Abstract
Cannabidiol (CBD) is the most abundant cannabinoid in Cannabis sativa that has no psychoactive properties. CBD has been approved to treat inflammation, pain and spasticity associated with multiple sclerosis (MS), of which demyelination and oligodendrocyte loss are hallmarks. Thus, we investigated the protective effects of CBD against the damage to oligodendrocyte progenitor cells (OPCs) mediated by the immune system. Doses of 1 μM CBD protect OPCs from oxidative stress by decreasing the production of reactive oxygen species. CBD also protects OPCs from apoptosis induced by LPS/IFNγ through the decrease of caspase 3 induction via mechanisms that do not involve CB1, CB2, TRPV1 or PPARγ receptors. Tunicamycin-induced OPC death was attenuated by CBD, suggesting a role of endoplasmic reticulum (ER) stress in the mode of action of CBD. This protection against ER stress-induced apoptosis was associated with reduced phosphorylation of eiF2α, one of the initiators of the ER stress pathway. Indeed, CBD diminished the phosphorylation of PKR and eiF2α induced by LPS/IFNγ. The pro-survival effects of CBD in OPCs were accompanied by decreases in the expression of ER apoptotic effectors (CHOP, Bax and caspase 12), and increased expression of the anti-apoptotic Bcl-2. These findings suggest that attenuation of the ER stress pathway is involved in the ‘oligoprotective’ effects of CBD during inflammation.
Similar content being viewed by others
Main
Cannabidiol (CBD) is the most abundant cannabinoid in Cannabis sativa that is devoid of psychoactive properties. CBD exerts anti-inflammatory, antioxidant and neuroprotective effects,1 and it has been approved for the treatment of inflammation, pain and spasticity associated with multiple sclerosis (MS).2 Studies in an animal model of EAE have shown that CBD ameliorates the severity of the disease by attenuating neuroinflammation and axonal damage.3 Oligodendrocyte progenitor cells (OPCs) are relatively quiescent cells derived from precursors of the perinatal CNS that make up around 5–8% of the glial cell population in the adult; in the injured CNS, they can divide and are thought to differentiate to new myelinating oligodendroytes that replace those that have been lost in demyelinating areas.4 OPCs are highly vulnerable to inflammation and oxidative stress as they have a high metabolic rate, high intracellular iron, and low concentrations of the antioxidative glutathione; they also express an arsenal of molecules rendering them susceptible to inflammatory cytokines or high calcium levels among others.5 It is known that inflammation contributes to oligodendroglial damage in demyelinating diseases such as MS.6 Synthetic cannabinoids such as WIN 55212-2 and HU211 can protect oligodendrocyte progenitors cells (OPCs) from the apoptosis induced by the withdrawal of trophic support,7 although their utility is limited due to their unwanted psychotropic effects. However, little is known about the effects of CBD on the apoptosis of OPCs induced by inflammation. Although CBD induces cytotoxicity in oligodendrocytes of the optic nerve under basal conditions by increasing intracellular calcium,8 it also prevents apoptotic signaling in neurons by reducing calcium influx.9 The pharmacological basis of the effects of CBD remains elusive, although multiple potential targets of CBD have been proposed in function of the stimuli and cell type involved.1
The endoplasmic reticulum (ER) stress response modulates the response of oligodendrocytes to inflammatory stimuli,10 and it involves the activation of the double-stranded RNA-activated serine/threonine kinase (PKR), which has been implicated as an important component of host responses to infection and various situations of cellular stress.11 PKR is one of the ER transmembrane protein factors that coordinates an adaptive program known as the integrated stress response by phosphorylating the translation initiation factor 2α (eIF2α).12 Oligodendrocytes produce vast amounts of myelin and they are highly sensitive to homeostatic changes in the ER.10 The most rapidly activated pathway in conditions of ER stress involves translational repression, which can be mediated by the activation of PKR among others, and results in the phosphorylation of eiF2α.13 Although this pathway appears to offer cytoprotection to a variety of cell types,14 it can also activate apoptosis in others 15; particularly in oligodendrocytes the ER stress outcome may be determined by the developmental status of the cell, as in fully myelinated mature oligodendrocytes it promotes cell survival, but in actively myelinating/remyelinating oligodendrocytes leads to cell death.10 Indeed, ER stress has been linked with the apoptosis of myelinating oligodendrocytes induced by IFNγ16 and during ischemia.17 Moreover, several human diseases that involve demyelination/hypomyelination appear to involve aggravated ER stress. In Charcot–Marie–Tooth disease,18 Vanishing White Matter disease,19, 20 and even in immune-mediated demyelinating disorders such as MS,21 severe ER stress and activation of the unfolded protein response (UPR) are considered central to the pathogenesis of the disease.
In the present study, we provide evidence that CBD offers protection to OPCs against inflammation-induced damage, as well as protecting OPCs from oxidative stress by decreasing ROS production. Finally, we demonstrate that the protective effects of CBD against inflammatory damage and ER stress are associated with modifications in the expression of apoptotic effectors of the UPR.
Results
Dose–response studies of the effects of CBD on OPCs
As CBD has different effects on distinct cell types, we evaluated its effects on primary OPC cultures under basal conditions. In dose–response experiments (0.1, 1, 2.5 and 5 μM) CBD failed to induce cell death at low concentrations (0.1 and 1 μM: Figure 1a), although some cytotoxicity was observed at higher concentrations, resulting in the death of 23.38±3.98% of cells (P⩽0.01) after a 24-h exposure to 2.5 μM CBD, and of 33.13±5.6% (P⩽0.001) at 5 μM. Based on these findings, a dose of 1 μM was selected for the subsequent experiments.
