Abstract
T-cell exhaustion was originally identified during chronic infection in mice, and was subsequently observed in humans with cancer. The exhausted T cells in the tumor microenvironment show overexpressed inhibitory receptors, decreased effector cytokine production and cytolytic activity, leading to the failure of cancer elimination. Restoring exhausted T cells represents an inspiring strategy for cancer treatment, which has yielded promising results and become a significant breakthrough in the cancer immunotherapy. In this review, we overview the updated understanding on the exhausted T cells in cancer and their potential regulatory mechanisms and discuss current therapeutic interventions targeting exhausted T cells in clinical trials.
Similar content being viewed by others
Facts
-
T-cell exhaustion is a hyporesponsive state of T cells in chronic environment, with increased inhibitory receptors, decreased effector cytokines and impaired cytotoxicity.
-
Most T cells in tumor microenvironment are exhausted, leading to cancer immune evasion.
-
PD-1 is the major inhibitory receptor regulating T-cell exhaustion, T cells with high PD-1 expression lose the ability to eliminate cancer.
-
Reversing T-cell exhaustion represents an inspiring strategy to treat cancer.
Open Questions
-
What is the definition of ‘exhausted T cell’?
-
What is the differentiation process of T cells in tumor microenvironment?
-
How does tumor microenvironment regulate T-cell exhaustion?
-
Reversing T-cell exhaustion represents promising cancer therapy, what are the limitations and adverse reactions? How to improve treatment efficiency?
-
What should be further studied about T-cell exhaustion?
-
What are the similarities and differences between T-cell exhaustion in chronic infection and T-cell exhaustion in cancer?
T cells are the major force of adaptive immunity. Following exposure to foreign antigens, naive T cells (CD44lowCD62Lhi) activate and expand greatly during the first 1–2 weeks. Subsequently, T cells acquire effector functions, including the production of effector cytokines and granzyme/perforin-mediated cytotoxicity. After the peak of T-cell proliferation, 90–95% of effector T cells (CD44hiCD62low) die via apoptosis. The surviving T cells differentiate into memory T cells and are maintained in the resting state.1 The memory T-cell differentiation is observed in most cases of acute inflammation.2 Upon re-exposure to the same or similar antigens, memory T cells expand more quickly and regain higher effector function than naive T cells.3, 4 These capacities allow memory T cells to persist and to confer protective immunity for a long time, even after the antigen withdraws.
In contrast, tumor antigens are weakly immunogenic self-molecules, and most tumor-specific T cells are of low precursor frequencies and low T-cell receptor (TCR) affinity because tumor-specific T cells with high avidity are deleted during the thymic selection process.2 In addition, the process of antigen presentation is impaired in tumor microenvironment (TME), leading to insufficient priming and boosting of T cells.5 Although effector T cells enter TME, they are regulated by a complex immunosuppressive network that consists of cancer cells, inflammatory cells, stromal cells and cytokines. Among these TME components, cancer cells, inflammatory cells and suppressive cytokines have crucial roles in regulating T-cell phenotype and function. These components drive T cells terminally to differentiate into ‘exhausted’ T cells.5
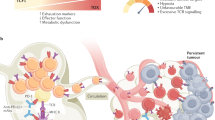
Exhausted T cells were primarily identified in a chronic lymphocytic choriomeningitis virus (LCMV) infection model. The LCMV-specific CD8+T cells expressing activation markers (CD69hiCD44hiCD62Llow) were unable to perform the anti-viral functions.6 T-cell exhaustion is a state of T-cell dysfunction in chronic environment, exhausted T cells express high levels of inhibitory receptors, including programmed cell death protein 1 (PD-1), lymphocyte activation gene 3 protein (LAG-3), T-cell immunoglobulin domain and mucin domain protein 3 (TIM-3), cytotoxic T lymphocyte antigen-4 (CTLA-4), band T lymphocyte attenuator (BTLA) and T-cell immunoglobulin and immunoreceptor tyrosine-based inhibitory motif domain (TIGIT).7, 8, 9, 10, 11, 12 The other principal characteristic of exhausted T cells is the loss of function in a hierarchical manner. Such functions as interleukin-2 (IL-2) production and ex vivo killing capacity are lost at the early stage of exhaustion,13 whereas tumor necrosis factor-α (TNF-α) production is lost at the intermediate stage, interferon-γ (IFN-γ) and granzyme B (GzmB) production are lost at the advanced stage of exhaustion.14 The first evidence connecting exhausted T cells with TME was that overexpressed programmed cell death 1 ligand 1 (PD-L1, the ligand of PD-1) on mouse mastocytoma P815 cells rendered them less susceptible to the specific TCR-mediated lysis by cytotoxic T cells in vitro and remarkably enhanced their tumorigenesis and invasiveness in vivo, which indicates that the expression of PD-L1 contributes to immune evasion.15 Most T cells in TME differentiate into exhausted T cells, express high levels of inhibitory receptors and produce less effector cytokines, and lose the ability to eliminate cancer. T-cell exhaustion may be related with defective memory T cells formation, and the final stage of T-cell exhaustion is the physical deletion, by which severely exhausted T cells are cleared in TME (Figure 1).
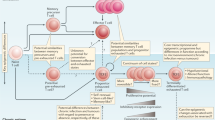
T-cell exhaustion and differentiation in TME. Naive T cells (CD44lowCD62Lhi) activate and differentiate into effector T cells (CD44hiCD62Llow) in secondary lymphoid organ. When effector T cells enter TME, they are polarized into exhausted T cells, with decrease in effector cytokines (IL-2/IFN-γ/TNF-α/GzmB) and increase in inhibitory receptors (PD-1/CTLA-4/TIM-3/LAG-3//BTLA/TIGIT). Subsequently exhausted T cells may turn to be defective memory T cells or be deleted physically
In this review, we discuss the potential mechanisms involved in T-cell exhaustion in TME. We also introduce the therapeutic interventions that target exhausted T cells in clinical trials.
Intrinsic Mechanisms Involving in T-Cell Exhaustion and Differentiation in TME
Complete activation of T cells requires three signals, the first signal is the interaction of antigenic peptide–MHC complex with TCR, the second signal is costimulatory or co-inhibitory signal provided by antigen-presenting cells, the third signal is the stimulation by extracellular cytokines such as IL-2.16 Among these signals, the second signal determines the promotion or inhibition of T-cell cytokine production and effector function, appropriate co-inhibitory signals dampen inflammation to avoid tissue damage from excessive immune reaction, whereas durative and overmuch co-inhibitory signals lead to T-cell hyporesponsiveness.17 Co-inhibitory signals are primarily mediated by inhibitory receptors that are the major phenotypes of exhausted T cells.18 Genomic studies on exhausted T cells in chronic LCMV infection defined specific molecular pathways distinct from effector T cells and memory T cells, primarily including increased inhibitory receptors and decreased cytokine signaling pathways, and so on.19 Consistent with chronic infection, T cells in TME also exhibit exhausted phenotype and function. Exhausted T cells in cancer express high levels of inhibitory receptors, including PD-1, CTLA-4, TIM-3, LAG-3, BTLA and TIGIT, as well as show impaired effector cytokine production, such as IL-2, TNF-α, IFN-γ and GzmB (Figure 1).
