Abstract
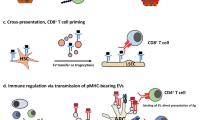
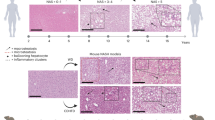
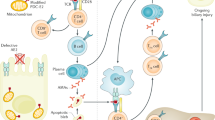
Primary biliary cirrhosis (PBC) is a chronic cholestatic liver disease for which an autoimmune pathogenesis is supported by clinical and experimental data, including the presence of autoantibodies and autoreactive T cells. The etiology remains to be determined, yet data suggest that both a susceptible genetic background and unknown environmental factors determine disease onset. Multiple infectious and chemical candidates have been proposed to trigger the disease in a genetically susceptible host, mostly by molecular mimicry. Most recently, several murine models have been reported, including genetically determined models as well as models induced by immunization with xenobiotics and bacteria.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Hirschfield GM, Heathcote EJ . Cholestasis and cholestatic syndromes. Curr Opin Gastroenterol 2009; 25: 175–179.
Kaplan MM, Gershwin ME . Primary biliary cirrhosis. N Engl J Med 2005; 353: 1261–1273.
Lleo A, Battezzati PM, Selmi C, Gershwin ME, Podda M . Is autoimmunity a matter of sex? Autoimmun Rev 2008; 7: 626–630.
Ludwig J, Dickson ER, McDonald GS . Staging of chronic nonsuppurative destructive cholangitis (syndrome of primary biliary cirrhosis). Virchows Arch A Pathol Anat Histol 1978; 379: 103–112.
Pares A, Rodes J . Natural history of primary biliary cirrhosis. Clin Liver Dis 2003; 7: 779–794.
Lee YM, Kaplan MM . The natural history of PBC: has it changed? Semin Liver Dis 2005; 25: 321–326.
Selmi C, Zuin M, Gershwin ME . The unfinished business of primary biliary cirrhosis. J Hepatol 2008; 49: 451–460.
Bouman A, Heineman MJ, Faas MM . Sex hormones and the immune response in humans. Hum Reprod Update 2005; 11: 411–423.
Gershwin ME, Selmi C, Worman HJ, Gold EB, Watnik M, Utts J, et al. Vierling, risk factors and comorbidities in primary biliary cirrhosis: a controlled interview-based study of 1032 patients. Hepatology 2005; 42: 1194–1202.
Alvaro D, Invernizzi P, Onori P, Franchitto A, de Santis A, Crosignani A, et al. Estrogen receptors in cholangiocytes and the progression of primary biliary cirrhosis. J Hepatol 2004; 41: 905–912.
Nelson JL, Furst DE, Maloney S, Gooley T, Evans PC, Smith A, et al. Microchimerism and HLA-compatible relationships of pregnancy in scleroderma. Lancet 1998; 351: 559–562.
Murata H, Nakauchi H, Sumida T . Microchimerism in Japanese women patients with systemic sclerosis. Lancet 1999; 354: 220.
Invernizzi P, de Andreis C, Sirchia SM, Battezzati PM, Zuin M, Rossella F, et al. Blood fetal microchimerism in primary biliary cirrhosis. Clin Exp Immunol 2000; 122: 418–222.
Nomura K, Sumida Y, Yoh T, Morita A, Matsumoto Y, Taji S, et al. Lack of evidence for leukocyte maternal microchimerism in primary biliary cirrhosis. World J Gastroenterol 2004; 10: 2415–2416.
Schoniger-Hekele M, Muller C, Ackermann J, Drach J, Wrba F, Penner E, et al. Lack of evidence for involvement of fetal microchimerism in pathogenesis of primary biliary cirrhosis. Dig Dis Sci 2002; 47: 1909–1914.
Corpechot C, Barbu V, Chazouilleres O, Poupon R . Fetal microchimerism in primary biliary cirrhosis. J Hepatol 2000; 33: 696–700.
Selmi C . The X in sex: how autoimmune diseases revolve around sex chromosomes. Best Pract Res Clin Rheumatol 2008; 22: 913–922.
