Abstract
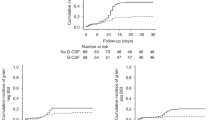
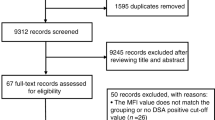
Follistatin is an angiogenic factor elevated in the circulation after allogeneic hematopoietic cell transplantation (HCT). Elevations in follistatin plasma concentrations are associated with the onset of and poor survival after acute GvHD (aGvHD). Using data from the Blood and Marrow Transplant Clinical Trials Network 0402 study (n=247), we sought to further quantify the longitudinal associations between plasma follistatin levels in transplant recipients, as well as baseline HCT donor follistatin levels, and allogeneic HCT outcomes. Higher recipient baseline follistatin levels were predictive of development of aGvHD (P=0.04). High donor follistatin levels were also associated with the incidence of aGvHD (P<0.01). Elevated follistatin levels on day 28 were associated with the onset of grade II–IV aGvHD before day 28, higher 1-year non-relapse mortality (NRM) and lower overall survival. In multivariate analyses, individuals with follistatin levels >1088 pg/mL at day 28 had a 4-fold increased risk for NRM (relative risk (RR)=4.3, 95% confidence interval (CI) 1.9–9.9, P<0.01) and a nearly three-fold increased overall risk for mortality (RR=2.8, 95% CI 1.5–5.2, P<0.01). Given the multiple roles of follistatin in tissue inflammation and repair, and the confirmation that this biomarker is predictive of important HCT outcomes, the pathobiology of these relationships need further study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
D’Souza A,ZX. Current uses and outcomes of hematopoietic cell transplantation (HCT): CIBMTR Summary Slides. 2016.
Gooley TA, Chien JW, Pergam SA, Hingorani S, Sorror ML, Boeckh M et al. Reduced mortality after allogeneic hematopoietic-cell transplantation. N Engl J Med 2010; 363: 2091–2101.
Atsuta Y, Hirakawa A, Nakasone H, Kurosawa S, Oshima K, Sakai R et al. Late mortality and causes of death among long-term survivors after allogeneic stem cell transplantation. Biol Blood Marrow Transplant 2016; 22: 1702–1709.
Duncan CN, Majhail NS, Brazauskas R, Wang Z, Cahn JY, Frangoul HA et al. Long-term survival and late effects among one-year survivors of second allogeneic hematopoietic cell transplantation for relapsed acute leukemia and myelodysplastic syndromes. Biol Blood Marrow Transplant 2015; 21: 151–158.
Li Z, Rubinstein SM, Thota R, Savani M, Brissot E, Shaw BE et al. Immune-mediated complications after hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2016; 22: 1368–1375.
Mosesso K . Adverse Late and Long-Term Treatment Effects in Adult Allogeneic Hematopoietic Stem Cell Transplant Survivors. Am J Nursing 2015; 115: 22–34.
Doring M, Cabanillas Stanchi KM, Feucht J, Queudeville M, Teltschik HM, Lang P et al. Ferritin as an early marker of graft rejection after allogeneic hematopoietic stem cell transplantation in pediatric patients. Ann Hematol 2016; 95: 311–323.
Massaro K, Costa SF . Role of biomarkers as predictors of infection and death in neutropenic febrile patients after hematopoietic stem cell transplantation. Mediterr J Hematol Infect Dis 2015; 7: e2015059.
Tatekawa S, Kohno A, Ozeki K, Watamoto K, Ueda N, Yamaguchi Y et al. A novel diagnostic and prognostic biomarker panel for endothelial cell damage-related complications in allogeneic transplantation. Biol Blood Marrow Transplant 2016; 22: 1573–1581.
Yu J, Storer BE, Kushekhar K, Abu Zaid M, Zhang Q, Gafken PR et al. Biomarker panel for chronic graft-versus-host disease. J Clin Oncol 2016; 34: 2583–2590.
Holtan SG, Verneris MR, Schultz KR, Newell LF, Meyers G, He F et al. Circulating angiogenic factors associated with response and survival in patients with acute graft-versus-host disease: results from Blood and Marrow Transplant Clinical Trials Network 0302 and 0802. Biol Blood Marrow Transplant 2015; 21: 1029–1036.
Kozian DH, Ziche M, Augustin HG . The activin-binding protein follistatin regulates autocrine endothelial cell activity and induces angiogenesis. Lab Invest 1997; 76: 267–276.
Gavino MA, Wenemoser D, Wang IE, Reddien PW . Tissue absence initiates regeneration through follistatin-mediated inhibition of activin signaling. eLife 2013; 2: e00247.
de Kretser DM, O'Hehir RE, Hardy CL, Hedger MP . The roles of activin A and its binding protein, follistatin, in inflammation and tissue repair. Mol Cell Endocrinol 2012; 359: 101–106.
Hedger MP, de Kretser DM . The activins and their binding protein, follistatin-diagnostic and therapeutic targets in inflammatory disease and fibrosis. Cytokine Growth Factor Rev 2013; 24: 285–295.
Argiles JM, Orpi M, Busquets S, Lopez-Soriano FJ . Myostatin: more than just a regulator of muscle mass. Drug Discov Today 2012; 17: 702–709.
