Abstract
The amyloid beta (Aβ) pathway is strongly implicated in neurodegenerative conditions such as Alzheimer’s disease and more recently, glaucoma. Here, we identify the α2 adrenergic receptor agonists (α2ARA) used to lower intraocular pressure can prevent retinal ganglion cell (RGC) death via the non-amyloidogenic Aβ-pathway. Neuroprotective effects were confirmed in vivo and in vitro in different glaucoma-related models using α2ARAs brimonidine (BMD), clonidine (Clo) and dexmedetomidine. α2ARA treatment significantly reduced RGC apoptosis in experimental-glaucoma models by 97.7% and 92.8% (BMD, P<0.01) and 98% and 92.3% (Clo, P<0.01)) at 3 and 8 weeks, respectively. A reduction was seen in an experimental Aβ-induced neurotoxicity model (67% BMD and 88.6% Clo, both P<0.01, respectively), and in vitro, where α2ARAs significantly (P<0.05) prevented cell death, under both hypoxic (CoCl2) and stress (UV) conditions. In experimental-glaucoma, BMD induced ninefold and 25-fold and 36-fold and fourfold reductions in Aβ and amyloid precursor protein (APP) levels at 3 and 8 weeks, respectively, in the RGC layer, with similar results with Clo, and in vitro with all three α2ARAs. BMD significantly increased soluble APPα (sAPPα) levels at 3 and 8 weeks (2.1 and 1.6-fold) in vivo and in vitro with the CoCl2 and UV-light insults. Furthermore, treatment of UV-insulted cells with an sAPPα antibody significantly reduced cell viability compared with BMD-treated control (52%), co-treatment (33%) and untreated control (27%). Finally, we show that α2ARAs modulate levels of laminin and MMP-9 in RGCs, potentially linked to changes in Aβ through APP processing. Together, these results provide new evidence that α2ARAs are neuroprotective through their effects on the Aβ pathway and sAPPα, which to our knowledge, is the first description. Studies have identified the need for α-secretase activators and sAPPα-mimetics in neurodegeneration; α2ARAs, already clinically available, present a promising therapy, with applications not only to reducing RGC death in glaucoma but also other neurodegenerative processes involving Aβ.
Similar content being viewed by others
Main
Glaucoma is a major cause of visual impairment worldwide and is characterised by optic neuropathy and visual field loss. Retinal ganglion cell (RGCs) apoptosis is considered an early hallmark of glaucoma1 and raised intraocular pressure (IOP) is presently the only modifiable risk factor.2 As a proportion of glaucoma patients continue to lose vision despite effective IOP control,3 IOP-independent risk factors are increasingly thought to have a role in glaucoma pathology.
Amyloid beta (Aβ), the major constituent of senile plaques in Alzheimer’s disease (AD), has recently been implicated in glaucoma pathology.4, 5 Aβ is associated with abnormal processing of amyloid precursor protein (APP). APP can be cleaved either by α-secretase via the non-amyloidogenic pathway, producing soluble APPα (sAPPα), or β-secretase producing sAPPβ, and Aβ, via the amyloidogenic pathway.6 Using rodent glaucoma models, the amyloidogenic pathway has recently been identified as a target for the development of novel neuroprotective glaucoma therapies.4, 5 Here, Aβ deposition was found to induce RGC apoptosis, a finding supported by a study on glaucoma patients reporting reduced Aβ concentrations in the vitreous.7 Aβ may therefore be important in the stress–response to glaucomatous neurodegeneration and offers a novel therapeutic target.4
Brimonidine (BMD), Clonidine (Clo) and Dexmedetomidine (Dex) are α2 adrenergic receptor agonists (α2ARAs). Apraclonidine, a para-amino derivative of Clo, is a topical α2ARA8 routinely used in the clinic to reduce IOP spikes induced by neodymium:YAG laser treatment for posterior capsule scarring after cataract surgery.9 However, the reduced activity of Apraclonidine in controlling IOP with chronic usage10 coupled with increased risk of follicular conjunctivitis,11 renders it unsuitable for long-term glaucoma management. BMD was introduced as an IOP-lowering agent; however, increasing experimental evidence suggests it also has IOP-independent neuroprotective activity.12 This was clinically demonstrated in a prospective, randomised-controlled study where BMD was reported to significantly preserve visual field in low-tension glaucoma patients compared with the beta-blocker timolol.13 Both Clo and Dex are used as anaesthetics,14 Clo is used to treat migraine, hypertension and menopausal flushing,15 and Dex for sedation during intensive care.16 In vivo studies have demonstrated Clo and BMD to have retinal neuroprotection17, 18, 19 with functional benefits,20, 21 and Dex to have neuroprotection against cerebral ischaemia,22 excitotoxicity23 as well as in a model of traumatic brain injury.24
Although α2AA and α2AB receptors have been identified in the RGC layer (RGCL) of the inner retina,25 the mechanisms by which α2A agonists exert neuroprotection are not well-established. Various pathways have been proposed, including cyclic adenosine monophosphate (cAMP) reduction,26 NMDA receptor neuromodulation,21 increasing cell survival proteins p-Akt and bcl-2 (ref. 27) and neurotrophic factor expression.22 The present study seeks to delineate the mechanisms of α2A-mediated neuroprotection using glaucoma-related in vivo and in vitro models, and investigate the involvement of the Aβ-pathway.
Results
α2ARAs are neuroprotective against retinal neuronal death in vitro and in vivo
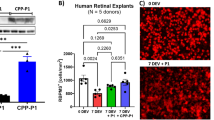
Retinal neuronal cells (RNs) were pre-treated for 24 h with BMD, Dex or Clo before insulting with the hypoxia-mimic cobalt chloride (CoCl2)28 or UV light to induce neurotoxicity, based on previously determined IC50 doses.29 CoCl2 induced a decrease in cell viability in both primary and immortalised cell types, which was significantly reduced with BMD at all concentrations assessed (0.1–100 μM, P<0.01 Figures 1a and c), whereas Clo was protective at 0.1, 1 and 100 μM (P<0.05), whereas Dex was effective at 0.01 μM (P<0.001, Figure 1a).
α2 agonists are neuroprotective against RGC death in vitro. α2 agonists’ effects on neuroprotection were investigated in vitro using the MTT assay in immortalised RNs against CoCl2 (hypoxic) and UV (stress) insults; against 250 μM CoCl2 BMD showed significant neuroprotection at all concentrations tested, Dex showed protection at 0.01 μM and Clo was neuroprotective at 0.1, 1 and 100 μM (a). Against the insult of UV, BMD was protective at 100 and 10 μM and Clo and Dex were both protective at 0.01 μM (b). The protective effects of BMD at 10 and 100 μM against CoCl2 were reproduced in mouse-derived primary mixed retinal cultures (c). In immortalised RNs, BMD (10 μM) was found to be protective against an UV-light insult of 80 j/cm2 (d). All experiments were carried out in triplicate. All means±S.E.M.; * P<0.05, **P<0.01, ***P<0.001
BMD significantly increased cell viability of UV-insulted cells at 10 and 100 μM (P<0.001, Figure 1b). Clo and Dex were neuroprotective at 0.01 μM (P<0.001 and P<0.001, respectively, Figure 1b). BMD reduced UV-induced RN death in a dose-dependent manner with an IC50 value of 64±14 μM. At a peak activity of 1 mM, BMD significantly increased cell viability against UV insult (76.1% compared with 32.2%, respectively, P<0.001, Figure 1d).