Effects of CBD on OPC cytotoxicity. (a) Although CBD did not induce cell death at low concentrations (0.1 and 1 μM), cytotoxic effects were observed at 2.5 and 5 μM. OPCs were exposed to CBD and cell death was quantified 48 h later using the LDH method. Data represent the mean±S.E.M. of n=3 cultures analyzed in triplicate. Statistical significance was determined by a one-way ANOVA: **P⩽0.01 and ***P⩽0.001 versus untreated cells. (b) CBD did not augment OPC proliferation evident as an increase in BrdU incorporation. OPCs were incubated with BrdU (10 μM) for 24 h and at least 10 000 cells were then quantified by immunocytochemistry. (c) Flow cytometry analysis revealed the CBD does not affect the cell cycle progression of OPCs. Freshly isolated OPCs were incubated for 24 h in the presence or absence of CBD (1 μM), and the cell cycle of a minimum of 10 000 cells was analyzed on a FACSAria flow cytometer following PI staining. (d, e) CBD did not alter intracellular Ca2+ levels under basal conditions. OPCs were loaded with the Ca2+-sensitive dye Fluo-4 and the fluorescence signal was monitored on a scanning confocal microscope under basal conditions and after adding CBD (1 μM: n=5 coverslips). (d) Representative pseudocolor images showing Ca2+ levels in cultured OPCs under basal conditions and in the presence of CBD (1 μM). Scale bar=50 μm. (e) Fluorescence traces showing the Ca2+ time course in individual OPCs (n=8) from the experiment shown in (d), both under basal conditions and in the presence of CBD.
We next investigated the effect of CBD (1 μM) on the cell cycle by evaluating OPC proliferation. Quantification of BrdU+ cells in OPC primary cultures (n=10 000 cells, Figure 1b) revealed that CBD did not increase the proliferation of OPCs in vitro (47.65±8.61%) with respect to the controls (48.21±10.5%). These results were confirmed by subsequently analyzing the cell cycle by flow cytometry (Figure 1c), in which no differences were observed between G0/G1, S and G2/M phases.
At doses of 0.1 and 1 μM, CBD has been reported to increase intracellular Ca2+ and to induce oligodendrocyte death in the optic nerve.8 Thus, we investigated whether 1 μM CBD-induced Ca2+ release from intracellular stores in cultured OPCs loaded with the Ca2+-sensitive dye, Fluo-4. There was no difference in the fluorescence signal obtained under basal conditions and in the presence of CBD (1 μM: Figures 1d and e), indicating that intracellular Ca2+ levels were not significantly modified by CBD.
CBD protects OPCs from inflammatory stimuli and from apoptosis in a cannabinoid receptor-independent manner
As we previously reported that the LPS/IFNγ inflammatory stimuli induced cytotoxicity in OPCs,22 it was noteworthy that CBD (1 μM) protected OPCs from the noxious effects of inflammation (P⩽0.001, Figure 2a), decreasing cell death from 37.84±4.95% to 10.41±4.41%. Indeed, the induction of the apoptotic effector caspase 3 (Figure 2b) by LPS/IFNγ was reversed by the treatment with CBD (P⩽0.05), and the number of TUNEL+ cells (24.35±1.54%) fell to control levels in the presence of CBD (3.34±0.96%, P⩽0.001) when quantified 24 h post treatment (Figures 2c and d). To investigate the mechanisms underlying the oligoprotection offered by CBD, antagonists of CB1, CB2, TRPV1 and PPARγ receptors were administered before the LPS/IFNγ insult in the presence and absence of CBD. None of these antagonists reversed the protective effects of CBD observed in inflammatory conditions, suggesting that the effects of CBD are not mediated by these receptors (Figure 2a).
CBD protects against inflammatory damage by diminishing apoptosis and decreases the number of TUNEL+ OPCs through a mechanism that does not involve CB1, CB2, TRPV1 or PPARγ receptors. (a) LPS/IFNγ-induced cytotoxicity in OPCs was attenuated by CBD, a dose of 1 μM proving to be the most effective). Administration of CB1, CB2, TRPV1 or PPARγ antagonists (SR1, AM639, CPZ: 1 μM and GW9662: 50 nM) 30 min before the stimulus had no effect, indicating that none of these receptors are implicated in the protective effects of CBD. The data represent the mean±S.E.M. of n=3 independent cultures analyzed in triplicate, and the statistical analysis was performed using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: ***P⩽0.001 versus untreated cells, #P⩽0.05 and ###P⩽0.001 versus cells exposed to LPS/IFNγ alone. (b) Cleaved caspase3 western blot shows that LPS/IFNγ treatment induces the activation of the apoptotic pathway, whereas the co-treatment with CBD reduces this induction. OPCs were incubated with LPS/IFNγ in presence or absence of CBD (1 μM). Total protein extracts were prepared 24 h later and cleaved caspase 3 (19 KDa) was assessed in western blots probed with specific antibodies. The data represent the mean±S.E.M. optical density normalized to tubulin from three independent cultures analyzed in triplicate, and statistical analysis was performed using one-way ANOVA followed by the Bonferroni post-hoc test: **P⩽0.01 compared with non-treated cells, #P⩽0.05 compared with LPS/IFNγ group. (c and d) A2B5 and TUNEL staining show that LPS/IFNγ decreased OPC number by inducing apoptosis, an effect that was reversed by CBD as previously confirmed by caspase 3 measurement. OPCs were exposed for 24 h to the cytotoxic stimulus, in the presence or absence of CBD (1 μM), and 6000 OPCs cells were counted. Data represent the mean±S.E.M., and the statistical significance was determined using the Kruskal–Wallis ANOVA followed by Mann–Whitney U test: ***P⩽0.001 versus untreated cells, and ###P⩽0.001 versus cells exposed to LPS/IFNγ alone
CBD rescues OPCs from H2O2-induced death by decreasing ROS production
CBD is a resorcinol-based compound with direct and potent antioxidant properties;23 hence, we investigated whether CBD acts as an antioxidant in OPCs subjected to oxidative stress by evaluating its effects on the cell death and ROS production induced by hydrogen peroxide (100 μM). CBD prevented the detachment and swelling of OPCs induced by direct oxidative stress (Figure 3a), and decreased cell death from 84.89±6.93% to 39.12±1.82% (P⩽0.01, Figure 3b). Moreover, this effect was accompanied by a decrease in ROS production, as determined in DCF-DA assays 1 h post treatment (H2O2+vehicle, 216.63±15.7%; H2O2+CBD, 151.59±5.10%: P⩽0.001, Figure 3c). To separate the antioxidant properties of CBD of its possible cytoprotective effects on OPCs during inflammation, we also evaluated the effects of CBD on NO production in response to LPS/IFN-γ by measuring nitrites and by western blot to assess NOS-2 expression, but CBD was not able to modify NO production (data not shown).
