Abstract
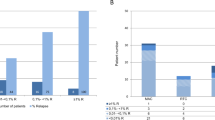
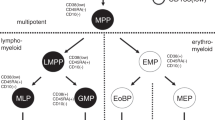
Flow cytometric routine CD34 analysis enumerates hematopoietic stem and progenitor cells irrespective of their subpopulations although this might predict engraftment dynamics and immune reconstitution. We established a multi-color CD34 assay containing CD133, CD45RA, CD10, CD38 and CD33. We examined PBSC, donor bone marrow (BMd) and BM of patients 1 year after allografting (BM1y) regarding their CD34 subset composition, which differed significantly amongst those materials: the early CD45RA−CD133+CD38low subpopulations were significantly more frequent in PBSC than in BMd, and very low in BM1y. Vice versa, clearly more committed CD34 stages prevailed in BM, particularly in BM1y where the proportion of multi-lymphoid and CD38++ B-lymphoid precursors was highest (mean 59%). CD33 was expressed at different intensity on CD45RA±CD133± subsets allowing discrimination of earlier from more committed myeloid precursors. Compared with conventional CD34+ cell enumeration, the presented multi-color phenotyping is a qualitative approach defining different CD34 subtypes in any CD34 source. Its potential impact to predict engraftment kinetics and immune reconstitution has to be evaluated in future studies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Siena S, Bregni M, Brando B, Belli N, Ravagnani F, Gandola L et al. Flow cytometry for clinical estimation of circulating hematopoietic progenitors for autologous transplantation in cancer patients. Blood 1991; 77: 400–409.
Siena S, Bregni M, Brando B, Ravagnani F, Bonadonna G, Gianni AM . Circulation of CD34+ hematopoietic stem cells in the peripheral blood of high-dose cyclophosphamide-treated patients: enhancement by intravenous recombinant human granulocyte-macrophage colony-stimulating factor. Blood 1989; 74: 1905–1914.
Sutherland DR, Anderson L, Keeney M, Nayar R, Chin-Yee I . The ISHAGE guidelines for CD34+ cell determination by flow cytometry. International Society of Hematotherapy and Graft Engineering. J Hematother 1996; 5: 213–226.
Keeney M, Chin-Yee I, Weir K, Popma J, Nayar R, Sutherland DR . Single platform flow cytometric absolute CD34+ cell counts based on the ISHAGE guidelines. International Society of Hematotherapy and Graft Engineering. Cytometry 1998; 34: 61–70.
Gratama JW, Orfao A, Barnett D, Brando B, Huber A, Janossy G et al. Flow cytometric enumeration of CD34+ hematopoietic stem and progenitor cells. European Working Group on Clinical Cell Analysis. Cytometry 1998; 34: 128–142.
Gonzalez-Requejo A, Madero L, Diaz MA, Villa M, Garcia-Escribano C, Balas A et al. Progenitor cell subsets and engraftment kinetics in children undergoing autologous peripheral blood stem cell transplantation. Br J Haematol 1998; 101: 104–110.
Saraceni F, Shem-Tov N, Olivieri A, Nagler A . Mobilized peripheral blood grafts include more than hematopoietic stem cells: the immunological perspective. Bone Marrow Transplant 2015; 50: 886–891.
Udomsakdi C, Eaves CJ, Sutherland HJ, Lansdorp PM . Separation of functionally distinct subpopulations of primitive human hematopoietic cells using rhodamine-123. Exp Hematol 1991; 19: 338–342.
Terstappen LW, Huang S, Safford M, Lansdorp PM, Loken MR . Sequential generations of hematopoietic colonies derived from single nonlineage-committed CD34+CD38- progenitor cells. Blood 1991; 77: 1218–1227.
Fritsch G, Buchinger P, Printz D, Fink FM, Mann G, Peters C et al. Rapid discrimination of early CD34+ myeloid progenitors using CD45-RA analysis. Blood 1993; 81: 2301–2309.
Kondo M, Wagers AJ, Manz MG, Prohaska SS, Scherer DC, Beilhack GF et al. Biology of hematopoietic stem cells and progenitors: implications for clinical application. Annu Rev Immunol 2003; 21: 759–806.
Bender JG, Williams SF, Myers S, Nottleman D, Lee WJ, Unverzagt KL et al. Characterization of chemotherapy mobilized peripheral blood progenitor cells for use in autologous stem cell transplantation. Bone Marrow Transplant 1992; 10: 281–285.
Reya T, Morrison SJ, Clarke MF, Weissman IL . Stem cells, cancer, and cancer stem cells. Nature 2001; 414: 105–111.