Effects of systemic α2A agonists BMD and Clo were examined in vivo using an ocular-hypertensive (OHT) rat model.30 Comparison of the IOP profile between untreated OHT control and no-OHT groups showed OHT surgery produced a significant increase in IOP up to 3 weeks post surgery (P<0.05, Figure 2a). Systemic Clo treatment lowered IOP at 1, 2 and 3 weeks compared with the untreated OHT group (all P<0.01), whereas systemic BMD had no effect on IOP (Figure 2a), as expected.31
α2 agonists are neuroprotective against RGC death in vivo. (a) Rats had IOP surgically elevated in one eye (OHT os) in an established model of ocular hypertension (OHT). IOP was significantly increased in untreated control (n=10) and systemic BMD-treated groups (n=10) compared with no-OHT (contralateral eyes), up to 3 weeks after surgery. In comparison, systemic Clo treatment significantly reduced IOP (n=10). (b) α2A agonist treatment (BMD, Clo) significantly decreased RGC apoptosis compared with untreated controls at 3 (43-fold and 50-fold reduction for BMD and Clo, respectively) and 8 (14-fold and 13-fold reduction for BMD and Clo, respectively) weeks after surgery. (c–e) Representative DARC images showing the in vivo retinal image of an untreated OHT (c) compared with BMD (d) and Clo-treated (e) rats at 3 weeks after IOP elevation. Each white spot represents an individual retinal ganglion cell undergoing apoptosis that is positive for fluorescently labelled annexin A5. (a) and (b) show means±S.E.M.; **P<0.01, ***P<0.001
Significantly, more apoptotic RGCs were observed at 3 and 8 weeks in the untreated OHT model compared with the no-OHT control eyes (P<0.01; Figure 2b), with peak RGC apoptosis occurring at 3 weeks, consistent with previous findings.1, 4 Both BMD and Clo significantly reduced RGC apoptosis compared with untreated controls at 3 weeks, by 97.7% and 98%, respectively (P<0.001), and at 8 weeks (92.8% and 92.3%, P<0.01), as shown in Figures 2b–e. No significant difference was observed between 3 and 8 weeks BMD and Clo-treated groups (P>0.05, Figures 2b–e). BMD’s anti-apoptotic effect was found to coincide with increased levels of the cell survival protein P-Bad both in vivo and ex vivo (Supplementary data). In summary, these experiments demonstrate that α2ARA reduce levels of RGC apoptosis and cell death both in vivo and in vitro.
The neuroprotective effect of α2ARAs is associated with modulation of Aβ in RNs in vitro and in vivo
Previous studies suggest that glaucoma-related RGC apoptosis involved Aβ, and its therapeutic targeting was neuroprotective.4 The interaction of α2ARAs BMD, Dex and Clo with RN-associated Aβ was investigated in vitro with CoCl2 and UV-associated cell toxicity using immunocytochemistry. Both CoCl2 and UV significantly increased Aβ levels (P<0.001, Figure 3a) by 1.5- and 2.2-fold, respectively. Treatment with α2ARA on CoCl2 insulted cells significantly decreased Aβ detected when co-treated with 10 and 100 μM BMD (P<0.01 and P<0.001, respectively), with a dose-dependent reduction in Aβ levels observed (20%(1 μM), 34.7%(10 μM) and 56.8%(100 μM), Figures 3b–d). At the same concentrations, Clo and Dex treatments were associated with reductions in Aβ staining of; Clo: 0.3, 21.4, 23.4% and Dex: 4, 33.5 and 30.8%, respectively. In all, 10 and 100 μM BMD treatment also significantly reduced APP detected, by 35.4 and 26.8% (Figures 3e–g; P<0.05). BMD treatment was more effective with lower concentrations on UV-induced Aβ, with 60.5, 64.5 and 81.4% decreases at 0.1 μM, 1 μM and 10 μM, respectively (P<0.001, Figure 3h).
α2A agonists directly reduce retinal neuronal Aβ and APP levels in different in vitrostress models. α2 agonists’ ability to reduce Aβ levels was next investigated in vitro in immortalised RNs using CoCl2 and UV insults, which significantly increased Aβ levels (a). Aβ levels were significantly reduced in CoCl2 samples when co-treated with 10 and 100 μM BMD (b). All α2A treatments were associated with a reduction in Aβ levels at concentrations of 10 and 100 μM, although BMD was found to be most effective. Representative images from CoCl2 insulted cells show BMD treatment (c) reduced Aβ (red) staining in RNs compared with CoCl2 only treatment (d); (α-tubulin staining (green), DAPI staining (blue)). APP levels were significantly reduced with 10 μM BMD treatment against CoCl2 insult (e). Representative images from CoCl2 insulted RGCs show BMD treatment (f); reduced APP (green) staining in RGCs compared with CoCl2 only treatment (g); (DAPI staining (blue)). (h) Staining for Aβ induced by UV insult revealed a significant decrease in levels with treatment of 0.1, 1 and 10 μM BMD. Experiments were carried out in triplicate. All data; means±S.E.M.; * P<0.05, **P<0.01, ***P<0.001
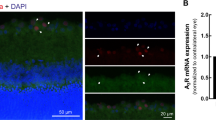
Consistent with previous in vivo findings,4 elevated levels of Aβ were observed in the RGCL 3 weeks post OHT model induction compared with no-OHT control (P<0.001, Figure 4a) associated with a significant increase in APP (P<0.001, Figure 4b).
The neuroprotective effect of α2A receptor agonists is associated with modulation of Aβ in vivo. (a) Immunohistochemistry revealed a significant increase in Aβ in OHT eyes compared with the no-OHT control at 3 weeks post IOP elevation. BMD and Clo treatment significantly reversed this effect (BMD; ninefold decrease at 3 weeks and 25-fold decrease at 8 weeks, Clo; a 3.4-fold decrease at 3 weeks). (b) APP concentrations were similarly increased at 3 weeks in comparison with the no-OHT control. BMD and Clo treatment significantly reversed this effect with a 36-fold (BMD) and eightfold (Clo) reduction in APP levels in the RGCL at 3 weeks, and a fourfold reduction (BMD and Clo) at 8 weeks. Representative images of Aβ (red), APP (green) and nuclei (DAPI, blue) labelled RGCL of a 3 weeks OHT model in the absence (c) and presence of BMD (d) and Clo treatment (e), showing increased Aβ and APP colocalisation (highlighted by red arrows) in the untreated OHT compared with α2A agonist treated eyes (d, e). (f) α2A agonist treatment significantly decreased colocalisation of Aβ and APP detected at both 3 (BMD and Clo) and 8 weeks (BMD) compared with untreated OHT eyes. (g) Assessment of Aβ neurotoxicity was performed following intravitreal injection of Aβ25–35 in vivo. Both BMD and Clo significantly reduced levels of RGC apoptosis as detected using AlexaFluor 488 labelled annexin A5 to label apoptosing RGCs. (h) Representative in vivo image of α2A agonist treated Aβ model and histologically ex vivo (i), demonstrating a reduction in annexin labelled RGCs compared with untreated Aβ model (j). In vitro experiments were carried out in triplicate. All data; means±S.E.M. * P<0.05, **P<0.01, ***P<0.001
Treatment of the OHT model with α2ARAs significantly reduced Aβ detected in the RGCL 3 weeks post IOP elevation (Figures 4a and c-e). BMD treatment was associated with a ninefold (3 weeks) and 25-fold (8 weeks) reduction in Aβ levels, whereas Clo induced a 3.4-fold (3 weeks) decrease (P<0.01 and P<0.05, respectively). A similar reduction in APP was observed in the RGCL with BMD treatment associated with a 36- (3 weeks) and a fourfold (8 weeks) reduction, and Clo an eightfold (3 weeks) and fourfold (8 weeks) reduction(P<0.01 in each case, Figures 4b–e). Furthermore, APP and Aβ showed greater colocalisation in the RGCL of the untreated OHT model (Figure 4c) compared with α2ARA-treated OHT model (Figures 4d and e); at 3 weeks (P<0.001 and P<0.01, BMD and Clo, respectively) and 8 weeks (P<0.001 BMD, Figure 4f). Although the Pearson’s coefficient values are not significantly different in the OHT and the no-OHT controls, in the OHT controls there is a decreased Aβ (Figure 4a) and APP (Figure 4b) levels, as demonstrated by the ratio between the Aβ intensity and Pearson’s coefficient value to in the no-OHT group being 5.10 compared with 28.6 in the OHT model at 3 weeks, and 8.87 at 8 weeks (Figures 4a and b). This change in colocalisation observed with α2ARA treatment is suggestive of altered processing of APP favouring the non-amyloidogenic pathway (Figure 4f), which is markedly different to the untreated no-OHT control, where less Aβ and APP was detected compared with the OHT model (Figures 4a).
