis factor-related apoptosis-inducing ligand (TRAIL) contributes to interferon gamma-dependent natural killer cell protection from tumor metastasis. J Exp Med 2001; 193: 661–670.
Yao L, Sgadari C, Furuke K, Bloom ET, Teruya-Feldstein J, Tosato G . Contribution of natural killer cells to inhibition of angiogenesis by interleukin-12. Blood 1999; 93: 1612–1621.
Bryceson YT, March ME, Ljunggren HG, Long EO . Activation, coactivation, and costimulation of resting human natural killer cells. Immunol Rev 2006; 214: 73–91.
Martin-Fontecha A, Thomsen LL, Brett S, Gerard C, Lipp M, Lanzavecchia A et al. Induced recruitment of NK cells to lymph nodes provides IFN-gamma for T(H)1 priming. Nat Immunol 2004; 5: 1260–1265.
Mocikat R, Braumuller H, Gumy A, Egeter O, Ziegler H, Reusch U et al. Natural killer cells activated by MHC class I(low) targets prime dendritic cells to induce protective CD8 T cell responses. Immunity 2003; 19: 561–569.
Kelly JM, Darcy PK, Markby JL, Godfrey DI, Takeda K, Yagita H et al. Induction of tumor-specific T cell memory by NK cell-mediated tumor rejection. Nat Immunol 2002; 3: 83–90.
Nguyen-Pham TN, Yang DH, Nguyen TA, Lim MS, Hong CY, Kim MH et al. Optimal culture conditions for the generation of natural killer cell-induced dendritic cells for cancer immunotherapy. Cell Mol Immunol 2012; 9: 45–53.
Piccioli D, Sbrana S, Melandri E, Valiante NM . Contact-dependent stimulation and inhibition of dendritic cells by natural killer cells. J Exp Med 2002; 195: 335–341.
Gerosa F, Baldani-Guerra B, Nisii C, Marchesini V, Carra G, Trinchieri G . Reciprocal activating interaction between natural killer cells and dendritic cells. J Exp Med 2002; 195: 327–333.
Maki G, Krystal G, Dougherty G, Takei F, Klingemann HG . Induction of sensitivity to NK-mediated cytotoxicity by TNF-alpha treatment: possible role of ICAM-3 and CD44. Leukemia 1998; 12: 1565–1572.
Costello RT, Sivori S, Marcenaro E, Lafage-Pochitaloff M, Mozziconacci MJ, Reviron D et al. Defective expression and function of natural killer cell-triggering receptors in patients with acute myeloid leukemia. Blood 2002; 99: 3661–3667.
Farag SS, Caligiuri MA . Cytokine modulation of the innate immune system in the treatment of leukemia and lymphoma. Adv Pharmacol 2004; 51: 295–318.
Smyth MJ, Cretney E, Kershaw MH, Hayakawa Y . Cytokines in cancer immunity and immunotherapy. Immunol Rev 2004; 202: 275–293.
Becknell B, Caligiuri MA . Interleukin-2, interleukin-15, and their roles in human natural killer cells. Adv Immunol 2005; 86: 209–239.
Rosenberg SA . Interleukin-2 and the development of immunotherapy for the treatment of patients with cancer. Cancer J Sci Am 2000; Suppl 1 S2–S7.
Colombo MP, Trinchieri G . Interleukin-12 in anti-tumor immunity and immunotherapy. Cytokine Growth Factor Rev 2002; 13: 155–168.
Rosenberg SA . Immunotherapy of cancer by systemic administration of lymphoid cells plus interleukin-2. J Biol Response Mod 1984; 3: 501–511.
Ghiringhelli F, Menard C, Terme M, Flament C, Taieb J, Chaput N et al. CD4+CD25+ regulatory T cells inhibit natural killer cell functions in a transforming growth factor-beta-dependent manner. J Exp Med 2005; 202: 1075–1085.
Rodella L, Zamai L, Rezzani R, Artico M, Peri G, Falconi M et al. Interleukin 2 and interleukin 15 differentially predispose natural killer cells to apoptosis mediated by endothelial and tumour cells. Br J Haematol 2001; 115: 442–450.