Adolfsson J, Mansson R, Buza-Vidas N, Hultquist A, Liuba K, Jensen CT et al. Identification of Flt3+ lympho-myeloid stem cells lacking erythro-megakaryocytic potential a revised road map for adult blood lineage commitment. Cell 2005; 121: 295–306.
Kamel AM, El-Sharkawy N, Mahmoud HK, Khalaf MR, El Haddad A, Fahmy O et al. Impact of CD34 subsets on engraftment kinetics in allogeneic peripheral blood stem cell transplantation. Bone Marrow Transplant 2005; 35: 129–136.
Takahashi M, Matsuoka Y, Sumide K, Nakatsuka R, Fujioka T, Kohno H et al. CD133 is a positive marker for a distinct class of primitive human cord blood-derived CD34-negative hematopoietic stem cells. Leukemia 2014; 28: 1308–1315.
Gorgens A, Radtke S, Horn PA, Giebel B . New relationships of human hematopoietic lineages facilitate detection of multipotent hematopoietic stem and progenitor cells. Cell Cycle 2013; 12: 3478–3482.
Gorgens A, Radtke S, Mollmann M, Cross M, Durig J, Horn PA et al. Revision of the human hematopoietic tree: granulocyte subtypes derive from distinct hematopoietic lineages. Cell Rep 2013; 3: 1539–1552.
Gorgens A, Ludwig AK, Mollmann M, Krawczyk A, Durig J, Hanenberg H et al. Multipotent hematopoietic progenitors divide asymmetrically to create progenitors of the lymphomyeloid and erythromyeloid lineages. Stem Cell Rep 2014; 3: 1058–1072.
Doulatov S, Notta F, Eppert K, Nguyen LT, Ohashi PS, Dick JE . Revised map of the human progenitor hierarchy shows the origin of macrophages and dendritic cells in early lymphoid development. Nat Immunol 2010; 11: 585–593.
Mori Y, Iwasaki H, Kohno K, Yoshimoto G, Kikushige Y, Okeda A et al. Identification of the human eosinophil lineage-committed progenitor: revision of phenotypic definition of the human common myeloid progenitor. J Exp Med 2009; 206: 183–193.
Radtke S, Gorgens A, Kordelas L, Schmidt M, Kimmig KR, Koninger A et al. CD133 allows elaborated discrimination and quantification of haematopoietic progenitor subsets in human haematopoietic stem cell transplants. Br J Haematol 2015; 169: 868–878.
Fritsch G, Witt V, Spengler HP, Pichler J, Scharner D, Zipperer E et al. Robust multi-parameter single-platform quantification of myeloid and B-lymphoid CD34 progenitor cells in all clinical CD34 cell sources and in thawed PBSC. Pediatr Hematol Oncol 2012; 29: 595–610.
Roug AS, Hokland LB, Segel E, Nielsen K, Toft-Petersen M, Van Kooten Niekerk PB et al. Unraveling stem cell and progenitor subsets in autologous grafts according to methods of mobilization: implications for prediction of hematopoietic recovery. Cytotherapy 2014; 16: 392–401.
Anderlini P, Korbling M . The use of mobilized peripheral blood stem cells from normal donors for allografting. Stem Cells 1997; 15: 9–17.
Schmitz N, Linch DC, Dreger P, Goldstone AH, Boogaerts MA, Ferrant A et al. Randomised trial of filgrastim-mobilised peripheral blood progenitor cell transplantation versus autologous bone-marrow transplantation in lymphoma patients. Lancet 1996; 347: 353–357.
Fritsch G, Stimpfl M, Kurz M, Printz D, Buchinger P, Fischmeister G et al. The composition of CD34 subpopulations differs between bone marrow, blood and cord blood. Bone Marrow Transplant 1996; 17: 169–178.
Leitner A, Strobl H, Fischmeister G, Kurz M, Romanakis K, Haas OA et al. Lack of DNA synthesis among CD34+ cells in cord blood and in cytokine-mobilized blood. Br J Haematol 1996; 92: 255–262.
Thornley I, Nayar R, Freedman MH, Stephens D, Crump M, Messner HA et al. Differences in cell cycle kinetics of candidate engrafting cells in human bone marrow and mobilized peripheral blood. Exp Hematol 2001; 29: 525–533.
Thornley I, Sutherland R, Wynn R, Nayar R, Sung L, Corpus G et al. Early hematopoietic reconstitution after clinical stem cell transplantation: evidence for stochastic stem cell behavior and limited acceleration in telomere loss. Blood 2002; 99: 2387–2396.