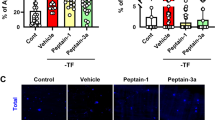
To further investigate whether α2ARA therapy acted via an Aβ-dependent pathway, α2ARAs were administered into a previously characterised in vivo Aβ-induced RGC apoptosis model.4 BMD and Clo treatment significantly reduced RGC apoptosis in response to intravitreal administration Aβ25–35 (25 nM), compared with Aβ25–35 only controls (Figures 4g–j). RGC apoptosis was reduced by 67% (BMD, P<0.01) and 88.6% (Clo, P<0.01), respectively, suggesting a direct effect of α2ARAs on Aβ-induced RGC apoptosis.
α2A agonists directly affect the non-amyloidogenic pathway and elicit neuroprotective activity through sAPPα
Having established α2ARA treatments reduce Aβ-associated-RGC apoptosis, we investigated whether these effects were mediated through changes to APP processing. Levels of sAPPα (a product of the non-amyloidogenic pathway6) were histologically assessed in the OHT model. sAPPα staining was not significantly different either at 3 or 8 weeks in the RGCL in untreated OHT and control eyes (Figure 5a). BMD treatment significantly increased sAPPα levels at both 3 and 8 weeks (2.1- and 1.6-fold increase, respectively) compared with untreated OHT controls (P<0.05 and P<0.01, Figures 5a–e). Clo treatment had no effect.
α2A agonists directly affect the non-amyloidogenic pathway and are neuroprotective through sAPPα. (a) Treatment with the α2A receptor agonist BMD significantly increased sAPPα levels at both 3 (2.1-fold) and 8 weeks (1.6-fold) compared with untreated control in the OHT model. (b–e) Representative retinal histological images of sAPPα (red) and nuclei (DAPI, labelled blue) of the RGCL of a 3 weeks (b, c) and 8 weeks. (d, e) OHT model in the absence (b, d) and presence (c, e) of BMD treatment, showing increased sAPPα staining with BMD. (f–h) sAPPα levels were significantly increased in vitro in the CoCl2 model with 10 and 100 μM BMD treatment compared with control (h). Representative images from BMD and CoCl2 treated cells (g), and CoCl2 only treated cells (f) stained for sAPPα (red), α tubulin (green), DAPI (blue), show significantly increased sAPPα staining with BMD treatment. (i) sAPPα activity was next assessed using UV light to induce RGC death; the sAPPα antibody treatment significantly inhibited the neuroprotective effects of BMD against UV, suggesting that BMD is neuroprotective through sAPPα, promoting APP processing through the non-amyloidenic pathway. in vitro experiments were carried out in triplicate. Data are means±S.E.M. *P<0.05, **P<0.01, ***P<0.001
The effect of BMD on the non-amyloidogenic pathway was confirmed in vitro using the hypoxia mimetic CoCl2 to induce RN toxicity. A twofold significant increase in sAPPα levels was observed in response to 10 μM and 100 μM BMD treatment (P<0.01, P<0.05, respectively, Figures 5f–h).
Having previously established BMD treatment reduces Aβ levels in response to UV light induced toxicity, the effect of an sAPPα antibody on UV-insulted and BMD-treated cells was investigated. Although sAPPα antibody exposure caused no significant change in RGC viability after UV exposure, it significantly inhibited protection by BMD therapy (Figure 5i). This observation, coupled with data demonstrating that α2ARA treatment significantly reduced APP levels, suggests α2ARA mediated RGC neuroprotection is achieved through increased sAPPα through upregulation of non-amyloidogenic APP processing.
The neuroprotective effect of α2ARAs via Aβ-related pathways involves modulation of the ECM
Laminin and MMP-9 expression have been implicated in Aβ-related pathways.32 The occurrence of RGC apoptosis in OHT is associated with a reduction in laminin in the RGCL at 3 months in the same OHT model.33 We therefore investigated whether extracellular matrix (ECM) modulation had a role in α2ARAs-mediated neuroprotection using the OHT model.
A twofold reduction in laminin was observed in the RGCL at 3 and 8 weeks post OHT induction compared with the no-OHT control eyes (P<0.05, Figure 6a). BMD treatment restored laminin levels in the OHT model RGCL at both 3 and 8 weeks (P<0.05, Figures 6a–e). A significant (P<0.05) twofold reduction in MMP-9 expression was observed in the RGCL 3 weeks post OHT induction but not at 8 weeks (Figures 6f–j). BMD treatment induced a marked but not statistically significant increase in MMP-9 levels at 8 weeks (Figure 6f). Laminin and MMP-9 expression was also investigated in the Aβ-inducing apoptosis model.4 BMD treatment was associated with a significant reduction in laminin deposition in the RGCL versus Aβ-treated controls, although there were no differences in comparison to the no-OHT control (unpaired t-test, P<0.05, Figure 6k).
The neuroprotective effect of α2A agonist via Aβ-related pathways involves modulation of the extracellular matrix. (a) OHT surgery induced a significant reduction in laminin levels in the RGCL at 3 weeks compared with the no-OHT control. BMD treatment significantly increased levels of laminin at 3 (2.2-fold) and 8 weeks (2.9-fold) in comparison with the respective controls. (b–e) Representative images show low levels of laminin (red) in the RGCL of a 3 (b) and 8 (d) weeks OHT eye, compared with the same time points in BMD-treated OHT eyes (c, e), (DAPI, blue). (f) MMP-9 levels in the RGCL were significantly lower at 3 weeks in OHT eyes compared with the no-OHT control. (g–j) Representative images show the marked but non-significant increase in general (pro and active forms) MMP-9 levels (green) in the RGCL of BMD-treated OHT models at 3 (h) and 8 (j) weeks compared with OHT control eyes (g, i), (DAPI, blue). (k) In comparison, a different pattern was seen in the Aβ neurotoxicity model, where BMD treatment was associated with a significant reduction in laminin in the RGCL. (l) Further assessment of MMP-9 activity was performed using zymography on immortalised RN exposed to CoCl2, where BMD treatment appeared to substantially reduce MMP-9 activity in both pro- and active forms, although this effect was reduced at a high concentration (100 μM). (m) BMD treatment did not significantly alter levels of MMP-9 in the RGCL of the Aβ apoptosis-inducing model, although levels were significantly different from no-OHT control. in vitro experiments were carried out in triplicate. Error bars±S.E.M. *P<0.05, **P<0.01, ***P<0.001
To further investigate the effect of α2ARAs on MMP-9 expression, in vitro studies were performed on RNs insulted with CoCl2. Using zymography, CoCl2 increased both pro- and active MMP-9 (Figure 6h, lane 2), compared with untreated cells (lane 1). Treatment with BMD reduced both pro- and active MMP-9 (Figure 6l). A marked but not statistically significant reduction in MMP-9 was observed histologically in the in vivo Aβ-induced apoptosis model, although in the Aβ-treated eyes, the MMP-9 staining was significantly lower than in the no-OHT controls (P<0.001, Figure 6m). These results suggest that α2ARA modulate laminin and MMP-9 expression in RGCs, which may be linked to changes in Aβ and APP processing.
Discussion
The present study confirms the neuroprotective actions of α2ARAs using in vivo and in vitro models of retinal neurodegeneration with a novel IOP-independent mechanism of action. This mechanism proposes that a reduction in RGC apoptosis is achieved through reduced Aβ production, and its precursor APP, via stimulation of the non-amyloidogenic pathway as evidenced by a significant increase in sAPPα, which leads to modification of ECM proteins laminin and MMP-9 (Figure 7).