Hayakawa M, Hatano T, Ogawa Y, Gakiya M, Ogura H, Osawa A . Treatment of advanced renal cell carcinoma using regional arterial administration of lymphokine-activated killer cells in combination with low doses of rIL-2. Urol Int 1994; 53: 117–124.
Boiardi A, Silvani A, Ruffini PA, Rivoltini L, Parmiani G, Broggi G et al. Loco-regional immunotherapy with recombinant interleukin-2 and adherent lymphokine-activated killer cells (A-LAK) in recurrent glioblastoma patients. Cancer Immunol Immunother 1994; 39: 193–197.
Hayes RL, Koslow M, Hiesiger EM, Hymes KB, Hochster HS, Moore EJ et al. Improved long term survival after intracavitary interleukin-2 and lymphokine-activated killer cells for adults with recurrent malignant glioma. Cancer 1995; 76: 840–852.
Keilholz U, Scheibenbogen C, Brado M, Georgi P, Maclachlan D, Brado B et al. Regional adoptive immunotherapy with interleukin-2 and lymphokine-activated killer (LAK) cells for liver metastases. Eur J Cancer A 1994; 30A: 103–105
Ma HL, Whitters MJ, Konz RF, Senices M, Young DA, Grusby MJ et al. IL-21 activates both innate and adaptive immunity to generate potent antitumor responses that require perforin but are independent of IFN-gamma. J Immunol 2003; 171: 608–615.
Berzofsky JA, Ahlers JD, Belyakov IM . Strategies for designing and optimizing new generation vaccines. Nat Rev Immunol 2001; 1: 209–219.
Kobayashi H, Dubois S, Sato N, Sabzevari H, Sakai Y, Waldmann TA et al. Role of trans-cellular IL-15 presentation in the activation of NK cell-mediated killing, which leads to enhanced tumor immunosurveillance. Blood 2005; 105: 721–727.
Zamai L, Ponti C, Mirandola P, Gobbi G, Papa S, Galeotti L et al. NK cells and cancer. J Immunol 2007; 178: 4011–4016.
Escudier B, Farace F, Angevin E, Charpentier F, Nitenberg G, Triebel F et al. Immunotherapy with interleukin-2 (IL2) and lymphokine-activated natural killer cells: improvement of clinical responses in metastatic renal cell carcinoma patients previously treated with IL2. Eur J Cancer A 1994; 30A: 1078–1083
Ishikawa E, Tsuboi K, Saijo K, Harada H, Takano S, Nose T et al. Autologous natural killer cell therapy for human recurrent malignant glioma. Anticancer Res 2004; 24: 1861–1871.
deMagalhaes-Silverman M, Donnenberg A, Lembersky B, Elder E, Lister J, Rybka W et al. Posttransplant adoptive immunotherapy with activated natural killer cells in patients with metastatic breast cancer. J Immunother 2000; 23: 154–160.
Miller JS, Tessmer-Tuck J, Pierson BA, Weisdorf D, McGlave P, Blazar BR et al. Low dose subcutaneous interleukin-2 after autologous transplantation generates sustained in vivo natural killer cell activity. Biol Blood Marrow Transplant 1997; 3: 34–44.
Burns LJ, Weisdorf DJ, DeFor TE, Vesole DH, Repka TL, Blazar BR et al. IL-2-based immunotherapy after autologous transplantation for lymphoma and breast cancer induces immune activation and cytokine release: a phase I/II trial. Bone Marrow Transplant 2003; 32: 177–186.
Ruggeri L, Capanni M, Urbani E, Perruccio K, Shlomchik WD, Tosti A et al. Effectiveness of donor natural killer cell alloreactivity in mismatched hematopoietic transplants. Science 2002; 295: 2097–2100.
Ruggeri L, Mancusi A, Perruccio K, Burchielli E, Martelli MF, Velardi A . Natural killer cell alloreactivity for leukemia therapy. J Immunother 2005; 28: 175–182.
Miller JS, Soignier Y, Panoskaltsis-Mortari A, McNearney SA, Yun GH, Fautsch SK et al. Successful adoptive transfer and in vivo expansion of human haploidentical NK cells in patients with cancer. Blood 2005; 105: 3051–3057.
Iliopoulou EG, Kountourakis P, Karamouzis MV, Doufexis D, Ardavanis A, Baxevanis CN et al. A phase I trial of adoptive transfer of allogeneic natural killer cells in patients with advanced non-small cell lung cancer. Cancer Immunol Immunother 2010; 59: 1781–1789.