Oxidative stress induced by H2O2 induces OPC detachment and death, an effect that was attenuated by CBD by decreasing ROS production. (a) Phase contrast images ( × 10) show that treatment with H2O2 induced the swelling and detachment of OPCs, an effect prevented by CBD treatment. (b) CBD protects OPCs from oxidative stress. OPCs were treated with H2O2 in the presence or absence of CBD (1 μM) and cell death was quantified 18 h later using the LDH method. The data represent the mean±S.E.M. of four independent cultures analyzed in triplicate, and the statistical significance was determined using one-way ANOVA followed by the Bonferroni post-hoc test: ***P⩽0.001 versus untreated cells, ##P⩽0.01 versus cells exposed to H2O2 alone. (c) CBD decreased ROS production under conditions of oxidative stress. OPCs were loaded with DCF-DA for 30 min and stimulated with H2O2 in the presence or absence of CBD (1 μM). Fluorescence was measured 2 h later at 485/530 nm in a microplate reader and the data represent the means±S.E.M. of n=3 independent cultures analyzed in triplicate. Statistical significance was determined using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: ***P⩽0.001 versus untreated cells, ###P⩽0.001 versus cells exposed to H2O2 alone
ER stress induces OPC death, an effect that is attenuated by CBD via decreased eiF2α phosphorylation
As ER stress is implicated in several diseases with inflammatory components, such as MS,21 we analyzed primary OPC death in response to activation of this cellular program. Tunicamycin-induced ER stress led to OPC death 24 h post treatment (45.81±4.7%: Figure 4a), which was attenuated by treatment with CBD (20.39±2.54%, P⩽0.01). Exposure to CBD also decreased the phosphorylation of the eiF2α protein (P⩽0.05), an initiator of the apoptotic pathway induced by ER stress (Figure 4b). Interestingly, tunicamycin-induced ER stress was not mediated by the phosphorylation of PKR, a potential activators of eiF2α in the ER (data not shown).
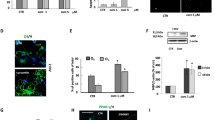
OPC death is mediated by ER stress, an effect that is attenuated by CBD through decreased PKR and eiF2α phosphorylation in conditions of inflammation. (a) CBD attenuated tunicamycin-induced OPC death. OPCs were incubated with tunicamycin (1 μg/ml) in the presence or absence of CBD (1 μM), and cell death was quantified 24 h later by the LDH method. The data represent the mean±S.E.M. of three independent cultures analyzed in triplicate, and the statistical significance was determined using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: ***P⩽0.001 versus untreated cells, ##P⩽0.01 versus cells exposed to tunicamycin alone. (b) Tunicamycin treatment induced the eiF2α phosphorylation, an effect that was attenuated by CBD. OPCs were incubated with tunicamycin (1 μg/ml) in the presence or absence of CBD (1 μM). Total protein extracts were prepared 5 min later and the phosphorylated (38 kDa) and total (38 kDa) eiF2α was assessed in western blots probed with specific antibodies. The data represent the mean±S.E.M. optical density normalized to tubulin from four independent cultures analyzed in triplicate, and the statistical significance was determined using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: **P⩽0.01 versus untreated cells, #P⩽0.05 versus cells exposed to tunicamycin alone. (c and d) Inflammation-induced PKR and eiF2α phosphorylation, an effect that was attenuated by CBD. OPCs were treated with LPS/IFNγ in the presence or absence of CBD (1 μM). Total protein extracts were prepared 5 min later and PKR (phosphorylated, 68 kDa; total, 68 kDa) and eiF2α (phosphorylated, 38 kDa; total, 38 kDa) was assessed in western blots probed with specific antibodies. The data represent the mean±S.E.M. optical density normalized to tubulin from five cultures, and the statistical significance was determined using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: **P⩽0.01 versus untreated cells, #P⩽0.05 versus cells exposed to LPS/IFNγ alone
CBD attenuates the activation of the ER apoptotic pathway in inflammatory conditions
Given the link between the mechanisms underlying inflammation and ER stress recently reported,24 we investigated the ER stress response induced by LPS/IFNγ. When we examined the effect of LPS/IFN-γ on PKR and eiF2α phosphorylation in OPCs, an increase in the phosphorylation of these proteins was evident in Western blots (Figures 4c and d). Interestingly, CBD impaired this increase in PKR and eiF2α phosphorylation, which remained at control levels (P⩽0.05), suggesting that one of the protective effects of CBD in OPCs involves the reduction of ER stress during neuroinflammation.