PD-1 expression was markedly upregulated on tumor-infiltrating CD8+ T cells and correlated with reduced cytokines in Hodgkin’s lymphoma, melanoma, hepatocellular carcinoma and gastric cancer patients.20, 21, 22, 23, 24 PD-1 expression on Jurkat cells increased after co-cultured with cancer cells, blockade of PD-1 pathway successfully restored T-cell function.25 CTLA-4 is an immune checkpoint receptor expressed only on T cells, and it competes with the costimulatory molecule CD28 in binding the ligands CD80/CD86 and initiating intracellular inhibitory signals.26 The interaction of CTLA-4 with CD80/CD86 generates inhibitory effects on T-cell activation and IL-2 production.27 One-third to half of CD8+ tumor-infiltrating lymphocytes (TILs) co-expressed PD-1 and CTLA-4, PD-1+CTLA-4+CD8+TILs were more severely exhausted in proliferation and cytokine production, whereas dual blockade of PD-1 and CTLA-4 enhanced T-cell function in cancer.28 Both PD-1 and CTLA-4 inhibited the activity of Akt, a crucial molecular in regulating glucose metabolism of T cells by elevating glucose transporter 1 expression and glycolysis, suggesting that glucose metabolism may contribute to T-cell exhaustion.29 In addition, TIM-3, LAG-3, BTLA and TIGIT also regulate T-cell exhaustion in cancer, which has been demonstrated in both animal experiments and cancer patients below.
In tumor-bearing animal models, co-expression of PD-1/TIM-3 was generally observed on TILs, among these cells, TIM-3+PD-1+CD8+TILs represented the predominant subset and exhibited greater exhausted phenotypes than TIM-3-PD-1- and TIM-3+PD-1-CD8+TILs, as defined by failure to proliferate and produce IL-2, TNF-α and IFN-γ, dual blockade of PD-1 and TIM-3 restored the anti-tumor function of exhausted CD8+T cells.30 In melanoma patients, TIM-3+PD-1+tumor-specific CD8+T cells were more dysfunctional than TIM-3-PD-1+ and TIM-3-PD-1-T cells, producing less IFN-γ, TNF-α and IL-2.31 Co-expression of PD-1/LAG-3 was also observed on CD8+TILs in tumor-bearing animal models, PD-1+LAG-3+TILs exhibited more exhausted phenotype and function than single positive or negative TILs, dual blockade of PD-1 and LAG-3 resulted in tumor regression.32 Similarly, LAG-3+PD-1+CD8+T cells were more dysfunctional in IFN-γ and TNF-α production compared with LAG-3+PD-1- or LAG-3-PD-1-CD8+subsets in human ovarian cancer.33 BTLA mediated the functional inhibition of CD8+T cells by its ligand herpes virus entry mediator,34 BTLA+PD-1+TIM-3+CD8+T cells were most dysfunctional among NY-ESO-1-specific CD8+T cells in melanoma patients. Combined blockade of BTLA, PD-1 and TIM-3 enhanced the proliferation and function of tumor-specific CD8+T cells, suggesting a role for BTLA in regulating T-cell exhaustion in advanced melanoma.11 Recently, another co-inhibitory receptor TIGIT was demonstrated in T-cell exhaustion. Similar with CTLA-4/CD28 and CD80/CD86, TIGIT competes with CD226 in binding the same set of ligands CD115/CD112, CD226 is a costimulatory signal for T-cell response, whereas TIGIT is a negative regulator.12, 35 Tumor antigen-specific CD8+T cells and CD8+TILs from melanoma patients expressed high levels of TIGIT, and TIGIT+CD8+T cells also co-expressed PD-1, combined blockade TIGIT with PD-1 promoted CD8+T cell proliferation and cytokine production.36 In tumor-bearing mouse, TIGIT was also highly expressed on TILs, antibody co-blockade of TIGIT and PD-L1 synergistically and specifically boosted CD8+T cell effector function, resulting remarkable tumor clearance.37 Above results suggest that PD-1 is the major regulator of T-cell exhaustion, in addition, the pattern of inhibitory receptor co-expression on the same CD8+T cell probably determines the severity of T-cell exhaustion, combined blockade inhibitory receptors represents inspiring strategies for cancer therapy.
The transcription factors Blimp-1, T-bet, NFATc1 and BATF are critical for T-cell exhaustion in chronic infection,38, 39, 40, 41 but the intracellular signal pathway involved in regulation of exhausted T cells in cancer remains poorly understood. PD-1 was elevated markedly in tumor-infiltrating T cells of Hodgkin’s lymphoma. Blockade of the PD-1 signaling pathway inhibited the phosphorylation of SHP-2, a SH2-containing tyrosine-specific protein phosphatase, and restored the IFN-γ-producing function, indicating that SHP-2 phosphorylation is involved in the PD-1 downstream intracellular signal transduction (Figure 2).20
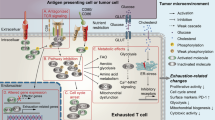
Potential regulatory mechanisms of T-cell exhaustion in TME. Cancer cells and stromal cells (tumor-associated DC, Treg, TAM and MDSC) are major extrinsic cells that regulate T-cell exhaustion, and IL-10 and TGF-β are both important extrinsic cytokines involved in exhausted process of T cells. Inhibitory receptors PD-1, CTLA-4, Tim-3, BTLA, LAG-3 and TIGIT on T cells are the major intrinsic regulatory factors of T-cell exhaustion. SHP-2 is the downstream of PD-1, IRF-9 and AP-1, which regulate PD-1 expression in transcriptional level
In addition, IFN-α induces and maintains PD-1 expression on the TCR-engaged primary mouse T cells through the association between IFN-responsive factor 9 and the IFN stimulation response element, suggesting the role of IFN-responsive factor 9 on regulating T-cell exhaustion.42 The tumor-infiltrating T cells exhibit upregulated expression of activator protein 1 (AP-1) subunit c-Fos. The ectopic expression of c-Fos in T cells promote tumor progression by inducing PD-1 expression via direct binding to the AP-1-binding site in the Pdcd1 (gene encoding PD-1) promoter, indicating that c-Fos directly regulates T-cell exhaustion in cancer (Figure 2).43
Exhausted T cells express low levels of CD122 (the β-chain of the IL-2 and IL-15 receptor) and CD127 (the IL-7 receptor α-chain) in chronic infection so that they lose the ability to survive long-term without antigens via IL-7- and IL-15-mediated memory maintenance.13 Although T cells with exhausted phenotype transferred into naive mice regained the ability to proliferate and control viral infection,44 it was also demonstrated that exhausted T cells hardly recovered normal differentiation of memory T cells in antigen-free recipients in infection models.45 These findings suggest that simply removing the antigen cannot restart normal memory T-cell differentiation. The effects of T-cell exhaustion on memory T-cell formation have also been demonstrated in TME. In tumor-bearing mouse models, TILs are divided into three subsets, namely, PD-1+TIM-3+, PD-1-TIM-3+ and PD-1-TIM-3- T cells. TIM-3+PD-1+T cells contain the largest population of effector/memory T cells with a high expression of CD44 and low expression of CD62L, but consist of the lowest population of central memory (CD44hiCD62Lhi) cells. The majority of the three TIL subsets express low to intermediate levels of CD44, whereas the CD44int cells are the lowest in TIM-3+PD-1+T cells.30 Owing to these results, we speculate that exhausted T cells in TME favor the differentiation of effector/memory T cells instead of central memory T cells, through which the long-term maintenance of anti-tumor immunity is impaired (Figure 1).