Lundqvist A, McCoy JP, Samsel L, Childs R . Reduction of GVHD and enhanced antitumor effects after adoptive infusion of alloreactive Ly49-mismatched NK cells from MHC-matched donors. Blood 2007; 109: 3603–3606.
Sconocchia G, Titus JA, Segal DM . Signaling pathways regulating CD44-dependent cytolysis in natural killer cells. Blood 1997; 90: 716–725.
Iannello A, Ahmad A . Role of antibody-dependent cell-mediated cytotoxicity in the efficacy of therapeutic anti-cancer monoclonal antibodies. Cancer Metastasis Rev 2005; 24: 487–499.
Alderson KL, Sondel PM . Clinical cancer therapy by NK cells via antibody-dependent cell-mediated cytotoxicity. J Biomed Biotechnol 2011; 2011: 379123
Sorkin LS, Otto M, Baldwin WM 3rd, Vail E, Gillies SD, Handgretinger R et al. Anti-GD(2) with an FC point mutation reduces complement fixation and decreases antibody-induced allodynia. Pain 2010; 149: 135–142.
Navid F, Santana VM, Barfield RC . Anti-GD2 antibody therapy for GD2-expressing tumors. Curr Cancer Drug Targets 2010; 10: 200–209.
Horton HM, Bernett MJ, Pong E, Peipp M, Karki S, Chu SY et al. Potent in vitro and in vivo activity of an Fc-engineered anti-CD19 monoclonal antibody against lymphoma and leukemia. Cancer Res 2008; 68: 8049–8057.
Zalevsky J, Leung IW, Karki S, Chu SY, Zhukovsky EA, Desjarlais JR et al. The impact of Fc engineering on an anti-CD19 antibody: increased Fcgamma receptor affinity enhances B-cell clearing in nonhuman primates. Blood 2009; 113: 3735–3743.
Parihar R, Dierksheide J, Hu Y, Carson WE . IL-12 enhances the natural killer cell cytokine response to Ab-coated tumor cells. J Clin Invest 2002; 110: 983–992.
Parihar R, Nadella P, Lewis A, Jensen R, de Hoff C, Dierksheide JE et al. A phase I study of interleukin 12 with trastuzumab in patients with human epidermal growth factor receptor-2-overexpressing malignancies: analysis of sustained interferon gamma production in a subset of patients. Clin Cancer Res 2004; 10: 5027–5037.
Ortaldo JR, Woodhouse C, Morgan AC, Herberman RB, Cheresh DA, Reisfeld R . Analysis of effector cells in human antibody-dependent cellular cytotoxicity with murine monoclonal antibodies. J Immunol 1987; 138: 3566–3572.
Schultz KR, Klarnet JP, Peace DJ, Cheever MA, Badger CC, Bernstein ID et al. Monoclonal antibody therapy of murine lymphoma: enhanced efficacy by concurrent administration of interleukin 2 or lymphokine-activated killer cells. Cancer Res 1990; 50: 5421–5425.
Parrish-Novak J, Dillon SR, Nelson A, Hammond A, Sprecher C, Gross JA et al. Interleukin 21 and its receptor are involved in NK cell expansion and regulation of lymphocyte function. Nature 2000; 408: 57–63.
Brady J, Hayakawa Y, Smyth MJ, Nutt SL . IL-21 induces the functional maturation of murine NK cells. J Immunol 2004; 172: 2048–2058.
Betting DJ, Yamada RE, Kafi K, Said J, van Rooijen N, Timmerman JM . Intratumoral but not systemic delivery of CpG oligodeoxynucleotide augments the efficacy of anti-CD20 monoclonal antibody therapy against B cell lymphoma. J Immunother 2009; 32: 622–631.
Kohrt HE, Houot R, Goldstein MJ, Weiskopf K, Alizadeh AA, Brody J et al. CD137 stimulation enhances the antilymphoma activity of anti-CD20 antibodies. Blood 2011; 117: 2423–2432.
Yamane BH, Hank JA, Albertini MR, Sondel PM . The development of antibody-IL-2 based immunotherapy with hu14.18-IL2 (EMD-273063) in melanoma and neuroblastoma. Expert Opin Investig Drugs 2009; 18: 991–1000.