To confirm the effects of CBD in combating the ER stress associated with inflammation, we analyzed ER mediators of the apoptotic pathway. CBD significantly dampened the induction of ER pro-apoptotic molecules by LPS/IFNγ, such as the initiator CHOP, a major ER stress marker, and the effector caspase 12, as evident by real-time (RT)-PCR (P⩽0.01: Figure 5). In addition, the balance of pro-apoptotic (Bax) and anti-apoptotic (Bcl-2) proteins, which is deregulated by LPS/IFNγ treatment, returned to the basal state in the presence of CBD (P⩽0.05). Furthermore, the expression of GADD34, a negative feedback protein in this pathway augmented when OPCs were treated with CBD (P⩽0.001), suggesting that this cannabinoid represses this apoptotic program.
Inflammation activates the ER apoptotic pathway in OPCs, an effect that was attenuated by CBD. (a) CBD attenuated the inflammation-induced increase in CHOP expression. (b) The upregulation of caspase 12 expression in conditions of inflammation was attenuated by CBD. (c) CBD restores the Bcl-2/Bax balance in OPCs treated with LPS/IFNγ. (d) CBD increases the expression of the negative feedback regulator GADD34 under conditions of inflammation. In all cases, OPCs were incubated with LPS/IFNγ in the presence or absence of CBD (1 μM). The mRNA expression of each gene was measured 24 h later by quantitative RT-PCR and normalized to the expression of the 18S gene. The data represent the mean±S.E.M. of three independent cultures analyzed in triplicate, and the statistical significance was determined using Kruskal–Wallis ANOVA followed by Mann–Whitney U test: *P<0.05, ***P⩽0.001 versus untreated cells; and #P⩽0.05, ##P⩽0.01 versus cells exposed to LPS/IFNγ alone
Discussion
In this study, we show that the nonpsychotropic cannabinoid, CBD, prevents OPC death induced by inflammatory, oxidative or direct ER stress. CBD does not modify the OPC cell cycle and its protective effect was unaltered by classical cannabinoid, vanilloid or PPARγ receptor antagonists. Moreover, the anti-apoptotic effect of CBD appears to be mediated by decreasing the expression of pro-apoptotic effectors and dampening the activity of the ER stress pathway. These findings define a novel mode of action for CBD in OPCs, supporting its therapeutic potential to protect OPCs in pathologies involving demyelination.
Neuroinflammation is one of the primary mechanisms underlying the pathogenesis of MS, and proinflammatory mediators are considered key effectors of the damage in demyelinating disorders. Indeed, previous studies have shown that inflammatory stimuli induce apoptosis in OPCs.6, 22 When we initially studied the effects of CBD on primary OPC cultures, cytotoxic effects were only observed at doses >2.5 μM. At doses of 0.1 and 1 μM, CBD was previously reported to increase intracellular calcium and provoke cytotoxic effects,8 although no such Ca2+ influx was observed here on exposure to 1 μM CBD. These conflicting findings may reflect the different source of oligodendrocytes (optic nerve versus encephalon) and/or the state of differentiation of the cells (mature oligodendrocytes versus progenitors), pointing out to a different effect of CBD depending on the developmental state of the cell. Although CBD has previously been implicated in the regulation of the cell cycle,1 we ruled out this possibility by studying BrdU incorporation and cell cycle progression. Importantly, at low doses, CBD protected OPCs from LPS/IFNγ-induced cell death, evident by the reduction of caspase 3 and the number of TUNEL+ cells. Although CBD protected OPCs from inflammatory damage, we did not observe alterations neither in nitrites nor NOS-2 induction by LPS/IFN-γ, indicating the lack of participation of NO in the protective effects of CBD. Although CB1 and CB2 receptors were expressed on OPCs,7 CBD-induced protection of OPCs was not mediated by the activation of these receptors. Blocking of vanilloid receptors or of the nuclear receptor PPARγ also had no effect on the capacity of CBD to protect OPCs from inflammatory damage, precluding the involvement of these receptors. These findings are consistent with reports of other effects of CBD that occur independently of classical and alternative cannabinoid receptors.25
CBD protected OPCs from hydrogen peroxide-induced oxidative stress by diminishing ROS production, consistent with the antioxidant properties attributed to this compound in different experimental models.26 This is an important finding, as OPCs are very vulnerable to oxidative stress,27 considered to be one of the pathogenic mechanisms underlying demyelination and axonal damage in MS.