T-cell exhaustion is related to physical T-cell deletion in cancer. PD-L1 is highly expressed in various tumor tissues, and the expression of PD-L1 inversely correlates with prognosis and survival. PD-L1-associated T-cell apoptosis is one of several potential mechanisms, which is supported by the inverse correlation between PD-L1 expression in tumor tissues and the number of TILs.46 In hepatocellular carcinoma patients, immunohistochemical staining indicated that PD-L1 expressed hepatoma cells and apoptotic infiltrating CD8+T cells were both enriched in tumor sections. IFN-γ secreted by CD8+T cells induced PD-L1 expression on hepatoma cells, which in turn promoted CD8+T cell apoptosis in vitro.47 Hepatic stellate cells isolated from hematocellular carcinoma expressed high levels of PD-L1, which was associated with enhanced T-cell apoptosis.48 These findings suggest that the advanced stage of T-cell exhaustion is the physical deletion (Figure 1).
It is worth mentioning that PD-1/TIM-3 or PD-1/LAG-3 co-expression on CD4+ TILs were also observed in a recurrent mouse melanoma model.30, 32 These tumor-specific CD4+T cells expressed inhibitory receptors, such as PD-1, TIM-3 and LAG-3.49 However, whether the function of tumor-infiltrating CD4+T cells is decreased or whether these cells are also exhausted remains unknown.
Extrinsic Mechanisms Regulating T-Cell Exhaustion in Cancer
TME consists of cancer cells, inflammatory cells, stromal cells and cytokines, these components form a complicated immunosuppressive network in cancer, which limits T-cell activation and induces T-cell dysfunction. The potential extrinsic factors involved in T-cell exhaustion in cancer include tumor cells, inflammatory cells and immunosuppressive cytokines (Figure 2).
TME is abundant with tumor antigens. Chronic tumor antigens induce durative activation of T cells in TME, which probably contribute to T-cell exhaustion. The expression of PD-L1 and programmed cell death 1 ligand 2 (PD-L2) is correlated with prognosis in some human malignancies50, 51, 52, 53, 54, 55, 56, 57, 58, 59, 60, 61, 62 (Table 1). The PD-L1/PD-1 signaling pathway is a crucial regulatory pathway of T-cell exhaustion in cancer. PD-L1 is abundantly expressed in cancer cells and stromal cells, and blockade of PD-L1/PD-1 enhances T-cell anti-tumor function.63 PD-L2 also binds to PD-1 and regulates T-cell function. The constitutive basal expression of PD-L2 is low, but PD-L2 expression can be induced on dendritic cells (DCs), macrophages and mast cells in response to IL-4 and IFN.64
Regulatory T (Treg) cells are an inhibitory subset of CD4+ T cells that maintain peripheral tolerance and prevent autoimmune diseases. Tregs also accumulate in tumor tissues and the peripheral blood of cancer patients and contribute to immune evasion.65, 66 The ectoenzymes CD39 and CD73 on Treg cells have been demonstrated to mediate the generation of pericellular adenosine, which suppressed the function of effector T cells by activating the adenosine A2A receptor.67, 68 High expression of CD25 on Tregs consumed excessive local IL-2, thereby impaired T-cell function.69, 70 In addition, inhibitory cytokines derived from Tregs, such as IL-10 and transforming growth factor β (TGF-β), also suppress the function of effector T cells.71, 72
DCs are a subset of professional antigen-presenting cells. Plasmacytoid DCs generated during cancer development can induce Treg differentiation via indoleamine 2,3-dioxygenase (IDO). The increased Tregs secreted IL-10 and significantly upregulated PD-L1 on conventional DCs.73 In the transgenic adenocarcinoma of the mouse prostate model, a population of DC with plasmacytoid phenotype was observed in TME. These tumor-associated DCs expressed low levels of the costimulatory ligands CD80, CD86 and CD40 but high levels of genes associated with T-cell exhaustion, including PD-L1 and IDO.74 These data indicate that plasmacytoid DCs also contribute to T-cell exhaustion.
Macrophages are critical cells in the innate immunity that defend the host against foreign pathogens. They are generally classified into two extreme phenotypes: M1 macrophages produce considerable pro-inflammatory cytokines, whereas M2 macrophages secrete several growth factors that activate the process of tissue repair and suppress adaptive immune responses.75 Macrophages accumulated in cancer are termed tumor-associated macrophages (TAMs).75 Tumor-derived signals such as M-CSF, CCL2, VEGF and angiopoietin-2 recruit blood monocytes through the tumor vessels and promote the polarization of macrophages in cancer sites.76, 77 TAMs exhibit an M2-like phenotype and possess pro-tumor immunity. Therefore, the correlation between TAM density and the patient’s prognosis is negative.78 The overexpression of CCL2 by murine fibrosarcoma cells resulted in an increase in TAMs numbers, which contributed to tumor growth in vivo.79 TAMs suppressed T-cell activation and proliferation by producing suppressive mediators, including IL-10 and TGF-β. In addition, TAMs were unable to trigger Th1-polarized immune responses rather than induce Treg formation.80 The TAMs from renal cell carcinoma patients induced the skewing of autologous blood-derived CD4+T cells toward a more exhausted phenotype, with decreased production of effector cytokines and enhanced expression of PD-1 and TIM-3.81
The accumulation of myeloid-derived suppressor cells (MDSCs) has been recognized as a major mechanism to promote carcinogenesis. These cells originate from myeloid tissue and are comprised of myeloid cell progenitors, precursors of DCs, monocytes, macrophages and granulocytes.82 They are typically CD11b+CD33+CD34+CD14-HLA-DR- cells in cancer patients, and are CD11b+Gr-1+ cells in tumor-bearing mice. MDSCs are further divided into ‘monocytic’ (CD11b+Ly6GlowLy6Chi) and ‘granulocytic/neutrophil-like’ (CD11b+Ly6GhiLy6Clow) MDSCs.83 They are considered to be a population of inhibitory cells because they suppress T-cell activation and induce T-cell exhaustion by multiple mechanisms. For example, in ovarian carcinoma animal models, CD11b+Gr-1+cells with a high expression of PD-L1 and CD80 markedly inhibited antigen-specific immune responses, whereas blockade of PD-L1 and CD80 in Gr-1+CD11b+cells abrogated immune suppression.84, 85 MDSCs derived from IL-10-stimulated DCs exhibited enhanced PD-L1 expression, and these cells induced T-cell dysfunction via the PD-L1/PD-1 signaling pathway.86 These results uncover the role of MDSCs in regulating T-cell exhaustion in cancer.