Diagram representing α2A agonists’ neuroprotective effect against Aβ toxicity. APP can be processed into Aβ or sAPPα through the amyloidogenic and non-amyloidogenic pathways, respectively. α2A receptor agonists can negatively affect the amyloidogenic pathway, preventing cell death, partly by modulating excitotoxicity caused by glutamate (GLU). α2A receptor agonists can also affect APP processing via the extracellular matrix, by modulating MMP-9 and laminin through LBP, preventing further toxic interactions with Aβ and by increasing processing of APP into sAPPα, promoting the non-amyloidogenic pathway. α2A receptor agonists can also increase levels of P-Bad, and therefore overall act to promote cell survival and neuroprotection
Compared with Clo, systemic BMD administration does not affect IOP,31, 34 suggesting that BMD’s neuroprotective effect is IOP independent. This observation is supported by the LoGTs study,13 where BMD was effective in preserving visual field independent of IOP reduction in adults with low-pressure glaucoma. Further investigations of the clinical use of BMD as a neuroprotectant are currently underway (clinicaltrials.gov NCT00658619, NCT00693485, NCT01229410). Furthermore, the ability of BMD to improve visual function is documented in rodent models of retinal disease.35, 36, 37
This study suggests that different activity levels between α2ARAs could be attributed to differences in their selectivity for the α2A and the α2AA subtype. BMD and Dex are direct agonists of the α2AA receptor subtype, and are inhibited by the α2AA antagonist yohimbine in vivo27 and in vitro.38 In comparison, Clo has reduced selectivity for α2 receptors.8,17, 39 Neuroprotective effects α2ARAs are understood to be primarily mediated though α2A receptors,11 supporting BMD’s effects in this study. α2A receptors are G-protein-coupled-receptors whose activation leads to an inhibition of adenylate cyclase and a decrease in cAMP.40 cAMP is implicated in Aβ modulation by stimulation of APP synthesis and processing, affecting the amyloidogenic and non-amyloidogenic pathways,41, 42 potentially through the cAMP/PKA/APP/Aβ pathway.43
Several mechanisms have been proposed for α2A-mediated neuroprotection, including increased expression of neurotrophic factors.17, 22, 27, 44, 45, 46 Other survival pathways include P-Akt, bcl-2 and extracellular signal-regulated kinase (ERK),27, 47 which support this study’s observed increase in P-Bad(Ser136). α2A agonists have also been reported to effect the glutamate pathway,48 with reductions in intracellular cAMP production and cytosolic calcium shown in RGCs.21 Recently, BMD was reported to reduce expression of NMDA subunits NR1 and NR2A in a model of ischaemia.19 Similar activity in excitotoxicity models is reported for Clo17, 49 and Dex50 in the CNS.
Elevated APP and Aβ have been reported in glaucoma models,4, 51 potentially linking elevated IOP promotion of APP processing, and inhibition of APP anterograde transport from the RGCL to the optic nerve.51, 52 BMD is reported to preserve optic nerve axons and active transport throughout the visual pathway in a rodent OHT model,18 which may explain the present study’s finding where α2A agonists reduced levels of APP and Aβ in the RCGL of the OHT model. This hypothesis is supported by our in vitro data, where CoCl2 and UV-induced elevation of APP and Aβ was inhibited by α2ARAs. A possible pathway by which this may occur is through α2ARAs’ ability to inhibit cAMP production.21
This study suggests for the first time that the neuroprotective effects of α2ARA BMD are directly associated with increased sAPPα, as the observed BMD-mediated neuroprotective effect was reversed using an sAPPα antibody in vitro. Furthermore, the increase in sAPPα appears to be specific to α2AA activity, as Clo did not produce a comparable effect.11 Previously, sAPPα was reported to be neuroprotective in vitro.53,29 More recently, Obregon et al. reported that sAPPα decreases Aβ generation directly by associating with the β-site APP-converting enzyme (BACE1) both in vivo and in vitro. Importantly, the authors proposed that the levels of sAPPα were so crucial that an imbalance could stimulate amyloidogenic APP processing,54 concluding that sAPPα mimetics are a potential therapeutic target for the treatment of AD. This was further highlighted in a recent paper by Willem where unwanted side-effects on neuronal activity were implicated by treatment with BACE1.55 The results of the present study suggest that α2AA agonists are sAPPα modulators, promoting RGC survival in a non-IOP-dependent manner.
A mechanism for the stimulation of sAPPα by α2A agonists may be through the activation of α-secretases, which can occur via protein kinase C (PKC), phosphatidylinositol 3-kinase (PI3K) and mitogen-activated protein kinase–ERK.56 Evidence suggests that APP cleavage by the α-secretase ADAM10 (a disintegrin and metalloproteinase and physiological α-secretase in neurons) constitutively produces sAPPα through 5-HT4 receptors in a cAMP-independent pathway. When stimulated by 5-HT4 receptors agonists, however, sAPPα secretion is mediated through cAMP/Epac (exchange protein activated by cAMP) signalling.57 A possible explanation for this study’s findings is that α2ARAs could directly activate α-secretase ADAM10 and sAPPα production through cAMP/Epac modulation.
ADAM10 and MMP-9 have been reported to stimulate sAPPα production and decrease Aβ, through α-secretase-like activity.58, 59 We present in vitro data suggesting that α2ARAs increase levels of pro-MMP-9 and sAPPα, whereas decreasing Aβ levels. This concurs with in vivo studies where elevated MMP-9 levels in a AβPP transgenic mouse model led to a reduced plaque burden and increased sAPPα levels.60 As both ADAM10 and MMP-9 are matrix metalloproteases, their activity levels may be similar.61, 62 In the retina, NMDA activation is reported to increase MMP-9 activity;63 α2A agonists could therefore reduce MMP-9 activity by inhibiting retinal excitotoxicity.21 Furthermore, MMP-9 is reported to be influenced by Aβ, as intracerebroventricularly injected Aβ is reported to increase MMP-9 levels in vivo.63 The reduction in Aβ levels by α2ARAs observed may be responsible for the reported reduction in active MMP-9 levels. The effects of α2ARAs on MMP-9 appear complex and closely related: α2A agonists may reduce active MMP-9 levels through modulation of NMDA and Aβ activity, but this reduction in MMP-9 may in-turn decrease its α-secretase-like activity and the subsequent promotion of the non-amyloidogenic pathway.
MMP-9 activity in retinal neurodegeneration is linked with laminin, it was reported that RGC degeneration is associated with reduced laminin and stimulation of MMP-9.33 We report similar changes in laminin in the RGCL of the OHT model, but at earlier time points than previously described. Laminin is suggested to be neuroprotective through a laminin-integrin signalling pathway, with evidence that laminin promotes RGC survival in vitro through β1 integrin-focal adhesion kinase signalling.64 The reduction in laminin reported in this study was reversed by α2A agonist BMD treatment. BMD has been reported to induce laminin binding protein expression, laminin-induced neuronal and axonal changes, essential for promoting axonal preservation and growth.65
Furthermore, laminin is linked to modification of APP and Aβ processing and found in senile plaques in Alzheimer’s Disease,66 where it prevents Aβ fibril formation and reduces neurotoxicity.32 This effect was confirmed in vivo, with laminin depletion accelerating Aβ-induced neurotoxicity, altering the distribution of Aβ aggregates in Caenorhabditis elegans.67 Intravitreal injection of Aβ25–35 was found to induce increased laminin in the RGCL, which was reversed by BMD treatment, contradictory to the effect of BMD treatment observed in the OHT model. The increase in laminin observed in the Aβ25–35 model may be a response to direct Aβ-induced neurotoxicity.32, 67 The reduction of Aβ-induced neurotoxicity with BMD treatment may result in an attenuation of the increased laminin levels in response to the acute presence of Aβ. This hypothesis is supported by the observation that BMD reduces levels of Aβ deposition in both the OHT and Aβ models in vivo, inhibiting Aβ neurotoxicity and RGC apoptosis.
In addition to modulating Aβ levels through sAPPα, this study confirms that α2A agonist BMD can elicit neuroprotection through P-Bad (Ser136) (Supplementary Figure1a–d). Aβ is reported to increase Bad de-phosphorylation and cell death by stimulating calmodulin–calcineurin activity.68 BMD-mediated reduction of Aβ may increase P-Bad, promoting cell survival pathways involving PI3K, known to be upregulated by BMD upstream of P-Bad.27 PI3K activity can itself decrease Aβ levels,69 providing further corroboration that BMD reduces Aβ. In addition, upstream of Bad, PKC activation simultaneously increases sAPPα and reduces Aβ levels, providing further support for non-amyloidogenic promotion of cell survival.70
An alternative and complementary pathway by which α2A agonists reduce Aβ expression in OHT, may be via oxidative stress modulation.26 Oxidative stress reduces expression of sAPPα and α-secretase activity71 and is implicated in the pathogenesis of glaucoma, where an ischaemic element is well-recognised.72 The observation that BMD increases sAPPα and reduces Aβ levels in RGCs when exposed to a hypoxic insult (CoCl2) supports evidence for α2A agonist’s neuroprotective activity under oxidative stress. Although Aβ1-42 monomers may possess neuroprotective function,6 Aβ oligomers and Aβ25–35 used in this study are widely reported to induce oxidative stress.4 The effects of α2A agonists against oxidative stress are supported by our observation that BMD and Clo are protective against Aβ25–35-induced RGC apoptosis in vivo.