Oligodendrocytes are very sensitive to alterations in ER homeostasis. Misfolded proteins generate ER stress and contribute to cell death in pathophysiological conditions, while mutations affecting the folding of myelin constituents lead to oligodendrocyte death.28 We investigated the role of ER stress in OPC death in vitro. Tunicamycin, an ER stressor, induced OPC cytotoxicity through a mechanism that involved the phosphorylation of eiF2α, without altering PKR phosphorylation, suggesting that the induction of the UPR pathway with the tunicamycin treatment can be mediated by other ER transmembrane protein factors such as IRE1α or ATF6. Activating this pathway has been linked with the developmental status of the cell 10 and here we present evidence of the detrimental effects of ER stress in OPCs. The ability of CBD to protect OPCs from the damage caused by ER stress through decreasing eiF2α phosphorylation highlights the potential therapeutic properties of this compound in pathological conditions in which ER homeostasis is compromised, as proposed in neurodegenerative and demyelinating diseases.29, 30
There is substantial evidence linking inflammation with ER stress through several intracellular pathways.11, 24 In animal models of MS, IFNγ induces ER stress in actively myelinating oligodendrocytes, leading to apoptosis and abnormalities in neuronal myelination.31 Our results point to the crosstalk between inflammation and ER stress in OPCs, as LPS/IFNγ-induced cell death involved the phosphorylation of PKR and eiF2α and hence, the apoptotic pathway activated by the UPR. This pathway has been associated with increased expression of pro-apoptotic factors, such as the CHOP transcription factor (C/EBP homologous protein)32 that primarily promote apoptosis by repressing Bcl-2 expression33 or by inducing caspase 12.34 In OPCs, we found that inflammation involved caspase 3 activation, induced the expression of CHOP and caspase 12, and altered the balance between Bax and Bcl-2, implicating ER stress in cell apoptosis.
Our findings constitute the first evidence that CBD protects OPCs from inflammation-induced apoptosis by blocking ER stress. In inflammatory conditions, CBD decreased the levels of phosphorylated PKR and eiF2α in OPCs. Moreover, this effect was accompanied by the restoration of CHOP, caspase 12, Bcl-2 and Bax mRNA to control levels, together with an increase in GADD34 expression, a negative feedback regulator of this pathway.35
In summary, the findings presented here indicate that low doses of CBD exert oligoprotective effects in OPCs under conditions of inflammation, oxidative and ER stress. In conditions of oxidative stress, the protective effect of CBD was mediated by a decrease in ROS production, while under neuroinflammatory conditions, CBD combated apoptosis by decreasing ER stress through the modulation of the PKR-eiF2α pathway. We propose that CBD, a C. sativa derivative that lacks psychoactive properties, is a good candidate to protect OPCs from different cytotoxic insults, with significant therapeutic potential for the treatment of demyelinating pathologies.
Material and Methods
Animals
Animal handling and care was performed in compliance with European Union guidelines (86/609/EEC) and Spanish regulations (BOE67/8509-12; BOE1201/2005) regarding the use and care of laboratory animals, and all the protocols were approved by the local Animal Care and Ethics Committee of the CSIC.
Reagents
Griess reagent (sulfanilamide, N-(1-naphtyl)ethylenediamine), BrdU, DCFDA, hydrogen peroxide, LPS and tunicamycin were purchased from Sigma-Aldrich (Madrid, Spain). IFNγ was acquired from Peprotech (London, UK), CPZ from Alexis Biochemicals (Lausen, Sweden), CBD, AM630 and GW9662 from Tocris (Bristol, UK) and SR1 was kindly provided by Sanofi-Aventis (Montpellier, France).
Culture of oligodendrocyte progenitors
Primary cultures of OPCs derived from P0–P2 Wistar rats were prepared as described previously,22, 36 with some modifications in doi:10.1038/protex.2011.218 (Open Nature exchange protocols only on line). Cells were plated on poly-D-lysine-coated plates at 50 000 cells/cm2 for western blotting or 25 000 cells/cm2 for other assays, and they were maintained for 3 days at 37 °C and 5% CO2 in serum-free defined medium containing 5 ng/ml of growth factors (bFGF and PDGF-AA).
Cell toxicity
Oligodendrocyte death was quantified by measuring the release of lactate dehydrogenase (LDH) from damaged cells into the bathing medium 18, 24 and 48 h after exposure to hydrogen peroxide, tunicamycin and LPS/IFNγ, respectively, according to the manufacturer’s instructions (cytotoxicity detection kit, Roche, Manhein, Germany). All experiments compared the cell death induced with the basal levels of cell death in the cultures.
TUNEL assay
OPCs were seeded on poly-D-lysine-coated coverslips and maintained for 24 h with LPS/IFNγ and/or CBD. After they were fixed in 4% PFA, post-fixed in EtOH/acetic acid for 5 min at −20 °C and maintained in equilibration buffer for 1 min, they were incubated with the TdT enzyme in a reaction buffer for 1 h at 37 °C (Apoptosis detection kit, Chemicon, Millipore Ibérica, Madrid, Spain). After washing, the coverslips were incubated with the anti-DIG antibody in blocking solution and counterstained with DAPI. The data represent TUNEL+ cells as a percentage of the total number of cells.
Immunocytochemistry
For BrdU analysis, OPCs were seeded on poly-D-lysine-coated coverslips and incubated with BrdU (10 μM) for 24 h in the presence or absence of CBD. Cells were then fixed in 4% PFA for 20 min, treated with 2 N HCl for 10 min, blocked and incubated with anti-BrdU antibody (DSHB, 1:1000). After washing, the cells were incubated with an anti-mouse secondary antibody (1:1000) and counterstained with DAPI. For A2B5 staining, the cells were treated for 24 h with LPS/IFNγ in the presence or absence of CBD, incubated in vivo with anti-A2B5 marker (R&D Systems, Mineapolis, MN, USA, 1:200), fixed in 4% PFA and incubated with the secondary antibody (1:1000).