Meisel R, Enczmann J, Balzer S, Bernbeck B, Kramm C, Schonberger S et al. Similar survival following HLA-identical sibling transplantation for standard indication in children with haematologic malignancies: a single center comparison of mobilized peripheral blood stem cell with bone marrow transplantation. Klin Padiatr 2005; 217: 135–141.
Fan ZP, Yang K, Liu QF, Sun J, Xu D, Zhang Y et al. Comparison of clinical outcomes between unrelated donor peripheral blood stem cell transplantation and bone marrow transplantation for leukemia. Zhonghua Xue Ye Xue Za Zhi 2006; 27: 525–528.
Irfan M, Hashmi K, Adil S, Shamsi T, Farzana T, Ansari S et al. Beta-thalassaemia major: bone marrow versus peripheral blood stem cell transplantation. J Pak Med Assoc 2008; 58: 107–110.
Varmavuo V, Mantymaa P, Nousiainen T, Valonen P, Kuittinen T, Jantunen E . Blood graft composition after plerixafor injection in patients with NHL. Eur J Haematol 2012; 89: 128–135.
Varmavuo V, Mantymaa P, Silvennoinen R, Nousiainen T, Kuittinen T, Jantunen E . CD34+ cell subclasses and lymphocyte subsets in blood grafts collected after various mobilization methods in myeloma patients. Transfusion 2013; 53: 1024–1032.
Quach JM, Askmyr M, Jovic T, Baker EK, Walsh NC, Harrison SJ et al. Myelosuppressive therapies significantly increase pro-inflammatory cytokines and directly cause bone loss. J Bone Miner Res 2015; 30: 886–897.
Selleri C, Maciejewski JP, De Rosa G, Raiola A, Risitano AM, Picardi M et al. Long-lasting decrease of marrow and circulating long-term culture initiating cells after allogeneic bone marrow transplant. Bone Marrow Transplant 1999; 23: 1029–1037.
Woolthuis CM, Brouwers-Vos AZ, Huls G, de Wolf JT, Schuringa JJ, Vellenga E . Loss of quiescence and impaired function of CD34(+)/CD38(low) cells one year following autologous stem cell transplantation. Haematologica 2013; 98: 1964–1971.
Wolf E, Harms H, Winkler J, Reulbach U, Kirchner T, Niedobitek G et al. Terminal deoxynucleotidyl transferase-positive cells in trephine biopsies following bone marrow or peripheral stem cell transplantation reflect vigorous B-cell generation. Histopathology 2005; 46: 442–450.
Bhatia R, Van Heijzen K, Palmer A, Komiya A, Slovak ML, Chang KL et al. Longitudinal assessment of hematopoietic abnormalities after autologous hematopoietic cell transplantation for lymphoma. J Clin Oncol 2005; 23: 6699–6711.
Fedoriw Y, Samulski TD, Deal AM, Dunphy CH, Sharf A, Shea TC et al. Bone marrow B cell precursor number after allogeneic stem cell transplantation and GVHD development. Biol Blood Marrow Transplant 2012; 18: 968–973.
Acknowledgements
We would like to thank Daniela Scharner, Dijana Trbojevic and Elke Zipperer for their excellent commitment and input when establishing the described flow cytometric assay, and for their continuous support with cell preparation and data acquisition and evaluation. Dieter Printz is particularly acknowledged for his technical support in all issues of flow cytometry.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on Bone Marrow Transplantation website
Supplementary information
Rights and permissions
About this article
Cite this article
Dmytrus, J., Matthes-Martin, S., Pichler, H. et al. Multi-color immune-phenotyping of CD34 subsets reveals unexpected differences between various stem cell sources. Bone Marrow Transplant 51, 1093–1100 (2016). https://doi.org/10.1038/bmt.2016.88
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2016.88
This article is cited by
-
Widely applicable, extended flow cytometric stem cell enumeration panel for quality control of advanced cellular products
Scientific Reports (2022)
-
Bone Marrow Grafts From Pediatric Donors May Contain A Considerable Number of Hematogones
Indian Journal of Hematology and Blood Transfusion (2022)
-
Implications of hematopoietic stem cells heterogeneity for gene therapies
Gene Therapy (2021)
-
ARID3a expression in human hematopoietic stem cells is associated with distinct gene patterns in aged individuals
Immunity & Ageing (2020)
-
Allogeneic transplantation of peripheral blood stem cell grafts results in a massive decrease of primitive hematopoietic progenitor frequencies in reconstituted bone marrows
Bone Marrow Transplantation (2020)