Buhtoiarov IN, Neal ZC, Gan J, Buhtoiarova TN, Patankar MS, Gubbels JA et al. Differential internalization of hu14.18-IL2 immunocytokine by NK and tumor cell: impact on conjugation, cytotoxicity, and targeting. J Leukoc Biol 2011; 89: 625–638.
Hernandez-Ilizaliturri FJ, Reddy N, Holkova B, Ottman E, Czuczman MS . Immunomodulatory drug CC-5013 or CC-4047 and rituximab enhance antitumor activity in a severe combined immunodeficient mouse lymphoma model. Clin Cancer Res 2005; 11: 5984–5992.
Binyamin L, Alpaugh RK, Hughes TL, Lutz CT, Campbell KS, Weiner LM . Blocking NK cell inhibitory self-recognition promotes antibody-dependent cellular cytotoxicity in a model of anti-lymphoma therapy. J Immunol 2008; 180: 6392–6401.
Velardi A, Ruggeri L, Mancusi A, Aversa F, Christiansen FT . Natural killer cell allorecognition of missing self in allogeneic hematopoietic transplantation: a tool for immunotherapy of leukemia. Curr Opin Immunol 2009; 21: 525–530.
Cheng M, Zhang J, Jiang W, Chen Y, Tian Z . Natural killer cell lines in tumor immunotherapy. Front Med 2012; 6: 56–66.
Cheng M, Ma J, Chen Y, Zhang J, Zhao W, Wei H et al. Establishment, characterization and successful adaptive therapy against human tumors of NKG cell, a new human NK cell line. Cell Transplant 2011; 20: 1731–1746.
Yoneda N, Tatsumi E, Kawano S, Teshigawara K, Oka T, Fukuda M et al. Detection of Epstein-Barr virus genome in natural-killer-like cell line, YT. Leukemia 1992; 6: 136–141.
Tsuchiyama J, Yoshino T, Mori M, Kondoh E, Oka T, Akagi T et al. Characterization of a novel human natural killer-cell line (NK-YS) established from natural killer cell lymphoma/leukemia associated with Epstein-Barr virus infection. Blood 1998; 92: 1374–1383.
Yagita M, Huang CL, Umehara H, Matsuo Y, Tabata R, Miyake M et al. A novel natural killer cell line (KHYG-1) from a patient with aggressive natural killer cell leukemia carrying a p53 point mutation. Leukemia 2000; 14: 922–930.
Tonn T, Becker S, Esser R, Schwabe D, Seifried E . Cellular immunotherapy of malignancies using the clonal natural killer cell line NK-92. J Hematother Stem Cell Res 2001; 10: 535–544.
Klingemann HG . Natural killer cell-based immunotherapeutic strategies. Cytotherapy 2005; 7: 16–22.
Malmberg KJ, Bryceson YT, Carlsten M, Andersson S, Bjorklund A, Bjorkstrom NK et al. NK cell-mediated targeting of human cancer and possibilities for new means of immunotherapy. Cancer Immunol Immunother 2008; 57: 1541–1552.
Suck G, Branch DR, Smyth MJ, Miller RG, Vergidis J, Fahim S et al. KHYG-1, a model for the study of enhanced natural killer cell cytotoxicity. Exp Hematol 2005; 33: 1160–1171.
Suck G, Branch DR, Keating A . Irradiated KHYG-1 retains cytotoxicity: potential for adoptive immunotherapy with a natural killer cell line. Int J Radiat Biol 2006; 82: 355–361.
Robertson MJ, Cochran KJ, Cameron C, Le JM, Tantravahi R, Ritz J . Characterization of a cell line, NKL, derived from an aggressive human natural killer cell leukemia. Exp Hematol 1996; 24: 406–415.
Zhang C, Zhang J, Niu J, Tian Z . Interleukin-15 improves cytotoxicity of natural killer cells via up-regulating NKG2D and cytotoxic effector molecule expression as well as STAT1 and ERK1/2 phosphorylation. Cytokine 2008; 42: 128–136.
Garcia-Lora A, Martinez M, Pedrinaci S, Garrido F . Different regulation of PKC isoenzymes and MAPK by PSK and IL-2 in the proliferative and cytotoxic activities of the NKL human natural killer cell line. Cancer Immunol Immunother 2003; 52: 59–64.