Immunosuppressive cytokines, such as TGF-β and IL-10, are crucial factors during T-cell exhaustion. TGF-β in TME is mainly secreted by cancer cells, immune cells and fibroblasts.87 The role of the TGF-β signaling pathway in cancer is complex and paradoxical, varying by cell type and the stage of cancer. In general, TGF-β mediates tumor suppression via the inhibition of cancer cell proliferation and the induction of cancer cell apoptosis in early stages. It also promotes tumor cell invasion and metastasis through the modulation of immune response in later stages.88 Recent research has shown that TGF-β directly suppresses the cytotoxicity of CTLs by the transcriptional repression of genes encoding key functional cytokines, such as perforin, granzymes and cytotoxins.72, 89 Tumor-derived TGF-β directly suppressed CTL effector function by elevating miR-23a and downregulating Blimp-1, a key transcription factor involved in T-cell differentiation.90 In addition, the naive T cells treated with TGF-β favor the differentiation into Treg cells, which are involved in the T-cell exhaustion.91
Elevated IL-10 in TME is primarily secreted by TAMs, CD4+regulatory T cells and cancer cells.80, 92 IL-10 can exert anti-tumor activity through NK-mediated tumor cell lysis induced by downregulation of MHC-I. On the other hand, IL-10 also dampened anti-tumor immunity via an immunosuppressive role on DCs and macrophages.93 IL-10 induced PD-L1 expression on DCs, which in turn mediated the exhaustion process of T cells.86 Moreover, IL-10 has a significant role in the induction of Tregs.94 These findings demonstrate that IL-10 contributes to T-cell exhaustion in TME.
Therapeutic Interventions by Reversing Exhausted T Cells in Cancer
Research from bench to bedside indicates that the blockade of inhibitory receptors is a great breakthrough in cancer therapy. The blocking antibodies in clinical development primarily include CTLA-4 and PD-1/PD-L1 antibodies. Ipilimumab is an anti-CTLA-4 monoclonal antibody (mAb) approved for melanoma treatment by the US Food and Drug Administration (FDA) in 2011, and it is the first agent to show survival benefits for metastatic melanoma patients.95 Ipilimumab has also been evaluated in clinical trials for metastatic prostate cancer and advanced non-small cell lung cancer, ipilimumab alone or combined with other anti-tumor therapies showed significant clinical benefits for cancer patients.96 Tremelimumab is another anti-CTLA-4 monoclonal antibody in clinical trials for cancer therapy, and showed anti-tumor activity with a durable response in phases I and II clinical studies97 (Table 2).
PD-L1/PD-1 blockade reverses exhausted T cells and restores anti-tumor function. The PD-1 antibodies (pidilizumab, pembrolizumab and nivolumab) and PD-L1 antibodies (BMS-936559, MPDL3280A and MEDI4736) have been subjected to clinical trials.98 Pidilizumab is the first PD-1 mAb for clinical trials, significant clinical benefit and durable response was observed in patients with hematologic malignancies who received pidilizumab treatment.99 Pembrolizumab is a PD-1-blocking mAb with no cytotoxic activity against T cells and has been used for advanced melanoma patients in a phase I trial, the safety and tumor response were satisfactory.100 Nivolumab is another mAb to PD-1, which was first studied clinically in patients with advanced solid tumors, the objective responses for melanoma, renal cell carcinoma (RCC) and non-small cell lung cancer (NSCLC) patients were durable and lasted over 1 year63, 101 (Table 2).
A fully human monoclonal PD-L1 antibody BMS-936559 was studied in clinical trials. Durable tumor regression was observed in advanced melanoma, NSCLC, RCC and ovarian cancer patients with BMS-936559 treatment, and the adverse events were tolerated.102 MPDL3280A, a humanized PD-L1-blocking mAb, showed impressive anti-tumor effects in metastatic urothelial bladder cancer, the tolerability and efficacy in other advanced solid tumors were also acceptable.103 MEDI4736 is a PD-L1 antibody with modified Fc domain, which was studied in phase I or Ib clinical trials for advanced solid tumors, the results are encouraging104 (Table 2).
The combined therapies with immune checkpoint antibodies are also in clinical trials. For example, pidilizumab combined therapy with rituximab was used for follicular lymphoma, pembrolizumab followed by ipilimumab or BRAF inhibitor treatment was used for malignant melanoma patients.64 Combined therapy with Nivolumab and ipilimumab was recently applied in melanoma. The rate of objective response rate in malanoma patients received combined therapy was 61%, whereas that in melanoma patients received ipilimumab monotherapy was only 11%, the complete responses in combination group and ipilimumab monotherapy were 22 and 0% separately.105 These combination immunotherapies exhibit promising effects in improving outcomes for advanced cancer patients.
Conclusions and Perspectives
The presence of T cells in TME correlates with favorable prognosis. However, T cells in TME are always in hyporesponsive state. There are several hurdles that limit T cells to eliminate tumors. The major stumbling block for T-cell hyporesponsiveness in cancer is T-cell exhaustion. Exhausted T cells have a unique molecular signature that is markedly distinct from naive, effector or memory T cells. They are defined as T cells with decreased cytokine expression and effector function. Reversing exhausted T cells and restoring anti-tumor potential represents an inspiring strategy to treat cancer. An attractive option of reversing exhausted T cells is to block inhibitory receptors. In animal models, blockade of PD-1 partially reversed T-cell exhaustion, and multiple blockades of inhibitory receptors enhanced T-cell function more efficiently. For example, combined blockade of PD-1 and LAG-3, PD-1 and CTLA-4, and PD-1 and TIM-3 were more efficient. Blockade with monoclonal antibodies targeting the inhibitory receptors CTLA-4, PD-1 and PD-L1 emerged as a successful therapy for patients with advanced melanoma. The durable tumor responses were achieved with PD-1 and PD-L1 blockade in phase I trials in many cancers, and tumor responses were observed in a higher proportion of patients with melanoma than typically observed with ipilimumab, indicating that the blockade of the PD-L1/PD-1 pathway is a more promising strategy for cancer treatment. However, there still exists some limitation in T-cell exhaustion research. Firstly, the different regulation roles of inhibitory receptors remain to be elucidated, for example, PD-1 and TIM-3 may regulate different process of T-cell exhaustion. Secondly, reversing exhausted T cells in cancer may induce excessive T-cell activation and cytotoxicity, leading to adverse reaction, more intervention should be applied to attenuate cytotoxicity-induced injury. Thirdly, benefits from inhibitory receptors blockade are limited, more combined therapies should be applied to enhance response rate. These will advance our fundamental understanding of TME and carcinogenesis. Importantly, the approach of reversing T-cell exhaustion in TME provides a promising avenue to treat cancer.