Flow cytometry
Freshly isolated OPCs were maintained on uncoated plates for 24 h with vehicle or CBD. The cells were then collected, fixed in cold 70% ethanol for 30 min, resuspended in phosphate buffer saline (PBS) and incubated with 100 μg/ml Ribonuclease A (Sigma-Aldrich) and 50 μg/ml propidium iodide (PI; Sigma-Aldrich) for 30 min. Argon laser excitation at 488 nm was used to measure PI fluorescence through a band-pass 616/23 nm filter using a FACSAria flow cytometer (BD Biosciences, San Diego, CA, USA). Debris and duplets were excluded from the analysis and a minimum of 10 000 cells were acquired in each experiment. FACSDiva analysis software (BD Biosciences) was used to define the cell cycle stages.
Measurement of intracellular Ca2+
Cells were seeded on coverslips and incubated for 20–30 min at 37 °C in PBS containing Fluo4-AM (0.3 μM, Invitrogen, Barcelona, Spain) and pluronic F-127 (0.04%, Sigma-Aldrich). The coverslips were then transferred to the microscope chamber and bathed in an extracellular medium containing (in mM): NaCl 140, KCl 5, MgCl2 4, HEPES 10, glucose 10 and sucrose 6 (pH 7.35). All experiments were performed at room temperature. Cells were imaged with an Olympus (Barcelona, Spain) FV3 scanning confocal microscope equipped with a × 40 objective (NA, 0.8) and laser emission at 488 nm was used to excite Fluo-4. The fluorescent signal recorded is displayed as a pseudocolor image and the look-up-table used is indicated in each figure. The time frame acquisition was 1.12 s.
ROS determination
OPCs were loaded with dichlorodihydrofluorescein diacetate acetyl ester (DCFDA, 2 μM) for 30 min, washed and stimulated with hydrogen peroxide for 2 h or with LPS/IFNγ for 24 h in the presence or absence of CBD. Fluorescence was measured at 485/530 nm in a microplate reader and normalized to the negative control.
Western blot analysis
Western blot analysis was performed as previously described 7 using 30–40 μg of OPC protein extract and an anti-cleaved caspase3 (Asp175; 1:1000, Cell Signaling Technology, Denvers, MA, USA), anti-phospho (Ser51) eIF2α (1:1000; Cell Signaling Technology), anti-total eIF2α (1:1000; Cell Signaling Technology), anti-phospho (Thr446) PKR (1:1000, Upstate, Millipore Ibérica, Madrid, Spain) and anti-total PKR (1:1000, Millipore, Madrid, Spain). Anti-α-tubulin (1:40 000; Sigma-Aldrich) was used as a loading control.
RNA extraction, reverse transcription and RT-PCR
Total OPC RNA was extracted using the RNeasy mini columns kit (Qiagen, Crawley, UK) and treated with DNaseI (Qiagen), and the RNA concentration and purity were determined in a Nanodrop spectrophotometer (Nanodrop Technologies, Wilmington, DE, USA). Total RNA (1 μg) was reverse transcribed using the Promega reverse transcription kit (Promega, Madrid, Spain) and RT-PCR was performed on 1 μl of cDNA (corresponding to 50 ng RNA input) with 200 nM of the primers listed below (Applied Biosystems, Warrington, UK), quantifying expression using SYBR Green (Applied Biosystems). The amplification cycles involved an initial activation step at 50 °C for 2 min and a denaturation step at 95 °C for 10 min, followed by 40 cycles of denaturation at 95 °C for 15 s and annealing/extension at 60 °C for 1 min. PCR assays were carried out in 96-well plates using a 7500 Real-Time PCR system (Applied Biosystems). Each sample was assayed in duplicate and a 6-point standard curve was run in parallel. The ratio between the values obtained for each gene and the 18S house-keeping gene provided a relative quantification of expression. The 5′-3′primer secuences used were the following: CHOP (forward 5′-CCAAAATAACAGCCGGAACCT-3′; reverse 5′-CAAAGGCGAAAGGCAGAGACT-3′), GADD34 (forward 5′-AGCATGGACACGCCTTAGAAA-3′; reverse 5′-AGGCTGGGAGGAGGGATTT-3′), Bax (forward 5′-GGGTGGCAGCTGACATGTTT-3′; reverse 5′-TGATCAGCTCGGGCACTTTA-3′), Bcl-2 (forward 5′-TGAGAGCAACCGAACGCCCG-3′; reverse 5′-CCGTGGCAAAGCGTCCCCTC-3′), caspase 12 (forward 5′-GAAGGAAGGCCGAACCCGCC-3′; reverse 5′-TGCTCTGGACGGCCAGCAAAC-3′) and 18S (forward 5′-ATGCTCTTAGCTGAGTGTCCCG-3′; reverse 5′-ATTCCTAGCTGCGGTATCCAGG-3′)
Data analysis
All data are expressed as the mean±S.E.M. (n), where n refers to the number of cultures assayed, each obtained from a different group of animals and evaluated in triplicate. One-way ANOVA followed by the Bonferroni post-hoc test, or Kruskal—Wallis ANOVA followed by Mann–Whitney U test was used to determine the statistical significance in all cases. The level of significance was set at P<0.05.