Pedrinaci S, Algarra I, Garrido F . Protein-bound polysaccharide (PSK) induces cytotoxic activity in the NKL human natural killer cell line. Int J Clin Lab Res 1999; 29: 135–140.
Nagashima S, Mailliard R, Kashii Y, Reichert TE, Herberman RB, Robbins P et al. Stable transduction of the interleukin-2 gene into human natural killer cell lines and their phenotypic and functional characterization in vitro and in vivo. Blood 1998; 91: 3850–3861.
Zhang J, Sun R, Wei H, Tian Z . Characterization of interleukin-15 gene-modified human natural killer cells: implications for adoptive cellular immunotherapy. Haematologica 2004; 89: 338–347.
Jiang W, Zhang J, Tian Z . Functional characterization of interleukin-15 gene transduction into the human natural killer cell line NKL. Cytotherapy 2008; 10: 265–274.
Tam YK, Maki G, Miyagawa B, Hennemann B, Tonn T, Klingemann HG . Characterization of genetically altered, interleukin 2-independent natural killer cell lines suitable for adoptive cellular immunotherapy. Hum Gene Ther 1999; 10: 1359–1373.
Konstantinidis KV, Alici E, Aints A, Christensson B, Ljunggren HG, Dilber MS . Targeting IL-2 to the endoplasmic reticulum confines autocrine growth stimulation to NK-92 cells. Exp Hematol 2005; 33: 159–164.
Zhang J, Sun R, Wei H, Tian Z . Characterization of stem cell factor gene-modified human natural killer cell line, NK-92 cells: implication in NK cell-based adoptive cellular immunotherapy. Oncol Rep 2004; 11: 1097–1106.
Schirrmann T, Pecher G . Human natural killer cell line modified with a chimeric immunoglobulin T-cell receptor gene leads to tumor growth inhibition in vivo. Cancer Gene Ther 2002; 9: 390–398.
Schirrmann T, Pecher G . Specific targeting of CD33+ leukemia cells by a natural killer cell line modified with a chimeric receptor. Leuk Res 2005; 29: 301–306.
Uherek C, Tonn T, Uherek B, Becker S, Schnierle B, Klingemann HG et al. Retargeting of natural killer-cell cytolytic activity to ErbB2-expressing cancer cells results in efficient and selective tumor cell destruction. Blood 2002; 100: 1265–1273.
Muller T, Uherek C, Maki G, Chow KU, Schimpf A, Klingemann HG et al. Expression of a CD20-specific chimeric antigen receptor enhances cytotoxic activity of NK cells and overcomes NK-resistance of lymphoma and leukemia cells. Cancer Immunol Immunother 2008; 57: 411–423.
Imai C, Iwamoto S, Campana D . Genetic modification of primary natural killer cells overcomes inhibitory signals and induces specific killing of leukemic cells. Blood 2005; 106: 376–383.
Arai S, Klingemann HG . Natural killer cells: can they be useful as adoptive immunotherapy for cancer? Expert Opin Biol Ther 2005; 5: 163–172.
Luevano M, Madrigal A, Saudemont A . Generation of natural killer cells from hematopoietic stem cells in vitro for immunotherapy. Cell Mol Immunol 2012; 9: 310–320.
Kao IT, Yao CL, Kong ZL, Wu ML, Chuang TL, Hwang SM . Generation of natural killer cells from serum-free, expanded human umbilical cord blood CD34+ cells. Stem Cells Dev 2007; 16: 1043–1051.
Spanholtz J, Tordoir M, Eissens D, Preijers F, van der Meer A, Joosten I et al. High log-scale expansion of functional human natural killer cells from umbilical cord blood CD34-positive cells for adoptive cancer immunotherapy. PLoS One 2010; 5: e9221
Spanholtz J, Preijers F, Tordoir M, Trilsbeek C, Paardekooper J, de Witte T et al. Clinical-grade generation of active NK cells from cord blood hematopoietic progenitor cells for immunotherapy using a closed-system culture process. PLoS One 2011; 6: e20740
Condiotti R, Zakai YB, Barak V, Nagler A . Ex vivo expansion of CD56+ cytotoxic cells from human umbilical cord blood. Exp Hematol 2001; 29: 104–113.