Aβ neurotoxicity is associated with glutamate NMDA receptor activation and is the basis of the FDA-approved NMDA receptor antagonist Memantine for the treatment of Alzheimer’s Disease.73 This pathway has also been implicated in the development of Aβ induced-dendritic spine loss and tau-associated neurodegeneration.74 Short-term NMDA receptor stimulation is reported to increase non-amyloidogenic α-secretase-mediated APP processing and sAPPα production,75 whereas chronic stimulation is reported to have the opposite effect.76 α2ARAs can also modulate NMDA receptors; Dong et al. report that BMD acts post-synaptically on NMDA receptors by reducing levels of intracellular cAMP; this indirect effect could also be responsible for BMD suppressing Aβ-induced excitotoxicity.21 Clo has been shown to regulate GABAergic synaptic inputs in the CNS, which could explain its neuroprotective effect reported in this study in the OHT model.49
In conclusion, we confirm that α2ARAs are neuroprotective of RGC death in vivo and in vitro, substantiating previous reports that this effect is non-IOP dependent. We suggest a new mechanism by which this occurs; we show through multiple modalities that α2ARAs modulate Aβ toxicity, decreasing levels of Aβ and APP in vivo and in vitro, and increasing sAPPα formation through the non-amyloidogenic pathway (Figure 7). We specifically demonstrate that neuroprotective effects of α2ARA BMD are mediated through sAPPα. Furthermore, BMD affects laminin, in association with Aβ, which influences RGC survival. Recent studies have identified the need for α-secretase activators and sAPPα-mimetics in neurodegeneration. We propose that α2ARAs may be the most commonly available clinical sAPPα modulators, and being 'tried and tested' may offer an economical advantage as a pre-existing therapeutic for neuroprotection. The applications of α2ARAs may therefore not be limited to reducing RGC death in glaucoma but also to any neurodegenerative process where Aβ neurotoxicity is involved, such as AD. This work strongly advocates investigation of the therapeutic potential of α2ARAs in these disorders.
Materials and Methods
Ethics statement
All procedures were approved by the UK Home Office and the University College London Ethics Committee and were conducted in accordance with the Association for Research in Vision and Ophthalmology statement and ARRIVE guidelines.
Animals
Adult male Dark Agouti rats (200–250 g) (n=50) were maintained in a 12-hour light/12-hour dark cycle, and provided standard food and water ad libitum. Animals were anaesthetised by intraperitoneal administration of ketamine (37.5%) (Ketaset; Fort Dodge Animal Health) and medetomidine (25%) (Dormitor; Pfizer, Exton, PA, USA) at 2 ml/kg, except for IOP measurements, for which animals were anaesthetised by 0.4% isoflurane in oxygen.
Chemicals
BMD was purchased from Sigma Aldrich (Dorset, UK), or obtained from Allergan (Oregon, USA); Clo and Dex were purchased from Santa Cruz Biotechnology Inc (Santa Cruz, CA, USA).
Rat model of OHT
The OHT model was surgically induced in 30 rats using a well-established method.30 IOP was elevated in the left eye of each animal by injection of 50 μl hypertonic saline (1.80 M) into the episcleral veins using a syringe pump (UMP2, World Precision Instruments, Sarasota, FL, USA). A propylene ring, with a 1 mm gap cut out of its circumference, was placed around the equator to prevent saline outflow from other aqueous veins, as described previously.4, 33 Contralateral, un-operated eyes served as controls. The IOP of both eyes was measured in mmHg at regular intervals using a Tonolab Tonometer (Tiolat Oy, Heisinki, Finland). Treatments of BMD (n=10), Clo (n=10) and PBS control (n=10) were administered intraperitoneally at the time of surgery. Animals were imaged for RGC apoptosis by administrating Alexa-488-labelled annexin A5 (1.25 μg in 5 μl) intravitreally at 3 (n=15) and 8 (n=15) weeks, before being killed for histological assessment.1, 33 The ratio of IOP was calculated by dividing the IOP from the operated, OHT left eye (OS) by that of the un-operated, no-OHT right eye (OD). Analysts were masked to treatment group identity. Statistical analysis on IOP data was carried out using the non-parametric two-tailed Mann–Whitney test comparing treated OHT to untreated no-OHT control (n=5).
Rat model of Aβ
The Aβ model was prepared in 15 rats to induce RGC apoptosis as described previously.4 In brief, 25nmol Aβ25–35 (Sigma Aldrich) was dissolved in sterile water and intravitreally administered unilaterally. BMD (n=5) Clo (n=5) or vehicle (PBS) (n=5) was administered intraperitoneally at the time of Aβ administration. Rats were imaged for RGC apoptosis (as described above) at baseline and 3 days following treatments before sacrifice.
Histology and immunohistochemistry
RGC apoptosis counts were performed in vivo and histologically ex vivo, using whole-retina mounts.4 For whole-retina mounts, eyes were enucleated and immediately fixed in 4% paraformaldehyde following termination. Eyes were dissected at the equator, and the cornea, lens and vitreous were removed. RGC apoptosis was identified by fluorescent annexin A5 staining. RGC apoptosis density counts were performed in a masked fashion by three observers, and were calculated as previously described.4, 77
Immunohistochemistry was performed using antibodies listed in Table 1. Dissected eyes were fixed in 10% formalin before processing in methanol solutions with increasing concentrations, and embedding in paraffin.33 In total, 3 μm thick sections were then cut and incubated with antibodies diluted in TBTA (Table 1). Stained sections were analysed using fluorescent microscopy (Zeiss Axiovert S100) at x20 magnification, by a masked observer. The RGCL was segmented using a box of fixed proportions and image background noise was subtracted using a 25 pixel rolling ball radius, before recording the mean fluorescence intensity through the pixels’ grey values using ImageJ software (NIH) as previously described.78 Colocalisation analysis was carried out using the Pearson’s Coefficient test with the ImageJ JaCoP plugin79 on segmented double-labelled RGCL images.
Cell culture
Both primary murine retinal mixed neuronal cultures and an immortalised retinal neuronal (RN) cell line (a gift from Dr. Neeraj Agarwal, Department of Cell Biology and Genetics, UNT Health Science Centre, Fort Worth, TX, USA) were used. The immortalised line expresses retinal neuronal proteins Thy-1, Brn-3a and β3 tubulin80 and strong similarity to the 661w photoreceptor cell line.81 Immortalised cells were cultured in Dulbecco’s modified Eagle’s medium (DMEM; Sigma, Gillingham, UK), supplemented with 10% heat-inactivated fetal bovine serum (Life Technologies, Paisley, UK), 100 μg/ml penicillin and 100 mg/ml streptomycin (Life Technologies). Primary murine (C57BL/6) mixed retinal cultures were isolated from P0 pups and neuronal cells isolated by incubation in a solution containing 10 units of papain/ml, and cultured in DMEM with 25 mM HEPES supplemented with 5% FCS, 15 mM KCl, x0.75 Penicillin/Streptovidin/glutamine (Gibco, Paisley, UK) and serum extender (BD Biosciences, Oxford, UK).
Cell viability studies
The neuroprotective effects of α2 agonists were assessed in vitro using either the MTT or the alamarblue cell viability assays. In brief, RN were seeded at a density of 3 × 103 cells/well in a 96-well plate and cultured for 24 h (37 °C, 5% CO2) before incubation with specified concentrations of BMD prepared from a 24 mM stock solution in DMSO, Clo and Dex for 24 h. Cells were insulted with predetermined (IC50) concentrations of CoCl2 or UV-B light for 24 h. Cell viability was assessed using MTT assay, where cells were treated with 0.5 mg/ml MTT in culture media for 2 h before dissolving the resulting formazan crystals using DMSO (0.1 ml/well) and measuring absorbance (Safire microplate reader) at 570 nm. For the alamarblue viability assay, 10 μl of alamarblue solution was added per 100 μl DMEM and incubated for 1.5 h measuring absorbance (Safire microplate reader) at 570nm. All experiments were carried out in triplicate.