Carrel L, Willard HF . X-inactivation profile reveals extensive variability in X-linked gene expression in females. Nature 2005; 434: 400–404.
Invernizzi P, Miozzo M, Battezzati PM, Bianchi I, Grati FR, Simoni G, et al. Frequency of monosomy X in women with primary biliary cirrhosis. Lancet 2004; 363: 533–535.
Invernizzi P, Miozzo M, Selmi C, Persani L, Battezzati PM, Zuin M, et al. X chromosome monosomy: a common mechanism for autoimmune diseases. J Immunol 2005; 175: 575–578.
Miozzo M, Selmi C, Gentilin B, Grati FR, Sirchia S, Oertelt S, et al. Preferential X chromosome loss but random inactivation characterize primary biliary cirrhosis. Hepatology 2007; 46: 456–462.
Padgett KA, Lan RY, Leung PC, Lleo A, Dawson K, Pfeiff J, et al. Primary biliary cirrhosis is associated with altered hepatic microRNA expression. J Autoimmun 2009; 32: 246–253.
Sanchez-Pernaute O, Ospelt C, Neidhart M, Gay S . Epigenetic clues to rheumatoid arthritis. J Autoimmun 2008; 30: 12–20.
Hewagama A, Richardson B . The genetics and epigenetics of autoimmune diseases. J Autoimmun 2009; 33: 3–11.
Ozbalkan Z, Bagislar S, Kiraz S, Akyerli CB, Ozer HT, Yavuz S, et al. Skewed X chromosome inactivation in blood cells of women with scleroderma. Arthritis Rheum 2005; 52: 1564–1570.
Invernizzi P, Gershwin ME . The genetics of human autoimmune disease. J Autoimmun 2009; in press.
Bach N, Schaffner F . Familial primary biliary cirrhosis. J Hepatol 1994; 20: 698–701.
Jones DE, Watt FE, Metcalf JV, Bassendine MF, James OF . Familial primary biliary cirrhosis reassessed: a geographically-based population study. J Hepatol 1999; 30: 402–407.
Lazaridis KN, Talwalkar JA . Clinical epidemiology of primary biliary cirrhosis: incidence, prevalence, and impact of therapy. J Clin Gastroenterol 2007; 41: 494–500.
Selmi C, Mayo MJ, Bach N, Ishibashi H, Invernizzi P, Gish R, et al. Primary biliary cirrhosis in monozygotic and dizygotic twins: genetics, epigenetics, and environment. Gastroenterology 2004; 127: 485–492.
Selmi C, Invernizzi P, Zuin M, Podda M, Gershwin ME . Genetics and geoepidemiology of primary biliary cirrhosis: following the footprints to disease etiology. Semin Liver Dis 2005; 25: 265–280.
Invernizzi P, Gershwin ME . The genetic basis of primary biliary cirrhosis: premises, not promises. Gastroenterology 2008; 135: 1044–1047.
Hirschfield GM, Liu X, Xu C, Lu Y, Xie G, Gu X, et al. Primary biliary cirrhosis associated with HLA, IL12A, and IL12RB2 Variants. N Engl J Med 2009; 360: 2797–2798.
van de Water J, Ishibashi H, Coppel RL, Gershwin ME . Molecular mimicry and primary biliary cirrhosis: premises not promises. Hepatology 2001; 33: 771–775.
Christen U, Hintermann E, Holdener M, von Herrath MG . Viral triggers for autoimmunity: is the ‘glass of molecular mimicry’ half full or half empty? J Autoimmun 2009; in press.
Burroughs AK, Rosenstein IJ, Epstein O, Hamilton-Miller JM, Brumfitt W, Sherlock S . Bacteriuria and primary biliary cirrhosis. Gut 1984; 25: 133–137.
Butler P, Hamilton-Miller JM, McIntyre N, Burroughs AK . Natural history of bacteriuria in women with primary biliary cirrhosis and the effect of antimicrobial therapy in symptomatic and asymptomatic groups. Gut 1995; 36: 931–934.
Parikh-Patel A, Gold EB, Worman H, Krivy KE, Gershwin ME . Risk factors for primary biliary cirrhosis in a cohort of patients from the united states. Hepatology 2001; 33: 16–21.