Miller JS, Alley KA, McGlave P . Differentiation of natural killer (NK) cells from human primitive marrow progenitors in a stroma-based long-term culture system: identification of a CD34+7+ NK progenitor. Blood 1994; 83: 2594–2601.
Mrozek E, Anderson P, Caligiuri MA . Role of interleukin-15 in the development of human CD56+ natural killer cells from CD34+ hematopoietic progenitor cells. Blood 1996; 87: 2632–2640.
Kaufman DS, Hanson ET, Lewis RL, Auerbach R, Thomson JA . Hematopoietic colony-forming cells derived from human embryonic stem cells. Proc Natl Acad Sci USA 2001; 98: 10716–10721.
Kaufman DS . Toward clinical therapies using hematopoietic cells derived from human pluripotent stem cells. Blood 2009; 114: 3513–3523.
Knorr DA, Kaufman DS . Pluripotent stem cell-derived natural killer cells for cancer therapy. Transl Res 2010; 156: 147–154.
Woll PS, Martin CH, Miller JS, Kaufman DS . Human embryonic stem cell-derived NK cells acquire functional receptors and cytolytic activity. J Immunol 2005; 175: 5095–5103.
Woll PS, Grzywacz B, Tian X, Marcus RK, Knorr DA, Verneris MR et al. Human embryonic stem cells differentiate into a homogeneous population of natural killer cells with potent in vivo antitumor activity. Blood 2009; 113: 6094–6101.
Berg M, Lundqvist A, McCoy P, Jr, Samsel L, Fan Y, Tawab A et al. Clinical-grade ex vivo-expanded human natural killer cells up-regulate activating receptors and death receptor ligands and have enhanced cytolytic activity against tumor cells. Cytotherapy 2009; 11: 341–355.
Fujisaki H, Kakuda H, Shimasaki N, Imai C, Ma J, Lockey T et al. Expansion of highly cytotoxic human natural killer cells for cancer cell therapy. Cancer Res 2009; 69: 4010–4017.
Siegler U, Meyer-Monard S, Jorger S, Stern M, Tichelli A, Gratwohl A et al. Good manufacturing practice-compliant cell sorting and large-scale expansion of single KIR-positive alloreactive human natural killer cells for multiple infusions to leukemia patients. Cytotherapy 2010; 12: 750–763.
Gong W, Xiao W, Hu M, Weng X, Qian L, Pan X et al. Ex vivo expansion of natural killer cells with high cytotoxicity by K562 cells modified to co-express major histocompatibility complex class I chain-related protein A, 4-1BB ligand, and interleukin-15. Tissue Antigens 2010; 76: 467–475.
Denman CJ, Senyukov VV, Somanchi SS, Phatarpekar PV, Kopp LM, Johnson JL et al. Membrane-bound IL-21 promotes sustained ex vivo proliferation of human natural killer cells. PLoS One 2012; 7: e30264
Sutlu T, Stellan B, Gilljam M, Quezada HC, Nahi H, Gahrton G et al. Clinical-grade, large-scale, feeder-free expansion of highly active human natural killer cells for adoptive immunotherapy using an automated bioreactor. Cytotherapy 2010; 12: 1044–1055.
Tam YK, Martinson JA, Doligosa K, Klingemann HG . Ex vivo expansion of the highly cytotoxic human natural killer-92 cell-line under current good manufacturing practice conditions for clinical adoptive cellular immunotherapy. Cytotherapy 2003; 5: 259–272.
Arai S, Meagher R, Swearingen M, Myint H, Rich E, Martinson J et al. Infusion of the allogeneic cell line NK-92 in patients with advanced renal cell cancer or melanoma: a phase I trial. Cytotherapy 2008; 10: 625–632.
Ruggeri L, Mancusi A, Burchielli E, Capanni M, Carotti A, Aloisi T et al. NK cell alloreactivity and allogeneic hematopoietic stem cell transplantation. Blood Cells Mol Dis 2008; 40: 84–90.
Slavin S, Ackerstein A, Or R, Shapira MY, Gesundheit B, Askenasy N et al. Immunotherapy in high-risk chemotherapy-resistant patients with metastatic solid tumors and hematological malignancies using intentionally mismatched donor lymphocytes activated with rIL-2: a phase I study. Cancer Immunol Immunother 2010; 59: 1511–1519.