Abbreviations
- AP-1:
-
activator protein 1
- BTLA:
-
band T lymphocyte attenuator
- CTLA-4:
-
cytotoxic T lymphocyte antigen-4
- DC:
-
dendritic cell
- GzmB:
-
granzyme B
- IDO:
-
indoleamine 2,3-dioxygenase
- IFN:
-
interferon
- IL:
-
interleukin
- LAG-3:
-
lymphocyte activation gene 3 protein
- LCMV:
-
lymphocytic choriomeningitis virus
- mAb:
-
monoclonal antibody
- MDSC:
-
myeloid-derived suppressor cell
- NSCLC:
-
non-small cell lung cancer
- PD-1:
-
programmed cell death protein 1
- PD-L1:
-
programmed cell death 1 ligand 1
- PD-L2:
-
programmed cell death 1 ligand 2
- RCC:
-
renal cell carcinoma
- TAM:
-
tumor-associated macrophage
- TCR:
-
T-cell receptor
- TGF:
-
transforming growth factor
- TIGIT:
-
T-cell immunoglobulin and immunoreceptor tyrosine-based inhibitory motif domain
- TIL:
-
tumor-infiltrating lymphocyte
- TIM-3:
-
T-cell immunoglobulin domain and mucin domain protein 3
- TME:
-
tumor microenvironment
- TNF:
-
tumor necrosis factor
- Treg:
-
regulatory T cell
References
Wherry EJ, Ahmed R . Memory CD8 T-cell differentiation during viral infection. J Virol 2004; 78: 5535–5545.
Kim PS, Ahmed R . Features of responding T cells in cancer and chronic infection. Curr Opin Immunol 2010; 22: 223–230.
Kaech SM, Wherry EJ, Ahmed R . Effector and memory T-cell differentiation: implications for vaccine development. Nat Rev Immunol 2002; 2: 251–262.
Schluns KS, Lefrancois L . Cytokine control of memory T-cell development and survival. Nat Rev Immunol 2003; 3: 269–279.
Baitsch L, Fuertes-Marraco SA, Legat A, Meyer C, Speiser DE . The three main stumbling blocks for anticancer T cells. Trends Immunol 2012; 33: 364–372.
Zajac AJ, Blattman JN, Murali-Krishna K, Sourdive DJ, Suresh M, Altman JD et al. Viral immune evasion due to persistence of activated T cells without effector function. J Exp Med 1998; 188: 2205–2213.
Barber DL, Wherry EJ, Masopust D, Zhu B, Allison JP, Sharpe AH et al. Restoring function in exhausted CD8 T cells during chronic viral infection. Nature 2006; 439: 682–687.
Jin HT, Anderson AC, Tan WG, West EE, Ha SJ, Araki K et al. Cooperation of Tim-3 and PD-1 in CD8 T-cell exhaustion during chronic viral infection. Proc Natl Acad Sci USA 2010; 107: 14733–14738.
Crawford A, Wherry EJ . The diversity of costimulatory and inhibitory receptor pathways and the regulation of antiviral T cell responses. Curr Opin Immunol 2009; 21: 179–186.
Blackburn SD, Shin H, Haining WN, Zou T, Workman CJ, Polley A et al. Coregulation of CD8+ T cell exhaustion by multiple inhibitory receptors during chronic viral infection. Nat Immunol 2009; 10: 29–37.
Fourcade J, Sun Z, Pagliano O, Guillaume P, Luescher IF, Sander C et al. CD8(+) T cells specific for tumor antigens can be rendered dysfunctional by the tumor microenvironment through upregulation of the inhibitory receptors BTLA and PD-1. Cancer Res 2012; 72: 887–896.
Joller N, Hafler JP, Brynedal B, Kassam N, Spoerl S, Levin SD et al. Cutting edge: TIGIT has T cell-intrinsic inhibitory functions. J Immunol 2011; 186: 1338–1342.
Wherry EJ . T cell exhaustion. Nat Immunol 2011; 12: 492–499.
Wherry EJ, Blattman JN, Murali-Krishna K, van der Most R, Ahmed R . Viral persistence alters CD8 T-cell immunodominance and tissue distribution and results in distinct stages of functional impairment. J Virol 2003; 77: 4911–4927.
Iwai Y, Ishida M, Tanaka Y, Okazaki T, Honjo T, Minato N . Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade. Proc Natl Acad Sci USA 2002; 99: 12293–12297.
Murakami N, Riella LV . Co-inhibitory pathways and their importance in immune regulation. Transplantation 2014; 98: 3–14.
Maj T, Wei S, Welling T, Zou W . T cells and costimulation in cancer. Cancer J 2013; 19: 473–482.
Pauken KE, Wherry EJ . Overcoming T cell exhaustion in infection and cancer. Trends Immunol 2015; 36: 265–276.
Wherry EJ, Ha SJ, Kaech SM, Haining WN, Sarkar S, Kalia V et al. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity 2007; 27: 670–684.
Yamamoto R, Nishikori M, Kitawaki T, Sakai T, Hishizawa M, Tashima M et al. PD-1-PD-1 ligand interaction contributes to immunosuppressive microenvironment of Hodgkin lymphoma. Blood 2008; 111: 3220–3224.
Fourcade J, Kudela P, Sun Z, Shen H, Land SR, Lenzner D et al. PD-1 is a regulator of NY-ESO-1-specific CD8+ T cell expansion in melanoma patients. J Immunol 2009; 182: 5240–5249.
Ahmadzadeh M, Johnson LA, Heemskerk B, Wunderlich JR, Dudley ME, White DE et al. Tumor antigen-specific CD8 T cells infiltrating the tumor express high levels of PD-1 and are functionally impaired. Blood 2009; 114: 1537–1544.
Gehring AJ, Ho ZZ, Tan AT, Aung MO, Lee KH, Tan KC et al. Profile of tumor antigen-specific CD8 T cells in patients with hepatitis B virus-related hepatocellular carcinoma. Gastroenterology 2009; 137: 682–690.
Saito H, Kuroda H, Matsunaga T, Osaki T, Ikeguchi M . Increased PD-1 expression on CD4+ and CD8+ T cells is involved in immune evasion in gastric cancer. J Surg Oncol 2013; 107: 517–522.