Assessment of secreted MMP-9 activity by zymography
RNs were cultured to 70–80% confluence before pretreatment with BMD and insulting with 250 μM CoCl2 for 24 h. Conditioned media was collected in the presence of protease cocktail inhibitors (Merck, Millipore, Nottingham, UK), and concentrated using centrifugal filters with a MWCO of 10kDa. Total protein concentration was determined using a BCA assay kit (Thermo Scientific, Rockford, IL, USA) according to manufacturer’s instructions. Conditioned media containing 20 μg of protein per sample was run on a 10% SDS gel containing 0.1% gelatin (Sigma) at 180 V for 1 h rtp. SDS was removed by two 45 min washes in 2.5% PBS-Triton, followed by incubation in developing buffer (Invitrogen, Paisley, UK) overnight at 37 °C. Gels were stained with Coomassie blue to reveal clear bands indicating the presence of secreted pro- and active MMP-9.82
Immunocytochemistry
Immunocytochemistry was performed to elucidate mechanisms of α2 agonist-associated neuroprotection. RNs were seeded on glass coverslips before pre-treating with BMD, Clo or Dex for 24 h and insulted with 250 μM CoCl2 or UV-B light (80 j/cm2) for a further 24 h. Cells were fixed in 4% paraformaldehyde before permeabilizing with 0.1% PBS-Triton and blocking with 3% BSA. Cells were incubated overnight in either anti-P-Bad (Ser136), anti-sAPPα, anti-APP or anti-Aβ with anti-α Tubulin (Cell Signalling Technology, Beverly, MA, USA) to visualise cell structure. Antibodies were diluted 1:100 in 3% BSA, except anti-α Tubulin (1:50) (Table 1). Fluorescence microscopy and analysis was performed as described previously. All experiments were carried out in triplicate.
Experimental design
Sample size estimation for the OHT study was based on the size of 'neuroprotective' effects of BMD in glaucoma patients in preserving visual field in the LoGTs study.13 This effect was 90.9%, and based on a power of 0.85 and alpha of 5%, this provided a minimum number of four animals per group per time point. OHT rats were randomly assigned in blocks of three to treatment with either BMD or Clo (n=5 at 3 weeks and n=5 at 8 weeks), or vehicle (PBS, n=10). For the Aβ model, samples size was based on our previous published results.4 Ex vivo analyses were planned with five rats per group, but owing to one death and one atrophic retina, a final number of three to five rats per group were used, as sample material was limited. Animals were randomly assigned in blocks of three to treatment, as above. All in vitro experiments were carried out in triplicate.
Statistical analysis
Unless otherwise stated all statistical tests comprise a one-way ANOVA with either Dunnett’s or Tukey’s post-tests, with P<0.05 taken as statistical significance.
References
Cordeiro MF, Guo L, Luong V, Harding G, Wang W, Jones HE et al. Real-time imaging of single nerve cell apoptosis in retinal neurodegeneration. Proc Natl Acad Sci USA 2004; 101: 13352–13356.
Quigley HA, Broman AT . The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 2006; 90: 262–267.
Collaborative Normal-Tension Glaucoma Study. Comparison of glaucomatous progression between untreated patients with normal-tension glaucoma and patients with therapeutically reduced intraocular pressures. Collaborative Normal-Tension Glaucoma Study Group. Am J Ophthalmol 1998; 126: 487–497.
Guo L, Salt TE, Luong V, Wood N, Cheung W, Maass A et al. Targeting amyloid-beta in glaucoma treatment. Proc Natl Acad Sci USA 2007; 104: 13444–13449.
Goldblum D, Kipfer-Kauer A, Sarra G-M, Wolf S, Frueh BE . Distribution of amyloid precursor protein and amyloid-beta immunoreactivity in DBA/2J glaucomatous mouse retinas. Invest Ophthalmol Vis Sci 2007; 48: 5085–5090.
Chasseigneaux S, Allinquant B . Functions of Aβ, sAPPα and sAPPβ: similarities and differences. J Neurochem 2012; 120: 99–108.
Yoneda S, Hara H, Hirata A, Fukushima M, Inomata Y, Tanihara H . Vitreous fluid levels of beta-amyloid(1-42) and tau in patients with retinal diseases. Jpn J Ophthalmol 2005; 49: 106–108.
Burke J, Schwartz M . Preclinical evaluation of brimonidine. Surv Ophthalmol 1996; 41: S9–18.
Chen TC . Brimonidine 0.15% versus apraclonidine 0.5% for prevention of intraocular pressure elevation after anterior segment laser surgery. J Cataract Refract Surg 2005; 31: 1707–1712.
Chung HS, Shin DH, Birt CM, Kim C, Lee D, Levin DS et al. Chronic use of apraclonidine decreases its moderation of post-laser intraocular pressure spikes. Ophthalmology 1997; 104: 1921–1925.
Arthur S, Cantor LB . Update on the role of alpha-agonists in glaucoma management. Exp Eye Res 2011; 93: 271–283.
Cantor LB . The evolving pharmacotherapeutic profile of brimonidine, an alpha 2-adrenergic agonist, after four years of continuous use. Expert Opin Pharmacother 2000; 1: 815–834.
Krupin T, Liebmann JM, Greenfield DS, Ritch R, Gardiner S . A randomized trial of brimonidine versus timolol in preserving visual function: results from the Low-Pressure Glaucoma Treatment Study. Am J Ophthalmol 2011; 151: 671–681.
Mantz J, Josserand J, Hamada S . Dexmedetomidine: new insights. Eur J Anaesthesiol 2011; 28: 3–6.
JOINT FORMULARY COMMITTEE. Joint Formulary Committee. British National Formulary (online) London: BMJ Group and Pharmaceutical Press http://www.medicinescomplete.com (accessed on 10 September 2016). British National Formulary. 2016 (cited 2016 September 10). Available from http://www.evidence.nhs.uk/formulary/bnf/current/4-central-nervous-system/47-analgesics/474-antimigraine-drugs/4742-prophylaxis-of-migraine/clonidine-hydrochloride.
JOINT FORMULARY COMMITTEE. Joint Formulary Committee. British National Formulary (online) London: BMJ Group and Pharmaceutical Press http://www.medicinescomplete.com (accessed on 10 September 2016). British National Formulary. 2016 (cited 2016 September 10). Available from http://www.evidence.nhs.uk/formulary/bnf/current/15-anaesthesia/151-general-anaesthesia/1514-sedative-and-analgesic-peri-operative-drugs/15144-other-drugs-for-sedation/dexmedetomidine.
Chao HM, Chidlow G, Melena J, Wood JP, Osborne NN . An investigation into the potential mechanisms underlying the neuroprotective effect of clonidine in the retina. Brain Res 2000; 877: 47–57.
Lambert WS, Ruiz L, Crish SD, Wheeler LA, Calkins DJ . Brimonidine prevents axonal and somatic degeneration of retinal ganglion cell neurons. Mol Neurodegener 2011; 6: 4.
Lee D, Kim K-Y, Noh YH, Chai S, Lindsey JD, Ellisman MH et al. Brimonidine blocks glutamate excitotoxicity-induced oxidative stress and preserves mitochondrial transcription factor a in ischemic retinal injury. PLoS One 2012; 7: e47098.
Chao HM, Osborne NN . Topically applied clonidine protects the rat retina from ischaemia/reperfusion by stimulating alpha(2)-adrenoceptors and not by an action on imidazoline receptors. Brain Res 2001; 904: 126–136.
Dong C-J, Guo Y, Agey P, Wheeler L, Hare WA . Alpha2 adrenergic modulation of NMDA receptor function as a major mechanism of RGC protection in experimental glaucoma and retinal excitotoxicity. Invest Ophthalmol Vis Sci 2008; 49: 4515–4522.