Abbreviations
- ATF-6:
-
activation transcription factor 6
- BrdU:
-
5-bromo-2'-deoxyuridine
- CB1:
-
cannabinoid receptor type 1
- CB2:
-
cannabinoid receptor type 2
- CBD:
-
cannabidiol
- DCF-DA:
-
2',7'-dichlorofluorescein-diacetate
- eiF2α:
-
translation initiation factor 2α
- ER:
-
endoplasmic reticulum
- IFNγ:
-
interferon-gamma
- IRE1α:
-
inositol-requiring enzyme 1α
- ROS:
-
reactive oxygen species
- LPS:
-
lipopolysaccharide
- MS:
-
multiple sclerosis
- NO:
-
nitric oxide
- NOS-2:
-
nitric oxide syntase-2
- OPCs:
-
oligodendrocyte precursor cells
- PKR:
-
double-stranded RNA-activated serine/threonine kinase
- PPARγ:
-
peroxisome proliferator-activated receptor gamma
- RT-PCR:
-
reverse transcription PCR
- TRPV1:
-
transient receptor potential cation channel subfamily V member 1
- TUNEL:
-
terminal deoxynucleotidyl transferase dUTP nick end labeling
- UPR:
-
unfolded protein response
References
Izzo AA, Borrelli F, Capasso R, Di Marzo V, Mechoulam R . Non-psychotropic plant cannabinoids: new therapeutic opportunities from an ancient herb. Trends Pharmacol Sci 2009; 30: 515–527.
Sastre-Garriga J, Vila C, Clissold S, Montalban X . THC and CBD oromucosal spray (Sativex(R)) in the management of spasticity associated with multiple sclerosis. Expert Rev Neurother 11: 627–637.
Kozela E, Lev N, Kaushansky N, Eilam R, Rimmerman N, Levy R et al. Cannabidiol inhibits pathogenic T cells, decreases spinal microglial activation and ameliorates multiple sclerosis-like disease in C57BL/6 mice. Br J Pharmacol 163: 1507–1519.
Levine JM, Reynolds R, Fawcett JW . The oligodendrocyte precursor cell in health and disease. Trends Neurosci 2001; 24: 39–47.
Bradl M, Lassmann H . Oligodendrocytes: biology and pathology. Acta Neuropathol 2010; 119: 37–53.
Lehnardt S, Lachance C, Patrizi S, Lefebvre S, Follett PL, Jensen FE et al. The toll-like receptor TLR4 is necessary for lipopolysaccharide-induced oligodendrocyte injury in the CNS. J Neurosci 2002; 22: 2478–2486.
Molina-Holgado E, Vela JM, Arévalo-Martín A, Almazán G, Molina-Holgado F, Borrel J, Guaza C . Cannabinoids promote oligodendrocyte progenitor survival: involvement of cannabinoid receptors and phosphatidylinositol-3 kinase/Akt signaling. J Neurosci 2002; 22: 9742–9753.
Mato S, Victoria Sanchez-Gomez M, Matute C . Cannabidiol induces intracellular calcium elevation and cytotoxicity in oligodendrocytes. Glia 58, 1739-47.
Alvarez FJ, Lafuente H, Rey-Santano MC, Mielgo VE, Gastiasoro E, Rueda M et al. Neuroprotective effects of the nonpsychoactive cannabinoid cannabidiol in hypoxic-ischemic newborn piglets. Pediatr Res 2008; 64: 653–658.
Lin W, Popko B . Endoplasmic reticulum stress in disorders of myelinating cells. Nat Neurosci 2009; 12: 379–385.
Lee JH, Park EJ, Kim OS, Kim HY, Joe EH, Jou I et al. Double-stranded RNA-activated protein kinase is required for the LPS-induced activation of STAT1 inflammatory signaling in rat brain glial cells. Glia 2005; 50: 66–79.
Proud CG . eIF2 and the control of cell physiology. Semin Cell Dev Biol 2005; 16: 3–12.
Harding HP, Novoa I, Zhang Y, Zeng H, Wek R, Schapira M et al. Regulated translation initiation controls stress-induced gene expression in mammalian cells. Mol Cell 2000; 6: 1099–1108.
Lu PD, Jousse C, Marciniak SJ, Zhang Y, Novoa I, Scheuner D et al. Cytoprotection by pre-emptive conditional phosphorylation of translation initiation factor 2. EMBO J 2004; 23: 169–179.
Southwood CM, Garbern J, Jiang W, Gow A . The unfolded protein response modulates disease severity in Pelizaeus-Merzbacher disease. Neuron 2002; 36: 585–596.
Lin W, Harding HP, Ron D, Popko B . Endoplasmic reticulum stress modulates the response of myelinating oligodendrocytes to the immune cytokine interferon-gamma. J Cell Biol 2005; 169: 603–612.
Kraskiewicz H, FitzGerald U . Partial XBP1 knockdown does not affect viability of oligodendrocyte precursor cells exposed to new models of hypoxia and ischemia in vitro. J Neurosci Res 89: 661–673.
Pennuto M, Tinelli E, Malaguti M, Del Carro U, D'Antonio M, Ron D et al. Ablation of the UPR-mediator CHOP restores motor function and reduces demyelination in Charcot-Marie-Tooth 1B mice. Neuron 2008; 57: 393–405.
van der Voorn JP, van Dijk J, Garbern J, Thomas AA, Scheper GC, Powers JM et al. The unfolded protein response in vanishing white matter disease. J Neuropathol Exp Neurol 2005; 64: 770–775.
van Kollenburg B, van Dijk J, Garbern J, Thomas AA, Scheper GC, Powers JM et al. Glia-specific activation of all pathways of the unfolded protein response in vanishing white matter disease. J Neuropathol Exp Neurol 2006; 65: 707–715.
