Abstract
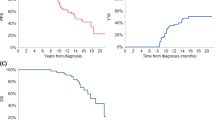
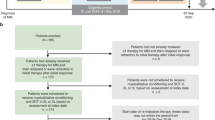
The role of auto-SCT in the treatment of multiple myeloma (MM) in the era of novel agents continues to evolve. It is now clear that the depth of response and clinical outcomes have significantly improved as a result of the combination of these strategies. However, not all patients with MM who undergo auto-SCT are able to sustain a meaningful response and 20% of patients relapse shortly after auto-SCT. In this study, we aimed to assess the impact of early relapse (ER) after auto-SCT on OS for MM patients undergoing single auto-SCT who had received novel agent-based induction regimens. All consecutive patients with MM undergoing single auto-SCT from January 2002 to September 2012 who had novel induction therapy were evaluated. A total of 184 patients were identified. The median OS and PFS for the group of transplanted patients were 93 and 25.4 months, respectively. Median time to relapse was 17.2 months with 40% having relapsed at the time of analysis. ER (<12 months post auto-SCT) was seen in 27 (36%) out of 75 patients who had relapsed, and median OS was significantly shorter than in those with non-ER. Multivariate analysis showed ER as the major independent prognostic factor for OS. On the basis of these findings, we conclude that not only attainment of a good response, but sustainability of it, appears to be a major prognostic variable in MM in the era of novel therapy. Patients with ER post auto-SCT should biologically be characterized in prospective studies to better understand the mechanisms of resistance associated with this particular entity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Attal M, Harousseau JL . The role of high-dose therapy with autologous stem cell support in the era of novel agents. Semin Hematol 2009; 46: 127–132.
Jagannath S . New drugs in multiple myeloma and the significance of autologous stem cell transplants. Clin Adv Hematol Oncol 2009; 7: 178–179.
Costa LJ, Zhang MJ, Zhong X, Dispenzieri A, Lonial S, Krishnan A et al. Trends in utilization and outcomes of autologous transplantation as early therapy for multiple myeloma. Biol Blood Marrow Transplant 2013; 19: 1615–1624.
Kumar S . Treatment of newly diagnosed multiple myeloma in transplant-eligible patients. Curr Hematol Malig Rep 2011; 6: 104–112.
Kumar S, Mahmood ST, Lacy MQ, Dispenzieri A, Hayman SR, Buadi FK et al. Impact of early relapse after auto-SCT for multiple myeloma. Bone Marrow Transplant 2008; 42: 413–420.
Venner CP, Connors JM, Sutherland HJ, Shepherd JD, Hamata L, Mourad YA et al. Novel agents improve survival of transplant patients with multiple myeloma including those with high-risk disease defined by early relapse (<12 months). Leuk Lymphoma 2011; 52: 34–41.
Hoering A, Crowley J, Shaughnessy JD Jr., Hollmig K, Alsayed Y, Szymonifka J et al. Complete remission in multiple myeloma examined as time-dependent variable in terms of both onset and duration in Total Therapy protocols. Blood 2009; 114: 1299–1305.
Paiva B, Gutierrez NC, Rosinol L, Vidriales MB, Montalban MA, Martinez-Lopez J et al. High-risk cytogenetics and persistent minimal residual disease by multiparameter flow cytometry predict unsustained complete response after autologous stem cell transplantation in multiple myeloma. Blood 2012; 119: 687–691.
Blade J, Samson D, Reece D, Apperley J, Bjorkstrand B, Gahrton G et al. Criteria for evaluating disease response and progression in patients with multiple myeloma treated by high-dose therapy and haemopoietic stem cell transplantation. Myeloma Subcommittee of the EBMT. European Group for Blood and Marrow Transplant. Br J Haematol 1998; 102: 1115–1123.
Durie BG, Harousseau JL, Miguel JS, Blade J, Barlogie B, Anderson K et al. International uniform response criteria for multiple myeloma. Leukemia 2006; 20: 1467–1473.
Blade J, Rosinol L . Advances in therapy of multiple myeloma. Curr Opin Oncol 2008; 20: 697–704.
Brenner H, Gondos A, Pulte D . Recent major improvement in long-term survival of younger patients with multiple myeloma. Blood 2008; 111: 2521–2526.
Leung-Hagesteijn C, Erdmann N, Cheung G, Keats JJ, Stewart AK, Reece DE et al. Xbp1s-negative tumor B cells and pre-plasmablasts mediate therapeutic proteasome inhibitor resistance in multiple myeloma. Cancer Cell 2013; 24: 289–304.
Chung KC, Tiedemann RE . Getting to the root of the problem: the causes of relapse in multiple myeloma. Exp Rev Anticancer Ther 2014; 14: 251–254.
Perez-Galan P, Mora-Jensen H, Weniger MA, Shaffer AL 3rd, Rizzatti EG, Chapman CM et al. Bortezomib resistance in mantle cell lymphoma is associated with plasmacytic differentiation. Blood 2011; 117: 542–552.
Shah J, Blade J, Sonneveld P, Harousseau JL, Lantz K, Londhe A et al. Rapid early monoclonal protein reduction after therapy with bortezomib or bortezomib and pegylated liposomal doxorubicin in relapsed/refractory myeloma is associated with a longer time to progression. Cancer 2011; 117: 3758–3762.
Harousseau JL . Integrating novel therapies in the transplant paradigm. Cancer J 2009; 15: 479–484.
Kumar S, Gertz MA, Dispenzieri A, Lacy MQ, Geyer SM, Iturria NL et al. Response rate, durability of response, and survival after thalidomide therapy for relapsed multiple myeloma. Mayo Clin Proc 2003; 78: 34–39.
Avet-Loiseau H, Attal M, Campion L, Caillot D, Hulin C, Marit G et al. Long-term analysis of the IFM 99 trials for myeloma: cytogenetic abnormalities [t(4;14), del(17p), 1q gains] play a major role in defining long-term survival. J Clin Oncol 2012; 30: 1949–1952.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This article was partly presented at the American Society of Hematology meeting, 2013, in New Orleans.
Author Contributions
VHJ-Z and VK performed research, collected, analyzed, interpreted data, performed statistical analysis and wrote the manuscript. and DER, ST, RT and CC designed research, analyzed and interpreted data and wrote the manuscript.
Rights and permissions
About this article
Cite this article
Jimenez-Zepeda, V., Reece, D., Trudel, S. et al. Early relapse after single auto-SCT for multiple myeloma is a major predictor of survival in the era of novel agents. Bone Marrow Transplant 50, 204–208 (2015). https://doi.org/10.1038/bmt.2014.237
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2014.237
This article is cited by
-
Targeted immunotherapy: harnessing the immune system to battle multiple myeloma
Cell Death Discovery (2024)
-
Allogeneic Stem Cell Transplantation in Patients with High-Risk Multiple Myeloma: Utopia or Continuous Challenge in Aiming for Cure?
Current Treatment Options in Oncology (2021)
-
Expert Panel Consensus Statement for Proper Evaluation of First Relapse in Multiple Myeloma
Current Hematologic Malignancy Reports (2019)
-
Early relapsed disease of multiple myeloma following up-front HDM-ASCT: a study based on the Danish Multiple Myeloma Registry in the period 2005 to 2014
Leukemia (2018)
-
Early relapse after autologous hematopoietic cell transplantation remains a poor prognostic factor in multiple myeloma but outcomes have improved over time
Leukemia (2018)