Dschietzig TB . Myostatin—from the mighty mouse to cardiovascular disease and cachexia. Clin Chim Acta 2014; 433: 216–224.
Michel U, Ebert S, Phillips D, Nau R . Serum concentrations of activin and follistatin are elevated and run in parallel in patients with septicemia. Eur J Endocrinol 2003; 148: 559–564.
Michel U, Shintani Y, Nau R . Serum follistatin concentrations are increased in patients with septicaemia. Clin Endocrinol 1998; 48: 413–417.
Chen MJ, Chen HF, Chen SU, Ho HN, Yang YS, Yang WS . The relationship between follistatin and chronic low-grade inflammation in women with polycystic ovary syndrome. Fertil Steril 2009; 92: 2041–2044.
Flanagan JN, Linder K, Mejhert N, Dungner E, Wahlen K, Decaunes P et al. Role of follistatin in promoting adipogenesis in women. J Clin Endocrinol Metab 2009; 94: 3003–3009.
Hansen J, Rinnov A, Krogh-Madsen R, Fischer CP, Andreasen AS, Berg RM et al. Plasma follistatin is elevated in patients with type 2 diabetes: relationship to hyperglycemia, hyperinsulinemia, and systemic low-grade inflammation. Diabetes Metab Res Rev 2013; 29: 463–472.
Teede H, Ng S, Hedger M, Moran L . Follistatin and activins in polycystic ovary syndrome: relationship to metabolic and hormonal markers. Metabolism 2013; 62: 1394–1400.
Yndestad A, Haukeland JW, Dahl TB, Bjoro K, Gladhaug IP, Berge C et al. A complex role of activin A in non-alcoholic fatty liver disease. Am J Gastroenterol 2009; 104: 2196–2205.
Hansen J, Brandt C, Nielsen AR, Hojman P, Whitham M, Febbraio MA et al. Exercise induces a marked increase in plasma follistatin: evidence that follistatin is a contraction-induced hepatokine. Endocrinology 2011; 152: 164–171.
Vamvini MT, Aronis KN, Chamberland JP, Mantzoros CS . Energy deprivation alters in a leptin- and cortisol-independent manner circulating levels of activin A and follistatin but not myostatin in healthy males. J Clin Endocrinol Metab 2011; 96: 3416–3423.
Hansen JS, Rutti S, Arous C, Clemmesen JO, Secher NH, Drescher A et al. Circulating follistatin is liver-derived and regulated by the glucagon-to-insulin ratio. J Clin Endocrinol Metab 2016; 101: 550–560.
Contal C, O'Quigley J . An application of changepoint methods in studying the effect of age on survival in breast cancer. Comput Stat Data Anal 1999; 30: 253–270.
Ceafalan LC, Manole E, Tanase CP, Codrici E, Mihai S, Gonzalez A et al. Interstitial outburst of angiogenic factors during skeletal muscle regeneration after acute mechanical trauma. Anat Rec (Hoboken, N.J.: 2007) 2015; 298: 1864–1879.
Anastasilakis AD, Polyzos SA, Skouvaklidou EC, Kynigopoulos G, Saridakis ZG, Apostolou A et al. Circulating follistatin displays a day-night rhythm and is associated with muscle mass and circulating leptin levels in healthy, young humans. Metabolism 2016; 65: 1459–1465.
Hansen JS, Plomgaard P . Circulating follistatin in relation to energy metabolism. Mol Cell Endocrinol 2016; 433: 87–93.
Ciaraldi TP, Ryan AJ, Mudaliar SR, Henry RR . Altered myokine secretion is an intrinsic property of skeletal muscle in type 2 diabetes. PLoS ONE 2016; 11: e0158209.
Levine JE, Braun TM, Harris AC, Holler E, Taylor A, Miller H et al. A prognostic score for acute graft-versus-host disease based on biomarkers: a multicentre study. Lancet Haematol 2015; 2: e21–e29.
Acknowledgements
We acknowledge the BMT CTN 0402 study investigators and participating centers. Support for this study was provided by grant #U10HL069294 to the BMT CTN from the National Heart, Lung and Blood Institute and the National Cancer Institute at the National Institutes of Health, along with contributions from Wyeth Pharmaceuticals Inc. The content is solely the responsibility of the authors and does not necessarily represent the official views of the above-mentioned parties. This ancillary study of plasma samples was supported by grants from the National Marrow Donor Program (SGH and LFN). We thank Michael Ehrhardt of the UMN Cytokine Reference Laboratory for expert technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Turcotte, L., DeFor, T., Newell, L. et al. Donor and recipient plasma follistatin levels are associated with acute GvHD in Blood and Marrow Transplant Clinical Trials Network 0402. Bone Marrow Transplant 53, 64–68 (2018). https://doi.org/10.1038/bmt.2017.236
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2017.236
This article is cited by
-
Seeking biomarkers for acute graft-versus-host disease: where we are and where we are heading?
Biomarker Research (2019)
-
Tight interplay in early pregnancy between follistatin and anti-mullerian hormone in women with polycystic ovarian syndrome (PCOS)
Archives of Gynecology and Obstetrics (2018)
-
Biomarkers in Graft-Versus-Host Disease: from Prediction and Diagnosis to Insights into Complex Graft/Host Interactions
Current Hematologic Malignancy Reports (2018)