Mhaille AN, McQuaid S, Windebank A, Cunnea P, McMahon J, Samali A et al. Increased expression of endoplasmic reticulum stress-related signaling pathway molecules in multiple sclerosis lesions. J Neuropathol Exp Neurol 2008; 67: 200–211.
Molina-Holgado E, Vela JM, Arévalo-Martín A, Guaza C . LPS/IFN-gamma cytotoxicity in oligodendroglial cells: role of nitric oxide and protection by the anti-inflammatory cytokine IL-10. Eur J Neurosci 2001; 13: 493–502.
Hampson AJ, Grimaldi M, Axelrod J, Wink D et al. Cannabidiol and (-)Delta9-tetrahydrocannabinol are neuroprotective antioxidants. Proc Natl Acad Sci USA 1998; 95: 8268–8273.
Zhang K, Kaufman RJ . From endoplasmic-reticulum stress to the inflammatory response. Nature 2008; 454: 455–462.
Lim MP, Devi LA, Rozenfeld R . Cannabidiol causes activated hepatic stellate cell death through a mechanism of endoplasmic reticulum stress-induced apoptosis. Cell Death Dis 2012; 10: 212–215.
El-Remessy AB, Tang Y, Zhu G, Matragoon S, Khalifa Y, Liu EK et al. Neuroprotective effects of cannabidiol in endotoxin-induced uveitis: critical role of p38 MAPK activation. Mol Vis 2008; 14: 2190–2203.
Back SA, Gan X, Li Y, Rosenberg PA, Volpe JJ . Maturation-dependent vulnerability of oligodendrocytes to oxidative stress-induced death caused by glutathione depletion. J Neurosci 1998; 18: 6241–6253.
Gow A, Southwood CM, Lazzarini RA . Disrupted proteolipid protein trafficking results in oligodendrocyte apoptosis in an animal model of Pelizaeus-Merzbacher disease. J Cell Biol 1998; 140: 925–934.
Stefani IC, Wright D, Polizzi KM, Kontoravdi C . The role of ER stress-induced apoptosis in neurodegeneration. Curr Alzheimer Res 2012; 9: 373–387.
Hoozemans JJ, van Haastert ES, Nijholt DA, Rozemuller AJ, Scheper W . Activation of the unfolded protein response is an early event in Alzheimer’s and Parkinson’s disease. Neurodegener Dis (in press).
Lin W, Kemper A, Dupree JL, Harding HP, Ron D, Popko B . Interferon-gamma inhibits central nervous system remyelination through a process modulated by endoplasmic reticulum stress. Brain 2006; 129 (Pt 5): 1306–1318.
Ron D, Habener JF . CHOP, a novel developmentally regulated nuclear protein that dimerizes with transcription factors C/EBP and LAP and functions as a dominant-negative inhibitor of gene transcription. Genes Dev 1992; 6: 439–453.
Gotoh T, Terada K, Mori M . hsp70-DnaJ chaperone pairs prevent nitric oxide-mediated apoptosis in RAW 264.7 macrophages. Cell Death Differ 2001; 8: 357–366.
Nakagawa T, Zhu H, Morishima N, Li E, Xu J, Yankner BA, Yuan J . Caspase-12 mediates endoplasmic-reticulum-specific apoptosis and cytotoxicity by amyloid-beta. Nature 2000; 403: 98–103.
Novoa I, Zeng H, Harding HP, Ron D . Feedback inhibition of the unfolded protein response by GADD34-mediated dephosphorylation of eIF2alpha. J Cell Biol 2001; 153: 1011–1022.
Almazan G, Afar DE, Bell JC . Phosphorylation and disruption of intermediate filament proteins in oligodendrocyte precursor cultures treated with calyculin. J Neurosci Res 1993; 36: 163–172.
Acknowledgements
We acknowledge the financial support of the Ministry of Science and Innovation (MICINN, project SAF-2010/17501), Instituto de Salud Carlos III (project RD07/0060/0010 RETICS program, Red Española de Esclerosis Múltiple, REEM). Mecha M is supported by REEM. We thank to Alfonso Araque and Eduardo D Martín for their help with electrophysiological studies. We are also grateful to Joaquín Sancho and Elisa Baides Rosell for their excelent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by D Bano
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Mecha, M., Torrao, A., Mestre, L. et al. Cannabidiol protects oligodendrocyte progenitor cells from inflammation-induced apoptosis by attenuating endoplasmic reticulum stress. Cell Death Dis 3, e331 (2012). https://doi.org/10.1038/cddis.2012.71
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2012.71
Keywords
This article is cited by
-
CBD hydroxyquinone photo-isomerises to a highly reactive intermediate
Scientific Reports (2023)
-
Chronic stress disrupts the homeostasis and progeny progression of oligodendroglial lineage cells, associating immune oligodendrocytes with prefrontal cortex hypomyelination
Molecular Psychiatry (2022)
-
A review on the syntheses of Dronabinol and Epidiolex as classical cannabinoids with various biological activities including those against SARS-COV2
Journal of the Iranian Chemical Society (2021)
-
Cisplatin-induced ototoxicity involves interaction of PRMT3 and cannabinoid system
Archives of Toxicology (2019)
-
Long Lasting High Lysine Diet Aggravates White Matter Injury in Glutaryl-CoA Dehydrogenase Deficient (Gcdh−/−) Mice
Molecular Neurobiology (2019)