Chen J, Wu XJ, Wang GQ . Hepatoma cells up-regulate expression of programmed cell death-1 on T cells. World J Gastroenterol 2008; 14: 6853–6857.
Chambers CA, Kuhns MS, Egen JG, Allison JP . CTLA-4-mediated inhibition in regulation of T cell responses: mechanisms and manipulation in tumor immunotherapy. Annu Rev Immunol 2001; 19: 565–594.
Teft WA, Kirchhof MG, Madrenas J . A molecular perspective of CTLA-4 function. Annu Rev Immunol 2006; 24: 65–97.
Duraiswamy J, Kaluza KM, Freeman GJ, Coukos G . Dual blockade of PD-1 and CTLA-4 combined with tumor vaccine effectively restores T-cell rejection function in tumors. Cancer Res 2013; 73: 3591–3603.
Parry RV, Chemnitz JM, Frauwirth KA, Lanfranco AR, Braunstein I, Kobayashi SV et al. CTLA-4 and PD-1 receptors inhibit T-cell activation by distinct mechanisms. Mol Cell Biol 2005; 25: 9543–9553.
Sakuishi K, Apetoh L, Sullivan JM, Blazar BR, Kuchroo VK, Anderson AC . Targeting Tim-3 and PD-1 pathways to reverse T cell exhaustion and restore anti-tumor immunity. J Exp Med 2010; 207: 2187–2194.
Fourcade J, Sun Z, Benallaoua M, Guillaume P, Luescher IF, Sander C et al. Upregulation of Tim-3 and PD-1 expression is associated with tumor antigen-specific CD8+ T cell dysfunction in melanoma patients. J Exp Med 2010; 207: 2175–2186.
Woo SR, Turnis ME, Goldberg MV, Bankoti J, Selby M, Nirschl CJ et al. Immune inhibitory molecules LAG-3 and PD-1 synergistically regulate T-cell function to promote tumoral immune escape. Cancer Res 2012; 72: 917–927.
Matsuzaki J, Gnjatic S, Mhawech-Fauceglia P, Beck A, Miller A, Tsuji T et al. Tumor-infiltrating NY-ESO-1-specific CD8+ T cells are negatively regulated by LAG-3 and PD-1 in human ovarian cancer. Proc Natl Acad Sci USA 2010; 107: 7875–7880.
Derre L, Rivals JP, Jandus C, Pastor S, Rimoldi D, Romero P et al. BTLA mediates inhibition of human tumor-specific CD8+ T cells that can be partially reversed by vaccination. J Clin Invest 2010; 120: 157–167.
Yu X, Harden K, Gonzalez LC, Francesco M, Chiang E, Irving B et al. The surface protein TIGIT suppresses T cell activation by promoting the generation of mature immunoregulatory dendritic cells. Nat Immunol 2009; 10: 48–57.
Chauvin JM, Pagliano O, Fourcade J, Sun Z, Wang H, Sander C et al. TIGIT and PD-1 impair tumor antigen-specific CD8+ T cells in melanoma patients. J Clin Invest 2015; 125: 2046–2058.
Johnston RJ, Comps-Agrar L, Hackney J, Yu X, Huseni M, Yang Y et al. The immunoreceptor TIGIT regulates antitumor and antiviral CD8(+) T cell effector function. Cancer Cell 2014; 26: 923–937.
Shin H, Blackburn SD, Intlekofer AM, Kao C, Angelosanto JM, Reiner SL et al. A role for the transcriptional repressor Blimp-1 in CD8(+) T cell exhaustion during chronic viral infection. Immunity 2009; 31: 309–320.
Kao C, Oestreich KJ, Paley MA, Crawford A, Angelosanto JM, Ali MA et al. Transcription factor T-bet represses expression of the inhibitory receptor PD-1 and sustains virus-specific CD8+ T cell responses during chronic infection. Nat Immunol 2011; 12: 663–671.
Agnellini P, Wolint P, Rehr M, Cahenzli J, Karrer U, Oxenius A . Impaired NFAT nuclear translocation results in split exhaustion of virus-specific CD8+ T cell functions during chronic viral infection. Proc Natl Acad Sci USA 2007; 104: 4565–4570.
Quigley M, Pereyra F, Nilsson B, Porichis F, Fonseca C, Eichbaum Q et al. Transcriptional analysis of HIV-specific CD8+ T cells shows that PD-1 inhibits T cell function by upregulating BATF. Nat Med 2010; 16: 1147–1151.
Terawaki S, Chikuma S, Shibayama S, Hayashi T, Yoshida T, Okazaki T et al. IFN-alpha directly promotes programmed cell death-1 transcription and limits the duration of T cell-mediated immunity. J Immunol 2011; 186: 2772–2779.
Xiao G, Deng A, Liu H, Ge G, Liu X . Activator protein 1 suppresses antitumor T-cell function via the induction of programmed death 1. Proc Natl Acad Sci USA 2012; 109: 15419–15424.
Utzschneider DT, Legat A, Fuertes Marraco SA, Carrie L, Luescher I, Speiser DE et al. T cells maintain an exhausted phenotype after antigen withdrawal and population reexpansion. Nat Immunol 2013; 14: 603–610.
Wherry EJ, Barber DL, Kaech SM, Blattman JN, Ahmed R . Antigen-independent memory CD8 T cells do not develop during chronic viral infection. Proc Natl Acad Sci USA 2004; 101: 16004–16009.
Lu B, Finn OJ . T-cell death and cancer immune tolerance. Cell Death Differ 2008; 15: 70–79.
Shi F, Shi M, Zeng Z, Qi RZ, Liu ZW, Zhang JY et al. PD-1 and PD-L1 upregulation promotes CD8(+) T-cell apoptosis and postoperative recurrence in hepatocellular carcinoma patients. Int J Cancer 2011; 128: 887–896.
Xia Y, Chen R, Ye SL, Sun R, Chen J, Zhao Y . Inhibition of T-cell responses by intratumoral hepatic stellate cells contribute to migration and invasion of hepatocellular carcinoma. Clin Exp Metastasis 2011; 28: 661–674.
Goding SR, Wilson KA, Xie Y, Harris KM, Baxi A, Akpinarli A et al. Restoring immune function of tumor-specific CD4+ T cells during recurrence of melanoma. J Immunol 2013; 190: 4899–4909.
Ohigashi Y, Sho M, Yamada Y, Tsurui Y, Hamada K, Ikeda N et al. Clinical significance of programmed death-1 ligand-1 and programmed death-1 ligand-2 expression in human esophageal cancer. Clin Cancer Res 2005; 11: 2947–2953.
Gao Q, Wang XY, Qiu SJ, Yamato I, Sho M, Nakajima Y et al. Overexpression of PD-L1 significantly associates with tumor aggressiveness and postoperative recurrence in human hepatocellular carcinoma. Clin Cancer Res 2009; 15: 971–979.