Degos V, Charpentier T, Le, Chhor V, Brissaud O, Lebon S, Schwendimann L et al. Neuroprotective effects of dexmedetomidine against glutamate agonist-induced neuronal cell death are related to increased astrocyte brain-derived neurotrophic factor expression. Anesthesiology 2013; 118: 1123–1132.
Maier C, Steinberg GK, Sun GH, Zhi GT, Maze M . Neuroprotection by the alpha 2-adrenoreceptor agonist dexmedetomidine in a focal model of cerebral ischemia. Anesthesiology 1993; 79: 306–312.
Schoeler M, Loetscher PD, Rossaint R, Fahlenkamp A V, Eberhardt G, Rex S et al. Dexmedetomidine is neuroprotective in an in vitro model for traumatic brain injury. BMC Neurol BioMed Central Ltd 2012; 12: 20.
Woldemussie E, Wijono M, Pow D . Localization of alpha 2 receptors in ocular tissues. Vis Neurosci 2007; 24: 745–756.
Lee KYC, Nakayama M, Aihara M, Chen Y-N, Araie M . Brimonidine is neuroprotective against glutamate-induced neurotoxicity, oxidative stress, and hypoxia in purified rat retinal ganglion cells. Mol Vis 2010; 16: 246–251.
Lai RK, Chun T, Hasson D, Lee S, Mehrbod F, Wheeler L . Alpha-2 adrenoceptor agonist protects retinal function after acute retinal ischemic injury in the rat. Vis Neurosci 2002; 19: 175–185.
Tulsawani R, Kelly LS, Fatma N, Chhunchha B, Kubo E, Kumar A et al. Neuroprotective effect of peroxiredoxin 6 against hypoxia-induced retinal ganglion cell damage. BMC Neurosci 2010; 11: 125.
Copanaki E, Chang S, Vlachos A, Tschäpe J-A, Müller UC, Kögel D et al. sAPPalpha antagonizes dendritic degeneration and neuron death triggered by proteasomal stress. Mol Cell Neurosci 2010; 44: 386–393.
Morrison JC, Moore CG, Deppmeier LM, Gold BG, Meshul CK, Johnson EC . A rat model of chronic pressure-induced optic nerve damage. Exp Eye Res 1997; 64: 85–96.
Weigert G, Resch H, Luksch A, Reitsamer Ha, Fuchsjager-Mayrl G, Schmetterer L et al. Intravenous administration of clonidine reduces intraocular pressure and alters ocular blood flow. Br J Ophthalmol 2007; 91: 1354–1358.
Morgan C, Bugueño MP, Garrido J, Inestrosa NC . Laminin affects polymerization, depolymerization and neurotoxicity of Abeta peptide. Peptides 2002; 23: 1229–1240.
Guo L, Moss SE, Alexander RA, Ali RR, Fitzke FW, Cordeiro MF . Retinal ganglion cell apoptosis in glaucoma is related to intraocular pressure and IOP-induced effects on extracellular matrix. Invest Ophthalmol Vis Sci 2005; 46: 175–182.
Hernández M, Urcola JH, Vecino E . Retinal ganglion cell neuroprotection in a rat model of glaucoma following brimonidine, latanoprost or combined treatments. Exp Eye Res 2008; 86: 798–806.
Ferencz JR, Gilady G, Harel O, Belkin M, Assia EI . Topical brimonidine reduces collateral damage caused by laser photocoagulation for choroidal neovascularization. Graefes Arch Clin Exp Ophthalmol 2005; 243: 877–880.
Evans DW, Hosking SL, Gherghel D, Bartlett JD . Contrast sensitivity improves after brimonidine therapy in primary open angle glaucoma: a case for neuroprotection. Br J Ophthalmol 2003; 87: 1463–1465.
Gandolfi SA, Sangermani C, Cimino L, Ungaro N, Tardini M, Viswanathan A et al. Is there a non-IOP related effect of brimonidine on visual field progression in human glaucoma? Invest Ophthalmol Vis Sci 2004; 45 ARVO E-Abstract 2298.
Ma D, Hossain M, Rajakumaraswamy N, Arshad M, Sanders RD, Franks NP et al. Dexmedetomidine produces its neuroprotective effect via the alpha 2A-adrenoceptor subtype. Eur J Pharmacol 2004; 502: 87–97.
Virtanen R, Savola JM, Saano V, Nyman L . Characterization of the selectivity, specificity and potency of medetomidine as an alpha 2-adrenoceptor agonist. Eur J Pharmacol 1988; 150: 9–14.
Maze M, Tranquilli W . Alpha-2 adrenoceptor agonists: defining the role in clinical anesthesia. Anesthesiology 1991; 74: 581–605.
Kumar a, La Rosa FG, Hovland a R, Cole WC, Edwards-Prasad J, Prasad KN . Adenosine 3’,5’-cyclic monophosphate increases processing of amyloid precursor protein (APP) to beta-amyloid in neuroblastoma cells without changing APP levels or expression of APP mRNA. Neurochem Res 1999; 24: 1209–1215.
Canepa E, Domenicotti C, Marengo B, Passalacqua M, Marinari UM, Pronzato M a et al. Cyclic adenosine monophosphate as an endogenous modulator of the amyloid-β precursor protein metabolism. IUBMB Life 2013; 65: 127–133.
Ricciarelli R, Puzzo D, Bruno O, Canepa E, Gardella E, Rivera D et al. A novel mechanism for cyclic adenosine monophosphate-mediated memory formation: Role of amyloid beta. Ann Neurol 2014; 75: 602–607.
Patel NJ, Chen MJ, Russo-Neustadt A a . Norepinephrine and nitric oxide promote cell survival signaling in hippocampal neurons. Eur J Pharmacol 2010; 633: 1–9.
Lönngren U, Näpänkangas U, Lafuente M, Mayor S, Lindqvist N, Vidal-Sanz M et al. The growth factor response in ischemic rat retina and superior colliculus after brimonidine pre-treatment. Brain Res Bull 2006; 71: 208–218.
Wen R, Cheng T, Li Y, Cao W, Steinberg RH . Alpha 2-adrenergic agonists induce basic fibroblast growth factor expression in photoreceptors in vivo and ameliorate light damage. J Neurosci 1996; 16: 5986–5992.
Kim HS, Chang YI, Kim JH, Park CK . Alteration of retinal intrinsic survival signal and effect of alpha2-adrenergic receptor agonist in the retina of the chronic ocular hypertension rat. Vis Neurosci 2007; 24: 127–139.
Donello JE, Padillo EU, Webster ML, Wheeler LA, Gil DW . alpha(2)-Adrenoceptor agonists inhibit vitreal glutamate and aspartate accumulation and preserve retinal function after transient ischemia. J Pharmacol Exp Ther 2001; 296: 216–223.
Li D-P, Atnip LM, Chen S-R, Pan H-L . Regulation of synaptic inputs to paraventricular-spinal output neurons by alpha2 adrenergic receptors. J Neurophysiol 2005; 93: 393–402.
Jolkkonen J, Puurunen K, Koistinaho J, Kauppinen R, Haapalinna A, Nieminen L et al. Neuroprotection by the alpha2-adrenoceptor agonist, dexmedetomidine, in rat focal cerebral ischemia. Eur J Pharmacol 1999; 372: 31–36.
McKinnon SJ, Lehman DM, Kerrigan-Baumrind LA, Merges CA, Pease ME, Kerrigan DF et al. Caspase activation and amyloid precursor protein cleavage in rat ocular hypertension. Invest Ophthalmol Vis Sci 2002; 43: 1077–1087.
Morin PJ, Abraham CR, Amaratunga A, Johnson RJ, Huber G, Sandell JH et al. Amyloid precursor protein is synthesized by retinal ganglion cells, rapidly transported to the optic nerve plasma membrane and nerve terminals, and metabolized. J Neurochem 1993; 61: 464–473.
Mattson MP, Cheng B, Culwell AR, Esch FS, Lieberburg I, Rydel RE . Evidence for excitoprotective and intraneuronal calcium-regulating roles for secreted forms of the beta-amyloid precursor protein. Neuron 1993; 10: 243–254.