Selmi C, Gershwin M . Bacteria and human autoimmunity: the case of primary biliary cirrhosis. Curr Opin Rheumatol 2004; 16: 406–410.
Leung PS, Park O, Matsumura S, Ansari AA, Coppel RL, Gershwin ME . Is there a relation between Chlamydia infection and primary biliary cirrhosis? Clin Dev Immunol 2003; 10: 227–233.
Abdulkarim AS, Petrovic LM, Kim WR, Angulo P, Lloyd RV, Lindor KD . Primary biliary cirrhosis: an infectious disease caused by Chlamydia pneumoniae? J Hepatol 2004; 40: 380–384.
Selmi C, Balkwill DL, Invernizzi P, Ansari AA, Coppel RL, Podda M, et al. Patients with primary biliary cirrhosis react against a ubiquitous xenobiotic-metabolizing bacterium. Hepatology 2003; 38: 1250–1257.
Mattner J, Savage PB, Leung P, Oertelt SS, Wang V, Trivedi O, et al. Liver autoimmunity triggered by microbial activation of natural killer T cells. Cell Host Microbe 2008; 3: 304–315.
Xu L, Shen Z, Guo L, Fodera B, Keogh A, Joplin R, et al. Does a betaretrovirus infection trigger primary biliary cirrhosis? Proc Natl Acad Sci USA 2003; 100: 8454–8459
Selmi C, Ross SR, Ansari AA, Invernizzi P, Podda M, Coppel R, et al. Lack of immunological or molecular evidence for a role of mouse mammary tumor retrovirus in primary biliary cirrhosis. Gastroenterology 2004; 127: 493–501.
McDermid J, Chen M, Li Y, Wasilenko S, Bintner J, McDougall C, et al. Reverse transcriptase activity in patients with primary biliary cirrhosis and other autoimmune liver disorders. Aliment Pharmacol Ther 2007; 26: 587–595.
Selmi C, Gershwin ME . The retroviral myth of primary biliary cirrhosis: is this (finally) the end of the story? J Hepatol 2009; 50: 548–554.
Long SA, Quan C, van de Water J, Nantz MH, Kurth MJ, Barsky D, et al. Immunoreactivity of organic mimeotopes of the E2 component of pyruvate dehydrogenase: connecting xenobiotics with primary biliary cirrhosis. J Immunol 2001; 167: 2956–2963.
Scaglione BJ, Salerno E, Gala K, Pan M, Langer JA, Mostowski H, et al. Regulatory T cells as central regulators of both autoimmunity and B cell malignancy in New Zealand Black mice. J Autoimmun 2009; 32: 14–23.
Jordan MA, Baxter AG . The genetics of immunoregulatory T cells. J Autoimmun 2008; 31: 237–244.
Longhi MS, Meda F, Wang P, Samyn M, Mieli-Vergani G, Vergani D, et al. Expansion and de novo generation of potentially therapeutic regulatory T cells in patients with autoimmune hepatitis. Hepatology 2008; 47: 581–591.
Kessel A, Bamberger E, Masalha M, Toubi E . The role of T regulatory cells in human sepsis. J Autoimmun 2009; 32: 211–215.
Lan RY, Cheng C, Lian ZX, Tsuneyama K, Yang GX, Moritoki Y, et al. Liver-targeted and peripheral blood alterations of regulatory T cells in primary biliary cirrhosis. Hepatology 2006; 43: 729–737.
Gershwin ME . The mosaic of autoimmunity. Autoimmun Rev 2008; 7: 161–163.
Gershwin ME, Ansari AA, Mackay IR, Nakanuma Y, Nishio A, Rowley M, et al. Primary biliary cirrhosis: an orchestrated immune response against epithelial cells. Immunol Rev 2000; 174: 210–225.
Invernizzi P, Crosignani A, Battezzati PM, Covini G, de Valle G, Larghi A, et al. Comparison of the clinical features and clinical course of antimitochondrial antibody-positive and -negative primary biliary cirrhosis. Hepatology 1997; 25: 1090–1095.