Kim JR, Moon YJ, Kwon KS, Bae JS, Wagle S, Kim KM et al. Tumor infiltrating PD1-positive lymphocytes and the expression of PD-L1 predict poor prognosis of soft tissue sarcomas. PLoS One 2013; 8: e82870.
Fay AP, Signoretti S, Callea M, Telomicron GH, McKay RR, Song J et al. Programmed death ligand-1 expression in adrenocortical carcinoma: an exploratory biomarker study. J Immunother Cancer 2015; 3: 3.
Zhang Y, Wang L, Li Y, Pan Y, Wang R, Hu H et al. Protein expression of programmed death 1 ligand 1 and ligand 2 independently predict poor prognosis in surgically resected lung adenocarcinoma. Onco Targets Ther 2014; 7: 567–573.
Muenst S, Schaerli AR, Gao F, Daster S, Trella E, Droeser RA et al. Expression of programmed death ligand 1 (PD-L1) is associated with poor prognosis in human breast cancer. Breast Cancer Res Treat 2014; 146: 15–24.
Hamanishi J, Mandai M, Iwasaki M, Okazaki T, Tanaka Y, Yamaguchi K et al. Programmed cell death 1 ligand 1 and tumor-infiltrating CD8+ T lymphocytes are prognostic factors of human ovarian cancer. Proc Natl Acad Sci USA 2007; 104: 3360–3365.
Maine CJ, Aziz NH, Chatterjee J, Hayford C, Brewig N, Whilding L et al. Programmed death ligand-1 over-expression correlates with malignancy and contributes to immune regulation in ovarian cancer. Cancer Immunol Immunother 2014; 63: 215–224.
Hino R, Kabashima K, Kato Y, Yagi H, Nakamura M, Honjo T et al. Tumor cell expression of programmed cell death-1 ligand 1 is a prognostic factor for malignant melanoma. Cancer 2010; 116: 1757–1766.
Wang L, Ma Q, Chen X, Guo K, Li J, Zhang M . Clinical significance of B7-H1 and B7-1 expressions in pancreatic carcinoma. World J Surg 2010; 34: 1059–1065.
Nomi T, Sho M, Akahori T, Hamada K, Kubo A, Kanehiro H et al. Clinical significance and therapeutic potential of the programmed death-1 ligand/programmed death-1 pathway in human pancreatic cancer. Clin Cancer Res 2007; 13: 2151–2157.
Karim R, Jordanova ES, Piersma SJ, Kenter GG, Chen L, Boer JM et al. Tumor-expressed B7-H1 and B7-DC in relation to PD-1+ T-cell infiltration and survival of patients with cervical carcinoma. Clin Cancer Res 2009; 15: 6341–6347.
Shi SJ, Wang LJ, Wang GD, Guo ZY, Wei M, Meng YL et al. B7-H1 expression is associated with poor prognosis in colorectal carcinoma and regulates the proliferation and invasion of HCT116 colorectal cancer cells. PLoS One 2013; 8: e76012.
Topalian SL, Hodi FS, Brahmer JR, Gettinger SN, Smith DC, McDermott DF et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 2012; 366: 2443–2454.
Ohaegbulam KC, Assal A, Lazar-Molnar E, Yao Y, Zang X . Human cancer immunotherapy with antibodies to the PD-1 and PD-L1 pathway. Trends Mol Med 2015; 21: 24–33.
Mougiakakos D, Choudhury A, Lladser A, Kiessling R, Johansson CC . Regulatory T cells in cancer. Adv Cancer Res 2010; 107: 57–117.
Nishikawa H, Sakaguchi S . Regulatory T cells in tumor immunity. Int J Cancer 2010; 127: 759–767.
Borsellino G, Kleinewietfeld M, Di Mitri D, Sternjak A, Diamantini A, Giometto R et al. Expression of ectonucleotidase CD39 by Foxp3+ Treg cells: hydrolysis of extracellular ATP and immune suppression. Blood 2007; 110: 1225–1232.
Kobie JJ, Shah PR, Yang L, Rebhahn JA, Fowell DJ, Mosmann TR . T regulatory and primed uncommitted CD4 T cells express CD73, which suppresses effector CD4 T cells by converting 5'-adenosine monophosphate to adenosine. J Immunol 2006; 177: 6780–6786.
Thornton AM, Shevach EM . CD4+CD25+ immunoregulatory T cells suppress polyclonal T cell activation in vitro by inhibiting interleukin 2 production. J Exp Med 1998; 188: 287–296.
Fontenot JD, Rasmussen JP, Gavin MA, Rudensky AY . A function for interleukin 2 in Foxp3-expressing regulatory T cells. Nat Immunol 2005; 6: 1142–1151.
Annacker O, Asseman C, Read S, Powrie F . Interleukin-10 in the regulation of T cell-induced colitis. J Autoimmun 2003; 20: 277–279.
Thomas DA, Massague J . TGF-beta directly targets cytotoxic T cell functions during tumor evasion of immune surveillance. Cancer Cell 2005; 8: 369–380.
Sharma MD, Baban B, Chandler P, Hou DY, Singh N, Yagita H et al. Plasmacytoid dendritic cells from mouse tumor-draining lymph nodes directly activate mature Tregs via indoleamine 2,3-dioxygenase. J Clin Invest 2007; 117: 2570–2582.
Hurwitz AA, Watkins SK . Immune suppression in the tumor microenvironment: a role for dendritic cell-mediated tolerization of T cells. Cancer Immunol Immunother 2012; 61: 289–293.
Allavena P, Mantovani A . Immunology in the clinic review series; focus on cancer: tumour-associated macrophages: undisputed stars of the inflammatory tumour microenvironment. Clin Exp Immunol 2012; 167: 195–205.
Mantovani A, Ming WJ, Balotta C, Abdeljalil B, Bottazzi B . Origin and regulation of tumor-associated macrophages: the role of tumor-derived chemotactic factor. Biochim Biophys Acta 1986; 865: 59–67.
Murdoch C, Tazzyman S, Webster S, Lewis CE . Expression of Tie-2 by human monocytes and their responses to angiopoietin-2. J Immunol 2007; 178: 7405–7411.
Lewis CE, Pollard JW . Distinct role of macrophages in different tumor microenvironments. Cancer Res 2006; 66: 605–612.
Bottazzi B, Walter S, Govoni D, Colotta F, Mantovani A . Monocyte chemotactic cytokine gene transfer modulates macrophage infiltration, growth, and susceptibility to IL-2 therapy of a murine melanoma. J Immunol 1992; 148: 1280–1285.
Mantovani A, Sozzani S, Locati M, Allavena P, Sica A . Macrophage polarization: tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol 2002; 23: 549–555.