Rosenberg SA, Lotze MT, Muul LM, Leitman S, Chang AE, Ettinghausen SE et al. Observations on the systemic administration of autologous lymphokine-activated killer cells and recombinant interleukin-2 to patients with metastatic cancer. N Engl J Med 1985; 313: 1485–1492.
Krause SW, Gastpar R, Andreesen R, Gross C, Ullrich H, Thonigs G et al. Treatment of colon and lung cancer patients with ex vivo heat shock protein 70-peptide-activated, autologous natural killer cells: a clinical phase i trial. Clin Cancer Res 2004; 10: 3699–3707.
Parkhurst MR, Riley JP, Dudley ME, Rosenberg SA . Adoptive transfer of autologous natural killer cells leads to high levels of circulating natural killer cells but does not mediate tumor regression. Clin Cancer Res 2011; 17: 6287–6297.
Curti A, Ruggeri L, D'Addio A, Bontadini A, Dan E, Motta MR et al. Successful transfer of alloreactive haploidentical KIR ligand-mismatched natural killer cells after infusion in elderly high risk acute myeloid leukemia patients. Blood 2011; 118: 3273–3279.
Rizzieri DA, Storms R, Chen DF, Long G, Yang Y, Nikcevich DA et al. Natural killer cell-enriched donor lymphocyte infusions from A 3-6/6 HLA matched family member following nonmyeloablative allogeneic stem cell transplantation. Biol Blood Marrow Transplant 2010; 16: 1107–1114.
Geller MA, Cooley S, Judson PL, Ghebre R, Carson LF, Argenta PA et al. A phase II study of allogeneic natural killer cell therapy to treat patients with recurrent ovarian and breast cancer. Cytotherapy 2011; 13: 98–107.
Shi FD, Ljunggren HG, la Cava A, van Kaer L . Organ-specific features of natural killer cells. Nat Rev Immunol 2011; 11: 658–671.
Subleski JJ, Wiltrout RH, Weiss JM . Application of tissue-specific NK and NKT cell activity for tumor immunotherapy. J Autoimmun 2009; 33: 275–281.
Sanchez-Correa B, Morgado S, Gayoso I, Bergua JM, Casado JG, Arcos MJ et al. Human NK cells in acute myeloid leukaemia patients: analysis of NK cell-activating receptors and their ligands. Cancer Immunol Immunother 2011; 60: 1195–1205.
Romagne F, Andre P, Spee P, Zahn S, Anfossi N, Gauthier L et al. Preclinical characterization of 1-7F9, a novel human anti-KIR receptor therapeutic antibody that augments natural killer-mediated killing of tumor cells. Blood 2009; 114: 2667–2677.
Sola C, Andre P, Lemmers C, Fuseri N, Bonnafous C, Blery M et al. Genetic and antibody-mediated reprogramming of natural killer cell missing-self recognition in vivo. Proc Natl Acad Sci USA 2009; 106: 12879–12884.
Purdy AK, Campbell KS . Natural killer cells and cancer: regulation by the killer cell Ig-like receptors (KIR). Cancer Biol Ther 2009; 8: 2211–2220.
Hayashi T, Hideshima T, Akiyama M, Podar K, Yasui H, Raje N et al. Molecular mechanisms whereby immunomodulatory drugs activate natural killer cells: clinical application. Br J Haematol 2005; 128: 192–203.
Fujii H, Trudeau JD, Teachey DT, Fish JD, Grupp SA, Schultz KR et al. In vivo control of acute lymphoblastic leukemia by immunostimulatory CpG oligonucleotides. Blood 2007; 109: 2008–2013.
Brandau S, Riemensberger J, Jacobsen M, Kemp D, Zhao W, Zhao X et al. NK cells are essential for effective BCG immunotherapy. Int J Cancer 2001; 92: 697–702.
Jha P, Golovko D, Bains S, Hostetter D, Meier R, Wendland MF et al. Monitoring of natural killer cell immunotherapy using noninvasive imaging modalities. Cancer Res 2010; 70: 6109–6113.