Benson GD, Kikuchi K, Miyakawa H, Tanaka A, Watnik MR, Gershwin ME . Serial analysis of antimitochondrial antibody in patients with primary biliary cirrhosis. Clin Dev Immunol 2004; 11: 129–133.
Heathcote EJ . Management of primary biliary cirrhosis. The American Association for the Study of Liver Diseases practice guidelines. Hepatology 2000; 31: 1005–1013.
Shimoda S, Miyakawa H, Nakamura M, Ishibashi H, Kikuchi K, Kita H, et al. CD4 T-cell autoreactivity to the mitochondrial autoantigen PDC-E2 in AMA-negative primary biliary cirrhosis. J Autoimmun 2008; 31: 110–115.
Sasaki M, Ikeda H, Nakanuma Y . Activation of ATM signaling pathway is involved in oxidative stress-induced expression of mito-inhibitory p21WAF1/Cip1 in chronic non-suppurative destructive cholangitis in primary biliary cirrhosis: an immunohistochemical study. J Autoimmun 2008; 31: 73–78.
Odin JA, Huebert RC, Casciola-Rosen L, LaRusso NF, Rosen A . Bcl-2-dependent oxidation of pyruvate dehydrogenase-E2, a primary biliary cirrhosis autoantigen, during apoptosis. J Clin Invest 2001; 108: 223–232.
Allina J, Stanca CM, Garber J, Hu B, Sautes-Fridman C, Bach N, et al. Anti-CD16 autoantibodies and delayed phagocytosis of apoptotic cells in primary biliary cirrhosis. J Autoimmun 2008; 30: 238–245.
Lleo A, Selmi C, Invernizzi P, Podda M, Coppel RL, Mackay I, et al. Apotopes and the biliary specificity of primary biliary cirrhosis. Hepatology 2009; 49: 871–879.
Volkmann M, Luithle D, Zentgraf H, Schnolzer M, Fiedler S, Heid H, et al. SLA/LP/tRNP((Ser)Sec) antigen in autoimmune hepatitis: identification of the native protein in human hepatic cell extract. J Autoimmun 2009; in press.
Tiegs G, Lohse AW . Immune tolerance: what is unique about the liver. J Autoimmun 2009; in press.
Oertelt S, Rieger R, Selmi C, Invernizzi P, Ansari AA, Coppel R, et al. A sensitive bead assay for antimitochondrial antibodies: chipping away at AMA-negative primary biliary cirrhosis. Hepatology 2007; 45: 659–665.
Picha L, Pakas I, Guialis A, Moutsopoulos HM, Vlachoyiannopoulos PG . Comparative qualitative and quantitative analysis of scleroderma (systemic sclerosis) serologic immunoassays. J Autoimmun 2008; 31: 166–174.
Meroni PL . Pathogenesis of the antiphospholipid syndrome: an additional example of the mosaic of autoimmunity. J Autoimmun 2008; 30: 99–103.
Longhi MS, Ma Y, Mieli-Vergani G, Vergani D . Aetiopathogenesis of autoimmune hepatitis. J Autoimmun 2009; in press.
Gershwin ME, Mackay IR, Sturgess A, Coppel RL . Identification and specificity of a cDNA encoding the 70 kd mitochondrial antigen recognized in primary biliary cirrhosis. J Immunol 1987; 138: 3525–3531.
Selmi C, Zuin M, Bowlus CL, Gershwin ME . Anti-mitochondrial antibody-negative primary biliary cirrhosis. Clin Liver Dis 2008; 12: 173–185, ix.
Bruggraber SF, Leung PS, Amano K, Quan C, Kurth MJ, Nantz M, et al. Autoreactivity to lipoate and a conjugated form of lipoate in primary biliary cirrhosis. Gastroenterology 2003; 125: 1705–1713.
Invernizzi P, Selmi C, Ranftler C, Podda M, Wesierska-Gadek J . Antinuclear antibodies in primary biliary cirrhosis. Semin Liver Dis 2005; 25: 298–310.