Dannenmann SR, Thielicke J, Stockli M, Matter C, von Boehmer L, Cecconi V et al. Tumor-associated macrophages subvert T-cell function and correlate with reduced survival in clear cell renal cell carcinoma. Oncoimmunology 2013; 2: e23562.
Bronte V . Myeloid-derived suppressor cells in inflammation: uncovering cell subsets with enhanced immunosuppressive functions. Eur J Immunol 2009; 39: 2670–2672.
Ostrand-Rosenberg S, Sinha P . Myeloid-derived suppressor cells: linking inflammation and cancer. J Immunol 2009; 182: 4499–4506.
Liu Y, Zeng B, Zhang Z, Zhang Y, Yang R . B7-H1 on myeloid-derived suppressor cells in immune suppression by a mouse model of ovarian cancer. Clin Immunol 2008; 129: 471–481.
Yang R, Cai Z, Zhang Y, Yutzy WH 4th, Roby KF, Roden RB . CD80 in immune suppression by mouse ovarian carcinoma-associated Gr-1+CD11b+ myeloid cells. Cancer Res 2006; 66: 6807–6815.
Kim YJ, Park SJ, Broxmeyer HE . Phagocytosis, a potential mechanism for myeloid-derived suppressor cell regulation of CD8+ T cell function mediated through programmed cell death-1 and programmed cell death-1 ligand interaction. J Immunol 2011; 187: 2291–2301.
Massague J . TGFbeta in cancer. Cell 2008; 134: 215–230.
Katz LH, Li Y, Chen JS, Munoz NM, Majumdar A, Chen J et al. Targeting TGF-beta signaling in cancer. Expert Opin Ther Targets 2013; 17: 743–760.
Trapani JA . The dual adverse effects of TGF-beta secretion on tumor progression. Cancer Cell 2005; 8: 349–350.
Lin R, Chen L, Chen G, Hu C, Jiang S, Sevilla J et al. Targeting miR-23a in CD8+ cytotoxic T lymphocytes prevents tumor-dependent immunosuppression. J Clin Invest 2014; 124: 5352–5367.
Chen W, Jin W, Hardegen N, Lei KJ, Li L, Marinos N et al. Conversion of peripheral CD4+CD25- naive T cells to CD4+CD25+ regulatory T cells by TGF-beta induction of transcription factor Foxp3. J Exp Med 2003; 198: 1875–1886.
Strauss L, Bergmann C, Gooding W, Johnson JT, Whiteside TL . The frequency and suppressor function of CD4+CD25highFoxp3+ T cells in the circulation of patients with squamous cell carcinoma of the head and neck. Clin Cancer Res 2007; 13: 6301–6311.
Landskron G, De la Fuente M, Thuwajit P, Thuwajit C, Hermoso MA . Chronic inflammation and cytokines in the tumor microenvironment. J Immunol Res 2014; 2014: 149185.
Roncarolo MG, Bacchetta R, Bordignon C, Narula S, Levings MK . Type 1 T regulatory cells. Immunol Rev 2001; 182: 68–79.
Momtaz P, Postow MA . Immunologic checkpoints in cancer therapy: focus on the programmed death-1 (PD-1) receptor pathway. Pharmgenomics Pers Med 2014; 7: 357–365.
Graziani G, Tentori L, Navarra P . Ipilimumab: a novel immunostimulatory monoclonal antibody for the treatment of cancer. Pharmacol Res 2012; 65: 9–22.
Camacho LH, Antonia S, Sosman J, Kirkwood JM, Gajewski TF, Redman B et al. Phase I/II trial of tremelimumab in patients with metastatic melanoma. J Clin Oncol 2009; 27: 1075–1081.
Kyi C, Postow MA . Checkpoint blocking antibodies in cancer immunotherapy. FEBS Lett 2014; 588: 368–376.
Berger R, Rotem-Yehudar R, Slama G, Landes S, Kneller A, Leiba M et al. Phase I safety and pharmacokinetic study of CT-011, a humanized antibody interacting with PD-1, in patients with advanced hematologic malignancies. Clin Cancer Res 2008; 14: 3044–3051.
Hamid O, Robert C, Daud A, Hodi FS, Hwu WJ, Kefford R et al. Safety and tumor responses with lambrolizumab (anti-PD-1) in melanoma. N Engl J Med 2013; 369: 134–144.
Ramalingam SS, Mazieres J, Planchard D, Stinchcombe TE, Dy GK, Antonia SJ et al. Phase II study of nivolumab (anti-PD-1, BMS-936558, ONO-4538) in patients with advanced, refractory squamous non-small cell lung cancer: metastatic non-small cell lung cancer. Int J Radiat Oncol Biol Phys 2014; 90: 1266–1267.
Tykodi SS . PD-1 as an emerging therapeutic target in renal cell carcinoma: current evidence. Onco Targets Ther 2014; 7: 1349–1359.
Powles T, Eder JP, Fine GD, Braiteh FS, Loriot Y, Cruz C et al. MPDL3280A (anti-PD-L1) treatment leads to clinical activity in metastatic bladder cancer. Nature 2014; 515: 558–562.
Lu J, Lee-Gabel L, Nadeau MC, Ferencz TM, Soefje SA . Clinical evaluation of compounds targeting PD-1/PD-L1 pathway for cancer immunotherapy. J Oncol Pharm Pract 2014; e-pub ahead of print 9 Jun 2014.
Postow MA, Chesney J, Pavlick AC, Robert C, Grossmann K, McDermott D et al. Nivolumab and ipilimumab versus ipilimumab in untreated melanoma. N Engl J Med 2015; 372: 2006–2017.
Acknowledgements
This work was supported by National Natural Science Foundation of China Grants (Nos. 31170838, 81472435, 81071772 and 81222031), and National Key Basic Research Program of China (973 program, grant No. 2012CB526603).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by H-U Simon
Rights and permissions
Cell Death and Disease is an open-access journal published by Nature Publishing Group. This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Jiang, Y., Li, Y. & Zhu, B. T-cell exhaustion in the tumor microenvironment. Cell Death Dis 6, e1792 (2015). https://doi.org/10.1038/cddis.2015.162
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2015.162
This article is cited by
-
Immune evasion in cell-based immunotherapy: unraveling challenges and novel strategies
Journal of Biomedical Science (2024)
-
Advances in nano-immunotherapy for hematological malignancies
Experimental Hematology & Oncology (2024)
-
Digital twins elucidate critical role of Tscm in clinical persistence of TCR-engineered cell therapy
npj Systems Biology and Applications (2024)
-
Knockdown of circZMIZ1 enhances the anti-tumor activity of CD8+ T cells to alleviate hepatocellular carcinoma
Functional & Integrative Genomics (2024)
-
Ray of dawn: Anti-PD-1 immunotherapy enhances the chimeric antigen receptor T-cell therapy in Lymphoma patients
BMC Cancer (2023)