Kircher MF, Gambhir SS, Grimm J . Noninvasive cell-tracking methods. Nat Rev Clin Oncol 2011; 8: 677–688.
Meller B, Frohn C, Brand JM, Lauer I, Schelper LF, von Hof K et al. Monitoring of a new approach of immunotherapy with allogenic (111)In-labelled NK cells in patients with renal cell carcinoma. Eur J Nucl Med Mol Imaging 2004; 31: 403–407.
Tavri S, Jha P, Meier R, Henning TD, Muller T, Hostetter D et al. Optical imaging of cellular immunotherapy against prostate cancer. Mol Imaging 2009; 8: 15–26.
Sutton EJ, Henning TD, Pichler BJ, Bremer C, Daldrup-Link HE . Cell tracking with optical imaging. Eur Radiol 2008; 18: 2021–2032.
Pichler BJ, Kolb A, Nagele T, Schlemmer HP . PET/MRI: paving the way for the next generation of clinical multimodality imaging applications. J Nucl Med 2010; 51: 333–336.
Patel D, Kell A, Simard B, Xiang B, Lin HY, Tian G . The cell labeling efficacy, cytotoxicity and relaxivity of copper-activated MRI/PET imaging contrast agents. Biomaterials 2011; 32: 1167–1176.
Iliopoulou EG, Kountourakis P, Karamouzis MV, Doufexis D, Ardavanis A, Baxevanis CN et al. A phase I trial of adoptive transfer of allogeneic natural killer cells in patients with advanced non-small cell lung cancer. Cancer Immunol Immunother 2010; 59: 1781–1789.
Lapteva N, Durett AG, Sun J, Rollins LA, Huye LL, Fang J et al. Large-scale ex vivo expansion and characterization of natural killer cells for clinical applications. Cytotherapy 2012; 14: 1131–1143.
Deng X, Terunuma H, Nieda M, Xiao W, Nicol A . Synergistic cytotoxicity of ex vivo expanded natural killer cells in combination with monoclonal antibody drugs against cancer cells. Int Immunopharmacol 2012; 14: 593–605.
Voskens CJ, Watanabe R, Rollins S, Campana D, Hasumi K, Mann DL . Ex-vivo expanded human NK cells express activating receptors that mediate cytotoxicity of allogeneic and autologous cancer cell lines by direct recognition and antibody directed cellular cytotoxicity. J Exp Clin Cancer Res 2010; 29: 134
Sutlu T, Stellan B, Gilljam M, Quezada HC, Nahi H, Gahrton G et al. Clinical-grade, large-scale, feeder-free expansion of highly active human natural killer cells for adoptive immunotherapy using an automated bioreactor. Cytotherapy 2010; 12: 1044–1055.
Geller MA, Cooley S, Judson PL, Ghebre R, Carson LF, Argenta PA et al. A phase II study of allogeneic natural killer cell therapy to treat patients with recurrent ovarian and breast cancer. Cytotherapy 2011; 13: 98–107.
Acknowledgements
This work was supported by the National Mega Project (#2012ZX10002-014), the National Hitech Project (863 project, #2012AA020901) and the project by Department of Health of Chinese Government (#20130211).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors have declared that no competing interests exist.
Rights and permissions
About this article
Cite this article
Cheng, M., Chen, Y., Xiao, W. et al. NK cell-based immunotherapy for malignant diseases. Cell Mol Immunol 10, 230–252 (2013). https://doi.org/10.1038/cmi.2013.10
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cmi.2013.10
Keywords
This article is cited by
-
Tumor microenvironment and immune system preservation in early-stage breast cancer: routes for early recurrence after mastectomy and treatment for lobular and ductal forms of disease
BMC Immunology (2024)
-
Immune modulation in malignant pleural effusion: from microenvironment to therapeutic implications
Cancer Cell International (2024)
-
NK cells encapsulated in micro/macropore-forming hydrogels via 3D bioprinting for tumor immunotherapy
Biomaterials Research (2023)
-
Tumor-specific cholinergic CD4+ T lymphocytes guide immunosurveillance of hepatocellular carcinoma
Nature Cancer (2023)
-
PD-L1/PD-1 blockage enhanced the cytotoxicity of natural killer cell on the non-small cell lung cancer (NSCLC) by granzyme B secretion
Clinical and Translational Oncology (2023)