Shimoda S, van de Water J, Ansari A, Nakamura M, Ishibashi H, Coppel R, et al. Identification and precursor frequency analysis of a common T cell epitope motif in mitochondrial autoantigens in primary biliary cirrhosis. J Clin Invest 1998; 102: 1831–1840.
Shimoda S, Harada K, Niiro H, Yoshizumi T, Soejima Y, Taketomi A, et al. Biliary epithelial cells and primary biliary cirrhosis: the role of liver-infiltrating mononuclear cells. Hepatology 2008; 47: 958–965.
Shimoda S, Ishikawa F, Kamihira T, Komori A, Niiro H, Baba E, et al. Autoreactive T-cell responses in primary biliary cirrhosis are proinflammatory whereas those of controls are regulatory. Gastroenterology 2006; 131: 606–618.
Shimoda S, Miyakawa H, Nakamura M, Ishibashi H, Kikuchi K, Kita H, et al. CD4 T-cell autoreactivity to the mitochondrial autoantigen PDC-E2 in AMA-negative primary biliary cirrhosis. J Autoimmun 2008; 31: 110–115.
Shimoda S, Nakamura M, Ishibashi H, Hayashida K, Niho Y . HLA DRB4 0101-restricted immunodominant T cell autoepitope of pyruvate dehydrogenase complex in primary biliary cirrhosis: evidence of molecular mimicry in human autoimmune diseases. J Exp Med 1995; 181: 1835–1845.
Shimoda S, Nakamura M, Ishibashi H, Kawano A, Kamihira T, Sakamoto N, et al. Molecular mimicry of mitochondrial and nuclear autoantigens in primary biliary cirrhosis. Gastroenterology 2003; 124: 1915–1925.
Shimoda S, Nakamura M, Shigematsu H, Tanimoto H, Gushima T, Gershwin M, et al. Mimicry peptides of human PDC-E2 163–176 peptide, the immunodominant T-cell epitope of primary biliary cirrhosis. Hepatology 2000; 31: 1212–1216.
Kita H, Naidenko OV, Kronenberg M, Ansari AA, Rogers P, He X, et al. Quantitation and phenotypic analysis of natural killer T cells in primary biliary cirrhosis using a human CD1d tetramer. Gastroenterology 2002; 123: 1031–1043.
Carambia A, Herkel J . CD4 T cells in hepatic immune tolerance. J Autoimmun 2009; in press.
Kita H, Matsumura S, He XS, Ansari AA, Lian ZX, van de Water J, et al. Quantitative and functional analysis of PDC-E2-specific autoreactive cytotoxic T lymphocytes in primary biliary cirrhosis. J Clin Invest 2002; 109: 1231–1240.
Lan RY, Salunga TL, Tsuneyama K, Lian ZX, Yang GX, Hsu W, et al. Hepatic IL-17 responses in human and murine primary biliary cirrhosis. J Autoimmun 2009; 32: 43–51.
Selmi C, Lleo A, Pasini S, Zuin M, Gershwin ME . Innate immunity and primary biliary cirrhosis. Curr Mol Med 2009; 9: 45–51.
Pares A, Caballeria L, Rodes J, Bruguera M, Rodrigo L, Garcia-Plaza A, et al. Long-term effects of ursodeoxycholic acid in primary biliary cirrhosis: results of a double-blind controlled multicentric trial. UDCA-Cooperative Group from the Spanish Association for the Study of the Liver. J Hepatol 2000; 32: 561–566.
Kikuchi K, Lian ZX, Yang GX, Ansari AA, Ikehara S, Kaplan M, Miyakawa H, Coppel RL, Gershwin ME . Bacterial CpG induces hyper-IgM production in CD27(+) memory B cells in primary biliary cirrhosis. Gastroenterology 2005; 128: 304–312.
Moritoki Y, Lian ZX, Wulff H, Yang GX, Chuang YH, Lan R, et al. AMA production in primary biliary cirrhosis is promoted by the TLR9 ligand CpG and suppressed by potassium channel blockers. Hepatology 2007; 45: 314–322.
Mao TK, Lian ZX, Selmi C, Ichiki Y, Ashwood P, Ansari A, et al. Altered monocyte responses to defined TLR ligands in patients with primary biliary cirrhosis. Hepatology 2005; 42: 802–808.