Obregon D, Hou H, Deng J, Giunta B, Tian J, Darlington D et al. Soluble amyloid precursor protein-α modulates β-secretase activity and amyloid-β generation. Nat Commun 2012; 3: 777.
Willem M, Tahirovic S, Busche MA, Ovsepian S V, Chafai M, Kootar S et al. η-Secretase processing of APP inhibits neuronal activity in the hippocampus. Nature 2015; 526: 443–447.
Thathiah A, De Strooper B . The role of G protein-coupled receptors in the pathology of Alzheimer’s disease. Nat Rev Neurosci 2011; 12: 73–87.
Cochet M, Donneger R, Cassier E, Gaven F, Lichtenthaler SF, Marin P et al. 5-HT4 receptors constitutively promote the non-amyloidogenic pathway of APP cleavage and interact with ADAM10. ACS Chem Neurosci 2013; 4: 130–140.
Postina R . Activation of α-secretase cleavage. J Neurochem 2012; 120: 46–54.
Talamagas AA, Efthimiopoulos S, Tsilibary EC, Figueiredo-Pereira ME, Tzinia AK . Abeta(1-40)-induced secretion of matrix metalloproteinase-9 results in sAPPalpha release by association with cell surface APP. Neurobiol Dis 2007; 28: 304–315.
Hashimoto G, Sakurai M, Teich AF, Saeed F, Aziz F, Arancio O . 5-HT4 receptor stimulation leads to soluble AβPPα production through MMP-9 upregulation. J Alzheimers Dis 2012; 32: 437–445.
Geng L, Wang W, Chen Y, Cao J, Lu L, Chen Q et al. Elevation of ADAM10, ADAM17, MMP-2 and MMP-9 expression with media degeneration features CaCl2-induced thoracic aortic aneurysm in a rat model. Exp Mol Pathol 2010; 89: 72–81.
Kim YH, Jung JC . Suppression of tunicamycin-induced CD44v6 ectodomain shedding and apoptosis is correlated with temporal expression patterns of active ADAM10, MMP-9 and MMP-13 proteins in Caki-2 renal carcinoma cells. Oncol Rep 2012; 28: 1869–1874.
Mizoguchi H, Takuma K, Fukuzaki E, Ibi D, Someya E, Akazawa K et al. Matrix metalloprotease-9 inhibition improves amyloid beta-mediated cognitive impairment and neurotoxicity in mice. J Pharmacol Exp Ther 2009; 331: 14–22.
Santos ARC, Corredor RG, Obeso BA, Trakhtenberg EF, Wang Y, Ponmattam J et al. β1 integrin-focal adhesion kinase (FAK) signaling modulates retinal ganglion cell (RGC) survival. PLoS One 2012; 7: e48332.
Prokosch V, Panagis L, Volk GF, Dermon C, Thanos S . Alpha2-adrenergic receptors and their core involvement in the process of axonal growth in retinal explants. Invest Ophthalmol Vis Sci 2010; 51: 6688–6699.
Murtomäki S, Risteli J, Risteli L, Koivisto UM, Johansson S, Liesi P . Laminin and its neurite outgrowth-promoting domain in the brain in Alzheimer’s disease and Down’s syndrome patients. J Neurosci Res 1992; 32: 261–273.
Jensen LT, Møller TH, Larsen SA, Jakobsen H, Olsen A . A new role for laminins as modulators of protein toxicity in Caenorhabditis elegans. Aging Cell 2012; 11: 82–92.
Reese LC, Zhang W, Dineley KT, Kayed R, Taglialatela G . Selective induction of calcineurin activity and signaling by oligomeric amyloid beta. Aging Cell 2008; 7: 824–835.
Lee K-Y, Koh S-H, Noh MY, Kim SH, Lee YJ . Phosphatidylinositol-3-kinase activation blocks amyloid beta-induced neurotoxicity. Toxicology 2008; 243: 43–50.
Yang H-Q, Pan J, Ba M-W, Sun Z-K, Ma G-Z, Lu G-Q et al. New protein kinase C activator regulates amyloid precursor protein processing in vitro by increasing alpha-secretase activity. Eur J Neurosci 2007; 26: 381–391.
Quiroz-Baez R, Rojas E, Arias C . Oxidative stress promotes JNK-dependent amyloidogenic processing of normally expressed human APP by differential modification of alpha-, beta- and gamma-secretase expression. Neurochem Int 2009; 55: 662–670.
Tezel G . The immune response in glaucoma: a perspective on the roles of oxidative stress. Exp Eye Res 2011; 93: 178–186.
Danysz W, Parsons CG . Alzheimer’s disease, β-amyloid, glutamate, NMDA receptors and memantine—searching for the connections. Br J Pharmacol 2012; 167: 324–352.
Tackenberg C, Grinschgl S, Trutzel A, Santuccione a C, Frey MC, Konietzko U et al. NMDA receptor subunit composition determines beta-amyloid-induced neurodegeneration and synaptic loss. Cell Death Dis 2013; 4: e608.
Hoey SE, Williams RJ, Perkinton MS . Synaptic NMDA receptor activation stimulates alpha-secretase amyloid precursor protein processing and inhibits amyloid-beta production. J Neurosci 2009; 29: 4442–4460.
Lesné S, Ali C, Gabriel C, Croci N, MacKenzie ET, Glabe CG et al. NMDA receptor activation inhibits alpha-secretase and promotes neuronal amyloid-beta production. J Neurosci 2005; 25: 9367–9377.
Salt TE, Nizari S, Cordeiro MF, Russ H, Danysz W . Effect of the Aβ aggregation modulator MRZ-99030 on retinal damage in an animal model of glaucoma. Neurotox Res 2014; 26: 440–446.
Hoh Kam J, Lenassi E, Jeffery G . Viewing ageing eyes: diverse sites of amyloid Beta accumulation in the ageing mouse retina and the up-regulation of macrophages. PLoS One 2010; 5: e13127.
Cordeiro M, Guo L, Coxon K, Duggan J . Realtime imaging of retinal ganglion cell apoptosis. Eur Ophthalmic Rev 2010; 4: 88–91.
Galvao J, Davis B, Tilley M, Normando E, Duchen MR, Cordeiro MF . Unexpected low-dose toxicity of the universal solvent DMSO. FASEB J 2014; 28: 1317–1330.
Van Bergen NJ, Wood JPM, Chidlow G, Trounce I a, Casson RJ, Ju W-K et al. Recharacterization of the RGC-5 retinal ganglion cell line. Invest Ophthalmol Vis Sci 2009; 50: 4267–4272.
Guo L, Hussain AA, Limb GA, Marshall J . Age-dependent variation in metalloproteinase activity of isolated human Bruch’s membrane and choroid. Invest Ophthalmol Vis Sci 1999; 40: 2676–2682.
Acknowledgements
We would like to thank Ali Hussein, William Cheung and David Lara for their kind expert technical assistance. MFC, LG and BMD are funded through Wellcome Trust; additional funding was received from UCL PoC and through an unrestricted research grant from Allergan as a contribution towards some in vivo work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Professor MF Cordeiro holds a patent regarding DARC technology. The remaining authors declare no conflict of interest.
Additional information
Edited by A Verkhratsky
Supplementary Information accompanies this paper on Cell Death and Disease website
Supplementary information
Rights and permissions
Cell Death and Disease is an open-access journal published by Nature Publishing Group. This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Nizari, S., Guo, L., Davis, B. et al. Non-amyloidogenic effects of α2 adrenergic agonists: implications for brimonidine-mediated neuroprotection. Cell Death Dis 7, e2514 (2016). https://doi.org/10.1038/cddis.2016.397
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2016.397
This article is cited by
-
Crocetin confers neuroprotection and is anti-inflammatory in rats with induced glaucoma
Molecular Biology Reports (2023)
-
Polydopamine nanoparticles attenuate retina ganglion cell degeneration and restore visual function after optic nerve injury
Journal of Nanobiotechnology (2021)
-
The evaluation of short- and long-term stability studies for brimonidine in aqueous humor by DPV/BDDE method—possible application for direct assay in native samples
Analytical and Bioanalytical Chemistry (2019)