Chuang YH, Lian ZX, Yang GX, Shu SA, Moritoki Y, Ridgway W, et al. Natural killer T cells exacerbate liver injury in a transforming growth factor beta receptor II dominant-negative mouse model of primary biliary cirrhosis. Hepatology 2008; 47: 571–580.
Oertelt S, Ridgway WM, Ansari AA, Coppel RL, Gershwin ME . Murine models of primary biliary cirrhosis: comparisons and contrasts. Hepatol Res 2007; 37(Suppl 3): S365–S369.
Oertelt S, Lian ZX, Cheng CM, Chuang YH, Padgett KA, He X, et al. Anti-mitochondrial antibodies and primary biliary cirrhosis in TGF-beta receptor II dominant-negative mice. J Immunol 2006; 177: 1655–1660.
Moritoki Y, Zhang W, Tsuneyama K, Yoshida K, Wakabayashi K, Yang G, et al. B cells suppress the inflammatory response in a mouse model of primary biliary cirrhosis. Gastroenterology 2009; 136: 1037–1047.
Wakabayashi K, Lian ZX, Moritoki Y, Lan RY, Tsuneyama K, Chuang Y, et al. IL-2 receptor alpha(−/−) mice and the development of primary biliary cirrhosis. Hepatology 2006; 44: 1240–1249.
Amano K, Leung PS, Xu Q, Marik J, Quan C, Kurth M, et al. Xenobiotic-induced loss of tolerance in rabbits to the mitochondrial autoantigen of primary biliary cirrhosis is reversible. J Immunol 2004; 172: 6444–6452.
Wakabayashi K, Lian ZX, Leung PS, Moritoki Y, Tsuneyama K, Kurth M, et al. Loss of tolerance in C57BL/6 mice to the autoantigen E2 subunit of pyruvate dehydrogenase by a xenobiotic with ensuing biliary ductular disease. Hepatology 2008; 48: 531–540.
Wakabayashi K, Yoshida K, Leung PS, Moritoki Y, Yang GX, Tsuneyama K, et al. Induction of autoimmune cholangitis in non-obese diabetic (NOD).1101 mice following a chemical xenobiotic immunization. Clin Exp Immunol 2009; 155: 577–586.
Irie J, Wu Y, Wicker LS, Rainbow D, Nalesnik MA, Hirsch R, et al. NOD.c3c4 congenic mice develop autoimmune biliary disease that serologically and pathogenetically models human primary biliary cirrhosis. J Exp Med 2006; 203: 1209–1219.
Oo YH, Adams DH . The role of chemokines in the recruitment of lymphocytes to the liver. J Autoimmun 2009; in press
Fukushima N, Nalbandian G, van de Water J, White K, Ansari AA, Leung P, et al. Characterization of recombinant monoclonal IgA anti-PDC-E2 autoantibodies derived from patients with PBC. Hepatology 2002; 36: 1383–1392.
Lleo A, Selmi C, Invernizzi P, Podda M, Gershwin ME . The consequences of apoptosis in autoimmunity. J Autoimmun 2008; 31: 257–262.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Selmi, C., Meda, F., Kasangian, A. et al. Experimental evidence on the immunopathogenesis of primary biliary cirrhosis. Cell Mol Immunol 7, 1–10 (2010). https://doi.org/10.1038/cmi.2009.104
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cmi.2009.104
This article is cited by
-
Integrative bioinformatics analysis and experimental validation of key biomarkers for risk stratification in primary biliary cholangitis
Arthritis Research & Therapy (2023)
-
The latest research trends in primary biliary cholangitis: a bibliometric analysis
Clinical and Experimental Medicine (2022)
-
Liver-resident NK cells suppress autoimmune cholangitis and limit the proliferation of CD4+ T cells
Cellular & Molecular Immunology (2020)
-
Primary biliary cirrhosis associated with Graves’ disease in a male patient
Clinical Journal of Gastroenterology (2016)
-
Hair dyes as a risk for autoimmunity: from systemic lupus erythematosus to primary biliary cirrhosis
Autoimmunity Highlights (2013)